Prevention of Venous Thromboembolism in the Medical Patient: Fact vs. Fiction
Authors: Franklin Michota, MD, Section Head, Hospital Medicine, Department of General Internal Medicine, The Cleveland Clinic Foundation, Cleveland, OH; and Wael Saber, MD, Section of Hospital Medicine, Department of General Internal Medicine, The Cleveland Clinic Foundation, Cleveland, OH.
Peer Reviewer: Mark Knudson, MD, Department of Family and Community Medicine, Wake Forest University School of Medicine, Winston Salem, NC.
Physicians increasingly are aware of the need to provide prophylaxis against venous thrombosis for the medically ill patient in the hospital environment. Venous thromboembolism (VTE), which includes the entities of deep vein thrombosis (DVT) and pulmonary embolism (PE), is a common disease that affects more than 2 million people each year and accounts for more than 250,000 hospitalizations annually.1 The most serious complication of DVT is PE, which may be responsible for as many as 200,000 deaths each year and remains preventable up to 50% of the time.2 These statistics have been described as a "crisis in thrombosis," prompting a coalition lead by the Society of Hospital Medicine to establish the first inaugural DVT Awareness Month in March 2004. Unfortunately, despite this heightened awareness regarding the need and the overwhelming evidence of the efficacy of drug-based prevention strategies, recent studies confirm that the majority of hospitalized patients receive no VTE protection.3 Many clinicians still do not appreciate the need for effective prophylaxis in the medically ill patient. This article attempts to separate the fact from fiction regarding VTE prophylaxis. — The Editor
Fact: Prevention Is Necessary, Even Though VTE Is a Treatable Condition, and Therapies Should Not Be Delayed Until Symptoms Develop.
Almost all PE originates from an existing clot in the deep venous system of the legs, of which more than half are clinically silent.4 In fact, the first manifestation of the disease may be fatal PE that often is not recognized in medical patients. Autopsy results from the Framingham study documented 50 deaths from PE in medically ill patients. In 74% of these deaths, the clinicians had no suspicion of PE as a cause of death prior to autopsy.5 VTE accounts for 10% of all in-hospital mortality, with 25% of all fatal PE occurring as sudden death.6 For patients that suffer a fatal PE yet survive the first few seconds, the remaining will die in the next two hours. Anticoagulation for PE does nothing to reduce mortality from the first event; it is intended to reduce the risk of recurrence, which could again lead to mortality. The risk of PE death remains significant despite initial survival, as the long-term case fatality rate is 19% at one year.6 For the elderly, PE carries a one-year mortality rate of 39%. Identifying patients at risk and applying preventative measures is the only way to decrease VTE-related mortality.
VTE survivors also are at risk for developing chronic post-thrombotic syndrome (PTS). Approximately 20% of patients with a single DVT will suffer a recurrence.7 Of those who develop a second DVT, almost half will experience a third. Multiple episodes of VTE increase the risk for PTS, which is characterized by chronic pain, edema, skin induration, and ulceration of the lower extremities. PTS is estimated to occur in one-third of VTE survivors within 10 years.8
In economic terms, the cost of a primary DVT is similar to that of an acute myocardial infarction or stroke.9 The additional long-term health care cost of PTS is about 75% of the cost of a primary DVT. Medicare beneficiaries represented almost half of the total inpatient DVT cases in the United States in 2002. That year, the total hospital DVT care-related Medicare bill was estimated to be $2.7 billion.10
Unfortunately, another significant consequence today from the failure to prevent VTE is medicolegal. Most legal actions are triggered by a plaintiff's perception that an unexpected adverse event, such as PE, was preventable.11 Furthermore, claims data from Physicians Insurance, a national malpractice clearinghouse, ranks pulmonary emboli 18th on a list of the 40 most common conditions generating malpractice claims. Physicians most commonly involved in these claims are internists, family practitioners, emergency medicine physicians, and cardiovascular surgeons. Most of the claims allege a delayed or missed diagnosis, and the average indemnity paid is $194,486.12
Fact: Prophylaxis Is Still Necessary, Even Though Some Evidence May Show Declines in VTE Among Certain Patient Populations.
