Salaries on the rise
Salaries on the rise
HPR survey shows raises are back on the table
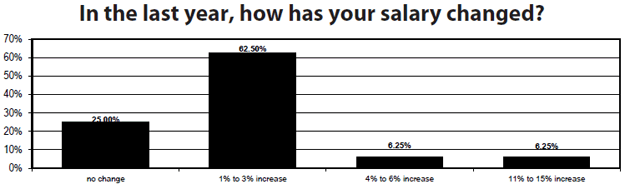
Two years ago, when Hospital Peer Review did its salary survey, we were in the midst of the deepest recession that this country had known since the Great Depression. And salaries reflected that. Some who responded to the survey had experienced cuts in their salaries, and a third of them reported they hadn’t had a raise that year. This year, three-quarters of the respondents reported a raise in salary. Half of them said the increase was just 1-3%, but there were others who were seeing a raise of greater than 5%.
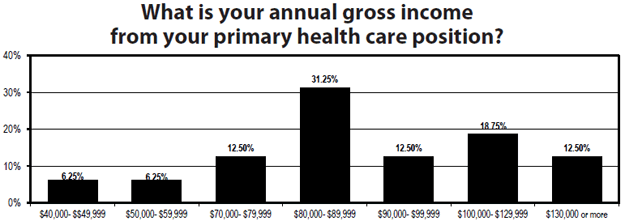
Salaries are mostly in the same range, with about half of respondents making between $40,000 and $80,000 per year, a bit more than 30% taking home between $80,000 and $89,000 annually, and an eighth earning in the $90,000-99,000 range. Nearly a third make more than $100,000.
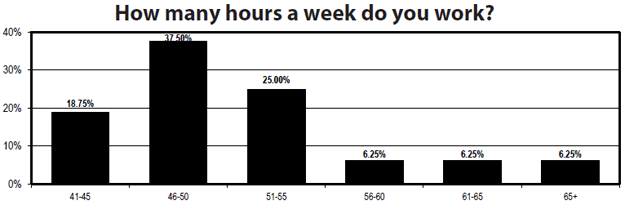
People are working more for their pay and earning those raises. While in 2010 there were some respondents who weren’t working full time and just one working more than 60 hours a week, everyone is pulling at least 40 hours a week this time. And just less than 20% are working 56 hours a week or more. Most work between 46 and 55 hours a week.
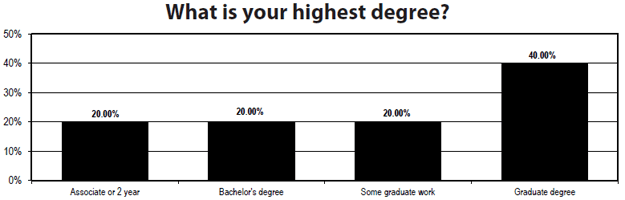
There seems to be more room for less educated staff, which may indicate a loosening of the purse strings for new hires. There are some respondents who have two-year degrees or two years of college. Two years ago, everyone had at least a bachelor’s degree, and more than half had a graduate degree of some sort. Two-thirds either had an advanced degree or had spent some time in graduate school. This year’s survey shows 40% with a graduate degree, and 20% in each of the other categories: AA degree, bachelors degree, and some graduate work.
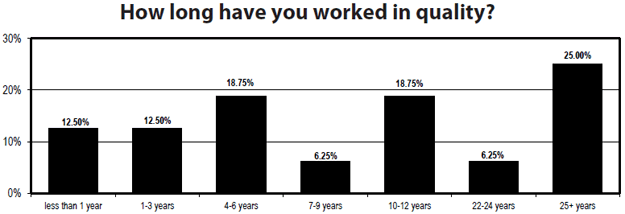
The experience level of quality professionals is impressive. A quarter of respondents said they had spent at least a quarter of a century working in the quality arena. Another quarter had worked as quality professionals for between 10 and 24 years. Just an eighth clocked less than a year in the setting. Everyone had at least 10 years in healthcare in general, but more than two-thirds had more than 25 years.
That experience is reflected in the age of respondents. Nearly three-quarters are over 50, with a fifth in the 51-55 range, 40% in the 56-60 range, and another 13% aged 61-65. There are some youngsters, though: 20% are younger than 40. But given that age and experience level, there is probably going to be some difficulty finding the kind of experience that hospitals have now as their current quality leaders retire.
Changing job, changing need
That’s something on the mind of many people in healthcare. “It is hard to find the right person,” says Larry Mandelkehr, MBA, CPHQ, director of the department of performance improvement at the UNC Health Care System in Chapel Hill, NC. “We will have to create the right environment to retain staff — a combination of challenging work, a supportive environment, and flexibility.” And to do that, he says, it’s entirely likely they’ll have to pay more in salary. “Finding the right match is hard and more important than the budget.”
He adds that they will add staff as the things that have to be measured, abstracted, or acted upon increase. That means that more core measures — and there are two more just announced by The Joint Commission (see story page 10) — means more staff are needed.
