Gynecologic Complaints in the Adolescent Female
Gynecologic Complaints in the Adolescent Female
Authors:
Brianne Jo Steele, MD, Stanford Kaiser Emergency Medicine Residency.
Sophia Yen, MD, MPH, Assistant Professor, Division of Adolescent Medicine, Department of Pediatrics, Lucile Packard Children’s Hospital/Stanford University Medical School.
N. Ewen Wang, MD, Associate Director of Pediatric Emergency Medicine, Division of Emergency Medicine, Department of Surgery, Stanford University Medical School.
Peer Reviewer:
Ghazala Q. Sharieff, MD, FACEP, FAAEM, FAAP, Director of Pediatric Emergency Medicine, Palomar Pomerado Health System/California Emergency Physicians, Clinical Professor, University of California, San Diego.
The adolescent patient presenting to the emergency department with gynecologic-related complaints deserves special considerations compared to the adult female patient with similar problems. The majority of patients will have straightforward presentations, but recognition of a gynecologic problem or patient with an atypical presentation is critical. This article reviews the most common gynecologic complaints the adolescent may have.
— Ann M. Dietrich, MD, Editor
Introduction
Adolescent girls may not be straightforward about gynecologic issues, and the emergency practitioner should specifically and in a sensitive manner ask about the patient’s gynecologic history. Young women in this age group are the most likely to have irregular menstrual cycles, with abnormal vaginal bleeding being a very common emergency department complaint. The adolescent patient is also at greater risk than an adult for sexually transmitted infections, which must be diagnosed and treated by emergency physicians. Another vital topic is emergency contraception that may be requested by the adolescent female patient. The goal of this article is to address these and other related issues in an effort to improve the emergency physician’s recognition and management of gynecologic complaints in the adolescent.
General Approach to the Adolescent Female Patient
Taking an Adolescent History. The teenage patient may not be forthcoming about her true chief complaint. She may feel embarrassed, be afraid of disapproval, or require confirmation of confidentiality prior to discussion. Vague abdominal complaints or nonspecific chief complaints may be the adolescent’s attempt to seek care for genitourinary complaints.
The provider should focus on the adolescent as the patient and address her directly. After the emergency practitioner has elicited past medical and family history and the parents’ chief complaint, consideration should be given to having the parents excused from the room to allow the adolescent the opportunity to discuss concerns and complete the examination in private. Using a nonjudgmental tone of voice and explicitly telling the patient that she has the right to confidential reproductive health care will encourage disclosure. Seeing the patient without her parent/guardian also provides an important opportunity to ask the patient whether she is sexually experienced, using drugs, or being pressured into these or any other high-risk activities. Drug and alcohol abuse have been associated with higher-risk sexual behaviors, including earlier sexual debut, multiple partners, and inconsistent use of contraception.1 Answers to the questions in Table 1 will allow the emergency provider to gauge the patient’s risk for abusive relationships, pregnancy, and sexually transmitted infections. The provider can choose which questions are the most applicable for a given patient.

This history should not take more than a few minutes for a busy practitioner to complete. Furthermore, this interaction provides a unique opportunity for the emergency medicine practitioner to provide education and anticipatory guidance to the patient. Although traditionally preventative medicine has been considered outside the scope of emergency medicine, emergency physicians have become a source of primary care for patients who have barriers to regular care. About 75% of adolescents utilize the health care system each year, and many of these visits are in the emergency department or urgent care facility. If the emergency physician does not provide education to the high-risk adolescent, that patient may be at preventable risk for sexually transmitted infections, abuse, or unplanned pregnancy.3,4
The Adolescent Gynecologic Exam
Frequently, young female patients in the emergency department have not had a prior pelvic exam. If the current complaint necessitates a gynecologic exam, consent must be obtained from the adolescent. Reassurance and answering all questions prior to the exam should reduce patient and parental stress. Again, the parents should be excused from the room if the adolescent prefers, and a chaperone should accompany the provider. After the patient dons a gown, removes her undergarments, and is provided with a sheet to cover her lap, describe each step of the exam before you start the exam and again as you perform the exam. Use appropriately sized specula to minimize discomfort. First, an external exam should be performed, looking for infectious lesions, signs of vaginitis, and also any signs of abuse (note that in the majority of exams, even if there is abuse, there are no signs). Second, a speculum exam is performed to inspect the cervix and vaginal vault for bleeding, discharge from the cervical os, cervical lesions, or other abnormalities. Finally, a bimanual exam should be performed to detect any adnexal tenderness, masses, or cervical motion tenderness.
