Minor Trauma Management: Part II
Minor Trauma Management: Part II
Authors: Justin L. Weppner, DO, Lieutenant, Medical Corps, USN, Naval Medical Center Portsmouth, Portsmouth, VA.
James A. McCombs, DO, Lieutenant, Medical Corps, USN, Naval Medical Center Portsmouth, Portsmouth, VA.
Peer Reviewer: Michael C. Bond, MD, FACEP, FAAEM, Assistant Professor, Residency Program Director, Department of Emergency Medicine, University of Maryland School of Medicine
Disclaimer: The views expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Department of the Navy, Department of Defense, or the United States Government.
This is the second issue in the series on minor trauma. This issue deals with neck and chest injuries. Emergency providers must differentiate between minor injuries and the rarer serious injuries, all while being cost effective and avoiding unnecessary radiation.
— Sandra M. Schneider, MD, Editor
Minor Neck Trauma
It is estimated that more than one million whiplash injuries occur each year due to motor vehicle collisions. Barnsley et al1 estimated that the annual incidence of symptoms due to whiplash injury is 3.8 cases per 1,000 population. The annual incidence of spinal cord injury is predicted to be 40 cases per one million population in the United States, or 12,000 new cases each year. In 2012, an estimated 270,000 people in the United States experienced a spinal cord injury. Since 2005, the average age of spinal cord injury has remained at 41.0 years, with 80.6% of injuries reported to the national database involving male patients. Motor vehicle collisions account for 39.2% of spinal cord injuries, followed by falls (28.3%) and acts of violence (14.6%).2
History
An accurate history, including mechanism of injury, is particularly important in the evaluation of patients with blunt cervical trauma, as it is an important factor in deciding who needs c-spine imaging.3 If the neck trauma is a result of a motor vehicle collision, it is important to determine where the vehicle was struck, where the patient was seated, if restraints were used, if airbags deployed, and if the patient was ejected from the vehicle. If the mechanism of injury was from a fall, it is important to determine the height from which the patient fell and any events that precipitated the fall, such as syncope or seizure. Question the patient regarding the quality, severity, and location of pain. Associated signs and symptoms, such as loss of consciousness, presence of weakness, or paresthesias, are particularly important.
Physical Examination
Asking the patient questions provides key information about airway patency, the patient’s mental status, and the patient’s ability to breathe. Emergency physicians should always evaluate the patient for signs of intoxication, as the physical examination of an intoxicated patient may be unreliable. While maintaining spinal precautions, inspect and palpate the entire neck and back for injury. Open the cervical collar and inspect the neck for midline trachea, crepitus, hematoma, or lacerations that could compromise the airway. Palpate the neck for the presence of focal midline cervical tenderness and paraspinal tenderness. It is important to remember that paraspinal muscle tenderness without midline tenderness does not exclude vertebral injury. Based on the 2001 prospective study of 8,924 subjects by Stiell et al, posterior midline tenderness only had 86% sensitivity for clinically important c-spine injury.3
Perform a complete neurological examination of the patient as soon as possible, with periodic serial examinations to assess the possibility of an evolving spinal cord injury. Examine the patient’s motor function thoroughly, followed by a sensory examination. (See Figure 1.) A dermatome map aids in identifying the area of deficit. (See Figure 2.) This should be assessed initially using light touch, moving from any area of diminished sensation to an area of normal sensation. While light touch assesses the posterior column of the spinal column, pinprick assesses the anterior column. Note the presence or absence of reflexes and rectal tone as well.
Figure 1: Spinal Cord Level
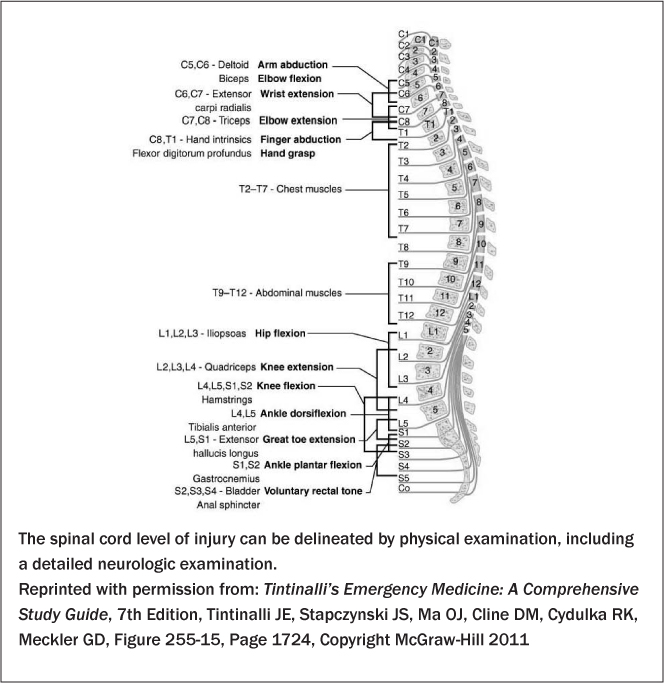
Figure 2: Dermatomes for Sensory Examination
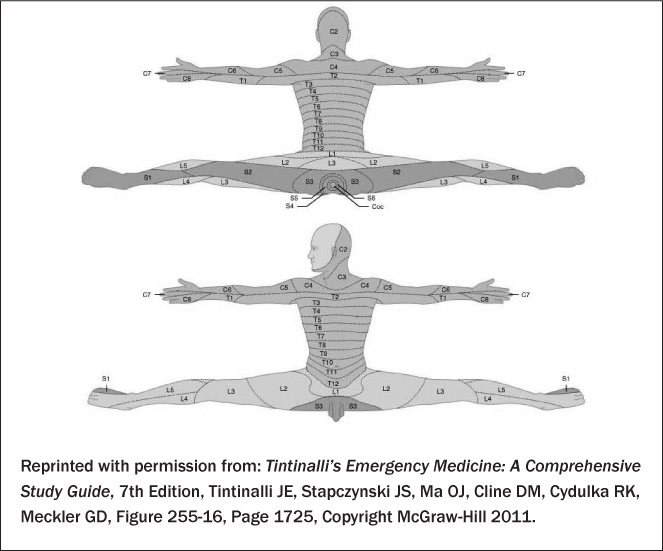
Radiographic Indications
Because a spinal cord injury may lead to devastating neurologic consequences, clinicians have historically taken a liberal approach to imaging the c-spine after trauma.4 According to the results of the National Hospital Ambulatory Care Survey, only 4% of c-spine radiographs demonstrate a fracture.5 Two clinical decision rules have been developed to guide physicians in their use of radiography. The National Emergency X-Radiography Utilization Study (NEXUS) Low-Risk Criteria are based on a multicenter, prospective observational study involving 34,069 trauma patients. The decision rule requires patients to meet five criteria to be classified as having a low probability of injury: no midline cervical tenderness; no focal neurologic deficit; normal alertness; no intoxication; no painful, distracting injury. (See Table 1.) The decision rule identified all but eight of 818 patients who had spinal injuries. Only two of these patients had clinically significant injury: one required surgical stabilization of an injury, and neither sustained permanent neurologic injury. The sensitivity, specificity, and negative predictive value of the NEXUS were 99.0% (95% CI, 98.0–99.6%), 12.9% (95% CI, 12.8–13%), and 99.8% (95% CI, 99.6–100%), respectively.6
