The Facial Trauma Patient in the Emergency Department: Review of Diagnosis and Management, Part III
Part III: Mandible, Mouth, Ear, and Pediatric Trauma
Authors: Gary D. Hals MD, PhD, Attending Physician, Department of Emergency Medicine, Palmetto Richland Memorial Hospital, Columbia, SC; Brandi McClain-Carter, MD, Resident Physician, Department of Emergency Medicine, Palmetto Richland Memorial Hospital, Columbia, SC; and Brent Mullis, MD, Chief Resident, Department of Emergency Medicine, Palmetto Richland Memorial Hospital, Columbia, SC.
Peer Reviewers: Andrew D. Perron, MD, FACEP, FACSM, Residency Program Director, Department of Emergency Medicine, Maine Medical Center, Portland; and Howard A. Werman, MD, Associate Professor of Clinical Emergency Medicine, The Ohio State University College of Medicine and Public Health, Columbus; Medical Director, MedFlight, Columbus, OH.
Parts I and II of this series discussed general facial wound repair, forehead and scalp trauma, eye trauma, nasal trauma, and midface fractures. This third and final part of the series covers mandible, mouth, ear, and pediatric trauma.—The Editor
Mandible Trauma
Chin Laceration Repair. Chin wounds are common and easily occur from falls where the patient leads with the chin and does not break the fall with his or her hands. Lacerations here can be repaired as in the forehead or cheek and, other than the mandible, there are no deep structures to evaluate for occult injury. Anesthesia can be administered with or without epinephrine, and the skin can be closed with 6-0 suture. Mental nerve blocks can be useful to anesthetize the skin without direct injection into the wound. (See section on Nerve Blocks in Part I.) A few minor precautions bear mentioning. While scars from these injuries are relatively well hidden, the physician still needs to be careful when realigning the skin edges. Blunt trauma often produces a tangential wound, and one must align the suture bites cautiously to keep the skin edges even. Also, chin wounds usually are good candidates for closure with tape or wound glue, but be aware that when the chin stays wet from saliva (i.e., in young children, etc.), neither may stay in place long enough to prevent wound dehiscence.
Mandible Fractures. Fractures of the mandible are common in relation to other facial bones. Some authors rate the mandible as the second most commonly fractured facial bone behind the nasal bone,1 while others give the mandible top billing.2 Common mechanisms include assaults, motor vehicle accidents (MVAs), and falls, all of which produce direct impact upon the chin. Figure 1 shows the incidence of fracture of each section of the mandible. At 36%, the condyle is the most frequently injured area, followed by the body (21%), and angle (20%). (See Figure 1.) The actual frequency of fracture depends in part on the mechanism; assaults produce a higher frequency of angle fractures, while MVAs cause more condylar fractures. This difference likely may be explained by the different direction of the forces in each case. MVAs cause a more direct blow to the symphysis, driving it superiorly and stressing the condyle, while assaults usually have a more direct blow to the body (i.e., from a punch to the face) and direct force to the angle. Another important point is that mandible fractures from MVAs never should be viewed as an isolated injury. One study of 148 patients with mandible fracture from MVA found that 65% had associated life-threatening injury, and 8% died as a result.3 Another study found that 2.6% of patients with mandible fracture from MVA also had cervical spine (C-spine) fracture.4
Figure 1.
Sites and Frequency of Mandible Fractures
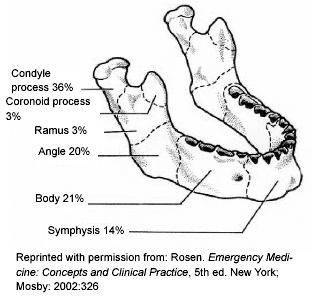
There are several unique features of mandible fractures that one must bear in mind. The U shape of the mandible makes the likelihood of multiple fractures high. One study found while approximately half (53%) will have unilateral fractures, 46% had two or more fracture sites.5 The U shape also means that the fracture site may be distant from the actual site of impact. In other words, being struck on the left side of the jaw may produce a fracture on the right side of the mandible. Condylar fractures are common and can be associated with occult fractures of the temporal bone and tympanic membrane rupture. Lastly, condylar fractures can be difficult to detect on plain films of the mandible, even with a Panorex. In some cases, a facial computed tomography (CT) scan is needed to fully rule out a condylar fracture.
Clinical features of mandible fracture often can be obvious. These include complaints of malocclusion, inability to open the mouth (trismus), facial asymmetry, and sublingual ecchymosis. Be aware that patients with unstable mandible fractures may not tolerate being supine for C-spine immobilization, as loss of support and swelling can cause airway impingement. When possible, allowing the patient to sit upright can relieve symptoms. Fractures often are open inside the mouth, and any intraoral and or gingival laceration needs to be detected, as open fractures are treated very different than closed fractures. (See below.) In some cases, the only evidence of an open fracture will be bleeding around the teeth. If the diagnosis is unclear, having the patient grasp a tongue blade between the teeth and resist while the examiner twists the blade can be a useful test. The physician should twist the blade to both sides to test each hemimandible. Patients with mandible fractures will open their mouths against resistance, while those without fracture can hold enough pressure that the blade will break off. This test is quick and easy to perform and is reported to have 95% sensitivity for mandible fracture.6 While damage to the mental nerve is rare, inferior alveolar nerve injury is more common, and sensation to the lower lip/chin should be evaluated and documented.