Updates on Issues of Confidentiality
Confidentiality is paramount in this age group. A teenage patient will want to know that certain services can be provided confidentially (i.e., without parental consent or notification), including the diagnosis and treatment of sexually transmitted infections or pregnancy. By law, parents are not allowed to force an adolescent to undergo a pregnancy test nor tests for drugs of abuse. However, confidentiality has limits that should be explained to the adolescent patient. Specifically, sexual and physical abuse are not protected under minor consent laws, and they require parental notification for the safety of the minor unless the parent is the one suspected of abusing the patient.
Vaginal Bleeding
Overview. Vaginal bleeding is a common complaint in the emergency department. In adults, the differential diagnosis of vaginal bleeding in the non-pregnant patient includes fibroids, polyps, or malignancy. However, in the adolescent patient, this complaint is most commonly due to dysfunctional uterine bleeding with anovulation (95%) and, much less frequently, due to pathologies such as bleeding dyscrasias, endocrine disorders, or malignancy.5-7 Although it is outside the scope of this review, it is also important to consider complications of pregnancy, such as spontaneous abortion or ectopic pregnancy, in the differential diagnosis of irregular vaginal bleeding in the adolescent patient. A negative pregnancy test is critical prior to consideration of other etiologies of vaginal bleeding.
Pathophysiology and Differential Diagnosis of Vaginal Bleeding. Dysfunctional uterine bleeding (DUB), the most common cause of abnormal vaginal bleeding in the adolescent, is defined as irregular uterine bleeding not due to structural lesions or systemic diseases. In adolescents, anovulatory cycles are responsible for the majority of DUB. Anovulation is caused by the relative immaturity of the hypothalamic-pituitary-ovarian axis in this age group. During the first two years after menarche, 55-80% of cycles are anovulatory; by year four or five of menstruation, only 20% of cycles are anovulatory.4-7
Polycystic ovarian syndrome (PCOS) is the most common endocrine cause of anovulatory cycles and resulting DUB. The syndrome is diagnosed clinically by symptoms including hirsutism and irregular menstrual cycles. PCOS is associated with insulin resistance and obesity, although 10% of PCOS patients are normal or under weight. The finding of polycystic ovaries on a transvaginal ultrasound supports the diagnosis, although it is not required for the clinical diagnosis of PCOS. The suspicion of this syndrome warrants referral to gynecology, adolescent medicine, or a family practitioner for further workup.7,8
In the differential of adolescent abnormal uterine bleeding, another etiology for the emergency physician to consider, though much less common, is a bleeding dyscrasia. The emergency provider may be the first physician to encounter patients with an underlying bleeding disorder, as heavy menstrual bleeding is the most commonly experienced sequela. In a series of studies, patients requiring hospitalization for menstrual bleeding had a 5-28% prevalence of bleeding disorders. Many of these patients will enter the hospital through the emergency department.9,10 While it is not crucial that the emergency provider make the final diagnosis of the particular bleeding disorder, it is imperative to include a bleeding disorder in the differential, especially in those patients with a positive family history, patients with heavy bleeding at menarche, or those requiring transfusion and admission. Also, once hormonal treatments are started, it is much more difficult to make a diagnosis of a blood dyscrasia.
Clinical Features and History of Vaginal Bleeding. The evaluation of vaginal bleeding should start with an assessment of the patient’s hemodynamic stability. Unstable or potentially unstable patients should have two large-bore IVs established and volume replacement with isotonic saline and packed red blood cells, if indicated.