Table 1: NEXUS Low-risk Criteria
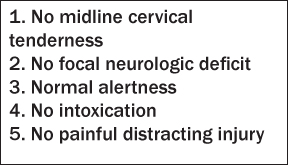
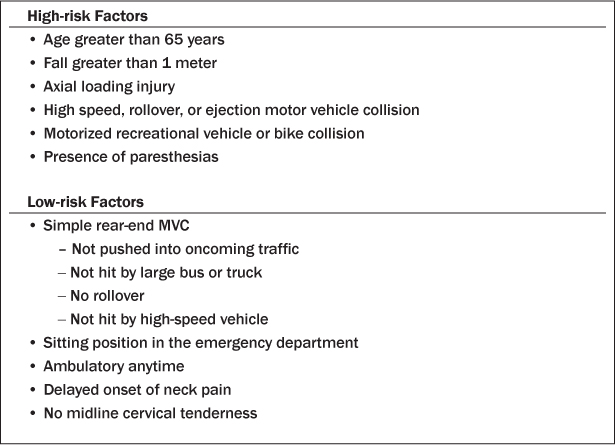
To address the low specificity of the NEXUS, Stiell et al3 developed the Canadian Cervical Spine Rule (CCS) based on 25 selected clinical predictors of spine injury. A prospective cohort sample of 8,924 adults who presented to the ED was evaluated by plain radiography, CT, and a structured follow-up telephone interview. The resultant model and the CCS comprised three main questions: Is there any high-risk factor present that mandates radiography (i.e., age 65 years or older, dangerous mechanism, or paresthesias in extremities)? Is there any low-risk factor present that allows safe assessment of range of motion (i.e., simple rear-end motor vehicle collision, sitting position in the ED, ambulatory at any time since injury, delayed onset of neck pain, or absence of midline c-spine tenderness)? Can the patient actively turn his or her neck 45° to the left and right? The sensitivity and specificity of the CCS were 100% (95% CI, 98–100%) and 42.5% (95% CI, 40–44%), respectively.3 (See Table 2.)
Table 2: Canadian Criteria for Detecting Clinically Important Cervical Spine Injury

Stiell et al7 designed a prospective cohort study comparing the CCS and the NEXUS criteria. Among the 8,283 patients in the study, 169 (2%) had clinically important c-spine injuries. The CCS was more sensitive than the NEXUS criteria (99.4% vs. 90.7%, P < 0.001) and more specific (45.1% vs. 36.8%, P < 0.001) for injury, and its use would have resulted in lower radiography rates (55.9% vs. 66.6%, P < 0.001). The CCS would have missed one patient, and the NEXUS criteria would have missed 16 patients with important injuries. Stiell and colleagues concluded that the CCS is superior to the NEXUS criteria with respect to sensitivity and specificity, and would result in reduced rates of radiography.
The NEXUS and CCS criteria have both been compared to the gold standard c-spine CT scan. In a prospective study, 2,606 blunt trauma patients were evaluated at a level I trauma center. Of the 2,606 patients, 157 were found to have c-spine fractures on CT scan. The NEXUS criteria missed 26 of these 157 patients. Of the 26 missed fractures, 19 required further intervention, with 16 requiring collars, two requiring surgical intervention, and one requiring a halo brace.8 The CCS was evaluated in a prospective study of 3,201 blunt trauma patients; 192 patients were found to have a c-spine injury. In this trial, the CCS maintained 100% sensitivity as compared with CT, and no fracture was missed using this tool.9
Distracting Injuries
Controversy exists regarding what constitutes a distracting injury. The NEXUS investigators’ definition of a distracting injury included long bone fractures, visceral injury requiring surgical consultation, large lacerations, degloving injury or crush injury, large burns, or any other injury producing acute functional impairment.10 The Canadian study’s definition of distracting injury was “injuries such as fracture that are so severely painful that the neck examination is unreliable.”3 The concept that certain injuries may distract patients from other injuries is based on the gate theory of pain, in which distracting injuries may induce sufficient signaling through the spinal pathways that the patient may not notice spinal injuries. The proximity of the two painful stimuli to each other plays a major role in that one painful stimulus may inhibit another.11
Chang et al12 conducted a prospective cohort study of 4,698 patients undergoing radiographic evaluation of the spine following blunt trauma. Of the 4,698 patients, 336 had distracting injuries as the sole documented indication for obtaining radiographic studies of the vertebrae. Eight of the 336 patients had 14 acute vertebral injuries, including compression fractures (5), transverse process fractures (7), spinous process fracture (1), and c-spine rotary subluxation (1). Distracting injuries in the eight patients included 13 bony fractures. The authors concluded that in patients with distracting injuries, bony fractures of any type were important for identifying patients with vertebral injuries. Other types of injuries such as lacerations, soft-tissue contusions, head injuries, bony dislocations, abrasions, visceral injuries, dental injuries, burns, and ligamentous injuries did not contribute to the sensitivity for detection of vertebral injuries.
Heffernan et al13 conducted a prospective observational study of adult blunt trauma patients who underwent c-spine plain film radiography. Of 406 subjects, 10% had a c-spine fracture, of which 18% had a non-tender c-spine and an associated upper torso injury. No patient with injuries isolated to the lower torso and a non-tender neck had a c-spine fracture. The study concluded that upper torso injuries may be sufficiently painful to distract from a reliable c-spine examination, and in the presence of isolated painful lower torso injuries, patients are not distracted and may be aware of spine tenderness. However, this was a single-center study and limited by a small sample size; thus, caution must be exercised when excluding a lower extremity injury as a distracter.
