Procalcitonin in Sepsis: Is it Ready for Prime Time?
November 1, 2013
Reprints
Procalcitonin in Sepsis: Is it Ready for Prime Time?
Special Feature
By Betty Tran, MD, MS, Assistant Professor of Medicine, Pulmonary and Critical Care Medicine, Rush University Medical Center, Chicago. Dr. Tran reports no financial relationships relevant to this field of study.
Although mortality rates for sepsis have improved over the past two decades, its increasing incidence has resulted in a tripling of the number of in-hospital deaths related to sepsis over the same time period.1 Specific blood biomarkers are currently being studied with hopes that their use may improve our ability to distinguish between the systemic inflammatory response syndrome (SIRS) and sepsis, risk-stratify patients to facilitate early and appropriate triage and therapeutic decisions, and avoid the misuse and overuse of antibiotics. Procalcitonin (PCT) currently is the most studied. Its synthesis and secretion are upregulated by bacteria-specific proinflammatory mediators such as interleukin-1b, interleukin-6, and tumor necrosis factor-¦Á, and subsequently decrease with recovery from bacterial infections. In addition, the expression of PCT is attenuated by cytokines typically released during viral infections, such as interferon-¦Ã, and is overall not affected by medications such as steroids. PCT theoretically holds promise, but is there evidence to show that it should be a part of the medical management of all patients presenting with sepsis, and if so, in what capacity? This article aims to provide a current overview of the evidence for PCT in the diagnosis, risk stratification, and antibiotic treatment algorithms of patients presenting with sepsis in the ICU. Although PCT has also been studied in specific settings such as in patients with respiratory infections and in situations outside of the ICU, these topics are outside the scope of this overview.
PROCALCITONIN AS A DIAGNOSTIC MARKER FOR SEPSIS
It is widely accepted that early recognition and initiation of appropriate antibiotics in sepsis are paramount to improved patient outcomes.2 Distinguishing between SIRS and sepsis, however, is often difficult as patient-presenting symptoms are nonspecific, current microbiologic testing has low sensitivity and inherent delays, and no gold standard ultimately exists. The latter characteristic also makes it difficult to conduct studies evaluating PCT as a diagnostic test for sepsis in critically ill patients. Overall, data have been mixed.3-5 In the most recent meta-analysis, which also used the most stringent quality control methods, pooled sensitivity for PCT in the diagnosis of sepsis was 0.77 (95% confidence interval [CI], 0.72-0.81), specificity was 0.79 (95% CI, 0.74-0.84), with an area under the receiver operator characteristic curve (AUC) of 0.85 (95% CI, 0.81-0.88).5The authors only included studies with a well-defined reference standard of sepsis based on established definitions by the American College of Chest Physicians, the Society of Critical Care Medicine, or the German Sepsis Society, although diagnostic threshold values for PCT ranged considerably in all studies, from 0.25-5.79 ng/mL.5 Similar sensitivity, specificity, and AUC were also found in two subsequent single-center studies performed in Korea6 and the United Kingdom,7 with PCT cutoff values of 0.2 ng/mL and 1.0 ng/mL, respectively; negative predictive values ranged from 67-99% depending on the severity of sepsis and presence of organ dysfunction.
Although these statistics show that PCT may reasonably distinguish between SIRS and sepsis given the lack of a gold-standard diagnostic test, there are several pertinent questions that need to be addressed before recommending the widespread use of PCT as a diagnostic marker: 1) are its test characteristics (especially negative predictive value) sufficient to direct medical decision making in the setting of sepsis, and 2) is it significantly better than clinical judgment? For example, is the value of PCT alone enough to persuade a clinician to hold antibiotics in a critically ill patient being admitted for suspected sepsis without a confirmed infectious source?