The initial history of this complaint should include the onset and timing of the bleeding, including timing in relation to the last normal menstrual cycle and duration of bleeding. Inquire about regularity and duration of cycles and the age of menarche. The patient should try to quantify the bleeding, which may be difficult; ask specifically how frequently she is changing pads/tampons. Also ask specifically if she saw any clots with the bleeding.
In addition to the above general historical questions, further questions may help narrow the differential diagnosis of vaginal bleeding. For example, ovulatory cycle bleeding should be preceded by premenstrual symptoms (breast tenderness, bloating, mood swings, or cramping). Heavy, irregular bleeding without these preceding complaints is often triggered by an anovulatory cycle.5,8 Ask about a history of excessive bleeding (such as after dental procedures or prolonged nosebleeds) to screen for bleeding disorders, and similarly ask about family history of bleeding disorders and gynecologic issues.11 As always with the complaint of vaginal bleeding, ask about the potential of pregnancy, while keeping in consideration that patients are not always truthful about their sexual history and that a pregnancy test should be performed regardless.
Diagnostic Studies. Emergency department laboratory investigation for vaginal bleeding should always include a pregnancy test and a complete blood count. In patients requiring transfusion, with suspected bleeding disorder, or being considered for admission, order a coagulation panel and type and cross. In the pregnant patient, a pelvic ultrasound should be obtained to evaluate for possible ectopic pregnancy and for viability of the pregnancy. It would be helpful to draw LH, FSH, and TSH levels and a von Willebrand’s panel (VWP) because initiation of hormone therapy (to blunt bleeding) will invalidate LH and FSH results, while blood transfusion will alter the accuracy of the VWP test.
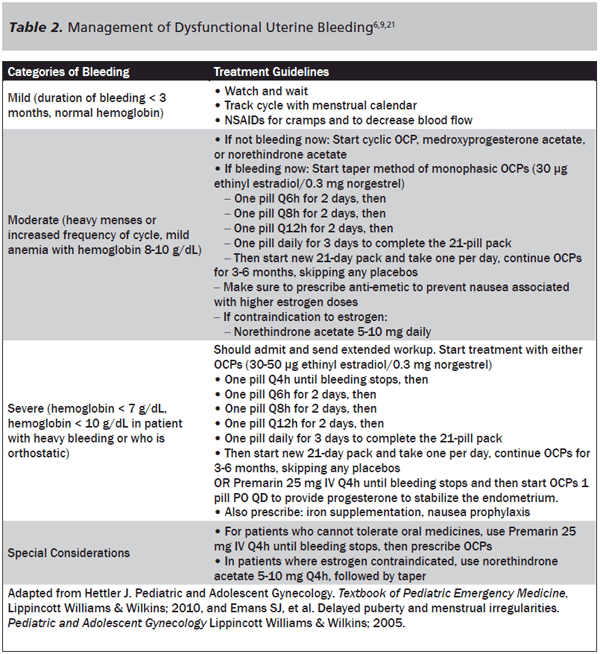
Treatment. The treatment choice for dysfunctional uterine bleeding will be guided by the volume of bleeding and by the results of the lab work obtained. Mild bleeding may be followed expectantly, for example, while moderate bleeding may prompt the emergency physician to start medication to slow bleeding. The patient should always be instructed to follow up with her primary care physician in case long-term OCPs are required to control bleeding, or in case further workup is needed to discover the etiology. In Table 2, the specifics of treatment plans and the levels of bleeding or anemia for which they are indicated are outlined in detail.
Sexually Transmitted Infections
Scope of Problem: The Rise of Sexually Transmitted Infections in Adolescents. Sexually transmitted infections (STIs) are an important emergency department complaint, and recent data show a rise in prevalence of many of these infections in adolescents. The CDC’s Division of Reproductive Health tracks the nationwide trends in sexually transmitted infections. The major findings in the 2002-2007 data included a rise in the prevalence of HIV in adolescents as well as in rates of syphilis. From 1996 to 2006, the rate of HIV in males aged 15-19 years nearly doubled. Many EDs are now using rapid HIV testing and some are even piloting universal testing in high prevalence areas such as Washington, DC.13,14 Similarly, the incidence of syphilis, which had been steadily declining between 1997-2005, has risen again, affecting 2.2 individuals per 100,000 in 2006, versus only 1.5 per 100,000 in 2004. Gonorrhea infection rates have plateaued in recent years after a decline for more than 20 years.13-15
Risk Factors for Sexually Transmitted Infections (STIs) in Adolescents. Multiple factors place this age group at risk for higher rates of all STIs. It is important, even in the often hectic environment of the emergency department, to screen higher-risk adolescents, including those with early sexual debut, multiple partners, inconsistent use of condoms, limited health care access, drug use, and men having sex with men. Remember that minors have the right in all states to confidential care for sexually transmitted infections.
