Timing is key for cauda equina syndrome diagnosis in the ED
By Charles E. Rawlings, MD, JD, Rawlings Neurosurgical Consulting/The MacKenzie Law Firm, Winston-Salem, NC.
Editor’s note: Low back pain is a frequent patient complaint in the emergency department (ED). In fact, the same patients may visit the ED repetitively with the same complaint. It is easy to be assuaged into thinking that these patients are merely seeking drugs, but to make that assumption can lead a clinician to miss the cauda equina syndrome and may result in a malpractice action if efforts are not taken to identify any new symptoms and signs in a patient with low back pain. This issue provides the reader with a solid understanding of diagnosing and caring for patients with cauda equina syndrome in the ED and the medicolegal issues that arise from failing to diagnose and appropriately treat these patients.
Introduction
A 25-year-old healthy male lifts a heavy piece of machinery while at work and immediately suffers low back and bilateral leg pain. The company physician places him on bed rest for one week. At the end of the week, the injured worker continues to experience both severe back and leg pain. He presents to his local ED with complaints of back and leg pain with no neurological findings, except for a positive straight leg raise. He is discharged home only to return the next day with urinary incontinence and a weak foot. An emergent magnetic resonance imaging (MRI) scan reveals a large ruptured disc at the L3-L4 level. Surgery is performed immediately, but the man has permanent bladder problems. He files suit against the ED for failure to diagnose his cauda equina syndrome.
A 50-year-old male with diabetes, hypercholesterolemia, hypertension, and chronic low back pain presents to the ED with an increase in his low back pain as well as a several-week history of urinary incontinence. The patient’s neurological examination essentially is normal, except for absent ankle reflexes. The ED physician obtains plain lumbar X-rays that show moderate degenerative changes. The patient is discharged home with follow-up to his local physician. Several days later, the same patient presents to a different ED with acute urinary retention. An emergent MRI reveals a large ruptured disc at the L4-L5 level. The patient undergoes emergency surgery, has permanent bladder dysfunction, and subsequently files suit against the first ED for failure to diagnose a cauda equina syndrome.
A 40-year-old otherwise healthy male presents to his local ED after work with a several-day history of severe back and right leg pain. His neurological examination reveals a weak (4/5) extensor hallucis longus on the right. Plain radiographs are normal, and the patient is discharged home with pain medications. The following morning, the same patient presents to the ED with increasing pain, increasing weakness, and difficulty voiding. Neurological examination essentially is unchanged from the previous evening, but the patient is unable to void without catheterization. The ED physician waits 12 hours to call an orthopedist, who waits until the next morning to obtain an MRI scan. The scan reveals a ruptured disc at the L3-L4 level. The patient undergoes surgery that afternoon but is left with permanent bladder dysfunction. The patient brings suit against the ED for failure to diagnose and treat his cauda equina syndrome in a timely manner.
The scenarios illustrate routine encounters in the ED involving the failure to diagnose and to treat cauda equina syndrome. In the first example, no medical negligence occurred; the patient did not have cauda equina syndrome upon his first visit to the ED. The next day, when the patient did have urinary symptoms, the management of the patient comported with the applicable standard of care.
In the second example, no medical negligence occurred for essentially the same reasons. The patient did not have acute cauda equina syndrome upon presentation to the first ED and as such received treatment that comported with the applicable standard of care. In the third example, the medical negligence should be obvious regarding both the treatment in the ED as well as the orthopedist’s treatment of the patient. Acute cauda equina syndrome is a neurological emergency and investigative procedures as well as treatment should be instituted as soon as possible. Both the ED physician’s delay in consultation and the orthopedist’s delay in ordering an MRI scan and performing surgery breached the applicable standard of care.
The most common causes of ED malpractice arise from misdiagnosis, the failure to diagnose, and the lack of consultation with appropriate specialists. Most failure-to-diagnose cases involve the failure to diagnose appendicitis, myocardial infarction, meningitis, ectopic pregnancy, and fractures.1 Although cauda equina syndrome is not among those entities most commonly misdiagnosed in the ED, it is accompanied by a common ED complaint — low back and leg pain — and if not properly diagnosed and treated, the condition carries high rates of morbidity, including permanent weakness, sensory loss, and bladder/bowel dysfunction.2,3 Therefore, a patient who presents to the ED with signs and symptoms compatible with cauda equina syndrome must be approached in a thorough, careful, and timely manner to exclude the possibility of acute cauda equina syndrome and its attendant need for emergency imaging and surgery.
Overview
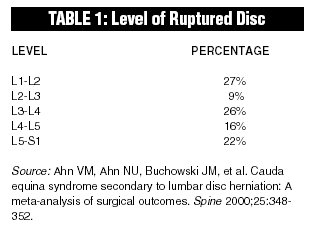
Cauda equina syndrome is a severe neurological disorder first described by Mixter and Barr in 1934.4 The disorder can be caused by any entity exerting pressure upon the cauda equina including hema-tomas, tumors, infections, or fractures. More importantly, however, 2%-6% of lumbar disc herniations result in cauda equina syndrome.5-10 As a consequence, if a patient is encountered in the ED suffering from cauda equina syndrome, most likely the cauda equina compression is secondary to a disc herniation and not a tumor, hematoma, or other entity (see Table 1).