In the PRORATA trial, a multicenter, randomized, controlled trial to evaluate the use of a PCT-guided antibiotic strategy vs standard care on patient mortality and antibiotic-free days, approximately 30% of physicians "broke protocol" by immediately giving antibiotics to patients in whom they could not rule out infection.8 In another multicenter, randomized, controlled trial from Belgium of PCT-guided vs standard antibiotic care, clinical judgment also superseded protocol recommendations based on PCT values as 53.7% of patients with low PCT levels (< 0.25 ¦Ìg/L) were nevertheless started on antibiotics. The majority of these treatments (30/43, 69.8%) were later confirmed as correct by infectious disease specialists reviewing the charts who were blinded to the PCT results. Furthermore, 33.8% of cases in which no infection was confirmed had PCT values > 1 ¦Ìg/L and 14.9% of cases with confirmed infection had a PCT level < 0.25 ¦Ìg/L, for a resulting AUC of 0.69. The authors concluded that these values were "too low to propose PCT as a marker of infection in ICU patients, at least in the setting of deciding whether to initiate or withhold antibiotics."9
PROCALCITONIN AS A PROGNOSTIC MARKER IN SEPSIS
The ability to risk-stratify patients with sepsis has important clinical implications. Accurate prognostication not only could be used to triage sicker patients more quickly to an ICU bed before later signs such as the development of lactic acidosis and organ dysfunction develop, but also could potentially identify patients at risk for undertreated infections and complications who could benefit from further interventions such as escalation of antibiotics, renewed search for occult infection, and possible surgical interventions and other methods of source control. Several studies have examined the relationship between PCT and mortality related to sepsis.
In a multicenter study of ICUs across Greece, the Hellenic Sepsis Study Group found that 28-day mortality rates for ICU patients with admit PCT levels ≤ 0.85 ng/mL were 25.6% compared to 45.3% for patients with levels > 0.85 ng/mL (odds ratio, 2.404; 95% CI, 1.385-4.171; P < 0.0001).10 In a follow-up study by the same group examining the effect of early changes in PCT levels, a decrease in PCT levels by > 30% or a level < 0.25 ng/mL by 72 hours after admission was associated with improved 28-day survival and was an independent indicator of favorable outcome regardless of disease severity.11
Other observational studies have also reported that changes in PCT rather than absolute values correlate with patient mortality. In a Finnish sepsis study, hospital mortality for patients admitted with sepsis was 12.2% in the group whose PCT decreased by at least 50% within 72 hours compared to 29.8% for patients with a < 50% decrease in PCT (P = 0.007).12 In a similar vein, a more recent U.S. study found that a PCT decrease of 80% over 72 hours was associated with a negative predictive value of 90% (95% CI, 0.77-0.97) for both ICU and hospital mortality.13 Extending this idea further, a larger German cohort study of 472 patients admitted to the ICU (including non-septic patients) found that an increase in the PCT level the first day after reaching a threshold of ≤ 1.0 ng/mL was independently associated with a 1.8-fold increased risk of mortality at 90 days (95% CI, 1.3-2.7; P = 0.002), with sustained increases over day 2 and 3 associated with progressively higher risks of mortality (relative risk [RR], 2.2; 95% CI, 1.6-3.0; P < 0.0001 and RR, 2.8; 95% CI, 2.0-3.8; P < 0.0001, respectively).14
Despite these findings, however, the only interventional study done thus far based on PCT levels failed to show an improvement in patient outcomes. The Procalcitonin and Survival Study (PASS) was a multicenter, randomized, controlled trial where patients were randomized to either a standard care or PCT group. In the PCT group, antimicrobial interventions were guided by "alert" or "nonalert" values. "Alert procalcitonin" was defined as a PCT level ≤ 1.0 ng/mL that was not decreasing by at least 10% from the previous day; if present, it prompted the medical team to increase substantially their antimicrobial spectrum coverage and to intensify efforts to find occult/uncontrolled sources of infection per protocol. Not only was 28-day mortality — the primary outcome — similar between the two groups, the PCT group had a higher number of days on mechanical ventilation (absolute difference 4.9%, P < 0.0001), longer ICU stays by 1 day (P = 0.004), and more evidence of acute kidney injury.15 The authors hypothesized that the increased antibiotic exposure in the PCT intervention group may have induced prolonged organ failure in this group.