Imaging can be done with standard plain films (i.e., Panorex, Towne, and lateral oblique views of the mandible), or with CT scan. Beware that CT is much more accurate for detection of condylar or some symphysis fractures than plain films. If plain films are used for imaging and the results are negative with a high suspicion of fracture, then CT should be obtained. In patients with multiple injuries, it often is more time efficient to study the face at the same time other scans (i.e., head, neck, abdomen, etc.) are being performed.
Treatment of mandible fracture is determined by whether the fracture is open or closed. Any patient who has evidence of an open mandibular fracture should be admitted for IV antibiotics. Most open fractures require surgical intervention (i.e., wiring or plating). Penicillin G (2-4 million units IV) or clindamycin (Cleocin) (600-900 mg IV) are the antibiotics of choice because of their activity against anaerobic bacteria. Up to 50% of open fractures may become infected without antibiotics, while treatment with antibiotics can reduce the rate to 5%.7 For those patients with closed fracture and minimal occlusion, the use of a Barton bandage to minimize jaw movement, liquid diet, analgesia, and outpatient follow-up with an oral surgeon are recommended.
Mandible Dislocations. The mandible can dislocate with or without preceding trauma. Traumatic dislocations require imaging before reduction to rule out associated condylar fracture. Atraumatic dislocation occurs as a result of a variety of conditions: increased masseter muscle tone, temporomandibular joint laxity, and neuroleptic induced extrapyramidal effects. Dislocation usually is bilateral but also can be seen unilaterally. The jaw can dislocate in the anterior, posterior, lateral, or superior planes. However, anterior dislocation occurs most commonly as the condyle is forced in front of the articular eminence. Anterior dislocation commonly is followed by spasm of the temporalis and lateral pterygoid muscles, which hold the mandible in the disarticulated position, and resists reduction. Posterior dislocations are rare and occur from a direct blow to the chin that does not result in fracture of the condylar neck. The condyle rests against the mastoid, which may disrupt the external auditory canal; thus, posterior dislocations can be associated with cranial nerve VII and/or VIII defects. Lateral dislocations are associated with mandibular fracture as the condylar head is forced laterally and then superiorly into the temporal space. Superior dislocations are seen with blows to a partially open mouth.
Patients will complain of pain anterior to the tragus, have difficulty speaking, and also may complain of malocclusion of the teeth. In cases lacking trauma, one should seek precise history preceding the event. Anterior dislocation can occur after laughing, yawning vomiting, taking a large bite, trauma, oral sex, dental extraction, overstretching of mouth during general anesthesia, or tonsillectomy.8 Physical exam usually will show an open mouth that cannot be closed. Palpable preauricular depression and mandibular deviation in the opposite direction of the dislocation also are common findings.
When the diagnosis is clear (i.e., obvious clinical findings with no history of trauma), one may proceed directly to reduction. (See Figure 2.) Short-acting muscle relaxants, such as midazolam (Versed 2-5 mg IV), aid reduction by decreasing muscle spasm. Local anesthetic also can be administered directly into the joint space at the level of the preauricular depression. Using a 21-gauge needle, 2 mL of 2% lidocaine can be injected anterior to the tragus to provide analgesia.8 There are two methods that commonly are used to reduce anterior dislocations. The most commonly used method involves having the patient seated with the head against the wall or a chair back. The examiner should be positioned so that the examiner’s elbow is flexed at the level of the patient’s mandible. With the examiner facing the patient, the examiner’s gloved thumbs should be placed inside the patient’s mouth on the occlusal surface of the molars. The examiner’s fingers should wrap around the angle and the body of the mandible. Downward and backward pressure then should be applied. Bilateral dislocations may require the reduction of one side at a time. Be aware that the mandible may snap closed once relocation is accomplished, and the use of protective gauze over the thumbs is advised to avoid injury. The second method of reduction involves having the examiner stand at the head of a supine patient. The thumbs are placed on the molars, and downward backward pressure is applied. Successful reduction will be evident if the patient is able to close the mouth immediately after manipulation. Post-reduction films usually are taken for the first dislocation, but otherwise are not required unless the procedure was unduly difficult with significant pain. Reduction can cause fracture or avulsion of the articular cartilage; however, this is rare.
Figure 2.
How to Reduce Mandible
Dislocation
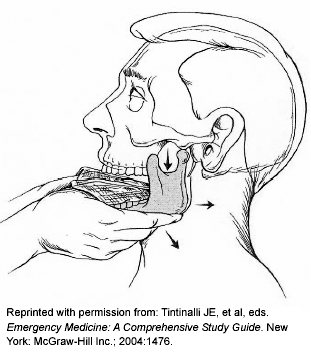
Patients may be discharged with specific instructions as long as the dislocation is not open, a superior dislocation, associated with fracture, or suspicious for nerve injury. In these cases, immediate consult by an otolaryngologist or oral surgeon is recommended. Discharged patients should have instructions to eat a soft diet, not to open the mouth wider than 2 cm for two weeks, and to support the jaw with their hands when they yawn. Non-steroidal anti-inflammatory drugs (NSAIDs) can be given for pain management, and follow-up within two weeks is recommended regardless of the dislocation type.
Ear Trauma
Wound Repair. While not as common as some other facial injuries, ear lacerations can present some hidden dangers if one is not aware of potential complications unique to the ear. The two major problems are cartilage injury and hematoma formation. Thus, repair of lacerations of the ear should have goals of covering exposed cartilage and minimizing hematoma formation. The ear has very little in the way of subcutaneous tissue, and is essentially skin and cartilage. As cartilage is relatively avascular, it relies on contact with the skin for nutrition. Remove the skin covering, and the cartilage does not survive. Thus, exposed cartilage must be recovered by skin during the repair, and hematomas must be evacuated to place the skin back in contact with the cartilage.