Although some authors have grouped patients with differing degrees of urinary dysfunction into separate categories,11,12 most define cauda equina syndrome as a neurological disorder characterized by the clinical features of low back pain, bilateral or unilateral leg pain (radiculopathy), saddle anesthesia, motor weakness, sensory deficit, and bladder or bowel incontinence (see Table 2).5-10 Significantly, the syndrome may progress to paraplegia and/or permanent bladder or bowel incontinence.5,6

Cauda equina syndrome is one of several neurological clinical entities known as epidural compression syndromes. Epidural compression syndromes result from a disease process arising from the epidural space that causes pressure on the neurological elements contained in that space. Such disease processes commonly include tumors, infections, degenerative processes (spinal stenosis and ruptured discs), trauma, congenital abnormalities, hematomas, and other rare conditions, such as lipomas and spinal arteriovenous malformations. The clinical manifestations directly correlate with the anatomical structure affected by the compression. As a result, epidural compression syndromes include spinal cord compression, conus medullaris syndrome, and of course, the cauda equina syndrome. A detailed discussion of spinal cord compression is beyond the scope of this article, but in short, cord compression presents as an acute or gradual reduction in spinal cord function below the level of the lesion. Neurological deficits associated with spinal cord compression include motor weakness progressing to quadriplegia and paraplegia, sensory dysfunction progressing to a complete sensory level, reflex changes, and bladder and bowel dysfunction. Cord compression, particularly acute cord compression, is distinguished easily from cauda equina syndrome and generally does not present problems from an ED diagnostic or management standpoint.
However, conus medullaris syndrome, while being a true spinal cord compression syndrome, can resemble cauda equina syndrome, particularly in an ED setting. The actual conus medullaris is the lower section of the spinal cord that tapers to an end generally at the L1-L2 level. Originating from the conus medullaris are the lower spinal nerve roots arising from spinal cord segments L4-S1. These spinal nerve roots comprise the actual cauda equina, and both the conus medullaris and cauda equina are contained in the thecal sac surrounded by cerebrospinal fluid. Because of this anatomical arrangement, the spinal cord lies in close proximity to the nerve roots and thus, any pressure in this T12-L1-L2 region can result in both spinal cord compression and nerve root compression with their concomitant signs and symptoms. Generally, a conus medullaris syndrome presents as a result of trauma and with much less pain than a cauda equina syndrome. Conus lesions generally are symmetric and generally are associated with a saddlelike distribution of sensory loss. Cauda equina lesions, on the other hand, should be considered multiple radiculopathies with their associated characteristic asymmetric neurological deficits, significant pain, and radicular findings. In reality, however, a conus medullaris syndrome can be confused easily with a cauda equina syndrome.
Regardless of the actual syndrome involved, diagnosis and management in the ED varies little between the two entities. Both generally are viewed as neurological emergencies and should be investigated and treated as such. For both entities, MRI scanning is the diagnostic tool of choice and emergency surgery is the treatment of choice. Unfortunately, prognosis is affected by the location of the lesion. As might be expected, patients with conus medullaris involvement generally have a poorer outcome when compared with the patients with cauda equina syndrome. Such a poor outcome is due to the actual spinal cord involvement seen in the patients with conus medullaris lesions.
The majority of lumbar disc herniations can be managed conservatively with surgery used only as a last resort for patients who experience increasing neurological deficits or who experience no clinical improvement following appropriate conservative measures. Cauda equina syndrome, on the other hand, generally is treated as a true surgical emergency. As Ahn notes, "It [cauda equina syndrome] is thought to be the primary absolute indication for the acute surgical treatment of lumbar disc herniation."5
A published comment following Shapiro’s article noted: "The reader should not be left with the impression that it is acceptable to wait up to 48 hours before surgery. The sooner the cauda equina is decompressed after the onset of symptoms the more likely it is that the patient will not be left with residual neurological deficits."6
Although patients with cauda equina syndrome may present to their family practitioners or even specialists such as neurosurgeons or orthopedists, many more present to the ED for initial evaluation and treatment. As mentioned previously, many patients present to the ED with a primary complaint of low back pain or radiculopathy, and only upon taking a history during a physical does the true nature of the complaint become apparent. Therefore, ED personnel frequently are involved in the initial evaluation and treatment of a patient with cauda equina syndrome, and may trigger events that lead to medicolegal difficulties. Such acts or omissions include failure of the nursing staff to document and communicate a patient’s symptoms, signs, or progression thereof; failure of a physician to obtain an accurate, thorough history accompanied by a complete physical and neurological examination, including a rectal examination; failure of the physician to recognize cauda equina syndrome; failure to obtain emergency imaging, consultation, or referral once a patient is diagnosed with cauda equina syndrome; failure to discuss the need for prompt return if bladder or bowel problems arise once the patient is discharged; and finally, discharging a patient without ruling out the presence of cauda equina syndrome.6,8,9
In the ED setting, the most important aspect of cauda equina syndrome is the need for early diagnosis and early referral leading to surgical treatment within 48 hours of the onset of symptoms.6,8,9 The following cases illustrate instances of cauda equina syndrome that generated medicolegal consequences.
