Opioid Use: The ED Conundrum
Opioid Use: The ED Conundrum
Authors:
Nirmala Abraham, MD, FABPM, Medical Director, Sycamore Pain Management Center, Miamisburg, OH.
Cathy D. Trame, RN, MS, CNS, BC, Manager, Acute and Perioperative Pain Program, Kettering Physician Network, Miamisburg, OH.
Peer Reviewer:
Clara L. Carls, DO, Program Director, Hinsdale Family Medicine Residency, Hinsdale, IL.
This article is adapted from one that originally appeared in the February 2013 issue of Primary Care Reports.
Every day, every shift, I am confronted by a patient that I believe is drug-seeking. Statistics and my own personal experience suggest these patients are becoming more common. Chronic pain has become a common disease, and many patients appear to believe they are entitled to ever increasing doses of pain medications. Policies of The Joint Commission and patient satisfaction questionnaires that ask if pain was adequately controlled reinforce these behaviors. Caught between wanting to limit opioid addiction and diversion and wanting to the address real pain and keep good patient satisfaction scores, the emergency physician is in a no-win situation.
Recently, I tried to help one such patient who had repeated visits to our emergency department for abdominal pain. Since I had seen him more than 20 times in the past few years, we had developed some relationship. Over time, I helped him understand that he needed another solution for his pain. He eventually made an appointment with a primary care provider, the first step to a pain clinic appointment. After waiting three months for an appointment, he was rapidly dismissed from the practice with a terse note in the record — "We don’t deal with patients who need opioids for pain." On the same day this patient returned to the ED, another appeared who had been refused a pain clinic appointment because there was concern she was addicted. These cases illustrate the frustration of both providers and patients who deal with chronic pain, addiction, and drug-seeking behavior.
— Sandra M. Schneider, MD, Editor
Introduction
Opioid use/abuse is an increasing problem. In a mail survey sent to a random community sample, 4.1% of respondents admitted to taking opioids at that time.1 These patients present to the emergency department (ED), often frustrated by inconsistent approaches to their pain. When their expectations for pain relief are not met, they can become upset and belligerent. Both The Joint Commission and patient satisfaction surveys ask specifically if a patient’s pain was controlled. Yet many of these patients display classic drug-seeking behavior, asking for drugs by name and quantities that are not indicated by their symptoms. To further aggravate the problem, patients on maintenance doses of opioids are often referred to the ED when they overuse their medications and run out. Primary care physicians (or their offices) deny additional medications, but then refer the patient to the ED.
Background
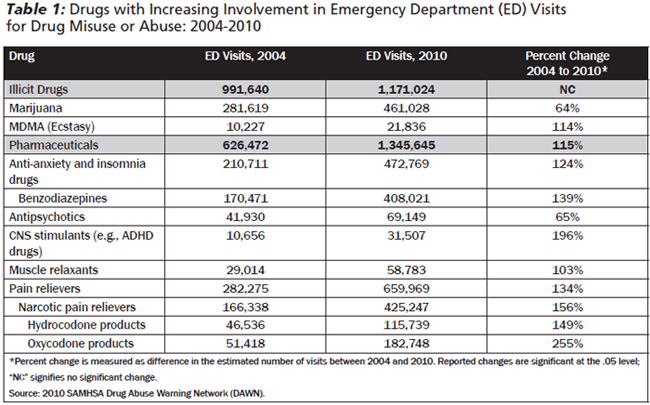
Statistics released by the Drug Abuse Warning Network (DAWN) tout the drastic upswing in the abuse of prescription opioids and the related deaths.2 EDs in the United States reported a 156% increase in the non-medical use of opioids from 2004-2010. (See Table 1.) In a recent national survey, 41% of ED physicians reported that 6-10% of their patients are there for chronic pain, and more than 7% stated that the number of patients presenting for chronic pain was more than 20%.3 In 2010, the misuse or abuse of drugs accounted for 46.8% of all ED visits related to adverse drug events. The most common drugs of abuse included oxycodone, with a 255% increase, and hydrocodone, with a 149% increase. During the same time period, benzodiazepine abuse increased 139%.