If cartilage is exposed but overlying skin can easily be closed (see Figure 3), then deep sutures in the cartilage are not likely to help. This is somewhat of a controversial issue, with one text recommending the use of deep sutures in cartilage9 and another recommending against it.10 If placing sutures in ear cartilage, use 5-0 or 6-0 absorbable (Vicryl) and remember that sutures easily will tear through cartilage. As any deep suture is a potential risk for infection, place sutures only at prominent landmarks, such as folds or ridges on the pinna. Debridement of skin overlying cartilage seldom is done as it quickly becomes impossible to close the wound. Cartilage, however, can be debrided carefully up to 5 mm in length if devitalized, or to make skin closure possible with minimal cosmetic deformity afterward.9 If more than 5 mm needs to be removed, the case should be referred to the consultant. Prophylactic antibiotics (i.e., cephalexin [Keflex] for 5 days) usually are given when deep sutures are placed.
Figure 3.
Illustration of Ear Laceration Repair
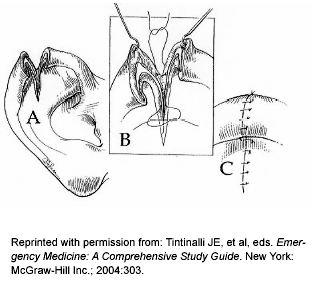
Perichondral hematomas of the ear are relatively common as a result of blunt trauma and, as mentioned above, require evacuation in the emergency department (ED) to prevent permanent cartilage loss (similar to nasal septum hematoma). Left untreated, these hematomas produce deformity of the ear known as "cauliflower ear" where the ear loses its distinct contours. Any hematoma likely should be drained when the patient presents, but cartilage damage still can occur if not drained in fewer than 72 hours from onset. Small hematomas may be decompressed with a needle, while larger hematomas can approach these in similar fashion to a cutaneous abscess. The hematoma can be drained through a small incision over its center. Compared to an abscess, though, drains usually are not needed. A pressure dressing is placed for 24 hours to prevent reoccurrence, and the patient re-checked at that time. It is not unusual for perichondral hematomas to re-accumulate and require aspiration more than once. Correct placement of a pressure dressing for the ear involves gauze pads (or cotton balls) first being placed around and especially behind the ear before the head and affected ear are wrapped with a circumferential dressing. Forgetting to place padding around the ear painfully will compress the ear against the skull and sometimes may cause pressure necrosis of ear cartilage. Given the potential complications from perichondral hematomas, it may be advisable to involve the consultant (at least by phone) from the beginning.
Otherwise, simple clean lacerations not involving cartilage can be closed with 6-0 suture taking small (1-2 mm) bites. (See Figure 3.) Remember to pay close attention to realign major surface landmarks, as noticeable disfigurement can result. Correct management can prevent such complications. Anesthetic agents should not contain epinephrine, and should be injected in small volumes with 27- or 30-gauge needles. As with the eyelid and the lip, injection of too much anesthetic can distort landmarks and place too much tension on closures. Larger wounds can be treated with an ear block. (See section on Nerve Blocks in Part I.) A cotton ear plug can be inserted in the ear canal during irrigation to limit entry of fluid. Through-and-through wounds are easiest to close if one repairs cartilage first (if needed), then posterior skin followed by anterior skin. Significant lacerations involve crush and shearing forces with a higher likelihood of injury to the perichondral nutrient supply and resultant cartilage necrosis. A compressive dressing will be required to curb the formation of a hematoma and resultant cartilage necrosis, fibrotic tissue organization, and development of cauliflower ear. Some authors recommend placement of a pressure dressing on the ear for 24 hours for all injuries,9 while others only recommend placement when one is concerned for hematoma development.10 If no bandage is placed, treat the repaired wound like other areas of the face. Apply a thin layer of antibiotic ointment and wash normally after 24-48 hours.
Contaminated wounds (i.e., bite wounds), complex lacerations, or those with tissue loss should be treated by the consultant. Be sure the patient receives the first dose of antibiotics while still in the ED; otherwise, surprising delays can take place before the first dose is obtained, whether the patient is discharged or admitted. The patient should be evaluated for related trauma, such as tympanic membrane (TM) perforation and basilar skull fracture. Hemotympanum and Battle’s sign, or ecchymosis over the mastoid process, clinically correlate with presence of basilar skull fracture.
Deep Structure Injury. Traumatic TM perforation can occur with blunt or penetrating ear trauma. Common mechanisms for blunt trauma are a direct blow to the ear (i.e., a slap to the side of the head) or a fall at speed onto the water, such as while water-skiing or wake-boarding. Patients being treated for external ear trauma should have both TMs visualized to rule out occult trauma. Lacerations in the ear canal without a history of penetrating trauma are suspicious for longitudinal temporal bone fracture. The condyle of the mandible also can be driven posteriorly and fracture the anterior canal wall. Likewise, hemotympanum is synonymous with basilar skull fracture. Blood clots may obscure the canal and need to be removed by suction to allow visualization of the TM. Active bleeding also suggests an open fracture in the canal. Persistent bleeding of the ear canal should prompt one to consider cerebrospinal fluid (CSF) otorrhea and open skull fracture. (See section on CSF Rhinorrhea in Part I.) Even if no fractures are identified, large ear canal lacerations should be referred to the otolaryngologist for stenting to prevent canal stenosis.