Case #1
In Gustavo Landin and Patricia Landin v. Roland Zachow, PA, Thomas Strawmyer, MD, and Concentra Health Services, Inc. d/b/a Concentra Medical Center,13 the plaintiff and his wife brought a medical negligence suit based upon an alleged failure to diagnose the plaintiff’s progressive cauda equina syndrome. The defendants included the physician assistant, the supervising physician, and the hospital.
In January 1998, Mr. Gustavo Landin, a steel factory worker, sustained a significant on-the-job back injury resulting in severe low back pain and bilateral, radiating, leg pain. Mr. Landin was sent to Concentra Medical Center for evaluation, work-up, and treatment.
Upon arrival at Concentra Medical Center, Mr. Landin was seen and evaluated by Roland Zachow, a physician assistant under the supervision of Thomas Strawmyer, MD. Upon presentation, Mr. Landin complained of severe lower back pain as well as bilateral, lower extremity radiating pain. When requested to provide a urine sample, Mr. Landin was unable to do so. Neither Mr. Zachow nor Dr. Straw-myer performed any further testing upon or diagnostic evaluations of Mr. Landin.
Mr. Landin subsequently was assigned the diagnosis of lower back strain and discharged to home. The medical records noted that an L5-S1 injury had been ruled out, although the procedure by which it had been so was not specified. Mr. Landin was given a prescription for physical therapy and pain medication but received no instruction or warnings with regard to any bladder problems.
The following morning, Mr. Landin returned to Concentra Medical Center with continued severe pain radiating down both legs, perineal numbness, and bladder distension with incontinence. Mr. Landin underwent immediate bladder catheterization resulting in removal of 1400 cc urine; normal bladder capacity is 200 cc to 400 cc. A neurosurgeon was consulted immediately, diagnosed Mr. Landin with cauda equina syndrome, and performed emergency surgery.
Following surgery, Mr. Landin was left with permanent bladder dysfunction, permanent sexual dysfunction, and the need for enemas to stimulate bowel movements. During the course of the suit, Mr. Landin’s neurosurgical expert testified that the delay in diagnosing his cauda equina syndrome resulted in his permanent bladder, bowel, and sexual dysfunction. The case settled for a confidential amount prior to trial.
Discussion
The Landin case illustrates several important points regarding the failure to diagnose cauda equina syndrome in an acute setting. The first principle involves a patient who presents with severe low back pain and bilateral lower extremity radiculopathy accompanied by bladder dysfunction. Although cauda equina syndrome following a traumatic event is somewhat uncommon, as has been noted previously, its hallmarks are severe low back pain, bilateral sciatica, and urinary dysfunction.5-10,14 Shapiro noted that in 70% of patients presenting with cauda equina syndrome, bilateral sciatica heralded the impending cauda equina compression, while the other 30% of patients presented with the fully developed syndrome.6-8 In addition, he noted that urinary retention always preceded urinary incontinence and that "it is important to recognize these patients and to not treat them conservatively." 8 Such a failure would or could be classified under the failure to diagnose cauda equina syndrome or the failure to recognize the syndrome even in the face of positive clinical signs and symptoms.
In Mr. Landin’s case, both the physician assistant and supervising physician failed to diagnose cauda equina syndrome as well as failed to recognize and investigate the syndrome. Mr. Landin presented with severe lower back pain and bilateral sciatica/radiculopathy accompanied by an inability to urinate (urinary retention). His presentation fits with the clinical syndrome of cauda equina syndrome, and he should have been diagnosed, investigated with appropriate radiographic studies (e.g., MRI), and treated for such in a timely manner. By failing to do so, both the physician assistant and physician breached the applicable standard of care in their treatment of Mr. Landin.
Another issue presented in the Landin case involves the follow-up instructions regarding bladder or bowel symptoms provided to a patient with severe back pain and sciatica who is discharged and treated conservatively. Cauda equina syndrome can progress to complete bladder dysfunction, but it does not exist until bladder dysfunction is noted in a patient.5-10 In fact, most authors define the onset of cauda equina syndrome by the onset of bladder or bowel dysfunction.5-10,15 More importantly, as Shapiro notes, more than 85% of patients develop the signs and symptoms of cauda equina syndrome during a period of a few hours. As a result, it is incumbent upon health care personnel who discharge patients with severe back and leg pain to instruct them in the proper procedure for emergency follow-up if bladder or bowel symptoms occur. In a patient with severe back and leg pain, conservative therapy can be appropriate. In a patient who develops bladder dysfunction and is classified as suffering from cauda equina syndrome, emergent diagnosis and treatment is indicated. The above comports with the issues raised in Kostuik’s publications where he noted that cauda equina syndrome must be viewed as a surgical emergency and that its treatment or lack thereof can generate multiple medicolegal controversies for the ED and its personnel. 6-9
In Mr. Landin’s case, no health care worker provided follow-up instructions to him regarding bladder dysfunction and the need for urgent return or follow-up care. By failing to emphasize the possibility of bladder dysfunction and the need for emergent follow-up, the physician assistant and physician who discharged the patient with bladder retention in association with the severe back pain and bilateral sciatica breached the applicable standard of care.