There is some evidence that the incidence of VTE has declined in recent years, particularly in surgical patients, and this probably reflects the success of prophylaxis strategies as well as other aspects of surgical and postoperative care. Yet, approximately three out of four fatal PE cases occur in medical patients—not surgery patients. Autopsy series demonstrate that, during the past three decades, the incidence of fatal PE has remained constant for non-surgical patients.13 The Rochester Epidemiology Project documents that the incidence of DVT has remained unchanged for men and is increasing for older women.14 Most epidemiologic studies document that the elderly are particularly vulnerable to PE. With the advancing age of the population, VTE will become an escalating problem for medical inpatients.
Fact: Many Average Medical Patients Are at High Enough Risk for VTE to Warrant Routine Prophylaxis.
Most protocols for VTE prophylaxis primarily have addressed the surgical patient. In fact, the schematic of VTE risk used in North America is derived from epidemiologic studies in surgical patients. (See Table 1.) Nearly 100,000 patients have been included in trials concerning the prevention of VTE in surgery, whereas only about 15,000 patients have been included in such trials in medical care. Medically ill patients account for fewer than 10% of those identified as prophylaxis candidates in the 2001 American College of Chest Physicians (ACCP) recommendations for anticoagulation. This has led many to assume erroneously that the medical patient was not at significant risk.
Much of the former evidence in medical patients that would allow an estimation of risk has suffered from tightly defined populations that do not adequately represent the heterogeneous medical inpatient today. Observed rates of thrombosis reported in the literature still vary widely depending on how the medical population is defined. The best evidence to determine the average risk for medical patients is found in recently performed placebo-controlled trials of new anticoagulants. These FDA-labeling studies are actually landmark epidemiologic trials. In the only such trial published to date, Samama and colleagues found the venographic proximal DVT rate in a typical medically ill population that averaged 2.3 risk factors for VTE, to be as high as 5%.15 Most recently, the ARTEMIS trial found a 1.2% fatal PE rate in their medically ill placebo group.16 This data suggests that the average medical patient today is in fact at high risk for VTE and, in some cases, in the very high risk category. Hospitalization itself has been found to be the most significant adjusted population attributable risk factor for VTE, further suggesting that all inpatients, surgical and medical, are at high risk for VTE.17
Knowledge of clinical risk factors for VTE helps to support these concepts and forms the basis for the appropriate use of prophylaxis, as well as the formulation of pre-test probability for VTE diagnosis. (See Table 2.) However, it must be emphasized that individual risk assessment models have not been validated, and there is little understanding of how various VTE risk factors interact to determine any one patient’s individual risk for thrombosis. In addition, individualizing prophylaxis is logistically complex and will be associated with less than optimal compliance. Within the current hospital environment, virtually all medical patients are acutely ill and compromised by restricted mobility. Most patients will have multiple risk factors, and the risks are cumulative.18 One study demonstrated that one out of five hospitalized patients had at least three VTE risk factors a decade ago.19 Current medical inpatients are older, sicker, and more complex. Today, it is estimated that 90% or more of medical patients will need prophylaxis.
Table 2. Risks for VTE

Fact: There Is No Evidence that Occasional Ambulation Is an Effective Protection Strategy for High-Risk Patients.
Ambulation has long been thought of as the best and cheapest form of prophylaxis. Yet, this hypothesis never has been tested. Ambulation is a marker of health. It is speculation to think that one could take an acutely ill person, force him or her to ambulate, and thus protect the patient from a prothrombotic state. Ambulation does increase venous flow in the same manner as intermittent pneumatic compression (IPC) devices. However, IPCs have been shown to be effective only if worn 24 hours daily for multiple days.20 Patients cannot ambulate continuously, and it is unclear how much is needed to reduce the risk for VTE. It is even less clear that any hospitalized patient could ambulate more than the smallest fraction of the day. For example, even if a patient ambulated for 15 minutes every hour while awake, he or she still would be in bed for more than 80% of the day. There simply is no evidence that bathroom privileges or even occasionally walking down the hospital corridor is an efficacious VTE protection strategy for high-risk patients.
Fact: There Is Not Enough Evidence on the Effectiveness of Mechanical Compression Devices in Medical Patients.