Some physiologic features place the teenage patient at higher risk for contraction of STIs. The adolescent-aged host frequently has a more naïve immune system to sexually transmitted infections. Other anatomic differences in this age group place the patient at higher risk. Adolescent women have a larger cervical ectropion than adults, thus increasing the STI risk because these cells have greater susceptibility to infection than other types of cervical cells.
History Taking for Patients with Suspected Sexually Transmitted Infection. The complaints that bring an adolescent patient to the emergency department for an STI may include vaginal discharge, pruritis, dysuria, dyspareunia, abdominal pain, or even just a request for STI testing with fears of an exposure. Gonorrhea produces symptoms an average of 10 days after exposure, and may include urinary discomfort, vaginal discharge, dyspareunia, and also pelvic pain — remember to consider pelvic inflammatory disease and related sequelae, including tuboovarian abscesses. Another manifestation of this STI may be Bartholin’s gland abscesses, so when treating a gland abscess, screen for STI risk factors and consider empiric treatment. On the other hand, chlamydia is frequently asymptomatic. Up to 42% of patients affected by gonorrhea have a concomitant infection with chlamydia, necessitating testing and treatment for both, as addressed in Table 3.15
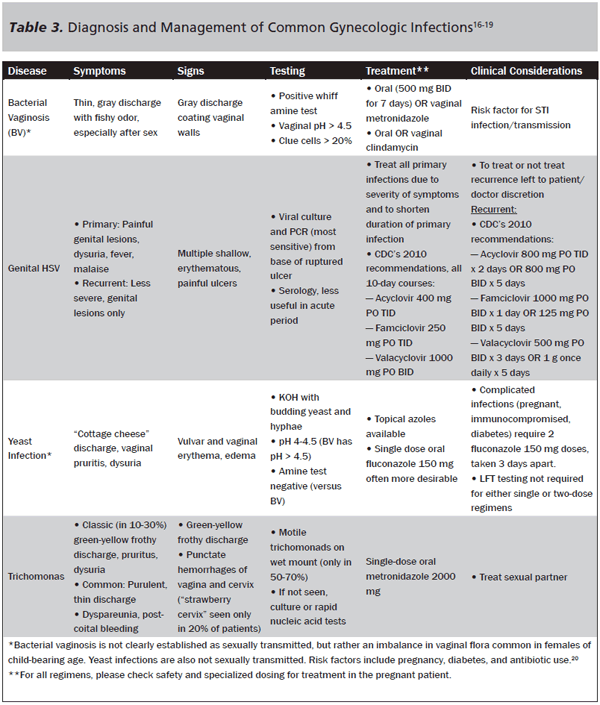
Treatment and Follow-up for Suspected Sexually Transmitted Infections. Because the adolescent patient may be difficult to contact for follow-up culture results, empiric treatment is indicated if the suspicion of disease is high. Remember that given confidentiality laws, the minor herself, rather than the parents, must be contacted with follow-up cultures. It may be useful to send test results to the primary care physician in order to ensure the results are delivered confidentially and in a setting in which that provider can initiate treatment and counseling.