PROCALCITONIN TO GUIDE ANTIBIOTIC DECISIONS IN SEPSIS
There has been considerable interest in promoting antibiotic stewardship in efforts to decrease the emergence of multidrug-resistant organisms and complications such as Clostridium difficile infection. Only five randomized, controlled trials have evaluated whether the use of PCT algorithms results in reduced antibiotic exposure without a harmful effect on patient outcomes in patients with sepsis. Two were performed specifically in the postoperative setting and found reductions in antibiotic exposure of 20% and 25% without differences in mortality, although neither was adequately powered to determine non-inferiority.16,17 The most recent trial by Annane et al was performed in a subset of patients with severe sepsis without a clear source of infection; their findings did not show evidence of a significant difference in antibiotic exposure with use of a PCT algorithm, although the study was terminated early due to low incidence of patients meeting their criteria.18
In a single-center study, Nobre et al found that duration of antibiotics was shorter by 3.2 days (95% CI, 1.1-5.4; P = 0.003) with no significant difference in 28-day and ICU mortality, and similar rates of cure in the PCT group.19 These findings, however, were observed only after using a per-protocol analysis that excluded a higher number of patients in the PCT group due to death, transfer, or the presence of complicated infections requiring extended antibiotics rather than an intention-to-treat analysis. Although the authors argue that this was their a priori target population, their final numbers were too small to conclude definitively that a shortened antibiotic course based on PCT levels did not do any harm.
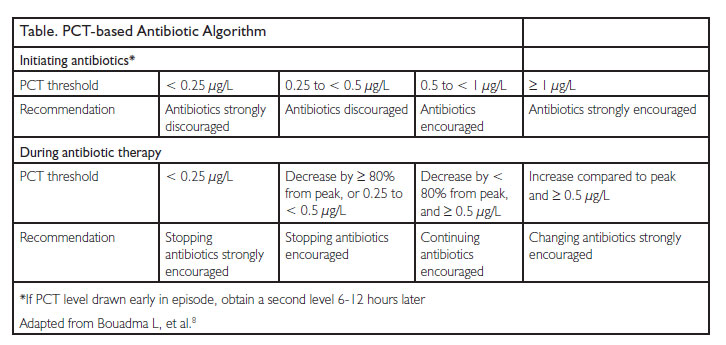
The PRORATA trial, which included 630 patients in multiple ICUs in France, is the only study sufficiently powered to determine non-inferiority in terms of 28-day and 60-day mortality between a PCT-guided antibiotic management protocol and standard care. The authors found that patients in the PCT group had 2.7 more antibiotic-free days (95% CI, 1.4-4.1; P < 0.0001) and a 23% relative reduction in days of antibiotic exposure, without a significant difference in overall mortality at 28 and 60 days.8 In addition, there were no significant differences in many secondary outcomes, including rate of relapse, superinfection, emerging multidrug-resistant bacteria, and ICU and hospital length of stay. The PCT-based antibiotic algorithm they used is summarized in the Table.
CONCLUSION
PCT has garnered significant interest as a biomarker in the management of critically ill patients with sepsis based on a number of studies mostly done in Europe. Currently, the FDA has approved at least three quantitative PCT assays in the United States that are commercially available, each costing an average of $25-30 per assay with turnaround time ranging from 1 hour to 1 day.20 Based on currently available data, the role of PCT as a diagnostic tool for sepsis appears limited given that its testing characteristics, especially negative predictive value, are insufficient to stop clinicians from superseding PCT protocols in favor of clinical judgment in this high-stakes population. Although there are multiple studies reporting that changes in PCT level correlate with mortality in patients with sepsis, the only interventional trial performed thus far has not shown that escalation of therapy based on PCT values has been beneficial, but has shown it actually may cause harm. Perhaps the most meaningful use of PCT may be in helping to determine the duration of antibiotic therapy in situations where an extended course of antibiotics is not necessarily required. There appears to be no worsening of patient mortality, but future studies should also focus on rate of recurrent infections and other infection-related complications as primary outcomes as well as the overall cost-effectiveness of this approach.