Use of non-pharmacologic VTE prevention strategies such as elastic stockings (ES) or IPC devices has not been well studied in heterogeneous medical populations. In fact, the only available studies in medical patients have been performed in the medical intensive care unit (ICU) setting, not in the general medical ward. One study demonstrated in the medical ICU that IPC was no better than no prophylaxis at all.21 The researcher diagnosed upper or lower limb DVT in 32% receiving no prophylaxis, vs. 33% in patients using IPC devices. Another study also found IPC to be ineffective in the ICU setting.22 The researchers diagnosed lower limb DVT by Doppler ultrasonography in 25% of patients receiving no prophylaxis, vs. 19% in patients using IPC (P = 0.42). However, consistent data from trials with surgical patients suggest that both ES and IPC likely will modulate venous thrombosis to some degree and, unlike drug-based strategies, they carry no risk for hemorrhage.20 ES alone are unlikely to be helpful in contemporary medical patients, as they yield only modest risk reductions in low-risk surgical populations. On average, IPC devices have produced 40-50% relative risk reductions in even high-risk surgical groups, yet they have several significant limitations in the medically ill population. First, the mechanical devices must be worn continuously to maintain a protective effect, thus essentially placing the patient on bed rest. This increases VTE risk due to immobility and may significantly harm the hospitalized elder in regard to dependence for activities of daily living and the need for rehabilitation prior to returning home. Second, the devices are uncomfortable to wear, thereby destroying sleep hygiene. Poor sleep hygiene has been associated with episodes of delirium in hospitalized elderly patients.23 Finally, these devices simply have not been studied adequately in medical patients to recommend them as an alternative to pharmacologic strategies that have established efficacy. In fact, in its latest consensus statement on the use of antithrombotic therapy, the ACCP does not recommend non-pharmacologic strategies in general medical patients with clinical risk factors for VTE—only drug-based strategies carry the 1A recommendation. Use of ES or IPC strategies for the prevention of VTE in the medically ill population should be limited to those situations where the risk of bleeding is believed to exceed the risk of thrombosis. Such patients may include those with active bleeding, coagulopathy, or thrombocytopenia. (See Table 3.) However, these situations will be in the minority, and most medically ill patients will require drug-based prophylaxis.
Table 3.
Potential Contraindications
to Drug-
Based VTE Prophylaxis Strategies

Fact: LMWH Once Daily May Be Best Approach to Protect the Medically Ill Patient from VTE.
In general medical patients with risk factors for VTE, the ACCP recommends either low-dose unfractionated heparin (LDUH) twice or three times per day or daily low-molecular weight heparin (LMWH).20 (See Table 4.) However, a recent U.S. consensus panel has dropped LDUH twice daily as a recommended strategy, favoring LMWH over the uncommonly used LDUH every eight hours.24 Clinicians outside the United States already have adopted this approach. The IMPROVE registry documents that LMWH is the preferred pharmacologic VTE prophylaxis regimen for medical patients worldwide, in contrast to the United States, which still favors unfractionated heparin twice daily.25
Table 4. Low Molecular Weight Heparin vs. Unfractionated Heparin
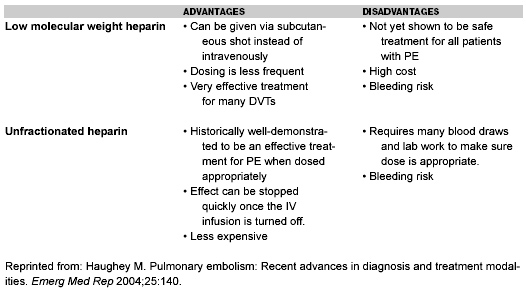
There is surprisingly little efficacy data with LDUH administered twice daily in heterogeneous medical patients. The only published placebo-controlled studies used tightly defined patient populations and were performed two decades ago.26,27 For those medical patients in the highest risk groups, such as in the medical ICU, the literature is conflicting.21,22 Furthermore, in a direct comparison trial in geriatric patients, LDUH twice daily was equivalent to placebo doses of LMWH.28 The best efficacy data with LDUH twice daily comes from ischemic stroke patients, not contemporary medical patients.29,30