Other Considerations in Gonorrhea and Chlamydia Testing: New Testing Modalities and Follow-up Testing. Gonorrhea and chlamydia can be tested for routinely in the emergency department with endocervical or self- or physician-administered vaginal swabs. These infections can also be tested by urine testing, but require a first void or “dirty” urine sample, while another common test collected during workup for abdominal complaints, a urinalysis for bacterial infection, is done mid-stream. However, mid-stream urine testing for chlamydia has been shown to be sensitive, making simultaneous collection for both STIs and urinary tract infections in the emergency department much simpler.18
All patients with gonorrhea or chlamydia require retesting in 3 months to ensure clearance of the disease, given its potential for long-term harm, including infertility and pelvic inflammatory disease. If the infection is present at this follow-up, it is more likely to be due to re-infection rather than resistant infection. Proper education to the adolescent patient is imperative, including notification of all partners from the 60 days prior to diagnosis and instructions to abstain from sexual activity until 7 days after initiation of treatment of both partners. Patients should be advised to follow up with their primary care provider to initiate partner treatment/notification if tests come back positive.15,21
The presence of one sexually transmitted infection portends the risk for other concomitant infections, including human immunodeficiency virus (HIV). The emergency physician evaluating a patient for gonorrhea and chlamydia should consider ordering testing for syphilis and HIV to do a complete STI workup. Alternatively, if the emergency physician can ensure reliable follow-up, these additional screening tests may be performed by the primary care provider.22
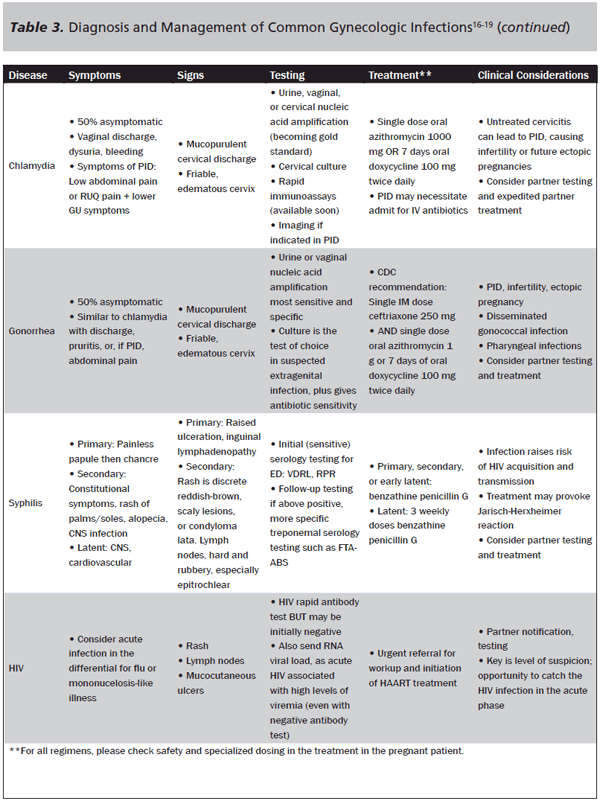
Alternative Treatment Options in Gonorrhea/Chlamydia. Treatment regimens for gonorrhea and chlamydia are found in Table 3. If the adolescent patient refuses an intramuscular injection, there are oral-only regimens, although these are not recommended as first line because of quinolone resistance by Neisseria gonorrhoeae. However, if local gonorrhea resistance is low and the patient is also at low risk, the provider could alternatively prescribe:
- single dose cefixime 400 mg PO; or
- levofloxacin 500 mg PO daily for 7 days; or
- ofloxacin 300 mg PO BID for 7 days; or
- erythromycin base 500 mg PO QID for 7 days.
This should be prescribed in addition to the single dose of azithromycin 1 g PO, or doxycycline 100 mg PO BID for 7 days, to prevent resistance.21
The Possibility of Resistant Neisseria Gonorrhoeae. There has been growing concern about cephalosporin-resistant Neisseria gonorrhoeae. The 2010 CDC recommendations continue to support the regimen of ceftriaxone 250 mg IM once plus azithromycin 1 g orally once or doxycycline 100 mg PO BID for 7 days.21 Laboratories are identifying small, although notable rates of resistance in both gonorrhea and chlamydia cultures. However, there is insufficient prevalence of resistant strains to warrant significant changes to the current treatment recommendations. The recommendation is ceftriaxone plus azithromycin for dual coverage against gonorrhea to prevent further resistance.17,23
The emergency practitioner should watch for any future updates in CDC recommendations as concerns for resistance grow.