REFERENCES
- Martin GS, et al. The epidemiology of sepsis in the United States from 1979 through 2000. N Engl J Med 2003;348:1546-1554.
- Dellinger RP, et al. Surviving sepsis campaign: International guidelines for management of severe sepsis and septic shock: 2012. Crit Care Med 2013;41:580-637.
- Uzzan B, et al. Procalcitonin as a diagnostic test for sepsis in critically ill adults and after surgery or trauma: A systematic review and meta-analysis. Crit Care Med 2006;34:1996-2003.
- Tang BM, et al. Accuracy of procalcitonin for sepsis diagnosis in critically ill patients: Systematic review and meta-analysis. Lancet Infect Dis 2007;7:210-217.
- Wacker C, et al. Procalcitonin as a diagnostic marker for sepsis: A systematic review and meta-analysis. Lancet Infect Dis 2013; 13:426-435.
- Jekarl DW, et al. Procalcitonin as a diagnostic marker and IL-6 as a prognostic marker for sepsis. Diagn Microbiol Infect Dis 2013; 75:342-347.
- Llewelyn MJ, et al. Sepsis biomarkers in unselected patients on admission to intensive or high-dependency care. Crit Care 2013; 17:R60.
- Bouadma L, et al. Use of procalcitonin to reduce patients’ exposure to antibiotics in intensive care units (PRORATA trial): A multicentre randomized controlled trial. Lancet 2010;375:463-474.
- Layios N, et al. Procalcitonin usefulness for the initiation of antibiotic treatment in intensive care unit patients. Crit Care Med 2012;40:2304-2309.
- Giamarellos-Bourboulis EJ, et al. Procalcitonin as an early indicator of outcome in sepsis: A prospective observational study. J Hosp Infect 2011;77:58-63.
- Georgopoulou AP, et al. Early changes of procalcitonin may advise about prognosis and appropriateness of antimicrobial therapy in sepsis. J Crit Care 2011;26:331e1-7.
- Karlsson S, et al. Predictive value of procalcitonin decrease in patients with severe sepsis: A prospective observational study. Crit Care 2010;14:R205.
- Schuetz P, et al. Procalcitonin decrease over 72 hours in US critical care units predicts fatal outcome in sepsis patients. Crit Care2013;17:R115.
- Jensen JU, et al. Procalcitonin increase in early identification of critically ill patients at high risk of mortality. Crit Care Med 2006;34:2596-2602.
- Jensen JU, et al. Procalcitonin-guided interventions against infections to increase early appropriate antibiotics and improve survival in the intensive care unit: A randomized trial. Crit Care Med 2011;39:2048-2058.
- Hochreiter M, et al. Procalcitonin to guide duration of antibiotic therapy in intensive care patients: A randomized prospective controlled trial. Crit Care 2009;13:R83.
- Schroeder S, et al. Procalcitonin (PCT) ¨C guided algorithm reduces length of antibiotic treatment in surgical intensive care patients with severe sepsis: Results of a prospective randomized study. Langenbecks Arch Surg 2009;394:221-226.
- Annane D, et al. Procalcitonin levels to guide antibiotic therapy in adults with non-microbiologically proven apparent severe sepsis: A randomized controlled trial. BMJ Open 2013;3:e002186.
- Nobre V, et al. Use of procalcitonin to shorten antibiotic treatment duration in septic patients. Am J Respir Crit Care Med 2008;177:498-505.
- Schuetz P, et al. Role of procalcitonin in managing adult patients with respiratory tract infections. Chest 2012;141:1063-1073.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