Case #2
In Sullivan v. Johnson,16 the female plaintiff filed a medical malpractice suit based upon a failure to timely diagnose a cauda equina syndrome when she presented to an ED with complaints of back pain and a "numb crotch." She alleged that the delay in diagnosis resulted in her permanent bladder and bowel dysfunction. The defendant named in the suit was the ED physician who allegedly failed to diagnose Ms. Sullivan’s cauda equina syndrome.
In 1990, Ms. Sullivan, a 35-year-old female, presented to her local ED with the chief complaint of low back pain and a "numb crotch." Ms. Sullivan was seen and evaluated during her initial visit by the ED physician, Dr. Johnson. She subsequently was discharged to home for conservative treatment with appropriate discharge instructions.
After approximately six hours, Ms. Sullivan experienced a feeling of bladder fullness but was unable to void (urinary retention). She immediately phoned the same ED and spoke with Dr. Johnson, who advised her to return immediately to the ED. Ms. Sullivan did as she was instructed.
During her second visit to the ED, Ms. Sullivan was diagnosed as suffering from cauda equina syndrome. She underwent emergency surgery for decompression of her cauda equina. Ms. Sullivan suffered permanent bladder and bowel dysfunction with urinary difficulty and the need for mechanical bowel stimulation.
During the course of the trial, Ms. Sullivan’s emergency medicine expert testified that Dr. Johnson breached the applicable standard of care by failing to diagnose cauda equina syndrome during the first ED visit. Both the plaintiff’s treating orthopedist and emergency medicine expert testified that her permanent bladder and bowel dysfunction resulted from the delay in diagnosis. However, Dr. Johnson testified that the plaintiff never complained of a "numb crotch." Moreover, his neurosurgical expert testified that Dr. Johnson did not breach the standard of care and could not make the diagnosis of cauda equina syndrome based solely on low back pain. Additionally, he testified that diagnosis and treatment at the time of the plaintiff’s first ED visit would not have changed the outcome. The jury found for the defendant.
Discussion
The Sullivan case illustrates several points regarding the ED treatment of a patient with possible cauda equina syndrome. The first point deals with the diagnosis. The diagnosis of cauda equina syndrome is not appropriate until bladder or bowel dysfunction exists in a patient.2,3,5-9 In addition, the first manifestation of bladder dysfunction in a patient with cauda equina syndrome is generally urinary retention.6,8 The urinary retention subsequently progresses to urinary incontinence with continued pressure on the cauda equina.6-8 Although bladder dysfunction can progress rapidly over several hours in a patient with potential cauda equina syndrome, the syndrome cannot be diagnosed in a patient whose only complaints are back pain and a numb crotch and who lacks any associated bladder dysfunction.
Ms. Sullivan presented to the ED with an undisputed chief complaint of back pain and possibly a "numb crotch." At no point did she complain of or exhibit any bladder dysfunction. Ms. Sullivan was discharged with a normal bladder. Based upon her complaints and absence of bladder dysfunction, Ms. Sullivan could not be diagnosed with cauda equina syndrome during her first ED visit inasmuch as her symptoms did not constitute the clinical entity of cauda equina syndrome. Ms. Sullivan did not develop the earliest bladder dysfunction manifested by patients with cauda equina syndrome — bladder retention — until six hours after her initial visit. Moreover, when she telephoned for instructions regarding her new symptoms, Dr. Johnson recognized the emergent nature of her condition and advised her appropriately. When she arrived at the ED, her new cauda equina syndrome was treated appropriately. The jury correctly found for the defendant.
Developed more thoroughly in a later case, the issue of timing of treatment for cauda equina syndrome as it relates to permanent sequelae is touched upon in the Sullivan case: The earlier diagnosis and treatment for cauda equina syndrome, the better. During the early period of cauda equina research, most researchers recommended that surgical decompression be performed within six hours of the onset of acute urinary symptoms in patients with cauda equina syndrome.7
As more investigation on cauda equina syndrome has been accomplished, the six-hour window has been increased to between 24 and 48 hours. Most researchers and clinicians now believe that a good outcome can be achieved in a patient who undergoes surgery within 24 to 48 hours of onset of their cauda equina syndrome, while significantly poorer outcomes are associated with surgical intervention after 48 hours.2, 3, 5-10
In the Sullivan case, Ms. Sullivan presented within six hours of her first visit to the ED with the first onset of urinary retention. She subsequently underwent emergent diagnostic evaluation and emergency surgery. Although the case does not specify the number of hours, her surgery was clearly within 24 hours of her first urinary symptoms, and in fact, was within 24 hours of her first presentation to the ED. Therefore, her treatment falls within the accepted time period for emergency surgical decompression. Moreover, based upon the current literature, a diagnosis and possible treatment six hours earlier would not have had a measurable effect upon her outcome. The defendant’s neurosurgical expert was correct in testifying that earlier treatment at the time of her first ED visit would not have altered her ultimate outcome. On both the issues of liability and causation, the Sullivan jury was correct from a medical standpoint.
