Palliative Care in the Emergency Department
Palliative Care in the Emergency Department
Authors: Travis E. DeVader, MD, Medical Director, Hospice and Palliative Care Services, Attending Physician, Department of Emergency Medicine, Kaweah Delta Medical Center, Visalia, CA.
Tammie E. Quest, MD, Director, Emory Palliative Care Center, Emory University, Atlanta, GA.
Peer Reviewer: Corita Grudzen, MD, MSHS, Assistant Professor, Department of Emergency Medicine, Mt. Sinai School of Medicine, Assistant Professor, Brookdale Department of Geriatrics and Palliative Medicine, Mt. Sinai School of Medicine, New York, NY.
The paradigm I grew up with in emergency medicine is that there are a limited number of ways to die, and our role was to intervene and prevent death using the principles of A, B, and C: airway, breathing, and circulation. This concept works well for the previously healthy acutely ill or injured patient. But for the patient nearing the end of a life-limiting illness, it is not appropriate and can even be cruel. The introduction of palliative care to the emergency department at first seems out of place; that is the place where patients are snatched from the jaws of death. But as the authors of this issue explain, the ABC of resuscitation can be revised to the ABCD of palliative care assessment to provide better care to patients and families in times of crisis.
— J. Stephan Stapczynski, MD, Editor
Introduction
Palliative care is the physical, spiritual, psychological, and social care provided to patients and families suffering with serious, life-threatening illness, no matter the stage of illness, and includes all treatment options, including those that are curative. In the emergency department (ED), we care for patients across the spectrum of illness. Most practicing emergency clinicians were not formally trained in the core competencies of palliative care, which include exquisite pain and symptom control as well as communication skills.
This article uses a case example to highlight how the areas of palliative care and emergency medicine intersect. It serves to introduce the key concepts of palliative care that are useful for practicing emergency clinicians. Although palliative care is not limited to caring for patients at the end of life, when patients do present with life-limiting illness, the emergency clinician should be prepared to care for these patients skillfully. By the end of this article, the reader should be able to define palliative care, understand its role in the ED, explain the utility of providing palliative care in the ED, and be able to apply the key concepts of symptom management in daily practice.
Case Study in Emergency Palliative Care
It is in the middle of a very busy shift. You are working in the area of your ED known as the critical zone. You have just finished intubating a patient with a large hemorrhagic stroke when the radio goes off again. “A 43-year-old male with respiratory distress. Severely altered. GCS 3. Tachycardic. Pressure is borderline at 100 systolic. Tachypnea noted. 91% on 15 L non-rebreather. ETA 5 minutes.”
This article is intended to be a primer in palliative care for the emergency clinician. We will follow the progress of our patient in our case example throughout the article and use his ED visit as a way to educate in the core principles of palliative care. The objectives include: defining palliative care; discussing acute and chronic illness trajectories; describing a rapid palliative care assessment; identifying symptom management in the actively dying patient; and when to obtain a palliative care consult. Barriers to providing palliative care in the ED, misperceptions, and pitfalls will also be explored.
Introduction: An Expanding Field
The specialty of emergency medicine (EM) functions to rapidly assess patients and quickly initiate life-sustaining measures in an effort to save lives and reduce injury. Increasingly, emergency clinicians see patients of all ages with more chronic illness burden who are living longer with their serious illnesses, who are in need of pain and symptom management, and who often are struggling with caregiver and support care needs. As a reflection of this increase, up to one-third of ED deaths are due to the effects of chronic disease.1 Consistent with previous studies, a recent report from Australia notes that nearly 70% of patients who died made at least one visit to the ED prior to death, with the mean number of ED visits at 1.9 per patient.2,3 In 2006 alone, there was less than a 1% increase in cancer diagnoses, but a 20% increase in ED visits for cancer patients.4 This, along with the fact that in 2006 nearly one-quarter of a million patients died in EDs in the United States, has begun to force emergency providers to ask if they are “doing the right thing” for their patients.5
When the end of life approaches, patients and families may intersect the ED for acute symptom management and other terminal illness needs. It is important that emergency providers have core palliative care skills. The American College of Emergency Physicians (ACEP) has issued a policy statement on the emergency physician’s role in establishing advance directives and providing end-of-life care.6 This, combined with the support for hospice and palliative medicine as a subspecialty, has spurred the evolution of emergency palliative care.