The Centers for Disease Control and Prevention (CDC) has reported equally disturbing data. In the United States, 100 people per day die from drug overdoses, a rate of death that has tripled since 1990.4 For every four deaths that occur due to prescription drugs, three are related to prescription opioids. Deaths from opioids now are greater than those from heroin and cocaine combined.5 The 2009 National Youth Risk Behavior Survey revealed that one in five high school students have taken a prescription drug that has not been prescribed for them,6 while one in 20 people ages 12 and older have admitted to using a prescription opioid within the past year for purely recreational reasons.7 A reported 12 million people in the United States use prescription opioids for the euphoric effect vs. pain relief. The abuse of methamphetamines, marijuana, cocaine, steroids, and even alcohol has shown a decline in the time period from 1999-2009.8
While our nation battles the abuse of prescription opioids, the prescribing of these medications has drastically increased. As the population lives longer, with coexisting aging issues related to pain, the demand for analgesic medications increases. The rise in obesity also contributes to the development of chronic pain related to stress on joints and the back. According to the CDC, in the past 15 years, the prescribing of opioids has increased tenfold.9 In 2010, there were enough opioids prescribed to medicate "every American adult around the clock for one month."10 History reveals that an increase in the availability of a drug increases the risk for abuse.11 Responsible prescribing of opioids, coupled with risk-mitigation strategies, has never been more paramount.
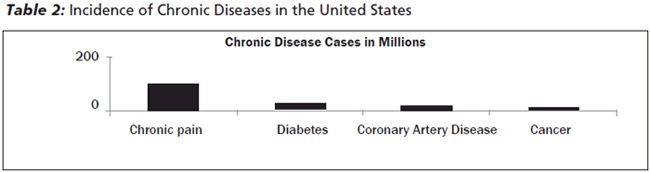
Opioid demand has increased as the number of patients with chronic pain has become more prevalent; in fact, chronic pain has reached epidemic proportions. The American Chronic Pain Association describes chronic pain as " ongoing or recurrent pain, lasting beyond the usual course of acute illness or injury or more than 3 to 6 months, and which adversely affects the individual’s well-being."12 Chronic pain affects approximately 100 million adults in the United States, costing an average of $2000 for every U.S. resident.13 The National Center for Health Statistics reported 26% of adults older than the age of 20 years experience chronic pain.14 Chronic pain is four times more prevalent than diabetes,15 nearly six times more prevalent than coronary heart disease,16 and eight times more prevalent than cancer.17 (See Table 2.)
According to the Institutes of Medicine, the most common chronic pain treated is low back pain (28.1%), followed by knee pain (19.5%) and migraine or headache pain (16.1%).13 Recent clinical guidelines recommend that emergency physicians use caution when treating patients with acute low back pain, and avoid opioids, which have not been shown to be more efficacious than nonsteroidal anti-inflammatory drugs (NSAIDs). When opioids are prescribed, the quantity should be for less than one week.18 Chronic pain historically has been managed poorly. In the 2006 "Voices of Chronic Pain" survey, respondents revealed that they felt little control over their pain (51%), and that breakthrough pain experienced on a daily basis greatly impacted their quality of life (60%).19 Sadly, 50-75% of cancer patients, at the time of death, have moderate-to-severe pain.20 Clearly, the increase in opioid prescribing has not been effective in alleviating chronic pain. When do these chronic conditions that are frequently evaluated and treated by the emergency physician warrant opioid prescribing?
Management of the Crisis
Government representatives have proposed legislation in an attempt to help mitigate the addiction crisis. Congressman Vern Buchanan (R-FL) proposed federal legislation, H.R. 1065: Pill Mill Crackdown Act of 2011, and Senator Joe Manchin (D-WV) proposed S. 1760: Pill Mill Crackdown Act of 2011 to increase fines and prison terms for individuals who prescribe opioids for monetary gain by running "pill mills."21 Although the bills are still in committee, it is likely that some federal legislation will be forthcoming. Many state medical boards have enacted legislation regarding rules for the prescribing of scheduled substances, while state legislators have enacted additional monitoring, fines, and imprisonment for illegal prescribing. Thirty-seven states have instituted prescription monitoring systems to help physicians, pharmacists, and law enforcement track the patterns of individuals obtaining controlled substances via prescriptions, while 11 additional states are in the legislative process for implementation.22 Linkage of information among states in nearby geographical locations is being planned in some regions to better monitor those individuals who cross state lines to hide prescription abuse. Emergency physicians have a responsibility to link into their state resources for monitoring prescriptions and to validate or invalidate patient behaviors that are suspicious of substance abuse. The Alliance of States with Prescription Monitoring Programs (www.pmpalliance.org) provides a list for available programs in your state.