Overall, LDUH administered twice daily has some evidence for efficacy, but the data is old and not representative of the general medical population seen in hospitals today. In contrast, LMWH efficacy has been studied in real-world patient populations. Samama and colleagues compared two different doses of enoxaparin (Lovenox) (20 mg or 40 mg) daily to placebo in the MEDENOX trial.15 The MEDENOX trial evaluated thromboprophylaxis in 1102 acutely ill medical patients who were at risk of thromboembolic complications due to severely restricted mobility. MEDENOX included general medical patients with acute disorders (average of 2.3 clinical risk factors), who were older than age 40, had projected hospital stays of fewer than six days, and previously had been immobilized for fewer than three days. Patients were randomized to placebo, enoxaparin 20 mg daily, or enoxaparin 40 mg daily for 6-14 days. The overall incidence of venographically detectable VTE was 14.9% in the placebo group (5% proximal DVT) vs. 5.5% in the enoxaparin group (P < 0.001). In this patient population, the 40 mg dose reduced the risk of VTE by 63%. No significant differences were found between the enoxaparin 20 mg dose and placebo in regards to efficacy. There was no increase in major bleeding or thrombocytopenia with either dose of enoxaparin compared to placebo. Recently, dalteparin (Fragmin) also has been FDA-approved for VTE prophylaxis in the medically ill patient. The PREVENT trial was a randomized, placebo-controlled trial in more than 3700 contemporary medically ill patients that demonstrated 5000 units of dalteparin daily reduced the incidence of DVT by 43% using clinical and duplex ultrasonography endpoints.31
LMWH has been compared to LDUH three times daily. One study32 compared 40 mg daily of enoxaparin to LDUH every eight hours in the PRIME study. The PRIME study was a multicenter, randomized, double-blind controlled trial in 959 patients who were immobilized for seven days, in addition to having another risk factor for VTE (i.e., congestive heart failure, malignancy, obesity, or age older than 60 years). There was no significant difference found between the two strategies by duplex ultrasonography (0.2% vs. 1.4%, P = NS); however, there was more bleeding in the LDUH group. Another study compared 40 mg daily of enoxaparin to LDUH every eight hours in more than 600 patients with severe respiratory diseases or congestive heart failure.33 Thromboembolic events were detected in 8.4% of patients receiving enoxaparin and 10.4% of those treated with LDUH (P = 0.015). In addition, overall bleeding occurred significantly more in the LDUH group compared to enoxaparin (3.6% vs. 1.5%, P < 0.05). Recently, McGarry and Thompson identified persons older than 40 years who were hospitalized for at least six days for an acute medical condition using a large, multihospital inpatient database.34 Patients then were selected if they received either 30-60 mg daily of enoxaparin (n = 479) or 5000 to 20,000 U daily of UFH (n = 2837) for VTE prophylaxis. The incidence of VTE was 64% lower (1.0% vs 2.9%) for the enoxaparin group vs. the UFH group (P = 0.02). Risks of major bleeds and mortality were similar in the two groups.
In summary, the weight of the evidence does not support the efficacy of LDUH twice daily in today’s medically ill patient. If LDUH is used, the escalated dose of 5000 units every eight hours is more appropriate. However, as Kleber et al have demonstrated, there are some patient populations where even the escalated dosing of LDUH is not as effective as LMWH given once daily.33
Fact: LMWH Is Safer with Respect to Bleeding than LDUH.
In the aforementioned FDA-labeling studies for both enoxaparin and dalteparin,15,31 neither strategy had greater major hemorrhage than the placebo injection. A meta-analysis on nine trials comparing LMWH to UFH in fixed doses (N = 4669) demonstrated significantly less bleeding with LMWH (0.4% vs 1.2%, P = 0.049).35 This represents a 52% risk reduction for major hemorrhage in favor of LMWH. Similar results have been found at weight-adjusted doses of LMWH as well—LMWH actually is less likely to bleed.36 For those rare patients that do suffer a major hemorrhage with LMWH, protamine sulfate will bind approximately 60% of the drug, and its anticoagulant effects are completely reversible with fresh frozen plasma.
The issue of safety would not be complete without taking heparin-induced thrombocytopenia (HIT) into consideration. (See Table 5.) HIT is an immune-mediated form of platelet activation that can lead to widespread thromboses throughout the body. HIT is the most severe adverse consequence of heparin therapy, and carries 30% mortality even when diagnosed immediately and treated with direct thrombin inhibitor. Recurrent VTE is the most common sequelae, with a 93-fold increased risk for PE.37 The incidence of HIT following five days of UFH therapy ranges between 3-6%, in contrast to LMWH, which ranges between 0.5-1%.38
Table 5.
Diagnosis of Heparin-induced
Thrombocytopenia (HIT)

Fact: LMWH Has Not Been Studied Adequately in Patients with Obesity or Elevated Creatinine.