Emergency Contraception
Background and Epidemiology. Teen pregnancy in the United States had been decreasing annually during 1991-2005, but subsequently increased again from 2005-2007, at a rate now of approximately 42.5 affected young women per 1,000.15,24 The emergency provider’s role in prevention of unplanned pregnancy is limited to the provision of emergency contraception. Any patient presenting to the emergency department for a pregnancy test who has had unprotected vaginal sex or contraceptive failure in the past 120 hours is a candidate for emergency contraception.
Indications for Emergency Contraception. The main indications to prescribe this class of medications are: unprotected sex, sexual assault, or failure of a contraceptive. Failures of prescribed contraceptives may include: a contraceptive vaginal ring in place for more than 5 weeks, contraceptive vaginal ring out for more than 3 hours, broken condoms, or missed doses of oral/vaginal/injection contraceptives. (See Table 4.)

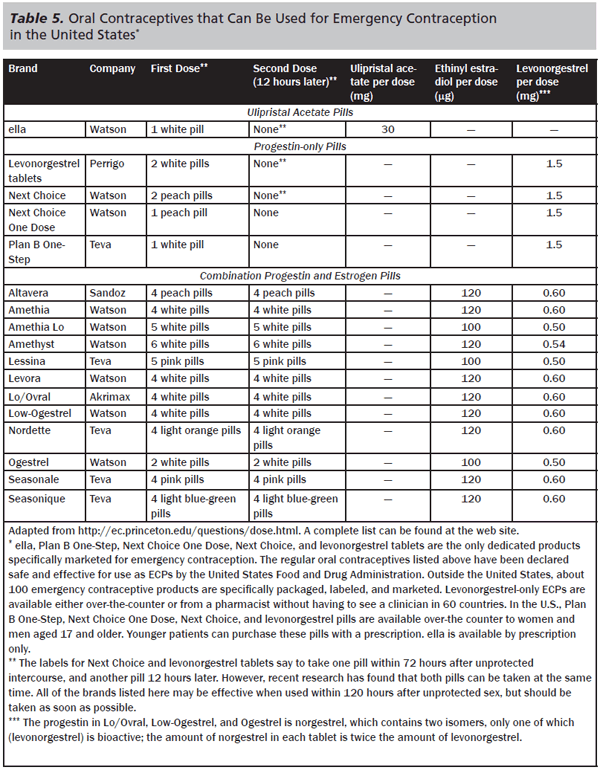
Treatment Regimens in Emergency Contraception. Originally, two main categories of emergency contraception existed: combination pills, sometimes referred to as the Yuzpe regimen, and progesterone-only pills.25,26 The Yuzpe regimen’s use is limited by severe nausea and vomiting as side effects and lower efficacy compared to other emergency contraception options. Only 57% of pregnancies are prevented by Yuzpe method versus 85% with levonorgestrel-only pills. Many brands of regular oral contraceptive pills can be used, in combinations unique to each brand, to provide emergency contraception. (See Table 5.) A complete list of approved pills is available at the Emergency Contraception website: http://ec.princeton.edu/questions/dose.html.
Levonorgestrel (trade name Plan B/Next Choice) is approved for use within 72 hours of unprotected sex, although the World Health Organization has shown efficacy up to 120 hours.
In 2010, the FDA approved ulipristal acetate (UPA, trade name ella), a progesterone receptor modulator. Its efficacy is proven up to 120 hours after unprotected sex, taken in a single 30-mg dose. In fact, if taken within 72 hours, UPA had a 42% lower pregnancy rate than levonorgestrel. If taken within 24 hours, UPA had a 65% lower pregnancy rate compared to levonorgestrel.11,27 However, the provider must keep in mind that UPA is not yet widely available in U.S. pharmacies.
Finally, another option, although it requires training for placement or immediate referral to a gynecologist/family practitioner, is the copper intrauterine device. If the patient has guaranteed follow-up with a provider who can place a copper IUD, this device may prevent up to 99.9% of pregnancies if it can be inserted within 5 days of unprotected sex.