Resources from pharmaceutical companies that manufacture and distribute potent opioids are readily available in the form of Risk Evaluation and Mitigation Strategies (REMS) and patient education tools. The FDA began requiring REMS in 2007 for extended-release and long-acting (ER/LA) opioid analgesics.23 In general, emergency physicians should avoid prescribing extended-release or long-acting opioid medications.
Complications of Opioid Use/Abuse
Clearly the most significant complication of chronic opioid use is death from overdose, as described above. Sadly, 92% of these deaths occur in individuals between the ages of 18 and 54 years.24 Diversion of the drug from the original patient occurred in 63% of these deaths.
Constipation is common with the use of opioids. There is some suggestion that constipation is higher with hydrocodone than with oxycodone.25 Sedation and nausea are also commonly seen. All opioids are known to be addictive.
Recently, chronic abdominal pain associated with prolonged opioid use has been described.26 Patients characteristically have an increase in their abdominal pain with increasing doses of narcotics. While constipation and nausea are common in this syndrome, vomiting is infrequent.27 Treatment is to wean the patient from their narcotic use and eventually eliminate the drug altogether. While treatment is effective, in the study by Tuteja, nearly 50% of patients resumed his or her narcotic use within three months of detoxification.
Available Tools and Resources
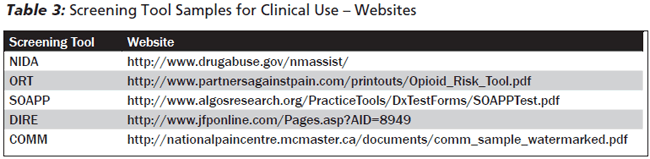
Screening Tools for Abuse Potential. Several assessment tools are available for screening patients for possible substance abuse. Tools that aid in predicting abuse potential prior to prescribing include NIDA Drug Use Screening Tool, Opioid Risk Tool (ORT), Screener and Opioid Assessment for Patients with Pain (SOAPP/SOAPP-R), and Diagnosis Intractability Risk Efficacy Tool (DIRE). However, many of these are cumbersome, and none have been validated in the ED setting. In specific cases, it may be beneficial to work with the patient’s primary care provider to provide the screening and establish a patient contract. Table 3 lists websites at which the tools can be accessed for clinical use.
Toxicology Screening. Random toxicology screening as an outpatient is recommended for any patient prescribed opioids longer than 3 months. Such testing is rarely used in the ED. However, in some EDs, patients with legitimate pain medication needs, such as those with sickle cell disease, are screened for cocaine use by urine toxicology, and if found to be positive, are denied outpatient prescriptions for opioids.28 Provisions should be made to ensure that the patient’s own urine is what is tested.
Opioid Agreements. An opioid agreement should delineate specific rules that the patient must follow while being prescribed opioids. These are best prepared between a patient and their primary care provider. According to APS and American Academy of Pain Medicine (AAPM) clinical guidelines,29 the following components should be included:
- A discussion of the risks and benefits of opioid therapy.
- The types of common side effects and risks of adverse effects, including abuse, addiction, and overdose.
- The risk of hyperalgesia, sexual, and endocrine dysfunction.
- Goals of opioid therapy.
- How the opioids should be taken; scheduled vs. as needed, and frequency, with guidelines for tapering and weaning. The patient should be informed when he or she might need to discontinue the medication, including signs of aberrant behavior.
- Expectations for office follow-up, refill process, pill counts, and random drug screening.
- Use of one prescriber and one pharmacy for opioid therapy.
- Guidance on safe storage of prescriptions to guard against theft and policy on theft replacement.
- How to properly dispose of opioids.
- Alternatives to opioid therapy.
Informed consent and a sample opioid agreement can be found in Appendix 6 and 7 at www.jpain.org/article/S1526-5900(08)00831-6/fulltext#appseca6. Once a pain contract is created, it should be followed in the ED and by all other providers. However, the ED needs to have a system to link these protocols in a useful way. Electronic medical records are quite useful, providing a notification that a protocol exists every time the patient presents.