In 2012, Rose et al13 conducted a study involving 761 blunt trauma patients with at least one distracting injury. A physician clinically cleared patients without complaints of pain and tenderness on physical examination. To evaluate if they missed any fractures, all patients clinically cleared with distracting injuries underwent CT scanning of the entire c-spine. A physician had initially clinically cleared 464 of the patients with distracting injuries. Following CT, only one patient (0.2%) who had been clinically cleared had a c-spine injury. Clinical exam had 99% sensitivity and greater than 99% negative predictive value for c-spine clinical examination in awake, alert patients with blunt trauma and distracting injuries. This was a single-center study and was limited by a relatively small sample size; hence, caution must be exercised when distracting injuries are present.
Radiographic Evaluation
A 3-view, cross-table lateral, anteroposterior, and open-mouth odontoid c-spine series was once the mainstay of c-spine radiographic evaluation. In a prospective study on the reliability of standard plain film screening of the c-spine, 23 patients (0.07% of all patients) had 35 injuries (including three unstable c-spine fractures) that were not visualized on adequate plain film imaging.10 These patients represented 2.81% of all injured patients with blunt trauma undergoing radiographic evaluation. Mower et al concluded that standard 3-view imaging provides reliable screening for most patients with blunt trauma, but will fail to identify significant unstable injuries on occasion.
In a 667-patient study of patients who had plain films and CT, 60 (9%) had an acute c-spine injury.15 Plain films had 45% sensitivity and 97.4% specificity. CT of the c-spine had 100% sensitivity and 99.5% specificity. All clinically significant injuries were detected by c-spine CT.
Holmes and Akkinepalli16 published a meta-analysis comparing plain films to CT of the c-spine. The pooled sensitivity for plain radiography was 52%, whereas it was 98% for CT. Other authors have reported similar findings.17-22 In two studies, c-spine CT was more time-efficient than plain films of the c-spine.23,24
CT has supplanted plain radiography as the primary modality for screening suspected c-spine injury after trauma in many institutions.
Magnetic resonance imaging (MRI) is considered the gold standard when cord injury is suspected without bony injury. After blunt trauma, spinal cord injury is uncommon, with a reported incidence of 0.1–0.5%.21,25-27 MRI may demonstrate other surgically correctable lesions such as acute disc herniations, bony compression, epidural and subdural hemorrhage, and vertebral artery occlusion. MRI is not appropriate for hemodynamically unstable patients because resuscitation and monitoring are difficult in the MRI suite. Contraindications to MRI include the presence of a pacemaker, non–MRI-compatible cerebral aneurysm clips, and metallic foreign bodies. The indications for emergent MRI include the presence of neurologic deficits attributable to spinal cord injury or suspicion of ligamentous injury on plain films or CT.
Interpretation of Plain Radiographs
The first priority is to ensure that the films are of good quality and that the lateral view visualizes the C7–T1 junction. A retrospective review of 216 trauma patients found that failure to visualize C7 and the C7–T1 junction was the most common error in radiographic assessment of c-spine injury.28
Cross-table Lateral View. Alignment. Three lines are used to assess alignment. (See Figure 3A.) Line 1 is the prevertebral soft tissue and extends down the posterior aspect of the airway. It should be several millimeters from the first three or four vertebral bodies, and then move further away at the laryngeal cartilage. Line 1 should be less than one vertebral body width from the anterior vertebral bodies and should have a smooth contour. Line 2 follows the anterior vertebral bodies and should be smooth and uninterrupted. Line 3 connects the posterior vertebral bodies and should be smooth and uninterrupted. Line 4 connects the posterior junction of the lamina with the spinous process. The spinal cord lies between lines 3 and 4. Any offset of either of these lines could mean a bony structure is impinging on the cord. Line 5 is not really a line so much as a collection of tips of the spinous processes. Their size and appearance are quite variable, although C7 is consistently the largest. A fracture of one of the spinous processes by itself is not a serious injury, but may herald a more serious injury.
Figure 3A: Spinal Cord Level
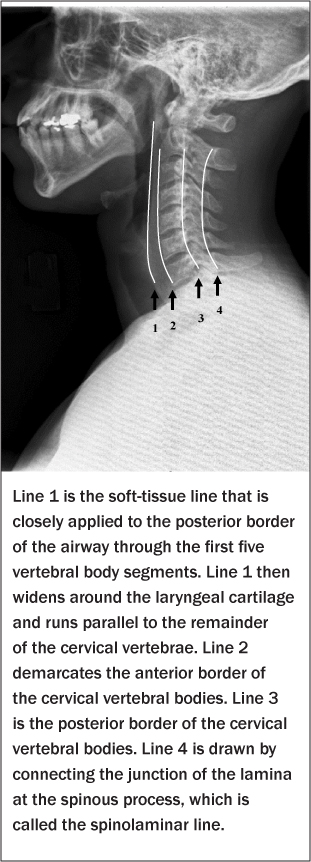
Assess the distance between the anterior arch of C1 and odontoid process (dens) of C2. This is best assessed in the lateral view, and the normal distance should not exceed 3 mm in adults.29 A widening of this space may indicate a Jefferson fracture of C1.
Bones. Evaluate the bones for obvious fractures and loss of vertebral body height. Acute compression fractures of the vertebral bodies and metastatic osteoblastic lesions result in areas of increased bone density.
Cartilage. Examine the disc spaces for widening or narrowing, either of which could indicate an acute traumatic injury. If the disc space is narrowed, it will usually be secondary to degenerative disease and accompanied by osteophytosis and sclerosis. Anterior or posterior widening of the intervertebral space or the interspinous space may be the only clue to an unstable dislocation.
Soft Tissues. Assess the soft tissues of the retropharyngeal space for the presence of prevertebral swelling and hemorrhage, which may be the only radiographic sign of spinal injury. The retropharyngeal space is measured from the anterior border of C2 to the posterior wall of the pharynx and should not exceed 6 mm. The space from the anterior border of the body of C6 to the posterior wall of the trachea should not exceed 22 mm.