LMWH has not been studied adequately in clinical trials in several important patient populations. These special patient groups include those with morbid obesity (> 150 kg) and those with severe renal insufficiency (CrCl < 30 mL/min). In contrast to renally insufficient patients, morbidly obese patients are at increased risk for VTE.19 In this setting, we are concerned more about the risk of thrombosis than the risk of hemorrhage. Recent post hoc analysis of cardiovascular trials using full weight-adjusted doses of LMWH and UFH found no differences in hemorrhage rates in obese and nonobese patients.39 In addition, LMWH has a theoretical advantage over UFH in morbidly obese patients as a result of higher fixed-dose subcutaneous bioavailability. However, Frederiksen et al found a significant correlation between body weight and the area under the curve of heparin concentration based on fixed LMWH dosing.40 Thus, even though LMWH already has greater subcutaneous bioavailability than UFH, this finding is probably the strongest evidence to date that escalated LMWH dosing may be necessary for effective VTE prophylaxis in obese patients. Gastric bypass surgical patients appear to benefit from escalated doses of LMWH given twice daily.41 Overall, LMWH should be viewed as the preferred pharmacologic strategy in the morbidly obese, not a contraindicated approach. Dosing may need to be individualized, depending on the patient and the clinical situation.
Patients with severe renal insufficiency are at increased risk for bleeding with pharmacologic prophylaxis (LMWH or UFH) in comparison to non-renally impaired patients.39 So, unlike morbidly obese patients, we are more concerned here with risk of hemorrhage. LMWH is cleared by the kidneys, and those with renal impairment will experience a prolonged elimination of the drug. This can lead to unintended high heparin levels over time, thus further increasing the risk for hemorrhage. However, it is important to use CrCl as the measurement of renal function, not a static creatinine value. Short courses (fewer than five days) of fixed-dose LMWH are unlikely to accumulate in patients with a CrCl greater than 20-30 ccs/min.42 For those patients requiring longer than one week of LMWH prophylaxis in the setting of renal insufficiency, an empiric reduction in the dose (30 mg enoxaparin daily) or increasing the dosing interval (40 mg every other day) is advised. Based on submitted pharmacokinetic data, current FDA guidelines for enoxaparin specifies 30 mg subcutaneously daily for medically ill patients with a CrCl less than 30 ccs/min. Clinicians should consider monitoring heparin concentrations via the anti-Xa assay for safe prophylaxis with LMWH in any patient who has a CrCl less than 10 ccs/min or for those patients on dialysis. Ultimately, in all patient assessments, the risk for bleeding must be weighed against the risk for thrombosis. Caution is advised in using UFH in renally impaired patients as well. Patients with high to very high risks for hemorrhage probably should not receive pharmacologic VTE prevention strategies; non-pharmacologic approaches would be preferred.
Fact: Increased Initial Costs of LMWH May Be Offset by Its Benefits.
Pharmacoeconomic data suggest that the increased initial cost of LMWH is more than offset by the benefits of lower morbidity and reduced hospitalization costs due to a reduction in VTE complications, recurrence, or adverse events related to prophylaxis.42,43 The results of a recent cost-analytic model indicate that thromboprophylaxis with 40 mg of enoxaparin daily is cost-effective in acutely ill medical patients compared to no prophylaxis.43 The authors emphasize that the effectiveness analysis in their model is consistent with the large body of clinical evidence demonstrating a better risk-to-benefit ratio when using LMWH rather than UFH for VTE prevention. Moreover, compared with thromboprophylaxis using UFH, enoxaparin prophylaxis was found to be cost-neutral.
Fact: Studies Are Examining the Potential Benefits of VTE Prophylaxis Outside the Hospital.
Several surgical populations have been studied in regard to the need to extend VTE prophylaxis out of the hospital setting. Patients who have undergone total hip replacement,44 or those who have undergone colorectal surgery for cancer,45 clearly benefit from as much as 30 days of prophylaxis out of the hospital. There is little evidence regarding when medically ill patients should discontinue prophylaxis. Most VTE prophylaxis trials in medical patients continued prophylaxis for 7-10 days. However, the DVT-FREE registry documented a significant portion of community DVT diagnoses were in patients hospitalized in the previous two weeks.3 Bosson et al46 performed a multicenter cross-sectional study on the risk factors, prophylaxis, and prevalence of VTE in subacute care facilities in France (n = 852). The rate of VTE anticoagulant prophylaxis was high (56%). DVT was noted by duplex ultrasonography in 16%, with a 6% rate of proximal DVT. There is no report of whether any of the subacute patients received prophylaxis in the acute care setting first, thus the impact of the results is limited. However, clearly this is a population at risk, with a surprisingly high rate of proximal thrombosis observed.