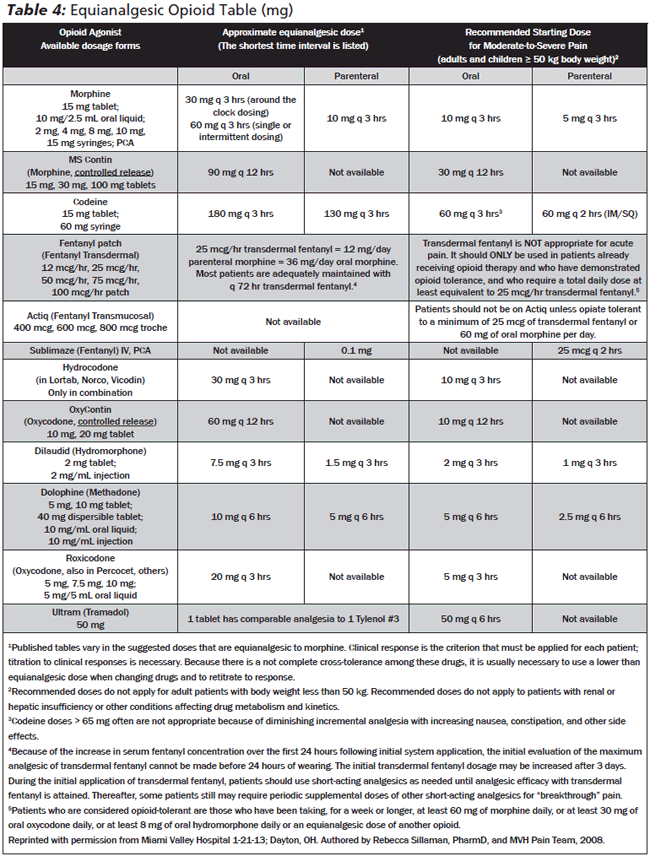
Equianalgesic Dosing Charts. Equianalgesic dosing charts provide dosing guidelines when switching from one opioid to another. (See Table 4.) Calculating an accurate conversion more likely provides a safe dose with analgesic efficacy. Making a switch in opioids without a calculation may cause oversedation or respiratory depression, or on the other end of the spectrum, inadequate analgesia. Dose conversions are most easily calculated by totaling the past 24-hour usage of all opioids into a morphine equivalent. The sum can then be used to convert to an equianalgesic amount of the newly prescribed opioid. Most references suggest using a one-third to one-half total reduction in the sum before conversion due to the patient’s incomplete cross tolerance, resulting in an unpredictable response.29 Additionally, most references caution against initiating methadone unless experienced in its use, such as a pain specialist or palliative care specialist. The long half-life of methadone, with the cumulative effect, and the unpredictability of equianalgesic conversions, can be dangerous. Patients maintained on a stable dose for pain management could be managed by a primary care provider; special licensing to prescribe methadone only applies to opioid detoxification or rehabilitation maintenance programs.30
Managing Pain with Opioids
The first step in prescribing opioids is the decision to initiate the therapy. Some decision-making steps have already been described, including the use of a screening tool and checking prescription history via a state website. Other assessment questions that have demonstrated predictive value may be utilized. Past or current use or abuse of tobacco, alcohol, or other illicit drugs all have been shown to increase the risks for future abuse, while existence of addictive behaviors, such as gambling, sex addiction, Internet addiction, kleptomania, or other impulse control disorders, are directly correlated with an increased risk of substance abuse.31-33 According to Grant, gamblers have been shown to have a tenfold increase in risk of substance abuse as compared with the normal population.31 Other addiction disorders demonstrate similar behaviors to substance abuse including uncontrolled use despite harm and diminished self-control due to cravings.31 Neurobiologists believe that the similarities of addictive disorders are attributable to abnormalities in serotonin production and availability.31 A discussion regarding past or current abuse behaviors should be included as part of the risk stratification for routine screening prior to opioid initiation.