In a retrospective study of 106 subjects and 93 control patients, a C2 prevertebral soft-tissue measurement greater than 6 mm had 59% sensitivity and 84% specificity for fractures at C1–C4. A C6 prevertebral soft-tissue measurement greater than 22 mm had 5% sensitivity and 95% specificity for fractures at C4–C7. Cutoffs of 6 mm at C2 and 22 mm at C6 as markers of c-spine injury failed to identify a large proportion of patients with c-spine fractures.29
Odontoid View. The lateral margins of the C1 ring should be aligned within 1–2 mm of the articular masses of the axis. The articular masses of C2 should appear symmetrical, as should the joint spaces between the articular masses of C1 and C2, as long as there is no rotation of the head. The distance between the odontoid and the C1 medial border should be equal, but a discrepancy of 3 mm or more is often seen in patients without pathology. A vertical line bisecting the odontoid process should form a 90-degree angle with a line across the superior aspect of the C2 articular masses. (See Figure 3B.)
Figure 3B: Odontoid View
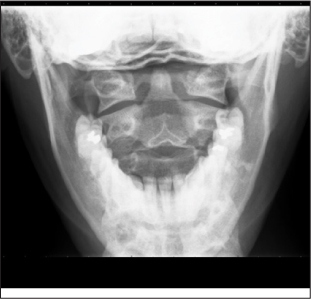
Anteroposterior View. The spinous processes should form a straight line, and the laryngeal and tracheal air shadows should be midline. Verify the regular outline of the lateral masses, and view the pedicles end-on to check for fracture. The spinous processes should form a straight line down the middle of the vertebral body and should be equidistant apart. If one spinous process is out of line with the others, a jumped facet may be present. (See Figure 3C.)
Figure 3C: Anteroposterior View
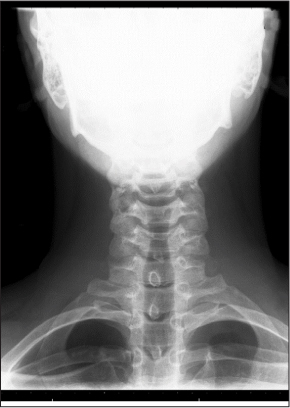
Oblique Views. Oblique views of the c-spine may be ordered to confirm a suspected posterior laminar fracture, a unilateral facet dislocation, or an actual subluxation. CT is often used.
Swimmer’s Lateral View. This view is often obtained to visualize the cervicothoracic junction when it is obscured by the shoulders on the true lateral. If the swimmer’s lateral view cannot be obtained, CT is usually required.
Flexion and Extension Views. Flexion and extension views are obtained when there is concern for ligamentous injury despite negative standard radiographs. Instability of the c-spine is suggested by any of the following: greater than 3.5 mm horizontal displacement between the discs; displaced apophyseal joints; widened disc spaces; greater than 30% loss of disc height; the presence of a prevertebral hematoma.30 In the acute setting, flexion and extension radiographs have been reported to have high false-positive and false-negative rates.31-33 Studies such as CT and MRI appear to be superior imaging modalities in patients with severe, localizing symptoms who have normal radiographs.34-36
Management
Pre-hospital Treatment. Pre-hospital personnel should have a high suspicion of c-spine injuries, and spinal immobilization should be initiated at the scene prior to transport. A 2003 Cochrane review identified no randomized controlled trials that evaluated pre-hospital spinal immobilization in the trauma patient.37 Spinal immobilization has never been proven to prevent secondary spinal injury.38
Kwan and Bunn39 reviewed 17 randomized controlled trials comparing various types of spinal immobilization devices in 529 healthy volunteers. Substantial head and neck motion were reported regardless of whether rolled towels or commercial foam wedges were used. The current protocol for pre-hospital spinal immobilization has a strong historical precedent based less on objective evidence and more on concern that a patient with an injured spine may deteriorate neurologically without immobilization.40 Estimates in the literature regarding the incidence of neurologic injury due to inadequate immobilization may have been exaggerated.38,41 However, there are examples of patients whose spinal injury occurred after immobilization devices were removed.
Many pre-hospital providers perform “precautionary immobilization” due to fear of missing a spinal cord injury. Spinal immobilization can result in increased scene time, increased patient pain, and subsequent unnecessary radiographic testing.38,42,43 Large prospective studies are needed to validate decision criteria to identify the subset of trauma patients that benefits from spinal immobilization.
Treatment of Cervical Strain and Non-specific Soft-Tissue Injury. Routine treatment for acute cervical strain injuries often consists of pain medications, non-steroidal anti-inflammatory drugs (NSAIDs), and muscle relaxants. Range-of-motion exercises and physical therapy may also be beneficial, but are not usually prescribed from the ED. Cervical collars are generally not helpful. Dehner et al44 compared two vs. 10 days of immobilization with a soft collar and found no difference in terms of pain, range of motion, or disability. In a randomized, parallel-group trial of 458 patients treated with immobilization, mobilization, or no specific treatment, there were no significant differences in prevention of pain, disability, and work capability one year after injury.45
Treatment of Cervical Spine Injury. If a c-spine injury is identified on radiography, surgery may be necessary to relieve impingement on the spinal cord caused by foreign bodies, herniated discs, bony fracture fragments, or an epidural hematoma.46,47
Pharmacotherapy in acute spinal cord injury is controversial. The National Acute Spinal Cord Injury Study suggested high-dose methylprednisolone therapy when administered within eight hours of spinal cord injury.48 The recommended dose of methylprednisolone is 30 mg/kg intravenous bolus, followed by an infusion of 5.4 mg/kg/h. The infusion is maintained for 24 hours in patients who are treated within three hours of injury, and for 48 hours in patients treated within 3–8 hours of injury. The overall methodology of the trial has been criticized.49 A subsequent randomized trial using an identical treatment protocol failed to demonstrate any benefit of corticosteroid therapy.50 In addition, the American Academy of Neurologic Surgeons questioned the benefits of treatment.51 At this time, no substantial evidence supports the utilization of methylprednisolone for acute blunt spinal cord injury, and its use should be considered an option for treatment.