Leaders in the field of EM also collaborated to begin educating more emergency providers in the core content of palliative care via the Education in Palliative and End-of-Life Care for Emergency Medicine (EPEC-EM).7 EPEC-EM has trained hundreds of emergency providers of all disciplines in palliative care skills necessary in the ED.
While considerable progress is being made in training practicing emergency physicians, current evidence suggests that knowledge and practice gaps still occur. While those practicing emergency medicine see the utility in providing palliative care, only 10% of EM residents described palliative care in the ED as desirable and feasible.5 Less than one-half of participating EM residents reported receiving formal training in pain management and managing the imminently dying patient, while less than 55% reported receiving training in managing the hospice patient and withholding and withdrawing life-sustaining therapies.8 EM residents reported receiving the most training in the legalities of end-of-life care and advance directives and little training in symptom management.9
Several recent studies have proven that providing palliative care in the ED is feasible. A pilot project in a community ED with a palliative care consult service provided 78 ED consults in four months.10 A convenience sample study of 50 elderly adults with chronic medical conditions found that more than one-half of the patients had unmet needs in the areas of physical symptom management, financial need, mental health needs, and lacking access to care, with the mean quality of life reported as 3.62 on the McGill Quality of Life index (range of possible responses 0-10).11 Evidence suggests that palliative care that begins in the ED may improve the process to allow patients and families to get the right care more efficiently. An interventional study in an urban ED was able to provide 894 palliative care consultations, in which 29% qualified for home health care services and 32% qualified for hospice. Ninety percent of the patients were admitted to the hospital, but the time to palliative care consultation decreased from 5 to 3 days and hospital length of stay was decreased from 5 to 4 days.12
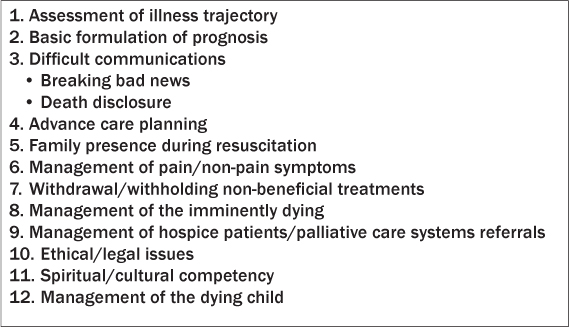
Table 1 lists 12 core competencies in palliative care that have been identified for the practicing emergency provider.13
Table 1: Palliative Care Core Competencies for Emergency Physicians13

Palliative care providers view the ED as the ideal place to begin to provide palliative care in order to alleviate the time the patient spends in the hospital suffering from symptoms before the palliative care consult is placed. A delay in the palliative care consult has unintended costs to the patient, his or her family, and the health care system as a whole.14 However, the ideal model for providing palliative care in the ED remains unknown. Since both emergency medicine and palliative care are relatively new specialties, little is known regarding the use of palliative care services in the ED and which patient populations stand to gain from a collaboration of the two fields.
Definitions
Palliative care is specialized medical care for patients with serious illnesses with the goal of improving the quality of life for both patients and families. Palliative care is much more than just medicine. It is a psychosocial model of care that includes assessments and treatment plans from the physician, nursing staff, pharmacists, social workers, chaplains, and alternative medicine practitioners. The goal of the palliative care team is to improve the quality of life for the patient and relieve distressing symptoms. Palliative care is provided in conjunction with traditional, life-sustaining, curative medical care.15
Hospice is a specialized part of palliative care that focuses on the care of the terminally ill. Patients enrolled in hospice have a prognosis of six months or less to live if the disease runs its usual course. Patients who unexpectedly outlive their prognosis can be recertified for an unlimited number of enrollment periods as long as they continue to have an expected prognosis of six months or less to live if the disease runs its usual course. Hospice care can be provided in an inpatient setting, including an acute care hospital, nursing facility, or a dedicated hospice facility. However, it is most often provided in the patient’s home. As part of the hospice benefit, the patient and family are provided with all of the durable medical equipment needed to provide care for the patient, all hospice diagnosis-related medications, and at least weekly nursing visits.