In summary, the emergency provider’s options include (in increasing order of efficacy): traditional OCP packs in regimens particular to each brand; levonorgestrel only (trade names Plan B or Next Choice); a new medication called ulipristal acetate (trade name ella); or the patient may be referred for emergency copper IUD.
It is imperative to counsel the patient on the following issues: close follow-up, the possibility of emergency contraception failure, and future contraceptive plans. Teens may ask the provider if emergency contraception will terminate an existing pregnancy. They should be educated that emergency contraception is not an abortive agent. Levonorgestrel works by delaying ovulation, and UPA may prevent ovulation, thus neither will disrupt an already fertilized and implanted pregnancy.11 Possible side effects to be communicated to the patient can include nausea/vomiting, headaches, and menstrual-like cramping. All patients should have a negative pregnancy test in the emergency department before UPA is prescribed.
Contraindications to Use of Emergency Contraception. For both the Yuzpe method and levonorgestrel emergency contraceptives, the only contraindications to use are allergy to the drugs or current pregnancy (only due to fact that emergency contraception will not be effective in case of confirmed pregnancy).
Legal and Confidentiality Considerations for Emergency Contraception. A physician can prescribe and also provide the so-called “morning-after pill” to the adolescent patient without parental consent or notification.19,28 In addition, legislation is now expanding to cover this aspect of women’s health. In 17 states, it is now law that health care facilities must offer emergency contraception to sexual assault patients.26 As of 2009, levonorgestrel-only emergency contraception pills are available “behind the counter,” with a form of identification, for men and women aged 17 years and older in all 50 states. Patients 16 years of age and younger require a prescription from the physician, except in nine states where laws have been passed to allow pharmacists to dispense emergency contraception pills without a prescription. These pharmacists must work in collaboration with a physician or have undergone specialized training to female patients of any age.11,19,28
Conclusion
In this review, the important considerations for the adolescent patient with a gynecologic complaint and subjects that are unique to this age group have been discussed. The emergency provider must obtain a complete and confidential history and physical exam. Many chief complaints warrant a consideration of the genitourinary system, as teenage patients are not always forthcoming with gynecologic complaints. The text has reviewed the common etiologies, workup, and treatment for abnormal uterine bleeding, one of the most common adolescent emergency department complaints. Emergency physicians must understand the current testing and treatment recommendations for sexually transmitted infections; patterns of resistance may change first-line recommendations in the future. The frequency of co-infection with multiple sexually transmitted infections should be considered. The report also reviewed the current treatment options and legality issues in the use of emergency contraception. This is meant as an overview of the unique issues in treating the adolescent female patient in the emergency department and as an update to the provider on the current topics in the gynecologic health of this population.
References
- Khan MR, et al. Longitudinal associations between adolescent alcohol use and adulthood sexual risk behavior and sexually transmitted infection in the United States: Assessment of differences by race. Am J Public Health 2012;102(5):867-876.
- Nusbaum M, Hamilton C. The proactive sexual health history. Am Fam Physician 2002;66(9):1705-1712.
- Causey AL, et al. Pregnant adolescents in the emergency department: Diagnosed and not diagnosed. Am J Emerg Med 1997;15(2):125-129.
- Sanfilippo JS, Lara-Torre E. Adolescent gynecology. Obstetrics and Gynecology 2009;113(4):935-947.
- Hertweck P, Yoost J. Common problems in pediatric and adolescent gynecology. Medscape Expert Review of Gynecology. http://www.medscape.org/view-article/720869; updated 4 May 2011. Accessed online 3/12/2012.
- Hettler J. Pediatric and adolescent gynecology. Textbook of Pediatric Emergency Medicine. Philadelphia, PA: Lippincott Williams & Wilkins; 2010.
- Strickland JL, Wall JW. Abnormal uterine bleeding in adolescents. Obstetrics and Gynecology Clin North Am 2003;30(2):321-335.
- Rosenfield RL. Clinical features and diagnosis of polycystic ovary syndrome in adolescents. In: Middleman AB, Geffner M, eds. UptoDate. Waltham, MA. Updated 6/15/2011. Accessed online 7/5/2012.