Case # 3
In William Moore v. Little Falls Hospital; Victor Osinaga, MD, OM Wadhera, MD, and Richard Chemielewski, MD,17 the plaintiff brought a medical negligence suit based upon the alleged failure to diagnose cauda equina syndrome, failure to make a timely referral, and failure to perform appropriate diagnostic tests. As a result of these failures, the plaintiff alleged that he had suffered permanent sensory loss as well as permanent bladder and bowel dysfunction. The defendants included the two ED physicians as well as the hospital that staffed and operated the ED.
In August 1993, Mr. William Moore, a 29-year-old male, injured his lower back lifting a heavy object while at work, which resulted in lower back pain. On Oct. 6, 1993, because of his lower back pain, Mr. Moore went to the ED at Little Falls Hospital and was evaluated by Dr. Osinaga, who obtained a history, performed a physical examination, and obtained plain lumbar radiographs. The x-rays were read as normal. Dr. Osinaga diagnosed Mr. Moore with low back syndrome and discharged him back to work.
On Oct. 10, 1993, Mr. Moore collapsed because of low back pain while on the job and was returned to the same ED where Dr. Chemielewski evaluated him. During this second visit, Mr. Moore complained of right lower extremity sciatica as well as the continuing lower back pain. Dr. Chemielewski examined Mr. Moore, diagnosed him with low back strain accompanied by right sciatica, and discharged him to home on conservative treatment, which included bed rest, work abstention, and medications.
On Oct. 18, Mr. Moore again presented to the ED with complaints of low back pain and lower extremity numbness. He was seen, examined, and released by Dr. Wadhera. On Oct. 20, Mr. Moore was referred to a neurosurgeon following new complaints of bladder dysfunction. The neurosurgeon diagnosed Mr. Moore as having cauda equina syndrome and performed emergency surgery. Following surgery, Mr. Moore suffered permanent bladder, bowel, and sexual dysfunction as well as sensory dysfunction.
During the trial, Mr. Moore claimed that he complained of bladder and bowel symptoms during the course of his ED treatment. The medical records and notes contained no documentation of any of those complaints. Moreover, during the early course of his treatment, Mr. Moore continued working. The jury returned a verdict for the defense.
Discussion
The Moore case illustrates many of the same points as the previous cases regarding the ED treatment of a patient with possible cauda equina syndrome. The case also illustrates several nuances regarding evaluating a patient with back and leg pain in the ED. Again, cauda equina syndrome only can be diagnosed in a patient with bladder symptoms; the patient may present with myriad symptoms, but such symptoms must include bladder complaints (see Table 2).2,3,5-9 A diagnosis of cauda equina syndrome cannot be based upon a patient’s complaints of back pain alone or even back pain in combination with lower extremity pain. In addition, a diagnosis of cauda equina syndrome cannot be made based only upon findings in a patient of weakness or numbness. All those signs and symptoms may be present in a patient with cauda equina syndrome, but without bladder symptoms, such signs and symptoms alone are not sufficient to establish the diagnosis of cauda equina syndrome. The majority of patients with back pain, radiculopathy, or even ruptured discs can be treated conservatively with bed rest, medications, physical therapy, and other related treatments.5,6 In fact, cauda equina syndrome is the only true indication for emergency surgery in a patient with a herniated disc.6,8,9

In the Moore case, Mr. Moore presented multiple times to the same ED during the course of several weeks with back and leg pain resulting from an accident that occurred months prior to his ED visit. During each of his visits, Mr. Moore complained of back pain, leg pain, and leg numbness but never complained of any bladder or bowel dysfunction. Mr. Moore was evaluated and examined by three different physicians, none of whom documented any complaints of bladder or bowel dysfunction. Therefore, Mr. Moore was not suffering from cauda equina syndrome during any of his ED evaluations. He was treated with the appropriate conservative therapy upon his discharge from the ED. This appropriate conservative therapy included bed rest, work abstinence, and medications; all modalities used to treat back and leg pain caused by a ruptured disc. At no time did the ED physicians breach the applicable standard of care regarding their diagnosis and treatment of Mr. Moore.
The Moore case also illustrates the importance of obtaining a detailed history from the patient and documenting any signs, symptoms, or complaints voiced by the patient. Cauda equina syndrome is a diagnosis based primarily upon bladder dysfunction accompanied by other related complaints. Therefore, an ED physician or nurse must take a detailed history, particularly regarding any bladder complaints.6,8,9 Such a history, and accompanying physical examination, must be well documented to establish the true diagnosis for the patient.6,8,9
In Mr. Moore’s case, Mr. Moore claimed that he complained of bladder dysfunction during his visits to the ED. No documentation for these complaints existed in the medical records, and more significantly, three different ED physicians, who each obtained a detailed history, from Mr. Moore noted no bladder complaints. In fact, Mr. Moore returned to work following his first visit and worked at least four days following his initial ED visit. His alleged complaints of bladder dysfunction were not validated by his physical actions and largely were unsubstantiated. Such unfounded allegations by a plaintiff demonstrate unequivocally the need for a thorough history and careful documentation of the complaints and findings in patients evaluated in the ED. In this case, the jury believed the defendant physicians and returned a verdict that complied with the medical realities of Mr. Moore’s situation.