Other predictors may include mental health disorders or a history of physical or sexual abuse as a child.32,33 Substance abusers report high rates of major depression and anxiety (23.5%) as well as high rates of sexual abuse (25.4%).34 As the incidence of anxiety disorders, mood disorders, or behavior disorders increases, there is a direct linear correlation with an increase in substance abuse.35 As the addiction develops, unemployment or frequent job changes, failed relationships or marital problems, involvement in litigation, seeing multiple medical providers, or "doctor shopping" may emerge.33
Patients with undermanaged pain may develop pseudoaddictive behaviors, which can be difficult to differentiate from addictive behaviors. Although both behaviors are not 100% consistent with each category, a comparison of the most likely categorized addictive and pseudoaddictive behaviors is included in Table 5.36
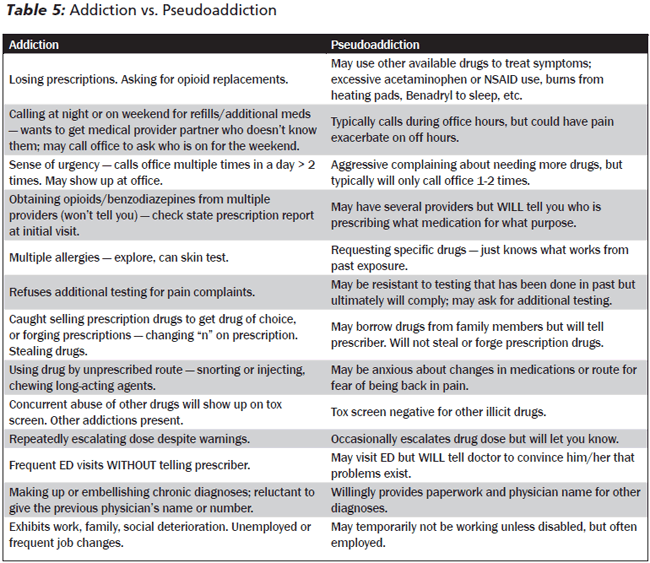
Patients who have altered prescriptions or sold their prescriptions have committed a felony. They should be reported to law enforcement.
Strategies for Dealing with Chronic Pain Patients in the ED
Patients with acute chronic pain can be some of the most frustrating to treat. The ED provider is often faced with little information about the patient’s past behavior or underlying disease. Without a pain protocol, they often are left to guess at what treatment is best. Even when drug-seeking behavior is identified, the ED is not the place to deal with addiction.
One strategy often used in the ED is to provide a limited amount of opioids and refer the patient to a pain treatment center. Most of these centers are located in urban areas, limiting their usefulness in rural areas. Patients should be warned in writing that failure to make or keep an appointment with a pain center will lead to a denial of further opioids from the ED.
Many states have prescription monitoring programs available to clinicians. These range from "after the fact" reporting that a patient has received many prescriptions from multiple physicians to an online check of recent prescriptions filled. While there are few studies of their effectiveness, in one study done in Ohio, access to recent prescription information led to a change in the current prescription in more than 40%, with 61% of patients receiving less medication and 39% receiving more.37
However, many monitoring programs are cumbersome, requiring special user names and passwords and multiple screens before the information becomes available. In some cases, upload of the data from pharmacies is not real-time, allowing patients to acquire large amounts of medications in a short period of time. Few, if any, of the programs cross state lines. Attempts to make query of these databases mandatory prior to prescribing an opioid have not been supported, largely because of these concerns. It is hoped that with time easily accessible, real-time databases will become available to aid the emergency physician.
Other strategies for dealing with opioid requests in the ED exist but have not been rigorously evaluated. Uncoordinated attempts at limiting opioids by individuals are not generally successful, as patients simply try again later with a different provider. It is better when a entire group or even an entire community decides to go "oxy-free." A variant on this is to provide repeat users of the ED with a letter outlining that in the future, no opioids will be prescribed without a written pain treatment protocol from their physician. It is essential that all ED providers are aware that such a letter has been issued and will abide by it.
Recently the state of Washington attempted to limit payment for some patients seen in EDs in an attempt to deal with escalating costs. The Washington State Chapter of the American College of Emergency Physicians working with other groups created a set of guidelines for prescribing opioids in the ED, which have a been adopted state-wide. (See Table 6.) These guidelines include the fact that stolen or lost prescriptions will not be replaced and long acting opioids will not be prescribed. While the results of this specific intervention have not been evaluated, these guidelines represent a starting point for other groups, including states, to develop guidelines for opioid use.

Managing the Palliative Care Patient on Opioids
Managing the pain of a terminally ill patient seems an obvious ethical responsibility, yet more than 50-90% of cancer patients report moderate-to-severe pain at the end of life.38 As many as 75% of heart failure patients in the last 6 months of life and 50% of AIDS patients describe pain related to the disease itself, comorbidities, or related treatment.38 A large study conducted from 1994-2006 concluded that about 26% of patients in the last 2 years of life experienced "clinically significant" or moderate pain on a regular basis, which increased to 46% in the last month of life.39 The American Medical Association Code of Ethics is clear by stating, "Physicians have an obligation to relieve pain and suffering and to promote the dignity and autonomy of dying patients in their care. This includes providing effective palliative treatment even though it may foreseeably hasten death."