Discharge Criteria
Musculoskeletal injuries of the spine involving mild to moderate discomfort and no neurologic impairment, abnormal radiographic findings, or other injuries requiring hospitalization are best handled on an outpatient basis. These patients should be followed-up closely, as 27% of patients experiencing neck pain in the ED following trauma will continue to have symptoms at one year after injury.52,53
Patients with minor trauma and insignificant mechanisms of injury who have isolated, stable cervical vertebral body compression fractures or spinous process fractures may be managed on an outpatient basis if there is no evidence of neurologic or ligamentous impairment and the patient’s pain can be adequately controlled with oral pain medications. Appropriate close follow-up should be established in all instances, as even minor spinal injuries may be associated with prolonged disability resulting from chronic pain.52-55
A patient with a radiographically normal c-spine imaging but continuous pain concerning for c-spine injury may be discharged with a hard collar if appropriate follow-up care can be established prior to discharge. If follow-up care cannot be arranged, an alternative approach would be to obtain a CT scan or MRI, as indicated, to evaluate the c-spine further.
Minor Chest Trauma
Approximately 50% of patients sustaining thoracic trauma will have a chest wall injury, with 10% of those injuries considered minor trauma. Simple rib fractures are the most common form of minor chest injury, accounting for more than half of blunt trauma thoracic injuries.56 The overall incidence is probably higher because not all rib fractures are seen on chest radiographs or otherwise detected.57 Ribs usually break at the point of impact or at the weakest point along the posterior angle of the rib. The fourth through ninth ribs are most commonly involved, while ribs 1–3 are relatively protected and ribs 9–12 are mobile, allowing movement at the anterior end.
History
Rib fractures can occur secondary to high- or low-energy stresses, depending on the patient’s age, pre-existing medical conditions, and mechanism of injury. The elderly usually sustain rib fractures because of a fall from a standing height, while rib fractures in younger adults are more often the result of a motor vehicle collision. Rib fractures can also occur following repeated stress from increased physical activity or poor biomechanics in sports-related activities such as rowing.
Physical Examination
Inspect the chest wall for contusion, abrasions, seat belt sign, and other signs of trauma. Observe the respiratory cycle for paradoxical chest wall movements or flail chest segments. A scaphoid abdomen may indicate a diaphragmatic injury with herniation of the abdominal contents into the chest. Palpation of the chest wall may reveal localized tenderness or crepitus due to fractures. Palpation of the chest with the patient coughing or straining may reveal abnormal motion of an unstable portion of the chest wall better than visual inspection. Percussion of the chest wall may be helpful in determining if hemothorax or pneumothorax is present. Dullness of percussion over the one side of the chest following trauma may be the first sign of hemothorax, while hyper-resonance may indicate pneumothorax. Unilaterally decreased breath sounds may indicate the presence of hemothorax or pneumothorax.
Radiographic Indications for Chest Radiograph
Conventional PA and lateral chest radiography has long been the mainstay in screening and diagnosis of thoracic injuries in stable patients with minor chest trauma.58,59 Several investigators have reported that in the absence of clinical indicators of trauma, the elimination of chest radiographs does not compromise patient care or lead to missed injuries or delays in diagnosis.60-62 In one study, the negative predictive value of the trauma surgeon’s judgment was 98.2%, which was superior to the use of clinical indicators alone. Reliance on the opinion of the trauma surgeon would have eliminated 49.9% of chest radiographs and prevented $100,078.22 worth of radiological reading charges.
Rodriguez et al63 conducted a prospective, multicenter observational study in an attempt to derive a decision instrument for patients that require chest imaging. The decision instrument derived included: chest pain; chest wall tenderness; distracting injury; rapid deceleration; intoxication; age greater than 60 years; and altered mental status. Among the individual criteria, chest pain and chest wall tenderness had the highest sensitivity (65%) for thoracic injury. The combination of all seven criteria being positive had the following screening performance: 99.3% sensitivity (95% CI, 97.4–99.8%), 14% specificity (95% CI, 12.6–15.4%), 99.4% negative predictive value (95% CI, 97.8–99.8%), and 11.7% positive predictive value (95% CI, 10.5–13.1%). More data are currently needed to validate this rule for selective imaging in chest trauma.
Paydar et al64 performed a prospective cross-sectional study on 1,008 hemodynamically stable blunt trauma patients with negative physical examinations for chest trauma. Of the 1,008 subjects, only one (0.1%) had an abnormal chest radiograph, and that was unrelated to trauma.
In 2006, Davis and Affatato65 found no difference between medications prescribed based on whether a fracture was diagnosed by the ED physician, indicating that interpretation of the rib series did not influence the ED physician’s treatment plan.
Fifty percent of single rib fractures are not seen on the initial radiograph study.66 In patients with a low-risk mechanism of injury, radiographs are not necessary if there are normal vital signs and physical examination findings, adequate oral pain control, and if the identification of an uncomplicated rib fracture would not alter injury management. However, if there is concern for pneumothorax or hemothorax, or if there are signs of thoracic injury, a radiograph should be obtained.67,68
CT scans are significantly more effective than chest radiographs for detecting rib fractures, but if rib fractures are strongly suspected or recognized on a clinical basis, a routine CT scan is not required unless other intrathoracic pathology is suspected. In most cases of minor chest trauma, radiographs should be ordered prior to CT. If injuries such as hemothorax, large pneumothorax, widened mediastinum, fracture of the first or second ribs, significantly displaced ribs, or fractured sternum are present, a chest CT scan should be obtained. It is also important to remember that if the patient has fractures of the lower ribs and has abdominal pain related to intra-abdominal injury, a CT scan of the abdomen and pelvis should be performed.69
Treatment of Minor Chest Trauma
The cornerstone of rib fracture management is pain control.57 Pain limits the ability to cough and breathe deeply, resulting in sputum retention, atelectasis, and reduction in functional residual capacity. Systemic opioids are often the first-line management for relieving pain. However, opioids cause sedation, respiratory depression, and cough suppression.70 Considering the potential side effects associated with opioid analgesic use, regional anesthetic techniques may be used to assist with pain control.
Intercostal nerve blocks are a simple and time-tested method for managing pain in patients with rib fractures, even in the ED.71 Success depends on blocking the intercostal nerves proximal to the fracture site. An intercostal nerve block posterior to the mid-axillary line will ensure blockade of the lateral cutaneous and anterior branch of the intercostal nerve.72 Due to overlapping innervations from the segments above and below it, blocking intercostal nerves above and below the fracture site is necessary. The reported incidence of complications includes nerve injury in 1.9 per 10,000 blocks, and pneumothorax incidence after intercostal nerve block is low.72,73 (See Figure 4.)