Most patients have not returned to baseline health at the time of hospital discharge. Therefore, it is unlikely that the elevated risk for VTE that occurs in the hospitalized setting becomes negligible in the immediate convalescent phase that occurs upon hospital discharge. The benefit of extending prophylaxis out of the hospital for acutely ill medical patients with prolonged immobilization currently is under investigation in the EXCLAIM trial. More than 3000 patients have been enrolled to date, and initial results are expected in the second half of 2005. Patients who still are in a monitored setting, such as a skilled nursing facility, will benefit from continued pharmacologic prophylaxis. For patients who are discharged home, the issue of safety becomes paramount. Patients should be considered for their risk for thrombosis as well as their risk for bleeding in an unmonitored environment. The EXCLAIM trial should best define safety and appropriate candidates for out-of-hospital prophylaxis.
Review of the Facts
The consistent evidence for inadequate VTE prophylaxis in most medically ill patients nationwide has been aptly described as the failure to prevent syndrome. The reasons for this failure are many, but the facts speak for themselves. The National Quality Forum (NQF) recently released a report that details 30 health care safe practices that should be utilized universally in applicable clinical care settings to reduce the risk of harm to patients.47 The 30 priority safe practices have been culled from an original pool of more than 220 candidate practices, based on each practice’s specificity, effectiveness, potential benefit, generalizability, and readiness for implementation. This set of safe practices has been reviewed carefully and endorsed by a diverse group of stakeholders, including the Joint Commission on the Accreditation of Healthcare Organizations (JCAHO) and the Centers for Medicare and Medicaid Services (CMS), pursuant to the National Quality Forum’s formal Consensus Development Process. The NQF best safe practice No. 17 is: "Evaluate each patient upon admission and regularly thereafter for the risk of developing deep vein thrombosis (DVT)/venous thromboembolism (VTE). Utilize clinically appropriate methods to prevent DVT/VTE." In similar efforts to address the "failure to prevent syndrome," JCAHO currently is reviewing VTE prophylaxis as a core quality measure to be added to their 225 hospital standards for accreditation, and CMS is investigating whether to add VTE prophylaxis as a future measure of hospital quality that will require public reporting.
All general medical patients should be assessed for clinical risk factors for VTE, recognizing that the majority will have multiple risk factors. Consensus panels recommend that general medical patients with clinical risk factors receive drug-based prophylaxis. Current evidence does not support the routine use of twice daily LDUH in today’s acutely ill medical inpatient. LDUH three times daily may be efficacious in most medical patients; however, it is associated with an increased risk for bleeding and HIT. The preferred strategy for prevention in the medically ill population deemed to be high to very high risk for VTE is LMWH. (See Figure 1.)
Figure 1. Rational Approach to VTE Prophylaxis in Hospitalized Patients
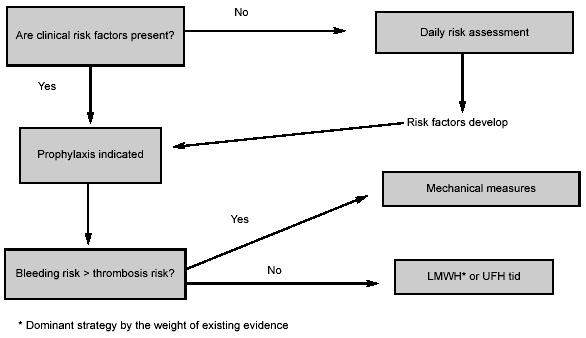
For those patients who have a high to very high risk for bleeding, non-pharmacologic strategies such as ES or IPC devices are recommended. (See Table 6.)
Table 6. Prevention of DVT and PE

References
1. Hirsh J, Hoak J. Management of deep vein thrombosis and pulmonary embolism: A statement for healthcare professionals. Council on Thrombosis, American Heart Association. Circulation 1996;93:2212-2245.
2. Heit JA, Silverstein MD, Mohr DN, et al. Predictors of survival after deep vein thrombosis and pulmonary embolism: A population-based cohort study. Arch Intern Med 1999;159: 445-453.
3. Goldhaber SZ, Tapson VF. A prospective registry of 5,451 patients with ultrasound-confirmed deep vein thrombosis. Am J Cardiol 2004;93:529-262.
4. Hull RD, Pineio GF. Clincial features of deep venous thrombosis. In: Hull RD, Raskob GE, Pineo GF, eds. VTE: An Evidence-based Atlas. Armonk, NY: Futura Publishing. 1996; 87-91.