Case #4
In Anonymous 47-Year-Old Female v. Anonymous Chiropractor and Anonymous Emergency Room Group,18 the female plaintiff brought a medical negligence suit based upon a chiropractor’s alleged negligent back manipulation that resulted in an acute herniated disc. In addition, her suit alleged a failure to diagnose her cauda equina syndrome in the ED, and a failure to treat her cauda equina syndrome in a timely manner causing her to suffer permanent bladder, bowel, and neurological dysfunction. The defendants named in the suit included the chiropractor who performed the alleged negligent back manipulation as well as the ED physician and ED group.
In Anonymous v. Anonymous, the female patient suffered chronic lower back pain with a multiple-year history of lumbar pain. Because of her back pain and paucity of treatment options, she presented to the chiropractor for therapeutic manipulations. The chiropractor performed several lumbar manipulations that resulted in the patient developing severe back pain, an inability to urinate, and perineal numbness.
Following the chiropractic manipulation and immediately following the above complaints, the female patient presented to the ED staffed by the ED group and its physician. In the ED, the patient was evaluated by the ED physician, found to have bladder dysfunction, diagnosed with urinary retention, and discharged home with no definitive follow-up or instructions.
Approximately 14 hours later, the female patient returned to the ED and was evaluated by a different ED physician who immediately diagnosed her with acute cauda equina syndrome and performed the appropriate emergent diagnostic evaluations.
The patient underwent emergency surgery. However, the patient experienced permanent bowel and bladder incontinence and permanent perineal numbness following her surgery.
Multiple neurosurgeons and ED experts were willing to testify as to the breaches of the standard of care of the ED physician and the ED group and that the delay in treatment was the direct cause of the plaintiff’s subsequent bladder, bowel, and neurological dysfunction. The case did not go to trial but settled for $2.975 million, of which the ED group contributed $2.5 million.
Discussion
The case of Anonymous v. Anonymous further illustrates several points already discussed, including the need for diagnosing cauda equina syndrome in a timely manner; the need for, and rationale behind, investigation of urinary retention; and the need for appropriate follow-up and discharge instructions in certain patients with back pain. The most important point developed in Anonymous v. Anonymous, however, is the timing of emergency surgery and its effect upon the ultimate outcome of the patient.
Prior to 1986 and the more recent studies detailing cauda equina syndrome, most authorities recommended that surgical treatment be performed within six hours after onset of an acute cauda equina syndrome.7
Recently, however, most authors advocate that patients with acute cauda equina syndrome undergo surgical treatment as early as possible, but no later than 48 hours after the onset of symptoms.2,3,5,6,8 In fact, most studies demonstrate that patients who underwent surgery more than 48 hours after onset of symptoms had a much poorer outcome than those patients who underwent surgery within 48 hours (see Table 3).2-5,8 In both Jennett and Robinson’s studies, two studies published prior to 1970, no patient underwent surgery within 48 hours of onset of their cauda equina syndrome symptoms.19,20 In Jennett’s study, only two of 14 patients regained bladder and bowel control; in Robinson’s study, one-half the patients continued with paralysis for more than two weeks.19,20

As more patients with cauda equina syndrome were studied, it became apparent that earlier surgeries lead to better outcomes. In a 1980 study, Nielsen reported that patients who underwent surgery within two days of onset of their cauda equina syndrome suffered fewer late bladder abnormalities than did those patients who underwent surgery after two days.21 In a 1986 study, Hellstrom documented 13 of 17 patients who underwent surgery within 48 hours of onset of their cauda equina syndrome and who experienced good return of bladder function.22 Hellstrom’s study also demonstrated increased sexual potency after earlier surgery.22 In 1986, Kostuik and researchers detailed 31 patients with cauda equina syndrome of whom 10 could be diagnosed with acute cauda equina syndrome presenting with bladder dysfunction and other signs and symptoms of the syndrome.7 In those patients with acute cauda equina syndrome, the time to operation ranged from six to 48 hours with an average of 1.1 days.7 Kostuik noted, "Detailed analysis of the results was not possible in this retrospective chart review."7 However, the study did note that postoperative motor results were considered good in the acute group patients who received surgery within 48 hours.7
Later studies, with detailed analyses, clearly have shown a benefit to early surgery, especially if surgery is performed within 48 hours of onset of acute cauda equina syndrome symptoms. In 1993, Shapiro reported 14 patients who presented with acute cauda equina syndrome as a result of a ruptured lumbar disc.6
In Shapiro’s study, all patients with urinary incon-tinence who underwent surgery within 48 hours regained continence and unassisted ambulation.6 However, only two of six patients with incontinence who underwent surgery after 48 hours of onset of symptoms regained bladder control.6 After his analysis, Shapiro noted, "Every effort should be made to operate within 24-48 hours of onset. Additionally, we now counsel all patients with less severe problems from disc disease to report any problems with bilateral weakness and/or incontinence emergently, so there is no delay in treatment. Early diagnosis and treatment does improve outcome from this uncommon lesion." 6
In a follow-up study, Shapiro studied 44 patients with acute cauda equina syndrome in detail, analyzed and compared the results of surgery performed within 48 hours of symptom onset with the results of surgery performed after 48 hours of symptom onset.8
In Shapiro’s study, 20 patients underwent surgery within 48 hours of symptom onset; of those 20 patients, 18 (90%) underwent surgery within 24 hours of symptom onset. In the remaining 24 patients, surgery was performed more than 48 hours after symptom onset. The causes of delay involved misdiagnosis by a primary care or ED physician, failure to obtain a diagnostic study, or delay of surgical treatment to a more convenient time for the surgeon. In the majority of cases where an inappropriate delay occurred, it involved a weekend or holiday.