Figure 4: Cross-sectional View of Intercostal Nerve Anatomy
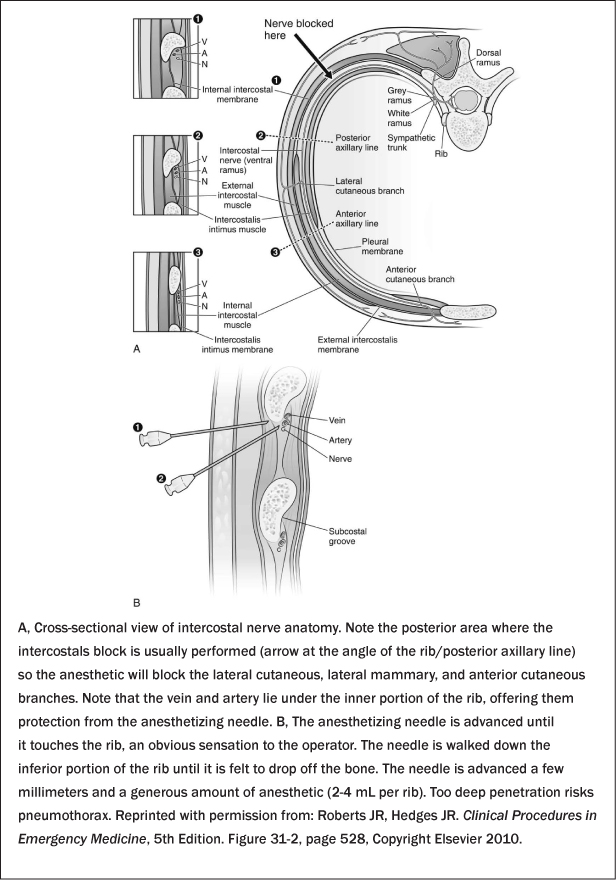
Oral analgesics such as NSAIDs and acetaminophen, which do not depress the central nervous system or the cardiovascular system, are useful adjuncts for mild to moderate pain.
Pain relief must be effective or patients will not maintain activity, and taking pain medications 30–45 minutes before activity and deep-breathing exercises is advised. Binders, belts, circumferential rib taping, and other restrictive devices should not be used because they promote hypoventilation with subsequent atelectasis and pneumonia.74
Admission Criteria
Patients should be admitted to the hospital for intractable pain not controlled with intercostal nerve blocks and opioid analgesics, inability to cough or clear secretions, compromised pulmonary function, or elderly patients with significant underlying pathology such as diabetes or congestive heart failure.75 There is a linear relationship between the number of fractures in all age groups and the development of complications.76 However, using the number of rib fractures alone as the threshold for admission is not advised, as each clinical situation requires individual evaluation.
In the elderly population, an increasing number of fractured ribs is associated with increasing morbidity and mortality.77,78 Bulger et al77 studied rib fractures in patients older than 65 years and found that with each additional rib fracture, mortality increased by 19% and risk of pneumonia increased by 27%. Aside from elderly patients with single rib fractures whose pain is adequately controlled, most patients older than 65 years should be evaluated beyond the ED in either an outpatient observation unit or admitted as an inpatient.79
Discharge Criteria
Most patients with simple rib fractures may be discharged. Patients with adequate pain control, no other system injuries, normal pulmonary function with no signs of lung parenchyma injury, and ability to cough and clear secretions may be discharged from the ED with strict precautions to return if shortness of breath develops, pain is not controlled with the medications prescribed, or if temperature exceeds 38°C. Patients should follow up with their primary care provider within 48–72 hours if their symptoms do not improve.80 Inform patients prior to discharge that they will experience severe pain for several days and that the rib fracture will take approximately six weeks to heal.
Summary
What first appears to be a minor injury may be significant. Emergency physicians must make rapid, cost-effective assessments of patients with minor injuries, diagnosing those patients who have serious injuries from the vast majority who do not.
The authors are military service members who prepared this work as part of their official duties. Title 17 U.S.C. 105 provides that “Copyright protection under this title is not available for any work of the United States Government.” Title 17 U.S.C. 101 defines a United States Government work as a work prepared by a military service member or employee of the United States Government as part of that person’s official duties.
References
1. Barnsley L, Lord S, Bogduk N. Whiplash injury. Pain 1994;58(3):283-307.
2. (NSCISC) NSCISC. Spinal Cord Injury Fact and Figures at a Glance. 2012. https://www.nscisc.uab.edu. Accessed 4/11/2013.
3. Stiell IG, Wells GA, Vandemheen KL, et al. The Canadian C-spine rule for radiography in alert and stable trauma patients. JAMA 2001;286(15):1841-1848.
4. Marx JA, Hockberger RS, Walls RM, et al. Rosen’s Emergency Medicine: Concepts and Clinical Practice, 7th ed. Philadelphia: Mosby/Elsevier; 2010.
5. McCaig LF, Nawar EW. National Hospital Ambulatory Medical Care Survey: 2004 emergency department summary. Adv Data 2006(372):1-29.
6. Hoffman JR, Mower WR, Wolfson AB, et al. Validity of a set of clinical criteria to rule out injury to the cervical spine in patients with blunt trauma. National Emergency X-Radiography Utilization Study Group. N Engl J Med 2000;343(2):94-99.
7. Stiell IG, Clement CM, McKnight RD, et al. The Canadian C-spine rule versus the NEXUS low-risk criteria in patients with trauma. N Engl J Med 2003;349(26):2510-2518.
8. Duane TM, Mayglothling J, Wilson SP, et al. National Emergency X-Radiography Utilization Study criteria is inadequate to rule out fracture after significant blunt trauma compared with computed tomography. J Trauma 2011;70(4):829-831.
9. Duane TM, Wilson SP, Mayglothling J, et al. Canadian Cervical Spine rule compared with computed tomography: A prospective analysis. J Trauma 2011;71(2):352-355; discussion 355-357.
10. Mower WR, Hoffman JR, Pollack CV, Jr., et al. Use of plain radiography to screen for cervical spine injuries. Ann Emerg Med 2001;38(1):1-7.
11. Bouhassira D, Le Bars D, Villanueva L. Heterotopic activation of A delta and C fibres triggers inhibition of trigeminal and spinal convergent neurones in the rat. J Physiol 1987;389:301-317.