Traumatic TM perforations occur most commonly on the anterior-inferior and postero-inferior quadrants of the TM. The location of the perforation cannot be predicted by the amount of hearing loss, but the size does correlate.11 The injury may appear slit-like, triangular, or stellate depending on the mechanism of injury. Be aware that postero-superior quadrant perforation is a risk for ossicle involvement. Be careful not to miss nystagmus, as it indicates possible round window rupture as well. The facial nerve and geniculate ganglion are nearby and also can be injured, giving varying degrees of facial paralysis. If nystagmus or facial nerve injury is present, immediate otolaryngologist consult should be obtained for possible surgical intervention. Fortunately, the rate of spontaneous healing for most TM perforations is nearly 80%.12 Simple linear TM perforations usually are watched and often heal spontaneously in 24 hours.13 Triangular or stellate lacerations may need surgical intervention to ensure adequate healing. Some ENTs place stents (i.e., cellophane, cigarette paper, etc.) over the TM wound to promote healing, while others have studied the use of gentamycin ointment (Garamycin), but no one technique appears superior.14 When the perforation involves water (i.e., during water-skiing, etc.), one should place the patient on prophylactic antibiotics (amoxicillin-clavulanate [Augmentin] 500 mg PO TID). All patients should have otolaryngologist follow-up in case further evaluation or complete audiological and vestibular testing need to be performed.
Oral Trauma
Wound Repair. Lip Lacerations. The lip is another common site for facial laceration and, unfortunately, also is one of the least forgiving if not closed properly. The vermillion border, or boundary between facial skin and lip skin, is the culprit. A step-off as little as 1 mm from uneven alignment of a wound is noticeable. To make matters worse, secondary procedures cannot easily repair a step-off after initial healing.10 Thus accurate realignment of the vermillion border is the critical step in lip wound repair, and is done as the first step—even before deep suture placement. (See Figure 4.)
Figure 4.
Illustration of Lip Laceration Repair

The distensible nature of the lips makes nerve blocks the technique of choice for anesthesia, as direct injection can inflate the lips and blur the vermillion border. Infraorbital nerve blocks are used for upper lip, and mental nerve blocks for lower lip repair. (See section of Nerve Blocks in Part I.) Remember that midline injuries will require dual nerve blocks for adequate results. Although the lips are full of bacteria, cleaning will not clear them or keep them from the wound during repair. Thus, the removal of gross contaminants is the only goal of lip wound irrigation. Prophylactic antibiotics may be considered for mucosal repairs (see below). Mucosal wounds also have the potential for harboring tooth fragments. If a tooth is chipped, fractured, or avulsed by the injury, be sure it is accounted for. If it is not, fully explore the lip wound to rule out retention of the fragment. Probing the wound is not an adequate examination for a retained tooth fragment. Soft-tissue x-rays of the area also may be helpful. Likewise, any patient returning with a lip wound infection and tooth trauma should be evaluated for a retained tooth fragment.
Simple lacerations are closed with 6-0 non-absorbable suture, and mucosal injuries closed with 6-0 or 5-0 absorbable. (See Figure 4.) Do not place non-absorbable suture anywhere inside the mouth, as the edges are sharp and very irritating. The mucosal surface of the lip is identified as the portion that is inside the mouth when the lips are closed normally. Again, realignment of the vermillion border is performed with the first suture placed, though this stitch may be left untied at first to ease deep suture placement. Through-and-through lip wounds are not unusual and are closed in three layers: deep muscle, skin, and mucosal surface. The orbicularis oris muscle is closed with 5-0 absorbable, but this is not placed or tied until after vermillion border realignment. It is important to tie extra knots (at least four square knots) on mucosal surface sutures as the constant motion of the tongue easily can work them loose otherwise.
Complex lip lacerations are best left for the consultant, although up to 25% of the lip can be lost without significant deformity or need for secondary reconstruction. Important exceptions to this rule are the upper lip below the nose and the commissures (corners of the mouth). Tissue loss here should be referred for repair. Likewise, any burn to the commissure (i.e., from biting an electrical cord) needs to be treated by an experienced consultant. These injuries can have delayed bleeding complications and can cause deforming contractures. Puncture wounds usually are closed on the skin surface only, and the mucosal surface is left open for drainage.
Lip wounds are not bandaged, and patients are instructed to avoid unnecessary pressure (i.e., stretching) of the lips. They also should be told to rinse the mouth after each meal to remove food particles from the healing wound surface. Sutures are removed in 4-5 days to reduce suture marks. At least one prospective, double-blind, placebo-controlled study supports the use of prophylactic antibiotics (penicillin) for intra-oral lacerations.15 Although the study size was relatively small, they found that none of the patients properly taking penicillin for 4-5 days after repair developed an infection, compared to 8% of controls. Clindamycin is the alternative in patients with allergy to penicillin.
Tongue and Mucosal Lacerations. While tongue and mucosal lacerations are relatively common, in most cases sutures are not required for adequate healing. Both areas heal quickly with minimal infection if left alone. Exceptions for mucosal wounds are flaps greater than 2-3 cm in size or gaping lacerations. These should be sutured to prevent food from being trapped under the wound and to reduce risk of infection. Even after healing, deep tongue wounds may heal with a permanent cleft in the tongue that can trap food and cause discomfort. Gaping wounds that are left to heal on their own also may heal with an abundance of scar tissue that can reduce tongue function and affect speech. Again, the wound should be explored for lost tooth fragments when combined with dental injury. Mucosal wounds usually re-approximate with just a few 5-0 or 6-0 absorbable sutures.