There are many myths surrounding pain management at the end of life, including saving strong analgesics until near death.40 The reality is that strong analgesics may be needed early in diagnosis to enhance the patient’s quality of life until death.
The World Health Organization published an analgesic ladder for cancer pain, familiar to most clinicians, suggesting initiation of therapy with an oral non-opioid with adjuvant for mild pain, progressing to opioids with non-opioids (NSAIDs or acetaminophen) and adjuvants for severe pain.41 Delay in aggressive pain therapy may occur if the patient’s pain is severe, and the clinician conservatively begins treatment at the base of the ladder. In an article written by Fine in 2012, it was noted that 20% of patients with advanced disease are not adequately managed with the analgesic ladder.42 Since the undertreatment of pain is widely published, related to the palliative population, multimodal therapies including neuropathic agents and opioids should be employed.
The American College of Physicians (ACP) published practice guidelines for end-of-life care in 2008 and recommended a combination of radiotherapy/radiopharmacology, opioids, NSAIDs, adjuvant medications, and particularly bisphosphonates for bone cancer from breast cancer or myeloma.43 Clinical guidelines developed regarding opioids for palliative care still recommend morphine as the primary mainstay of opioid therapy.44 A long-acting version of morphine for sustained pain, along with breakthrough dosing of a short-acting agent, is recommended. As with all opioid therapy, individual variances may require use of another opioid such as oxycodone or hydromorphone, particularly if the patient has renal dysfunction. Transdermal fentanyl preparations are not recommended for initial therapy, as a level of opioid tolerance should be established prior to initiating. If the patient cannot tolerate oral therapy, subcutaneous injection of opioid should be considered.44 Fear of respiratory depression from potent opioids should not outweigh the benefit of effective analgesia.45 Many states have compassionate care laws in place that protect the physician from litigation for treating the dying patient.
The emotional component of the experience of dying cannot be ignored when managing the pain of a palliative care patient. Multiple literature sources cite depression as a major component at the end of life.46 Clearly, undermanaged emotional distress can exacerbate physical pain. Interdisciplinary management of the patient is paramount for optimizing pain control. The ACP clinical guidelines include the following recommendations (summarized)43:
- Pain, dyspnea, and depression should be regularly reassessed.
- Pain therapies utilized at end of life should be clinically proven; for cancer pain, this includes the use of NSAIDs, opioids, and bisphosphonates.
- Dyspnea should be actively managed with opioids and oxygen.
- Depression should be treated with tricyclic antidepressants, SSRIs, and psychosocial support.
- Advance care planning, including completion of Advance Directives, should be completed.
Risks of addiction in the palliative care population in patients who have no previous history of addiction is extremely rare.47 Presenting signs of aberrant behaviors in terminal patients are often manifestations of pseudoaddiction and undertreated pain.47 Patients who have a prior history of substance abuse will need to be monitored more closely, just as any patient with an addiction history. Since substance abuse lends itself to a higher risk of chronic disease and cancer, patients should be actively screened regardless of terminal diagnosis.
Summary
The decision to prescribe opioids for a patient with non-cancer pain is a difficult and calculated one. Patients with a substance abuse or mental health history should not be denied opioids when experiencing a co-existing pain condition that is affecting their quality of life. Careful screening and using a pre-determined pain management plan is imperative for optimal management of all patients, including palliative care.
References
- Choung RS, Locke GR 3rd, Zinsmeister AR, et al. Opioid bowel dysfunction and narcotic bowel syndrome: A population-based study. Am J Gastroentol2009;104:1199-204.
- Drug Abuse Warning Network. Trends in Emergency Department Visits Involving Non-Medical Use of Narcotic Pain Relievers. Available at: www.samhsa.gov/data/2k10/DAWN016/OpioidED.htm. Accessed Dec. 21, 2012.
- Sandra M. Schneider, MD. Personal communication.
- Paullozzi LJ, Jones CM, Mack KA, et al. Centers for Disease Control. Vital signs: Overdoses of prescription opioid pain relievers — United States, 1999-2008. Morb Mortal Wkly Rep 2011;60;1487-1492.
