The Quality-Cost Connection: Applying the principles of process variation
Applying the principles of process variation
Realize improvements in efficiency and outcomes
By Patrice Spath, RHIT
Brown-Spath & Associates
Forest Grove, OR
During the 1980s, U.S. manufacturers began to study why the quality of Japanese products was much better than for those made in the United States.
The differences related to their adoption of methods derived from the theory of process variation. Whereas U.S. industries were satisfied if products fell within a range of acceptable standards, the Japanese focused on making things more alike.
By reducing variation in the production process, they were able to create products less likely to fail. Today, the theory of variation is being applied to the products and services of many U.S. industries, including health care.
When the principles of process variation are applied to health care activities, the result can be significant improvements in efficiency, customer service, and patient outcomes.
To appreciate how this happens, let’s explore what the theory of variation means in practice using a simple example:
Suppose the rate of patient falls on a medical unit goes up in one month. What would happen? In an authoritarian climate, staff members in the offending unit are warned to be more careful with patients. However, from what we now know about processes, the variation in patient falls is almost entirely due to the systems of patient care, not individual actions.
If the rate of falls in that medical unit is plotted over time, you most likely will find that the number stays within a predictable range, unless something in the system of care changes.
This is the first principle of the theory of variation — we should expect things to vary because they always do.
Variation happens
Health care managers, however, often act as though they do not expect things to vary. They set targets or standards and react to people’s failure to meet them. The table below illustrates patient fall data for one organization. The number of patient falls in each location is reported for a three-month period.
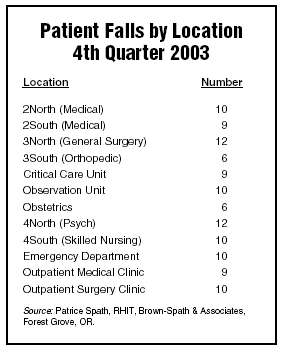
How would managers typically react to the data shown in the table? Would they develop a plan of action for reducing falls on 3North and 4North and give prizes to staff members in 3South and Obstetrics?
The theory of variation can help managers determine how best to interpret and act on the information.
If these same data were plotted on a control chart, you’d find that the process is in control and predictable. (See graph, below.)
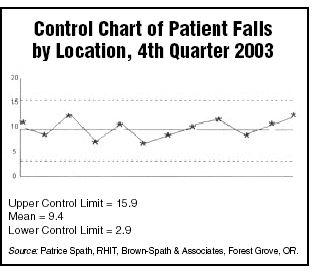
Data plotted on the control chart illustrate that the number of patient falls is stable but exhibits wide variation. The control chart shows that the number of falls could be as high as 16 or as low as three. An average of 9.4 is most likely.
These are the results that should be expected from the patient fall prevention practices currently used by staff members. The control limits (3 and 16) are derived statistically from the variation in the observed results.
This is the second principle of the theory of variation — understanding variation will tell us what to expect. If nothing changes in the patient fall prevention practices, the organization can expect falls in each location to be as low as three or as high as 16 per quarter, but more often the number will be right around the mean (9.4).
Understand variation
An important question is WHY does the rate of performance vary so much? To find the answer, we have to look at the techniques used to prevent patient falls. A simple way to do this is to ask the staff members the following questions:
- What do you need to keep patients from falling?
- How well do these practices work?
- What gets in the way of preventing patient falls?
- How much of your time is consumed by things that get in the way of preventing falls?
Once the organization knows more about the causes of variation, actions can be taken to reduce the number of patient falls in all locations.
If managers want to reduce patient falls, they would be far better off working on the causes of the problem rather than treating individuals or work teams as though they were different.
If everything that helps prevent falls was instituted throughout the organization and everything that hinders was removed, think how the overall rate of patient falls could be reduced.
This is the third principle of the theory of variation — understanding variation leads to improvement.
By investigating the causes, people can work on implementing actions that will reduce unit- to-unit variation and hopefully bring the overall rate of incidents down.
React the right way
When health care managers don’t understand the theory of variation, they can unknowingly make the situation even worse.
For example, when performance differences seen each reporting period are viewed as being caused by individuals, actions are taken at the individual level. In this example of patient falls, the director offered to throw a party for 3North and 4North staff members if they could get the rate of patient falls down to 9 or less next quarter.
What did staff members do? They stopped reporting patient falls, of course. In turn, this action caused further problems for the organization because it no longer had a good database of information about the types and causes of falls.
Which takes us back to the purpose of measuring process variation: Create processes that are less likely to fail. When managers react the wrong way to measurement data, things can get worse.
The theory of variation should be at the heart of world-class quality in all industries, including health care.
During the 1980s, U.S. manufacturers began to study why the quality of Japanese products was much better than for those made in the United States.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
