Look for careers beyond traditional CM roles
Look for careers beyond traditional CM roles
CM recognized for contributions to care
In today’s climate of healthcare reform and with the growing emphasis on quality, there are more opportunities for case managers than ever before.
The trend toward embedding case managers in physician offices and hospitals is increasing in many areas of the country, says Margaret Leonard, MS, RN-BC, FNP, senior vice president for clinical services at Hudson Health Plan with headquarters in Tarrytown, NY.
In her area, case managers are not only being embedded in physician practices and hospitals but insurance companies are starting to place case managers in federally qualified health centers.
“There also is a growing demand in psychiatric settings as providers realized that while they can take care of a patient’s psychosocial needs, many patients also have medical needs and can benefit from someone who can help them navigate the healthcare system and connect with a primary care medical home,” Leonard says.
Health homes offer opportunities
The new initiative from the Centers for Medicare & Medicaid Services that encourages providers and payers to work together to create Medicaid health homes also offers opportunities for case managers, Leonard adds. The Affordable Care Act provides a 90% funding match for organizations that become a health home, a model of care that emphasizes care coordination, she adds.
Larger payer organizations have professional case managers and have long appreciated the value of case management, adds B.K. Kizziar, RN-BC, CCM, CLP, owner of B.K. & Associates, a Southlake, TX, case management consulting firm. In addition, physician practices are beginning to recognize the value of case management, especially if they are part of a medical home model or accountable care organization, she says.
“Case managers are a commodity right now, and the need will only grow over the next few years,” says Toni Cesta, RN, PhD, FAAN, senior vice president, operational efficiency and capacity management at Lutheran Medical Center in Brooklyn, and partner and consultant in Dallas-based Case Management Concepts.
She predicts that the demand for case managers will increase as case managers are employed across the continuum of care.
Not enough nurses
The only problem with the increased demand for case managers is that there aren’t enough nurses and social workers to take care of everything some patients need, especially when patients need help accessing community resources, Leonard adds.
“My concern is that if physicians believe they can’t afford adding a case manager to their staff, they’re going to assign the job to a medical assistant or office staff. At present, there’s nothing that adequately defines care coordination or the credentials of case managers,” Kizziar adds.
Leonard points to an increase in the use of non-clinical staff called peer specialists or patient navigators who are well trained and are supervised by the case managers. “They can accompany patients to the pharmacy, help them sign up for medication assistance plans or go with them to the Housing Authority and guide them through the application process,” Leonard says.
Today’s healthcare environment offers numerous opportunities for case managers who want to work independently as individuals and companies seek help in navigating the complex healthcare system, Kizziar says.
“Case managers who want to be self-employed are going to have to create their own opportunities by selling the idea of case management to organizations that in the past may not have understood the need for it. The challenge in becoming an independent case manager is that nurses and social workers are not accustomed to marketing themselves,” Kizziar says.
Coordinating care
Some case managers have started businesses that coordinate care for senior citizens whose relatives live in another part of the country, Kizziar says.
“The family members want someone to make sure their relatives are getting the medical care they need, that they have enough food and can live safely at home,” Kizziar says. Case managers who want to be independent have numerous opportunities to contract with individuals or businesses, but they have to find their niche and market themselves, Kizziar says.
Some employers are contracting with case managers to assist employees in choosing the best insurance plan for their individual situations. “They aren’t selling the product. They’re providing counsel to people who may not understand the array of benefits packages available,” she says. Employers want their employees to have the policy that’s best for them because, in the long run, it will save them money, she adds. “Having employees well and at work is a win-win situation for everyone,” she says.
Leonard is part of a team from the Case Management Society of America (CMSA) who have been meeting with the Centers for Medicare & Medicaid Services on developing payment codes for case management services. “We are working to get reimbursement for case management services no matter where the care is delivered,” she says.
Kizziar, who works with hospitals around the country, reports that she hasn’t seen much change in salaries and doesn’t expect to until the economy improves.
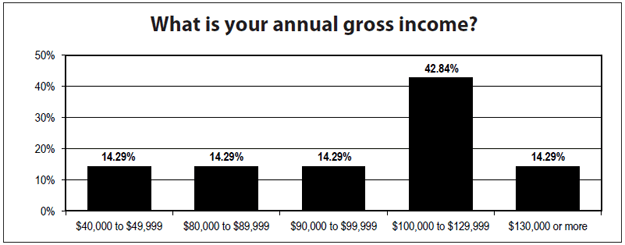
The majority of case managers who responded to Case Management Advisor’s annual salary survey (57%) reported salaries of $100,000 or more, and 42% reported that their salary didn’t change last year.
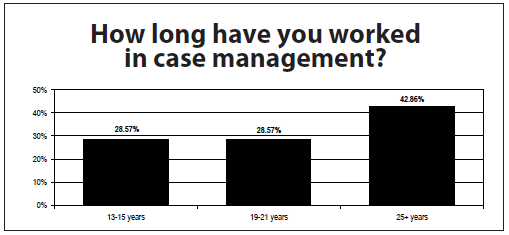
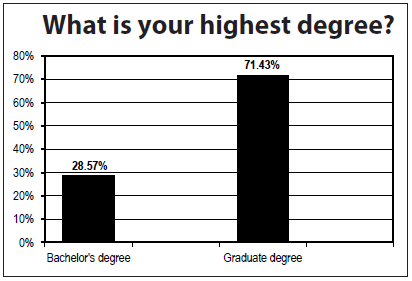
Case managers who responded to the survey are older, experienced, and well educated, with 100% reporting 25 years or more in the healthcare field and 43% who report being a case manager 25 years or longer. The majority of respondents (71%) report holding a graduate degree and 85% are age 56 or older.
The good news for case managers is that while employers might not be adding more staff, they aren’t laying off case managers either, Kizziar says.

“From what I hear from colleagues, the case management staff is not being affected when there are mergers and acquisitions. There is some consolidation, but the organizations are not touching the case management positions,” Leonard adds.
In todays climate of healthcare reform and with the growing emphasis on quality, there are more opportunities for case managers than ever before.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