5. Goldhaber SZ, Savage DD, Garrison RJ, et al. Risk factors for pulmonary embolism. The Framingham Study. Am J Med 1983;74:1023-1028.
6. Anderson FA Jr, Wheeler HB, Goldberg RJ, et al. A population-based perspective of the hospital incidence and case-fatality rates of deep vein thrombosis and pulmonary embolism. The Worcester DVT Study. Arch Intern Med 1991;151:933-938.
7. Michota FA. Venous thromboembolism prophylaxis in the medically ill patient. Clin Chest Med 2003;24:93-101.
8. Prandoni P, Lensing AW, Cogo A, et al. The long-term clinical course of acute deep venous thrombosis. Ann Intern Med 1996;125:1-7.
9. Bergqvist D, Jendteg S, Johansen L, et al. Cost of long-term complications of deep venous thrombosis of the lower extremities: An analysis of a defined patient population in Sweden. Ann Intern Med 1997;126:454-457.
10. Agency for Healthcare Research and Quality: Healthcare Cost and Utilization Project. HCUPNet. Available at: http://hcup.ahrq.gov/HCUPnet.asp.
11. Fink S, Chaudhuri TK, Davis HH. Pulmonary embolism and malpractice claims. South Med J 1998;91:1149-1152.
12. Physicians Insurance Website. Pulmonary embolus: The silent killer. September/October 1996 - Volume VII, Number 5. Available at: http://phyins.com/pi/risk/updates/sepoct96.html. Accessed 9/30.2004.
13. Sandler DA, Martin JF. Autopsy proven pulmonary embolism in hospital patients: Are we detecting enough deep vein thrombosis? J R Soc Med 1989;82:203-205.
14. Silverstein MD, Heit JA, Mohr DN, et al. Trends in the incidence of deep vein thrombosis and pulmonary embolism: A 25-year population-based study. Arch Int Med 1998;158: 585-593.
15. Samama MM, Cohen AT, Darmon JY, et al. A comparison of enoxaparin with placebo for the prevention of VTE in acutely ill medical patients. N Engl J Med 1999;341:793-800.
16. Cohen A, Davidson BL, Gallus AS, et al. Fondaparinux for the prevention of VTE in acutely ill medical patients. Blood 2003;102:15a.
17. Heit JA, O’Fallon M, Petterson T, et al. Relative impact of risk factors for deep vein thrombosis and pulmonary embolism. Arch Intern Med 2002;162:1245-1248.
18. Salzman EW, Hirsh J. The epidemiology, pathogenesis, and natural history of venous thrombosis. In: Colman RW, Hirsh J, Marder VJ, et al, eds. Hemostasis and Thrombosis: Basic Principles and Clinical Practice, 3rd ed. Philadelphia, PA: Lippincott, 1994; 1275-1296.
19. Anderson FA Jr, Wheeler HB, Goldberg RJ, et al. The prevalence of risk factors venous thromboembolism among hospital patients. Arch Intern Med 1992;152:1660-1664.
20. Geerts WH, Pineo GF, Heit JA, et al. Prevention of venous thromboembolism. Chest 2004;126:338s-400s.
21. Hirsch DR, Ingenito EP, Goldhaber SZ. Prevalence of deep venous thrombosis among patients in medical intensive care. JAMA 1995;274:335-337.
22. Marik PE, Andrews L, Maini B. The incidence of deep venous thrombosis in ICU patients. Chest 1997;111:661-664.
23. Inouye SK, Schlesinger M, Lydon T. Delirium: A symptom of how hospital care is failing older persons and a window to improve quality of hospital care. Am J Med 1999;106: 565-573.
24. Bosker G. Prophylaxis of venous thromboembolism (VTE) in the hospitalized medical patient. Hospital Medicine Consensus Reports. Dec. 1, 2003:1-20.
25. Tapson VF, Decousus H, Piovella F, et al. A multinational observational cohort study in acutely ill medical patients of practices in prevention of venous thromboembolism: Findings of the international medical prevention registry on venous thromboembolism (IMPROVE). Blood 2003; 102:321a.
26. Cade JF. High-risk of the critically ill for VTE. Crit Care Med 1982;10:448-450.
27. Ibarra-Perez K, Sandset PM. A double-blind and randomized placebo-controlled trial of low dose heparin in the intensive care unit. Semin Thromb Haemost 1988;11:25-33.