To get one of the jobs — new or replacing someone who left — the right candidate will have to have something special, and for Mandelkehr, that likely means Lean or Six Sigma certification. “It is becoming the norm,” he says. Familiarity with Affordable Care Act programs is also a plus for candidates.
The person who is successful on the job will be someone who is good at managing multiple projects. “They will have to be able to split their time into small slices, managing more projects, processes, and reportable measures,” Mandelkehr says.
Jerod Loeb, PhD, has seen great changes in the quality improvement field during his tenure at The Joint Commission. Currently executive vice president for the division of healthcare quality evaluation, he has spent nearly 20 years there breathing the quality message.
He thinks that knowing about high-reliability organizations will be a key for successful quality professionals in the future. As for how many such people an organization will need, that will depend in part on how much quality measurement has “been made a byproduct of healthcare delivery through use of electronic health records.”
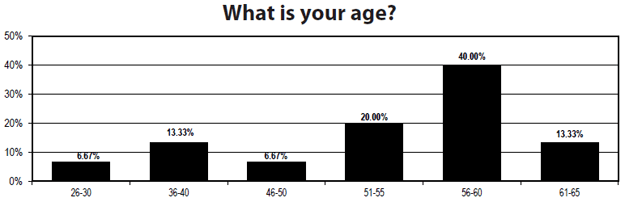
Retention is important, though. There is an aging workforce, and more emphasis on quality than ever, Loeb says. “Creating and maintaining a superior culture will help to retain the best and the brightest. But this is true within and outside of the sharp end of health care delivery.”
Loeb thinks that the end result of Meaningful Use will have a big impact on quality as a subsection of healthcare.
In her 30 years in healthcare, Mary Ann Holt, RN, MSN, a partner at IMA Consulting in Chadds Ford, PA, has seen quality improvement roles change from someone managing daily operations to someone looking intently at the way in which healthcare is delivered.
She thinks one of the key changes in the role to come is that the traditional silos separating functions, units, departments, and points on the continuum are going to disappear, or at least become less evident. If heart failure readmission rates are bad, you can’t just look at a bunch of parallel events to figure it out. You have to look at the way things intersect and interact. Pharmacy needs to look at medication reconciliation; nursing needs to focus on patient education; case management needs to look at the continuum of care. “And all of them need to understand they are working on the same thing,” says Holt.
Knowing how to communicate with providers at every level both within your facility and also outside it, elsewhere on the continuum of care, is going to be a vital element to success in QI. “Communications are more important now with the outpatient environment,” she says. “Quality managers need to be more aware of cultivating relationships with internal and external stakeholders.”
Accountable care organizations are a focus, as is service line management. So quality managers are going to have to step up and be the bridge between in- and outpatient providers. “As much as we depend on technology, that won’t be the solution, either,” Holt says. “Patient stays are at three or four days.” She remembers being a nurse at the bedside when newly admitted diabetes patients stayed in the hospital for five days, and cardiac cath-lab patients stayed three. Now it’s outpatient for one and six hours for the other. There isn’t a lot providers can do in a short patient stay regarding communicating with rehab and the outpatient physicians. “You will have to be that bridge. You will have to help every point on the continuum control costs and control readmissions.”
Help them learn what they need
Other skills she thinks are vital to a successful quality manager include reading financial reports and having a basic level of business education. “That’s not part of most nurses’ education, but if they move into quality positions, they will need it.”
She gives every member of her staff and everyone she mentors a subscription to the Harvard Business Review. It provides a wealth of business knowledge and ideas that can be poached from other industries for use in healthcare. It’s not a wild notion any more, with Lean management and airline reliability theories floating down the halls of the best facilities.
Look for formal classes — sometimes there are business classes that offer continuing education units, Holt says — or informal ways to improve your knowledge. Ask someone in the finance department to mentor you. Indeed, ramping up the mentoring system in your facility is one way you can help just about everyone do a better job at almost anything. “Some organizations are better than others at finding internal mentors for people. Be one of the good ones.”
Holt says you will probably have to find some expertise from within your organization — there just isn’t enough talent out there to replace everyone who will retire in the coming years. That makes identifying mentors even more important. Look at your board members, department heads, and directors and see what their skill set is. If you have people on staff who could use some of what they know, foster that. “We can’t just promote people and not support them in their new role,” she says. “You can’t say you’ll help educate someone for a new job and not follow through.”
For more information on this topic, contact:
- Larry Mandelkehr, MBA, CPHQ, Director, UNC Health Care System, Department of Performance Improvement, Chapel Hill, NC. Email: [email protected]. Telephone: 919-966-0488.
- Jerod Loeb, Ph.D., Executive Vice President, Division of Healthcare Quality Evaluation, The Joint Commission, Oakbrook Terrace, IL. Email: [email protected].
- Mary Ann Holt, RN, MSN, Partner, IMA Consulting, Chadds Ford, PA. Telephone: (866) 840-0151.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