12. Chang CH, Holmes JF, Mower WR, et al. Distracting injuries in patients with vertebral injuries. J Emerg Med 2005;28(2):147-152.
13. Heffernan DS, Schermer CR, Lu SW. What defines a distracting injury in cervical spine assessment? J Trauma 2005;59(6):1396-1399.
14. Rose MK, Rosal LM, Gonzalez RP, et al. Clinical clearance of the cervical spine in patients with distracting injuries: It is time to dispel the myth. J Trauma Acute Care Surg 2012;73(2):498-502.
15. Mathen R, Inaba K, Munera F, et al. Prospective evaluation of multislice computed tomography versus plain radiographic cervical spine clearance in trauma patients. J Trauma 2007;62(6): 1427-1431.
16. Holmes JF, Akkinepalli R. Computed tomography versus plain radiography to screen for cervical spine injury: A meta-analysis. J Trauma 2005;58(5):902-905.
17. Barba CA, Taggert J, Morgan AS, et al. A new cervical spine clearance protocol using computed tomography. J Trauma 2001;51(4):652-656; discussion 656-657.
18. Brown CV, Antevil JL, Sise MJ, et al. Spiral computed tomography for the diagnosis of cervical, thoracic, and lumbar spine fractures: its time has come. J Trauma 2005;58(5):890-895; discussion 895-896.
19. Rabb CH, Johnson JL, VanSickle D, et al. Are upright lateral cervical radiographs in the obtunded trauma patient useful? A retrospective study. World J Emerg Surg 2007;2:4.
20. Sanchez B, Waxman K, Jones T, et al. Cervical spine clearance in blunt trauma: Evaluation of a computed tomography-based protocol. J Trauma 2005;59(1):179-183.
21. Schenarts PJ, Diaz J, Kaiser C, et al. Prospective comparison of admission computed tomographic scan and plain films of the upper cervical spine in trauma patients with altered mental status. J Trauma 2001;51(4):663-668; discussion 668-669.
22. Widder S, Doig C, Burrowes P, et al. Prospective evaluation of computed tomographic scanning for the spinal clearance of obtunded trauma patients: Preliminary results. J Trauma 2004;56(6):1179-1184.
23. Daffner RH. Cervical radiography for trauma patients: A time-effective technique? AJR Am J Roentgenol 2000;175(5):1309-1311.
24. Daffner RH. Helical CT of the cervical spine for trauma patients: A time study. AJR Am J Roentgenol 2001;177(3): 677-679.
25. Davis JW, Phreaner DL, Hoyt DB, et al. The etiology of missed cervical spine injuries. J Trauma 1993;34(3):342-346.
26. Grossman MD, Reilly PM, Gillett T, et al. National survey of the incidence of cervical spine injury and approach to cervical spine clearance in U.S. trauma centers. J Trauma 1999;47(4):684-690.
27. Chiu WC, Haan JM, Cushing BM, et al. Ligamentous injuries of the cervical spine in unreliable blunt trauma patients: Incidence, evaluation, and outcome. J Trauma 2001;50(3):457-463; discussion 464.
28. Woodring JH, Lee C. Limitations of cervical radiography in the evaluation of acute cervical trauma. J Trauma 1993;34(1):32-39.
29. DeBehnke DJ, Havel CJ. Utility of prevertebral soft tissue measurements in identifying patients with cervical spine fractures. Ann Emerg Med 1994;24(6):1119-1124.
30. Bagley LJ. Imaging of spinal trauma. Radiol Clin North Am 2006;44(1):1-12, vii.
31. Khan SN, Erickson G, Sena MJ, et al. Use of flexion and extension radiographs of the cervical spine to rule out acute instability in patients with negative computed tomography scans. J Orthop Trauma 2011;25(1):51-56.
32. Insko EK, Gracias VH, Gupta R, et al. Utility of flexion and extension radiographs of the cervical spine in the acute evaluation of blunt trauma. J Trauma 2002;53(3):426-429.
33. Pollack CV, Jr., Hendey GW, Martin DR, et al. Use of flexion-extension radiographs of the cervical spine in blunt trauma. Ann Emerg Med 2001;38(1):8-11.
34. Crim JR, Moore K, Brodke D. Clearance of the cervical spine in multitrauma patients: The role of advanced imaging. Semin Ultrasound CT MR 2001;22(4):283-305.
35. Panacek EA, Mower WR, Holmes JF, eta l. Test performance of the individual NEXUS low-risk clinical screening criteria for cervical spine injury. Ann Emerg Med 2001;38(1):22-25.
36. Pitt E, Thakore S. Best evidence topic report. Role of flexion/extension radiography in neck injuries in adults. Emerg Med J 2004;21(5):587-588.
37. Kwan I, Bunn F, Roberts I. Spinal immobilisation for trauma patients. Cochrane Database Syst Rev 2001(2):CD002803.
38. Hauswald M, Ong G, Tandberg D, et al. Out-of-hospital spinal immobilization: Its effect on neurologic injury. Acad Emerg Med 1998;5(3):214-219.
39. Kwan I, Bunn F. Effects of prehospital spinal immobilization: A systematic review of randomized trials on healthy subjects. Prehosp Disaster Med 2005;20(1):47-53.
40. Bohlman HH. Acute fractures and dislocations of the cervical spine. An analysis of three hundred hospitalized patients and review of the literature. J Bone Joint Surg Am 1979;61(8):1119-1142.
41. McHugh TP, Taylor JP. Unnecessary out-of-hospital use of full spinal immobilization. Acad Emerg Med 1998;5(3): 278-280.
42. Barkana Y, Stein M, Scope A, et al. Prehospital stabilization of the cervical spine for penetrating injuries of the neck — is it necessary? Injury 2000;31(5): 305-309.
43. Haut ER, Kalish BT, Efron DT, et al. Spine immobilization in penetrating trauma: More harm than good? J Trauma 2010;68(1):115-120; discussion 120-111.
44. Dehner C, Hartwig E, Strobel P, et al. Comparison of the relative benefits of 2 versus 10 days of soft collar cervical immobilization after acute whiplash injury. Arch Phys Med Rehabil 2006;87(11):1423-1427.
45. Kongsted A, Qerama E, Kasch H, et al. Neck collar, “act-as-usual” or active mobilization for whiplash injury? A randomized parallel-group trial. Spine (Phila Pa 1976) 2007;32(6):618-626.