Tongue lacerations most often result from falls or seizures, and many tongue wounds can be left to heal without sutures. Sutures are recommended for any wounds on the edge of the tongue, through-and-through injuries, wounds that bisect the tongue, deep gaping wounds, wounds that have large flaps, or for control of bleeding. Uncooperative patients (children or adults) require sedation for tongue repair, and may need general anesthesia. Cooperative patients should have 2% or 4% lidocaine-soaked gauze placed over the wound for 4-5 minutes before injection of lidocaine. Epinephrine can be included if hemostasis is difficult, but should not be injected in the tip of the tongue. The tongue is held protruded by an assistant with dry gauze or by placing a stay suture through the anesthetized tip of the tongue. Absorbable 5-0 or 4-0 suture should be used as non-absorbable suture is very irritating in the mouth. All knots should be buried, as they are more comfortable and less likely to become untied through natural tongue motion. One can close the deep muscle layer, top and bottom mucosal surfaces all in a single stitch. Alternatively, one also can close the top and bottom surfaces separately, but take big enough bites to include the deep muscle layer. Small surface flaps simply are trimmed off, while larger flaps should be anchored in place by a few sutures. Aftercare consists of following a soft/liquid diet and rinsing the mouth with diluted peroxide solution for the first 2-3 days after repair. There is no literature on the need for prophylactic antibiotics for tongue wounds, and most patients do well without them.
Dental Trauma. Dental injuries are common, and include fractures, lunation (loose teeth with or without displacement), intrusion (teeth displaced vertically into alveolar bone), extrusion (teeth displaced by partial avulsion), and avulsion (complete displacement of the tooth from the socket). An avulsed permanent tooth (primary teeth are not reimplanted) is the worst-case scenario, and accounts for 16% of all dental injuries.16 Fortunately, this also is the case where the ED physician can have the most impact. As soon as the patient is stable, the tooth should be replaced into the socket. The tooth may be rinsed in saline or water first if visibly contaminated, but do not touch, clean, or rub the root as this can remove periodontal ligament fibers and dramatically can lower the chance of successful reimplantation. Teeth that have been dry for more than 20 minutes should be moistened with saline first or alternatively soaked in Hank’s solution for 20-30 minutes.16 If the tooth cannot be replaced in the socket immediately, it should be held in either the patient’s mouth, milk, or a commercial tooth container. If the tooth cannot be replaced quickly, chances for ultimate survival diminish abruptly; only 5% of teeth survive after two hours (almost a 1% per minute decrease).
Extrusion of a tooth is a common injury. Lateral displacement is more serious than anterior or posterior displacement, as lateral injuries are more likely to be associated with alveolar fracture. Extrusion injuries still are significant; 50% of teeth will have pulp necrosis in 1.5 years after trauma.16 Any tooth that is displaced enough to interfere with normal occlusion should be referred to a dentist for either extraction or repositioning and splinting. Likewise, a very loose tooth can be an aspiration risk, and should be splinted in the ED. Some emergency physicians (EPs) may be experienced and have the necessary equipment to do this in the ED, but most will require a dental consult in the ED. Intrusion of a tooth may even be to the point that the tooth is no longer visible. Attempts to pull the tooth back to normal position are not indicated. Dental referral should be provided to watch for re-eruption over four weeks, and extraction if does not. All patients with extrusion, lunation, or avulsion should have prophylactic antibiotics (penicillin or clindamycin if penicillin-allergic).
Tooth fractures are classified by location and severity. Ellis class I fractures involve only the enamel, which can be recognized by seeing only normal white tooth in the fracture. These injuries are only of cosmetic concern and may be referred for elective repair. Sharp edges can be uncomfortable and may be covered or smoothed temporarily with dental wax. Class II fractures involve the dentin, which appears yellowish in the fracture. These account for approximately 70% of tooth fractures.16 Patients often complain of heat and cold sensitivity, and require intervention. Dentin connects to the pulp and, if exposed, can act as a conduit for pulp infection. Dental cement can be used to cover dentin temporarily until the patient can see a dentist. Class III fractures involve the pulp and are identified by any pink color or bleeding from the fracture. They are treated similarly to class II fractures. Root fractures can occur with or without crown injury, and some may be identified only by x-ray. Patients should be informed that root fractures may be present and should be referred for dental follow-up. Long-term complications of tooth fracture include pulp death, root reabsorption, cosmetic color changes, and damage to permanent teeth not yet erupted.
Pediatric Facial Trauma
Pediatric patients unfortunately often suffer traumatic injuries. Lacerations alone are estimated to account for up to 40% of all pediatric patients presenting with injuries to the ED, and 60% of these wounds occur on the head.17 Males are twice as likely to be injured compared to females, and falls are a common cause. One should be aware of physical abuse as a cause when the stated history does not fit the injury seen or is not consistent with the patient’s development. One example is the 6-month-old who "climbs onto a counter and falls off" when it is not physically possible for a 6-month-old to do so. Linear lacerations that appear in a cluster on sites not commonly injured, i.e. the back, suggest being hit with a belt or other object. Finally, wounds or injuries around the genitals also can result from abuse and may need to be evaluated as such.
