More women moving to LARC methods — Will your facility follow the trend?
More women moving to LARC methods — Will your facility follow the trend?
Over 95% of 2012 Contraception Survey responses see rise in LARC usage
When it comes to family planning, more women are choosing long-acting reversible contraception (LARC) methods such as intrauterine devices (IUDs) and the contraceptive implant, say respondents to the 2012 Contraceptive Technology Update Contraception Survey. More than 95% of survey participants say women are choosing such methods, which is a jump over 2011’s 85% response. In 2011, 47.17% of respondents indicated they had performed 11 or more IUD insertions. In 2012, that number jumped to 62.5%. For implants, 59.3% in 2011 said their facility offered or planned to offer the implant. In 2012, that number rose to 63.4%.
What has led to the increase? There are several factors at play at Planned Parenthood of Southwest and Central Florida in Tampa, says Sharon Carlisle, CNM, lead clinician. More clinicians now are trained to insert intrauterine contraception, and there is a greater acceptance by clinicians of LARC methods as first-line contraception, she notes. More IUD insertions are being conducted immediately post surgical abortion or at the post medical abortion follow-up visit, says Carlisle. Also, screening for sexually transmitted infections are now primarily performed at the time of insertion, if indicated, says Carlisle.
Donna Gray, CNM, WHNP, clinician at the Wyoming County Men’s and Women’s Reproductive Health Services in Silver Springs, NY, says, “We are spending more time discussing LARC [methods]. Clients are willing to try them because they can’t remember oral contraceptives [OCs].” Gray described the cost of OCs as “ridiculous” in terms of the insurance plans’ high deductibles. Pill copay costs run between $50 and $75 per month, she says, “and clients can’t afford this.”
Copays of $50 to $75 per month mean that clients are paying $650 to $985 per year, says Robert Hatcher, MD, MPH, professor of gynecology and obstetrics at Emory University School of Medicine in Atlanta. This amount makes the cost of long-acting reversible methods that can be used for 3-10 years quite attractive compared to the cost of pills, he notes.
More women request the contraceptive implant (Nexplanon, Merck & Co. of Whitehouse Station, NJ), or IUDs than the contraceptive vaginal ring or transdermal patch, says Dolores Conroy, ARNP, senior advanced nurse practitioner specialist and nurse practitioner supervisor at Gulf County Health Department in Port Saint Joe, FL.
Jocelyn Stowell, CNM, ARNP, nurse practitioner at Liberty and Calhoun County Health Departments in Bristol and Blountstown, FL, says, “We promote the use of LARCs because of ease of use and low failure rates. Also, we have both Mirena and ParaGard available and a provider trained to put them in. We should have Nexplanon available soon also.”
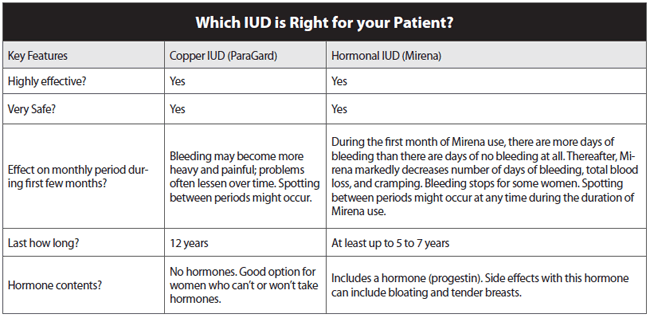
Clinician familiarity with LARC methods can make a difference in their use, says Debbie Wright, MSN, OGNP, nurse practitioner at the University of Wisconsin — Eau Claire Student Health Center. The student health center offers all three LARC methods, she notes. Wright, who estimates she performed 11-25 IUD insertions in 2012, says her familiarity with such methods, coupled with product advertising and the advocacy of a university human sexuality instructor, all have influenced the growing acceptance of long-acting methods among student women. (See the box below to get tips on helping women choose the right IUD for their needs.)