Based upon a X2 analysis, Shapiro determined that a delay in surgery was associated with a significantly greater chance for permanent motor weakness (P = 0.006), urologic dysfunction (P = 0.008), chronic severe pain (P = 0.025), and sexual dysfunction (P = 0.006). These results were demonstrated in the group of patients that received surgical therapy more than 48 hours after onset of symptoms. As a result, Shapiro noted that, "The data strongly support the management of cauda equina syndrome from lumbar disc herniation as a diagnostic and surgical emergency," and that "Obviously, nighttime, weekends, and holidays are not an excuse for neglecting an emergent approach."8
As further support for emergent surgery, Ahn, Kostuik, and other authors performed a meta-analysis of surgical outcomes of cauda equina syndrome as a result of lumbar disc herniation.5 They analyzed outcomes in 322 patients regarding the timing of surgical intervention following onset of cauda equina symptoms (based upon and defined as onset of urinary dysfunction).5 The patients were divided into several groups based upon time to surgery; the groups included those with a time to surgery of fewer than 24 hours, time to surgery of 24-48 hours, time to surgery of two to 10 days, time to surgery of 11 days to one month, and time to surgery of more than 1 month. For their analysis, Ahn and colleagues used logistic regression with regard to associated outcomes and time to surgery. Based upon such analysis, the researchers determined that there was a significant advantage to surgery performed within 48 hours of onset of symptoms compared with surgery performed after 48 hours of onset of symptoms. However, they found no difference between patients treated within 24 hours compared with those treated between 24 and 48 hours from onset of symptoms. In addition, they found no difference in outcome between the three groups treated more than 48 hours after onset of symptoms. In their conclusion, Ahn and Kostuik noted, "there was a significant advantage to treating patients within 48 hours as opposed to later than 48 hours, with improved outcomes in resolution of sensory deficit, motor deficit, urinary function, and rectal function."5
In the case of Anonymous v. Anonymous, the female plaintiff was diagnosed with cauda equina syndrome 14 hours after her initial presentation to the ED. She subsequently underwent emergency surgery within 24 hours of her initial presentation to the ED, easily within 48 hours of her initial injury and urinary dysfunction. Her experts, including Dr. Shapiro, (whose articles are noted in Table 3) agreed to testify that had she been diagnosed and treated in a timely manner, her injuries would not have been as severe. Unfortunately, based upon the studies reviewed above, as well as Gleave’s study11 (a study that demonstrates no difference in early vs. late surgery based upon different diagnostic criteria for cauda equina syndrome), the plaintiff’s injuries would have been the same whether she was treated at her initial visit or within 24 hours as she was.
Based upon the above studies, the difference in outcome manifests at 48 hours. Patients who have surgery before 48 hours of presentation do better than those with surgical therapy after 48 hours. Although most authors agree that the earlier the surgery the better, no statistically significant studies have demonstrated the superiority of surgery at six hours, 12 hours, 14 hours, or even 24 hours.
In the case of the Anonymous plaintiff, no statistically significant outcome differences are available. Based upon the above studies, the plaintiff in Anonymous would have had the same outcome if she had been treated emergently at her initial presentation vs. the treatment she actually received — surgery within 24 hours of her initial presentation. The case settled based, not upon concrete medical data, but the plaintiff’s initial faulty diagnosis and the possibility that the plaintiff may have had a better outcome if she had undergone surgery 14 hours earlier.
Summary
Cauda equina syndrome is a neurological entity caused by pressure upon the cauda equina generally due to a ruptured lumbar intervertebral disc. Other etiologies of cauda equina syndrome include tumor, infection or hematoma, but they are much less common than a ruptured disc. Cauda equina syndrome is characterized by low back pain, bilateral or unilateral lumbar radiculopathy, motor and sensory deficits as well as bladder or bowel dysfunction. Most researchers define cauda equina syndrome only when bladder dysfunction is present in the patient. Cauda equina syndrome does not exist and cannot be diagnosed in the absence of bladder dysfunction. Regarding treatment, most ruptured lumbar discs can be treated conservatively, either successfully or on an interim basis until surgery becomes necessary.
Cauda equina syndrome, however, is a true surgical emergency and is the only true absolute indication for surgical treatment of a patient with a ruptured lumbar disc. In fact, most authors recommend surgery as soon as possible with studies indicating much poorer results if the surgery is performed 48 hours or more following the onset of symptoms.