- Emans SJ, Laufer MR, Goldstein DP, eds. Dysfunctional uterine bleeding. Pediatric and Adolescent Gynecology, 5th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2005.
- Halimen S. Menorrhagia and bleeding disorders in adolescent females. English translation, from Hamostaseologie. 2012; volume 32.
- Duffy K, Gold MA. Adolescents and emergency contraception: Update 2011. Curr Opin Obstetrics & Gynecology 2011;23(5):328-333.
- Thomas MC. Treatment options for dysfunctional uterine bleeding. The Nurse Practitioner 2011;36(8):14-20.
- Hewitt P. EDs reluctant to grow routine HIV testing programs. Ann Emerg Med 2011;57(4):A16-A18.
- Kenen J. Routine HIV testing in the ED: The experience in the nation’s capitol. Ann Emerg Med 2011;57(4):0.
- Gavin L, MacKay AP, Brown K, et al. Sexual and reproductive health of persons aged 10-24 years — United States, 2002-2007. MMWR Surveillance Summary 2009;58(6):1-58.
- Cernik C, et al. The treatment of herpes simplex infections: An evidence-based review. Arch Intern Med 2008;168(11):1137-1144.
- Ison CA. Antimicrobial resistance in sexually transmitted infections in the developed world: Implications for rational treatment. Curr Opin Infect Dis 2012;25(1):73-78.
- Mangin D, et al. Chlamydia trachomatis testing sensitivity in midstream compared with first-void urine specimens. Ann Family Med 2012;10(1):50-53.
- Update on Emergency Contraception. Association of Reproductive Health Professionals. http://www.arhp.org/publications-and-resources/clinical-proceedings/ec. Updated March 2011. Accessed online 6/26/2012.
- Fethers K, et al. Bacterial vaginosis (BV) candidate bacteria: Associations with BV and behavioural practices in sexually-experienced and inexperienced women. PloS One 2012;7(2):e30633.
- Sexually Transmitted Diseases Treatment Guidelines, 2010. Centers for Disease Control website. http://www.cdc.gov/std/treatment/2010/. Updated August 2012. Accessed online 9/10/2012.
- McCabe E, Jaffe LR, Diaz A. Human immunodeficiency virus seropositivity in adolescents with syphilis. Pediatrics 1993;92(5):695-698.
- Tanaka M. Emergence of multidrug-resistant Neisseria gonorrhoeae strains circulating worldwide. Int J Urology 2012;19(2):98-99.
- Klein JD; American Academy of Pediatrics Committee on Adolescence. Adolescent pregnancy: Current trends and issues. Pediatrics 2005;116:281-286.
- Cremer M, Masch R. Emergency contraception: Past, present and future. Minerva Ginecologica 2010;62(4): 361-371.
- Emergency Contraceptive Pills and Adolescents. Expert faculty discussion forum. Medscape. http://www.medscape.org/viewarticle/470268. Updated February 2004. Accessed online 6/1/2012.
- Glasier AF, et al. Ulipristal acetate versus levonorgestrel for emergency contraception: A randomised noninferiority trial and meta-analysis. Lancet 2010;375(9714):555-562.
- Q&A About OTC Access to Emergency Contraception (EC), for Healthcare Providers. Office of Population Research & Association of Reproductive Health Professionals, Princeton University. http://ec.princeton.edu/questions/QA-OTC-access.html. Updated 6/14/2012. Accessed online 7/8/2012.
- Goodwin KD, et al. Protecting adolescents’ right to seek treatment for sexually transmitted diseases without parental consent: The Arizona experience with Senate Bill 1309. Public Health Reports 2012;127(3):253-258.
- LaCour DE, et al. Review: Dysfunctional uterine bleeding in adolescent females associated with endocrine causes and medical conditions. J Pediatric and Adolescent Gynecology 2010;23(2):62-70.
- Norwitz ER, Park JS. Overview of the etiology and evaluation of vaginal bleeding in pregnant women. In: Barss VA, ed. UpToDate. Waltham, MA, 2012. Updated January 2012. Accessed 8/18/2012.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