Counseling is key
How important is provider counseling when it comes to successful LARC use? It is “critical,” says Jeffrey Peipert, MD, MPH, MHA, Robert J. Perry professor of obstetrics and gynecology and vice chair for clinical research at Washington University School of Medicine in St. Louis. Definitive research from the Contraceptive CHOICE project in St. Louis, which was designed to evaluate reversible birth control methods, found that LARC methods are more effective than pills, patches, or rings in preventing unplanned pregnancy.1 Women who used birth control pills, the patch or vaginal ring were 20 times more likely to have an unintended pregnancy than those who used longer-acting forms such as an intrauterine device or implant.1
First, when choosing a contraceptive method, patients should be aware that LARC methods are the top-tier reversible options when it comes to effectiveness, notes Peipert, who served as lead investigator of the CHOICE research. Second, patients must be counseled regarding the potential side effects of each LARC method. They should be reassured that irregular and unpredictable bleeding are side effects of all three LARC methods, he notes.
In Mirena users, bleeding typically gets lighter over time and amenorrhea is common, Peipert observes. With the copper IUD, menses typically become regular, but flow might be slighter heavier. With the implant, the bleeding pattern is unpredictable, and patients must accept the fact that the implant can cause irregular bleeding, he states.
Studies have shown that structured counseling on the potential side effects of the contraceptive method has the potential to improve continuation and satisfaction rates, says Peipert.2 Patients should be counseled regarding side effects and potential non-contraceptive benefits of each method, he explains. “Mirena, for example, can control heaving bleeding and decrease dysmenorrhea, [while] Nexplanon also may reduce dysmenorrhea and may improve acne in women who have acne at baseline,” Peipert states. “Both IUDs reduce the risk of endometrial cancer.”
One of the reasons Norplant, the first contraceptive implant, was withdrawn from the market was the class action lawsuits against the pharmaceutical company that produced the method, observes Peipert. Women contended that they had not been adequately warned about Norplant’s possible side effects, such as irregular menstrual bleeding, headaches, nausea, and depression, he states. “Thus, for all contraceptive methods including LARC, patients should be carefully counseled about the risks, benefits, and alternatives for each method,” he states.
Knock down barriers
What are the barriers to increasing LARC access? David Turok, MD, MPH, associate professor of obstetrics and gynecology and codirector of the family planning fellowship at the Salt Lake City-based University of Utah, points to four misperceptions:
- Providers don’t have time for counseling.
- IUDs hurt, they’re hard to get in, and expensive.
- Too much irregular bleeding with the implant.
- Women discontinue the methods too quickly.3
Turok, who spoke at the meeting of the Association of Reproductive Health Professionals on the Contraceptive CHOICE Project, advises that clinics identify a staff member who is familiar with LARC methods to perform regular follow-up on IUD and implant users to ensure patient satisfaction with the methods. Women using LARC methods had the highest satisfaction at their one-year follow-up in the CHOICE project, which employed phone interviews to check method use at three, six, 12, 18, 24, 30, and 36 months post enrollment.4
Having a staff member connect with people and express some interest in their continued satisfaction with whatever method they have chosen seems to be important in people continuing with a method, Turok states. This person might not be the most highly credentialed staff member, but someone who is familiar with the benefits and disadvantages of LARC methods and can communicate those, he notes.
Acknowledge the imperfections that come with LARC methods. Expect failed insertions and higher rates of expulsion/removal, Turok notes.
“Keep your eye on the prize,” says Turok of LARC methods. “Increasing their use has the potential to dramatically decrease unintended pregnancies.” (Use English and Spanish versions of the “Get It & Forget It” patient information insert to talk with women about LARC.)
References
- Winner B, Peipert JF, Zhao Q, et al. Effectiveness of long-acting reversible contraception. N Engl J Med 2012; 366(21):1,998-2,007.
- Madden R, Mullersman JL, Omvig KJ, et al. Structured contraceptive counseling provided by the Contraceptive CHOICE Project. Contraception 2012. Doi: 10.1016/j.contraception.2012.07.015.
- Turok D. Maximizing LARC availability: bringing the lessons of the CHOICE Project to your community. Presented at the Reproductive Health 2012 conference. New Orleans; September 2012.
- Rosenstock JR, Peipert JF, Madden T, et al. Continuation of reversible contraception in teenagers and young women. Obstet Gynecol 2012; 120(6):1,298-1,305.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