Bite Wounds. Children suffer from bite wounds more often than adults, with a peak incidence occurring in the 5- to 14-year-old age group.18 Dog bites in adults occur more often to the extremities, but in children younger than 9 years, the injury is predominantly to the face and head.19 The culprit usually is an animal known to the patient, with only 3-15% of bites from wild animals. Bites wounds on the head of smaller children are higher risk for skull fracture or penetration. Another study pointed out that while facial fractures are not common from bite wounds, 87% of patients with facial fractures were younger than 16 years.20 The most commonly fractured bones were nasal or orbital bones. Any bite wound near the orbit also is a concern for puncture wound to the globe. Cat bites actually are at higher risk for infection than dog bites as they tend to be more of a puncture wound and are more difficult to clean. Larger, open wounds are less prone to infection. Because bite wounds typically carry a high bacterial load, physicians in the past have been reluctant to close them primarily. The literature now supports primary closure of all potentially disfiguring bite wounds on the face. The rate of bite wound infection is lowest for the face compared to other locations.19 Wound infection rates typically are in the 6% range for all wounds, and the rate varies from 1.4% to 5.8% for facial bites.21 After thorough irrigation with diluted (1%) povidone-iodine solution, devitalized tissue should be debrided. Certain areas of the face do not handle debridement well, specifically the nose, ears, and forehead. Even minor wound edge trimming can produce wounds that cannot be closed afterward. The ED physician should have a low threshold for plastic surgery/ facial trauma specialist consult for any complex or large bite wounds on the face. When repairing wounds in the ED, most physicians will use prophylactic antibiotics for facial bite wounds. Amoxicillin/clavulanate usually is prescribed for a 3-5 day course. The literature on the effectiveness of prophylactic antibiotics for dog bites is replete with examples of benefit and no-benefit articles. A recent meta-analysis, however, does support a reduction in rates of infection in high-risk cases.22 Cat and human bite wounds are more clear-cut examples of the need for prophylaxis. Patients should be instructed to return for recheck in fewer than 48 hours.
Dealing with Young Children and Parents. Pediatric patients with facial injuries present in the context of unique concerns. Young children fear needles and pain, while their parents are extremely concerned about their child’s comfort and even more anxious about scarring and future appearance. While some young children may not be able to be consoled in this context, remember that a young (1-5 years old) child’s receptive language skills are nearly always more advanced than their speech. Remembering to explain each step to the child in terms they can understand can go a long way to comforting the patient, which in turn can calm the parent(s). First, start by just taking a look. It can be helpful to keep the child in the mother or father’s arms for this step, as stranger anxiety and separation from the parent are deep-seated fears for infants and toddlers. Having a parent help expose the wound while the physician just observes the injury can be more fruitful than having the physician doing so. As there likely will be a point at which one has to force the child to submit to further examination or the repair procedure, it is helpful to delay this until the repair is ready to start. Any deep exploration or probing of the wound should be performed under anesthesia (as one would do for an adult). Direct pressure to control bleeding also can be much more successful if the parent is applying pressure.
As often can be the case in pediatrics, the parents may be the actual patients who consume the physician’s time during treatment of the injury. With younger children, this may be the first visit to the ED, and the parents’ imaginations can run wild with worst-case scenarios about permanent disfigurement. At times, parents may request or even demand wound closure by a plastic surgeon for very minor lacerations because they believe this will result in no scar from the repair. In general, the EP should spend time educating the parents about what plastic surgeons can provide for their child, but at the same time not try to sell them on the idea of having the ED physician close the wound. Doing so puts the EP at unnecessary risk because, if the parents are very concerned about the child’s appearance from the beginning, it is likely they may not be happy with the resulting scar at some point in the future. They may be left with the thought, "If only we had used the plastic surgeon from the start and not let the ER doctor convince us otherwise ." Simply educate the patient/family as follows, "All cuts that require sutures will leave a scar. The body heals wounds with scar tissue. The scar will change and usually improve in appearance during the next 12 months. Plastic surgeons trade one scar for another in the future after the wound heals. In general, every physician closes small, straight wounds in the same way. I will repair the wound or you can decide to have the plastic surgeon called in. The choice is up to you." Parents at times may ask, "What would you do if it were your child?" The EP should provide an honest answer and then refer the decision back to the family. After they have chosen to have the consultant called, it is helpful to give them a realistic time estimate on the consultant’s arrival and not to predict what the consultant will do (i.e., take them to the operating room, etc.). Making predictions that may not come true can generate distrust of the consultant if the consultant chooses not to follow your plan. If the family opts for ED physician closure, document briefly the discussion that took place and give them the referral for plastic surgeon follow-up even if they think it will not be needed. Remember that while the ED physician may know that a plastic surgery closure for a simple 1 cm laceration really makes little difference, the physician treating the parents’ perceptions, expectations, and fears.
Finally, it is useful to give written instructions on aftercare, as they may be too distracted at the time to remember everything that is said. Stress the importance of adequate sunscreen use on the scar for up to 12 months after injury to minimize or prevent permanent discoloration of facial scars. This should begin after all scabs are gone. As with adult facial wounds, they can wash the child’s wound normally with soap (no peroxide) after 24-48 hours. Most young children will leave sutures alone if they are out of sight, but a bandage may be useful to provide a layer of protection, whereas in adults the wound may be left uncovered.
Restraints and Sedation. Despite the physician’s best efforts at calming children, there always are those that cannot be treated without chemical or physical restraint. In some cases, i.e., penetrating eye trauma, the patient may require sedation just for safe performance of the initial exam. Physical restraint with a papoose usually is employed to preverbal children (i.e., toddlers and infants), but can be upsetting for the parents. Taking time to explain the need for restraint and the risks of alternatives (sedation) usually helps parents accept the restraint. Allowing parents to stay in the room for the procedure can be helpful unless the parent is unable to remain calm and actually worsens the child’s condition by their presence. Very young children usually are not consoled by seeing the parent in the room and just want to get up and leave. In these cases where both child and parent ultimately are more upset by being together, it is best for the parent to wait in the waiting room until the repair is finished. The EP can focus more completely on the repair and finish more rapidly when a parent is not hovering and crying over staff shoulders. The physician should strive to minimize the time in restraints. Everything should be made ready, including assembling suture materials, holding help, etc., before the child is placed in the restraint.