28. Bergmann J-F, Neuhart E. A multicenter randomized double-blind study of enoxaparin compared with unfractionated heparin in the prevention of venous thrombembolic disease in elderly inpatients bedridden for an acute medical illness. Thromb Haemost 1996;76:529-534.
29. McCarthy ST, Turner JJ, Robertson D, et al. Low-dose heparin as a prophylaxis against deep-vein thrombosis after acute stroke. Lancet 1977;2:800-801.
30. McCarthy ST, Turner JJ. Low-dose subcutaneous heparin in the prevention of deep vein thrombosis and pulmonary emboli following acute stroke. Age Ageing 1986;15:84-88.
31. Leizorovicz A, et al. A randomized placebo controlled trial of dalteparin for the prevention of venous thromboembolism in 3706 acutely ill medical patients: The PREVENT medical thromboprophylaxis study. J Thromb Haemost 2003;1(Suppl 1):OC396.
32. Lechler E, Schramm W, Flosbach CW, et al. The venous thrombotic risk in non-srugical patients: Epidemiological data and efficacy/safety profile of a low-molecular weight heparin. Haemostasis 1996; 26(suppl 2):49-56.
33. Kleber FX, et al. Randomized comparison of enoxaparin with unfractionated heparin for the prevention of venous thromboembolism in medical patients with heart failure or severe respiratory disease. Am Heart J 2003;145:614-621.
34. McGarry LJ, Thompson D. Prevention of venous thromboembolism with enoxaparin versus unfractionated heparin in acutely-ill medical inpatients. Blood 2003;102:320a.
35. Mismetti P, Laporte-Simitsidis S, Tardy B, et al. Prevention of venous thromboembolism in internal medicine with unfractionated or low-molecular weight heparins: A meta-analysis of randomized clinical trials. Thromb Haemost 2000;83:14-19.
36. Gould MK, Dembitzer AD, Doyle RL, et al. Low-molecular-weight heparins compared with unfractionated heparin for treatment of acute deep venous thrombosis. A meta-analysis of randomized, controlled trials. Ann Intern Med 1999;130: 800-809.
37. Warkentin TE. Heparin-induced thrombocytopenia: A clinicopathologic syndrome. Thromb Haemos 1999;82:439-437.
38. Warkentin TE, Kelton JG. A 14-year study of heparin-induced thrombocytopenia. Am J Med 1996;101:502-507.
39. Spinler A, Inverso SM, Cohen M, et al. ESSENCE and TIM 11B Investigators. Safety and efficacy of unfractionated heparin versus enoxaparin in patients who are obese and patients with severe renal impairment: Analysis from the ESSENCE and TIMI 11B studies. Am Heart J 2003;146: 33-41.
40. Frederiksen SG, Hedenbro JL, Norgren L. Enoxaparin effect depends on body-weight and current doses may be inadequate in obese patients. Br J Surg 2003;90:547-548.
41. Scholten DJ, Hoedema RM, Scholten SE. A comparison of two different prophylactic dose regimens of low molecular weight heparin in bariatric surgery. Obesity Surg 2002;12: 19-24.
42. Lamy A, Wang X, Kent R, et al. Economic evaluation of the MEDENOX trial: a Canadian perspective. Can Respir J 2002;9:169-177.
43. Lloyd AC, Anderson PM, Quinlan DJ, et al. Economic evaluation of the use of enoxaparin for thromboprophylaxis in acutely ill medical patients. J Med Econ 2001;4:99-112.
44. Dobesh PP. Novel concepts: Emerging data and the role of extended prophylaxis following hip fracture surgery. Am J Health Syst Pharm 2003;60(suppl 7):S15-S19.
45. Bergqvist D, ENOXACAN Study Group. Efficacy and safety of enoxaparin versus unfractionated heparin for prevention of deep vein thrombosis in elective cancer surgery: A double-blind randomized multicentre trial with venographic assessment. Br J Surg 1997;84:1099-1103.
46. Bosson JL, Labarere J, Sevestre MA, et al. Deep vein thrombosis in elderly patients hospitalized in subacute care facilities: a multicenter cross-sectional study of risk factors, prophylaxis, and prevalence. Arch Intern Med 2003;163: 2613-2618.
47. Safe Practices for Better Healthcare: A Consensus Report. National Quality Forum; 2003. Available at: www.qualityforum.org. Accessed 9/30/2004.
Physicians increasingly are aware of the need to provide prophylaxis against venous thrombosis for the medically ill patient in the hospital environment. This article attempts to separate the fact from fiction regarding VTE prophylaxis.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