Regarding the medicolegal implications of cauda equina syndrome, Shapiro noted, "Serious legal implications about emergency room and doctor office management of this problem exists." To avoid these "serious legal implications," practitioners must continue to view cauda equina syndrome as a true surgical emergency that requires both emergent diagnostic and treatment actions. Any patient with urinary dysfunction must be studied on an emergent basis, particularly if the patient has suffered an acute change coupled with other discogenic symptoms. The ED physician and nurse must be aware of the condition and must have the skills to diagnose the entity and order an MRI scan to evaluate the cauda equina and lumbar spine. Moreover, the ED physician and nurse must recognize that cauda equina syndrome is a surgical emergency requiring immediate referral to, or consultation with, a qualified spine surgeon. The patient cannot be allowed to linger without studies or consultation, a caveat that is especially true regarding evenings, weekends, or holidays. A patient with acute cauda equina syndrome cannot be treated as a routine back pain patient and to do so exposes the ED clinician to serious medicolegal consequences.
Endnotes
1. Louisell DW, Williams H. "ED Malpractice." In: Medical Malpractice Litigation Guide: Types of Liability and Malpractice. Newark, NJ: Matthew Bender; 2003. Available at: www.lexisnexis.com.
2. Shapiro S. Medical realities of cauda equina syndrome secondary to lumbar disc herniation. Spine 2000;25:348-352.
3. Shapiro S. Cauda equina syndrome secondary to lumbar disc herniation. Neurosurgery 1993;32:743-747.
4. Mixter WJ, Barr JS. Rupture of the intervertebral disc with involvement of the spinal cord. N Engl J Med 1934;211: 210-214.
5. Ahn VM, Ahn NU, Buchowski JM, et al. Cauda equina syndrome secondary to lumbar disc herniation: A meta-analysis of surgical outcomes. Spine 2000;25:348-352.
6. Shapiro S. Cauda equina syndrome secondary to disc herniation. Neurosurgery 1993;32:743-747.
7. Kostuik JP, Harrington I, Alexander D, et al. Cauda equina syndrome and lumbar disc herniation. J Bone Joint Surg [Am] 1986;68:386-391.
8. Shapiro S. Medical realities of cauda equina syndrome secondary to lumbar disc herniation. Spine 2000;25:348-352.
9. Kostuik JP. Cauda equina syndrome: An uncommon entity and medicolegal controversies. Neurosurg Focus 2004;16: 39-41.
10. Silveri CP, Simeone FA. "Lumbar Disc Disease," In: An HS (ed.). Principles and Techniques of Spine Surgery. Baltimore: Williams & Wilkins; 1998: pp. 425-443.
11. Gleave JRW, MacFarlane R. Cauda equina syndrome: What is the relationship between timing of surgery and outcome? Br J Neurosurg 2002;16:325-328.
12. Gleave JRW, MacFarlane R. Prognosis for recovery of bladder function following lumbar central disc prolapse. Br J Neurosurg 1990;4:205-209.
13. Gustavo Landin and Patricia Landin v. Roland Zachow, PA, Thomas Strawmyer, MD, and Concentra Health Services, Inc. d/b/a Concentra Medical Center, No. 2000-00945 (Harris County District Court, 165th, Texas, Oct. 11, 2001).
14. Robinson R. Massive protrusions of lumbar discs. Br J Surg 1965;52:858-865.
15. Tay ECK, Chacha PB. Midline prolapse of a lumbar intervertebral disc with compression of the cauda equina. J Bone Joint Surg [Br] 1979;61:43-46.
16. Sullivan v. Johnson, No. CV88-139 (Knox County, Maine, September 1992).
17. William Moore v. Little Falls Hospital; Victor Osinaga, M.; OM Wadhera, MD; and Richard Chemielewski, MD, No. 68642 (Herkimer Supreme Court, Utica, NY, Dec. 2, 1997).
18. Anonymous 47-Year-Old Female v. Anonymous Chiropractor and Anonymous Emergency Room Group, Case Number Withheld (Court of Common Pleas, Cuyahoga County, OH, May 1, 2002).
19. Jennett W. A study of 25 cases of compression of the cauda equina by prolapsed intervertebral discs. J Neurochem 1956;19:109-116.
20. Robinson R. Massive protrusions of the lumbar discs. Br J Surg 1965;52:858-865.
21. Nielsen B, de Nully M, Schmidt K, Hansen I. A urodynamic study of cauda equina syndrome due to lumbar disc herniation. Urol Int 1980;35:167-170.
22. Hellstrom P, Kortelainen P, Kontturi M. Late urodynamic findings after surgery for cauda equina syndrome caused by a prolapsed lumbar intervertebral disc. J Urol (Paris) 1980;135:308-312.
Low back pain is a frequent patient complaint in the emergency department. In fact, the same patients may visit the ED repetitively with the same complaint. It is easy to be assuaged into thinking that these patients are merely seeking drugs, but to make that assumption can lead a clinician to miss the cauda equina syndrome and may result in a malpractice action if efforts are not taken to identify any new symptoms and signs in a patient with low back pain. This issue provides the reader with a solid understanding of diagnosing and caring for patients with cauda equina syndrome in the ED and the medicolegal issues that arise from failing to diagnose and appropriately treat these patients.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