Older children (3-4 years and up) usually do benefit from having someone, such as a parent or often staff, distract the child during the procedure. Asking the child about pets, friends, favorite TV shows, etc., can be a great help in keeping his or her mind off the present situation. Also be aware of aspiration risks with restrained children. Crying with a full stomach can induce vomiting, so the physician should be ready to roll the child on his/her side if this occurs. Fortunately this is relatively easy and safe when using a papoose board. An assistant to hold the patient’s head still can be especially valuable when suturing facial wounds. Make sure the assistant uses his or her palms and not fingertips when holding the head to reduce pain and bruising. The lip can be a very challenging site for suturing in a young child. The assistant can help by applying gentle pressure underneath the jaws (but not with fingertips) to minimize movement. Unfortunately, no matter how still the body is, the lip/mouth cannot be immobilized just using physical restraints. Sedation often is needed in cases where the patient must be still to achieve good closure, such as alignment of the vermillion border, larger lacerations, etc.
There are multiple approaches to pediatric procedural sedation and a complete discussion is beyond the scope of this article. Choice of sedation option is based on expected procedure time, level of anesthesia required, resources at the facility, and the degree of immobility needed for the repair (i.e., does the patient need to be motionless?). The reader is referred to the general guidelines published by the American College of Emergency Physicians (ACEP).23
A few useful tips on pediatric sedation bear mentioning. One should remember that most sedation agents (benzodiazepines) do not provide analgesia. When using these types of sedation, remember also to inject local anesthetic or use an additional agent specifically for pain (i.e., fentanyl [Sublimaze], etc.). Midazolam has some great advantages for the ED setting. It has a short half-life (30-45 minutes), can be given IM/IV/O or intranasally, and has associated amnesia for the event. Dosing is as follows: 0.1-0.15 mg/kg IV; 0.2 mg/kg IM; 0.2-0.3 mg/kg intranasal; and 0.3-0.5 mg kg PO. Intranasal and PO routes are handy for younger children who are very anxious but do not require more controlled sedation. Parents like the idea that the child will not remember the procedure. Remember to wait the full 20-30 minutes for PO and intranasal dosing to have maximal effect. Ketamine (Ketalar) has unique properties that make it very useful for procedural sedation in the ED. It can be given IV (1-2 mg/kg) or IM (2-4 mg/kg) and induces a dissociative state where the patient is still, sedated, and anesthetized at the same time. The child truly will not move for about 10-15 minutes immediately after the IV push. Thus, unlike with midazolam, the physician should be ready to suture immediately after ketamine is given IV. Ketamine should be given in combination with atropine (0.02 mg/kg, with 0.1 mg as the minimum dose) to reduce hypersalivation. Emergence reactions are more common in older children (older than 4-5 years), and parents should be made aware of the possibility. To combat these emergence phenomena, one may choose to use a benzodiazepine (midazolam) in combination with a lower dose of ketamine.24
Facial Fractures. Facial fractures are not especially common in pediatric patients. Incidence of pediatric facial fracture ranges from 1-14% of all facial fractures.25 When bones break, though, the frequency is similar to adults. A 1993 series found the following breakdown in pediatric facial fractures: 45% nasal, 32% mandible, and 20% zygomatic or orbital fracture.26 Any diagnosis of facial fracture should prompt one to consider if the reported mechanism fits with the injury. One strongly should consider child abuse in that setting, and the patient’s entire body may need to be re-examined looking for other signs of non-accidental injury. In children younger than 6 years, the frontal bone is injured more commonly than in adults due to its prominence. Maxillary fractures also are rare as sinuses have not developed fully. Some complications of fractures are more common in children. Nasal fractures in children are at increased risk for developing septal hematomas, and these also can occur from blunt trauma without nasal fracture. Septal hematoma in children also carries major risk for cosmetic deformity. One study of 16 children (mean age 5 years, range 2-14 years) with septal hematomas found major complications requiring multiple reconstructive surgical procedures in 62% of their patients.27 By the age of 12-15 years, fracture patterns resemble those of adults.
Mandible fractures in children often are associated with other facial fractures. Fully 33% of children with mandible fractures will have another facial fracture.28 Another study also found a high incidence of associated internal injuries.29 (See next paragraph.) Younger children can be more difficult to examine, and may not easily open their mouths if painful. Chin lacerations are common, but also can be a sign of condylar fracture. These should be sought if the child has difficulty opening his or her mouth. While they may not do so on command, very few young children will cry without opening their mouths widely. Panorex and CT scan are the imaging modalities of choice, as in adults. Children have the added complexity of growth plate injury, and any diagnosed or suspected mandible fracture requires consult and usually admission from the ED. Condylar fractures are especially high risk and can lead to micrognathia and ankylosis of the temporomandibular joint.
When facial fractures are diagnosed, be aware of associated injury, as they occur in between 50-88% of cases.25,30 Children have a greater incidence of head trauma and intracranial injury than adults. Orbital fractures in children are especially high risk for neurocranial injury. In infants, facial injuries usually occur from falls out of a seat or stroller. At least one study has shown correlation with the size of a cephalohematoma and risk of skull fracture and/or intracranial injury.31 Parietal and temporal hematomas were higher risk than frontal ones, and size of scalp hematoma directly correlated with presence of deeper injury. Children also are higher risk for upper C-spine injury, and spinal cord injury without radiographic abnormality (SCIWORA). Consultation is recommended for any child with facial fractures as later facial growth can be altered, producing devastating cosmetic deformities. If a patient is discharged, follow-up must be in only a few days, as callus formation will complicate further treatment in as little as one week.