- Centers for Disease Control and Prevention. Unintentional Poisoning. Available at: www.cdc.gov/HomeandRecreationalSafety/Poisoning/index.html. Accessed Dec. 21, 2012.
- Centers for Disease Control and Prevention. National Youth Risk Behavior Survey, 2009. Available at: www.cdc.gov/mmwr/pdf/ss/ss5905.pdf. Accessed Dec. 21, 2012.
- Centers for Disease Control and Prevention. Vital Signs: Overdoses of Prescription Opioid Pain Relievers — United States, 1999-2008. Morbidity and Mortality Weekly Report (MMWR), November 4, 2011;60:1487-1492. Available at: www.cdc.gov/mmwr/preview/mmwrhtml/mm6043a4.htm?s_cid=mm6043a4_w. Accessed Dec. 21, 2012.
- Centers for Disease Control and Prevention. Illegal Drug Use. FastStats. Available at: www.cdc.gov/nchs/fastats/druguse.htm. Accessed Dec. 21, 2012.
- Centers for Disease Control and Prevention. Policy Impact: Prescription Painkiller Overdoses. Available at: www.cdc.gov/homeandrecreationalsafety/rxbrief/index.html. Accessed Dec. 21, 2012.
- Centers for Disease Control and Prevention. Policy Impact: Prescription Painkiller Overdoses. Available at: www.cdc.gov/homeandrecreationalsafety/rxbrief/index.html. Accessed Dec. 21, 2012.
- Okie S. A flood of opioids, a rising tide of death. N Engl J Med 2010;363:1981-1985.
- American Chronic Pain Association (ACPA). Glossary. Available at: http://theacpa.org/Glossary. Accessed Dec. 21, 2012.
- National Academies Press. Relieving Pain in America: A Blueprint for Transforming Prevention, Care, Education, and Research. Washington DC: The National Academies Press. Available at: http://books.nap.edu/openbook.php?record_id=13172&page=62. Accessed Dec. 21, 2012.
- U.S. Department of Health and Human Services. National Centers for Health Statistics. Health, United States, 2006: Chartbook on Trends in the Health of Americans 2006. Special Feature: Pain. Available at: www.cdc.gov/nchs/data/hus/hus06.pdf. Accessed Dec. 21, 2012.
- American Diabetes Association. Diabetes Statistics. Available at: www.diabetes.org/diabetes-basics/diabetes-statistics/. Accessed Dec. 21, 2012.
- Roger VL, et al. Heart disease and stroke statistics—2011 update: A report from the American Heart Association. Circulation 2011;123:e18-e209, page 20.
- American Cancer Society. Cancer Prevalence: How Many People Have Cancer? Available at: www.cancer.org/docroot/CRI/content/CRI_2_6x_Cancer_Prevalence_How_Many_People_Have_Cancer.asp. Accessed Dec. 21, 2012.
- Cantrill SV, Brown MD, Carlisle RJ, et al. Clinical policy: Critical issues in the prescribing of opioids for adult patients in the emergency department. Ann Emerg Med 2012;60:499-525.
- 2006 Voices of Chronic Pain Survey. American Pain Foundation.
- A controlled trial to improve care for seriously ill hospitalized patients. JAMA 1995;274:1591-1598.
- H.R. 1065 (112th): Pill Mill Crackdown Act of 2011. Available at: www.govtrack.us/congress/bills/112/hr1065. Accessed Dec. 21, 2012.
- U.S. Department of Justice. Drug Enforcement Administration. Office of Diversion Control. State Prescription Drug Monitoring Programs. October 2011. Available at: www.deadiversion.usdoj.gov/faq/rx_monitor.htm#4. Accessed Dec. 21, 2012.
- U.S. Food and Drug Administration. Approved Risk Evaluation and Mitigation Strategies (REMS). Available at: www.fda.gov/Drugs/DrugSafety/PostmarketDrugSafetyInformation-forPatientsandProviders/cm111350.htm. Accessed Dec. 21, 2012.
- Hall AJ, Logan JE, Tobin RL, et al. Patterns of abuse among unintentional pharmaceutical overdose fatalities. JAMA 2008;300:2613-2620.
- Marco CA, Plewa MC, Buderer N, et al. Comparison of oxycodone and hydrocodone for the treatment of acute pain associated with fractures: A double-blind, randomized, controlled trial. Acad Emerg Med 2005;282-288.