46. Vaccaro AR, Daugherty RJ, Sheehan TP, et al. Neurologic outcome of early versus late surgery for cervical spinal cord injury. Spine (Phila Pa 1976) 1997;22(22): 2609-2613.
47. Mirza SK, Krengel WF, 3rd, Chapman JR, et al. Early versus delayed surgery for acute cervical spinal cord injury. Clin Orthop Relat Res 1999(359):104-114.
48. Bracken MB, Shepard MJ, Collins WF, et al. A randomized, controlled trial of methylprednisolone or naloxone in the treatment of acute spinal-cord injury. Results of the Second National Acute Spinal Cord Injury Study. N Engl J Med 1990;322(20):1405-1411.
49. Hurlbert RJ. Methylprednisolone for acute spinal cord injury: An inappropriate standard of care. J Neurosurg 2000;93(1 Suppl):1-7.
50. Pointillart V, Petitjean ME, Wiart L, et al. Pharmacological therapy of spinal cord injury during the acute phase. Spinal Cord 2000;38(2):71-76.
51. Pharmacological therapy after acute cervical spinal cord injury. Neurosurgery 2002;50(3 Suppl):S63-72.
52. McNamara RM, O’Brien MC, Davidheiser S. Post-traumatic neck pain: A prospective and follow-up study. Ann Emerg Med 1988;17(9):906-911.
53. Atherton K, Wiles NJ, Lecky FE, et al. Predictors of persistent neck pain after whiplash injury. Emerg Med J 2006;23(3):195-201.
54. Ditunno JF, Jr., Formal CS. Chronic spinal cord injury. N Engl J Med 1994;330(8):550-556.
55. Ross PD. Clinical consequences of vertebral fractures. Am J Med 1997;103(2A):30S-42S; discussion 42S-43S.
56. Khandhar SJ, Johnson SB, Calhoon JH. Overview of thoracic trauma in the United States. Thorac Surg Clin 2007;17(1):1-9.
57. Ziegler DW, Agarwal NN. The morbidity and mortality of rib fractures. J Trauma 1994;37(6):975-979.
58. Reuter M. Trauma of the chest. Eur Radiol 1996;6(5):707-716.
59. Keough V, Pudelek B. Blunt chest trauma: Review of selected pulmonary injuries focusing on pulmonary contusion. AACN Clin Issues 2001;12(2):270-281.
60. Sears BW, Luchette FA, Esposito TJ, et al. Old fashion clinical judgment in the era of protocols: Is mandatory chest X-ray necessary in injured patients? J Trauma 2005;59(2):324-330; discussion 330-322.
61. Rodriguez RM, Hendey GW, Marek G, et al. A pilot study to derive clinical variables for selective chest radiography in blunt trauma patients. Ann Emerg Med 2006;47(5):415-418.
62. Nejati A, Khalaj S, Azizkhani R, et al. Evaluating validity of clinical criteria for requesting chest X-rays in trauma patients referred to emergency room. Adv Biomed Res 2012;1:22.
63. Rodriguez RM, Hendey GW, Mower W, et al. Derivation of a decision instrument for selective chest radiography in blunt trauma. J Trauma 2011;71(3):549-553.
64. Paydar S, Johari HG, Ghaffarpasand F, et al. The role of routine chest radiography in initial evaluation of stable blunt trauma patients. Am J Emerg Med 2012;30(1): 1-4.
65. Davis S, Affatato A. Blunt chest trauma: Utility of radiological evaluation and effect on treatment patterns. Am J Emerg Med 2006;24(4):482-486.
66. Mayberry JC, Trunkey DD. The fractured rib in chest wall trauma. Chest Surg Clin N Am 1997;7(2):239-261.
67. Bhavnagri SJ, Mohammed TL. When and how to image a suspected broken rib. Cleve Clin J Med 2009;76(5):309-314.
68. Livingston DH, Shogan B, John P, et al. CT diagnosis of rib fractures and the prediction of acute respiratory failure. J Trauma 2008;64(4):905-911.
69. Holmes JF, Ngyuen H, Jacoby RC, et al. Do all patients with left costal margin injuries require radiographic evaluation for intraabdominal injury? Ann Emerg Med 2005;46(3):232-236.
70. Moon MR, Luchette FA, Gibson SW, et al. Prospective, randomized comparison of epidural versus parenteral opioid analgesia in thoracic trauma. Ann Surg 1999;229(5):684-691; discussion 691-682.
71. Raj PP, Paradise LA. Pain Medicine: A Comprehensive Review, 2nd ed. St. Louis, MO: Mosby; 2003.
72. Roberts JR, Hedges JR, Chanmugam AS. Clinical Procedures in Emergency Medicine, 4th ed. Philadelphia, PA: W.B. Saunders; 2004.
73. Shanti CM, Carlin AM, Tyburski JG. Incidence of pneumothorax from intercostal nerve block for analgesia in rib fractures. J Trauma 2001;51(3):536-539.
74. Lazcano A, Dougherty JM, Kruger M. Use of rib belts in acute rib fractures. Am J Emerg Med 1989;7(1):97-100.
75. Barnea Y, Kashtan H, Skornick Y, et al. Isolated rib fractures in elderly patients: Mortality and morbidity. Can J Surg 2002;45(1):43-46.
76. Shorr RM, Rodriguez A, Indeck MC, et al. Blunt chest trauma in the elderly. J Trauma 1989;29(2):234-237.
77. Bulger EM, Arneson MA, Mock CN, et al. Rib fractures in the elderly. J Trauma 2000;48(6):1040-1046; discussion 1046-1047.
78. Holcomb JB, McMullin NR, Kozar RA, et al. Morbidity from rib fractures increases after age 45. J Am Coll Surg 2003;196(4):549-555.
79. Graff L. The Textbook of Observation Medicine: The Healthcare System’s Tincture of Time. 2011; http://www.acep.org/observationsection.
80. Misthos P, Kakaris S, Sepsas E, et al. A prospective analysis of occult pneumothorax, delayed pneumothorax and delayed hemothorax after minor blunt thoracic trauma. Eur J Cardiothorac Surg 2004;25(5):859-864.
This is the second issue in the series on minor trauma. This issue deals with neck and chest injuries. Emergency providers must differentiate between minor injuries and the rarer serious injuries, all while being cost effective and avoiding unnecessary radiation.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