References
1. Cantrill SV. Face. In: Marx J, et al, eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice, 5th ed. New York: Mosby Inc. 2002:314-329.
2. Azevedo AB, Trent RB, Ellis A. Population-based analysis of 10,766 hospitalizations for mandibular fractures in California, 1991 to 1993. J Trauma 1998;45:1084-1087.
3. Fischer K, Zhang F, Angel MF, et al. Injuries associated with mandible fractures sustained in motor vehicle collisions. Plast Reconstr Surg 2001;108:328-331.
4. Ardekian L, Gasper R, Peled M, et al. Incidence and type of cervical spine injuries associated with mandibular fractures. J Craniomaxillofac Trauma 1997;3:18-21.
5. Fridrich KL, Pena-Velasco G, Olson RAJ. Changing trends with mandibular fractures: A review of 1067 cases. J Oral Maxillofac Surg 1992;50:586-598.
6. Alonso LL, Purcell TB. Accuracy of the tongue blade test in patients with suspected mandibular fracture. J Emerg Med 1995;13: 297-304.
7. Lamphier J, Ziccardi V, Ruyo A, et al. Complications of mandibular fractures in an urban teaching center. J Oral Maxillofac Surg 2003; 61:745-749.
8. Haddon R, Peacock WF IV. Face and Jaw Emergencies. In: Tintinalli JE, et al, eds. Emergency Medicine: A Comprehensive Study Guide, 6th ed. New York: McGraw-Hill Inc; 2004:1471-1476.
9. Lammers RL. Principles of wound management. In: Roberts JR, Hedges JR, eds. Clinical Procedures in Emergency Medicine, 3rd ed. Philadelphia: W.B. Saunders Co;1998:533-559.
10. Trott AT. Special anatomic sites. In: Wounds and Lacerations: Emergency Care and Closure, 2nd ed. New York: Mosby-Year Book Inc;1997:178-207.
11. Voss SE, Rosowski JJ, Merchant SN, et al. How do tympanic-membrane perforations affect human middle-ear sound transmission? Acta Otolaryngol 2001;121:169-173.
12. Kristensen S. Spontaneous healing of traumatic tympanic membrane perforations in man: A century of experience. J Laryngol Otol 1992;106:1037-1050.
13. Kinney SE. Trauma to the Middle Ear and Temporal Bone. In: Cummings C, et al eds. Cummings: Otolaryngology Head and Neck Surgery, 3rd ed. New York: Mosby-Year Book Inc; 1998; 3076-3087.
14. Amadasun JE. An observational study of the management of traumatic tympanic membrane perforations. J Laryngol Otol 2002;116: 181-184.
15. Steele MT, Sainsbury CR, Robinson WA, et al. Prophylactic penicillin for intraoral wounds. Ann Emerg Med 1989;18:847-852.
16. Beaudreau RW. Oral and Dental Emergencies. In: Tintinalli JE, et al eds. Emergency Medicine: A Comprehensive Study Guide, 6th ed. New York: McGraw-Hill Inc; 2004:1482-1494.
17. Baker MD, Selbst SM, Lanuti M. Lacerations in urban children. AJDC 1990;14:87-92.
18. Marcy SM. Infections due to dog and cat bites. Ped Infect Dis 1982; 1:351-356.
19. Callaham ML. Treatment of common dog bites: Infection risk factors. Ann Emerg Med 1980;17:1321-1330.
20. Tu AH, Girotto JA, Singh N, et al. Facial fracture from dog bite injuries. Plast Reconstr Surg 2002;109:1259-1265.
21. Guy RJ, Zook EG. Successful treatment of acute head and neck dog bit wounds without antibiotics. Ann Plast Surg 1986;17:45-48.
22. Dire DJ. Emergency management of dog and cat bites wounds. Emerg Med Clin North Am 1992;10:719-736.
23. American College of Emergency Physicians. The use of pediatric sedation and analgesia. Ann Emerg Med 1993;22:626-627.
24. Priestley SJ, Taylor J, McAdam CM, et al. Ketamine sedation for children in the emergency department. Emerg Med 2001;13:82-90.
25. Haug RH, Adams JM, Conforti PJ, et al. Cranial fractures associated with facial fractures: A review of mechanism, type and severity of injury. J Oral Maxillofac Surg 1994;52:729-733.
26. Kaban LB. Diagnosis and treatment of fractures of the facial bones in children 1943-1993. J Oral Maxillofac Surg 1993;51:722-729.
27. Alvarez H, Osorio J, De Diego JI, et al. Sequelae after nasal septum injuries in children. Auris Nasus Larnyx 2000;27:339-342.
28. Schweinfurth JM, Koltai PJ. Pediatric mandibular fractures. Facial Plast Surg 1998;14:31-44.
29. Thaller SR, Mabourakh S. Pediatric mandibular fractures. Ann Plast Surg 1991;26:511-513.
30. Spring PM, Cote DN. Pediatric maxillofacial fractures. J La State Med Soc 1996;148:199-203.
31. Greenes DS, Schutzman SA. Clinical significance of scalp abnormalities in asymptomatic head-injured infants. Pediatr Emerg Care 2001;17:88-92.
Parts I and II of this series discussed general facial wound repair, forehead and scalp trauma, eye trauma, nasal trauma, and midface fractures. This third and final part of the series covers mandible, mouth, ear, and pediatric trauma.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