- Drossman DA, Morris CB, Edwards H, et al. Diagnosis, characteristics, and 3-month outcome after detoxification if 39 patients with narcotic bowel syndrome. Am J Gastroentol 2012;107:1426-1440.
- Tuteja AK, Biskupiak J, Stoddard GJ, et al. Opioid-induced bowel disorders and narcotic bowel syndrome in patients with chronic non-cancer pain. Neurogastroenterol Motility 2010;22:424-430.
- Sandra M. Schneider, MD. Personal communication.
- American Pain Society. Principles of Analgesic Use, 6th ed. Glenview, IL: APS; 2008.
- Medical College of Wisconsin. Gazelle G, Fine PG. Methadone for the Treatment of Pain, 2nd ed. Fast Facts and Concepts. 2006. Available at: www.eperc.mcw.edu/EPERC/FastFactsIndex/ff_075.htm. Accessed Dec. 21, 2012.
- Grant JE, et al. The neurobiology of substance and behavioral addictions. CNS Spectr 2006;11:924-930.
- National Institute on Drug Abuse. Preventing Drug Abuse among Children and Adolescents. Chapter 1: Risk factors and protective factors. Available at: www.drugabuse.gov/publications/preventing-drug-abuse-among-children-adolescents/chapter-1-risk-factors-protective-factors. Accessed Dec. 21, 2012.
- National Institutes of Health. Appendix C DSM-IV-TR Material. Criteria for Substance Abuse. Opioid Dependence. Available at: www.ncbi.nlm.nih.gov/books/NBK64247/. Accessed Dec. 21, 2012.
- Fergusson DM, et al. Exposure to childhood sexual and physical abuse and adjustment in early adulthood. Child Abuse Negl 2008;32:607-619.
- Merikangas KR, et.al. Lifetime prevalence of mental disorders in U.S. adolescents: Results from the national comorbidity survey replication-Adolescent supplement (NCS-A). J Am Acad Child Adolesc Psychiatry 2010;49:980-989.
- Portenoy RK, et al. Pain and Addiction; Chapter 17: p. 367. In: Clinical Textbook of Addiction Disorders, 3rd ed. Frances RJ, et al., eds. New York: Guilford Publications; 2009.
- Baehren DF, Marco CA, Droz DE, et al. A statewide monitoring program affects emergency department prescribing behaviors. Ann Emerg Med 2010;56:19-23.
- Broglio K, Cole BE. Pain management and terminal illness. Pract Pain Mmgt. 2008. Available at: www.practicalpainmanagement.com/resources/hospice/pain-management-terminal-illness. Accessed Dec. 21, 2012.
- Smith AK, et al. The epidemiology of pain during the last 2 years of life. Ann Intern Med 2010;153:563-569.
- Hospice Foundation of America. Myths about pain. Available at: www.hospicefoundation.org/painmyths. Accessed Dec. 21, 2012.
- World Health Organization. Cancer. WHO’s pain ladder. Geneva, Switzerland. Available at: www.who.int/cancer/palliative/painladder/en/. Accessed Dec. 21, 2012.
- Fine PG. Pain management and end-of-life care. Pain Mgmt 2012;2:325-328.
- Qaseem A, et al. Evidence-based interventions to improve the palliative care of pain, dyspnea, and depression at the end of life: A clinical practice guideline from the American College of Physicians. Ann Intern Med 2008;148:141-146.
- National Institute for Health and Clinical Excellence, 2012. Opioids in palliative care: Safe and effective prescribing of strong opioids for pain in palliative care of adults. NICE Clinical Guideline: Available at: www.nice.org.uk/nicemedia/live/12953/58519/58519.pdf. Accessed Dec. 21, 2012.
- Jackson V, Nabati L. 2012. End of life care: Ethical considerations in pain management. Up To Date Available at: www.uptodate.com/contents/end-of-life-care-ethical-considerations-in-effective-pain-management. Accessed Dec. 21, 2012.
- Lorenz KA, et al. Evidence for improving palliative care at the end of life: A systematic review. Ann Intern Med 2008;148:147-159.
- National Cancer Institute, 2011. Substance abuse issues in cancer. Available at: http://www.everydayhealth.com/health-center/substance-abuse-issues-in-cancer-pdq-supportive-care-health-professional-information-nci.aspx. Accessed Dec. 21, 2012.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