Due to recent health care reform via the Affordable Care Act, the hospice benefit for children suffering from terminal illness has changed. Pediatric patients can now receive both curative treatments and symptom-directed treatments while concurrently being enrolled in hospice. This new model of hospice care for children is designed to provide maximum support to patients and their families and to provide the best possible symptom management. It is too soon to tell if concurrent care will be enacted under the adult hospice benefit.
Illness Trajectories
There are four identifiable illness trajectories for patients with life-limiting illness. The first illness trajectory is sudden death. These are patients who arrive to the ED dead or die in the ED shortly after arrival from a sudden life-ending event such as major trauma, massive myocardial infarction (MI), intracranial hemorrhage, or massive pulmonary embolism (PE). The second trajectory is that of a terminal illness. The most commonly thought of terminal illness is cancer. At the time of diagnosis, the patient is usually high functioning and can maintain that level of function for most of the illness until the patient experiences a rapid decline in loss of function, progressing to death.
The third illness trajectory is organ failure. Patients who die from organ failure experience their disease as a set of crises. For instance, a patient with severe chronic obstructive pulmonary disease (COPD) has a baseline function, and with each subsequent exacerbation, loses some of that functional capacity. Eventually, an exacerbation will lead to the patient’s death.
The last trajectory is frailty. These patients usually reside in nursing homes. The classic example of a frail patient is the Alzheimer’s patient who has lost the ability to speak, is bed-bound, and refuses most food. Often, these patients are sent to the ED for altered mental status and fever.
Illness Trajectories for ED Patients
These traditional illness trajectories may not speak to the illness trajectories experienced by ED patients who are approaching the end of life. There are seven identified trajectories that are unique to the ED. First are patients who arrive dead. Second are patients who have had resuscitation attempted by EMS and who subsequently die in the ED. The third are patients who also may be successfully resuscitated in the field and survive until hospital admission. The fourth trajectory is defined as patients with a terminal illness who present to the ED, most likely due to symptoms out of control. The fifth trajectory includes frail, usually elderly patients who may present to the ED and are hovering near death. The sixth trajectory are patients who are alive and interactive when they arrive in the ED but arrest in the ED. Finally, the seventh trajectory are patients who die but who may have had a potentially preventable death.16
These seven scenarios in which providing palliative care is beneficial to the patients and families are unique to the ED setting. By identifying which illness trajectory a patient is experiencing and where on the death trajectory the patient currently is, the emergency care provider can more accurately identify those patients who would benefit from early palliative care.
The most common presenting complaint to the ED in patients of all death trajectories is shortness of breath, followed by neurological complaints including altered mental status. The rate of intensive care unit (ICU) admission and subsequent death was highest for the sudden death trajectory (third trajectory), followed by terminal illness (fourth trajectory). Pain was highest in the terminal illness death trajectory.17
There are three important assumptions made within this framework of end-of-life care. First, the patient, family, and health care provider agree that death is imminent. The second assumption is that the health care team knows and understands the disease trajectory of the patient. The final assumption is that all aspects of palliative care have time to be attended to, including bereavement care.18 While there has been one successful pilot program using volunteers to provide the family with bereavement care both during and after the ED visit, this is not the norm.19
Case Example Continued
EMS arrives and places your patient in a resuscitation bay. There has been virtually no significant change in condition since you received the radio communication. The patient’s eyes are closed and do not open to painful stimuli. Pupils are 3 mm and reactive. He barely moves his right arm to sternal rub. His skin feels warm. He appears chronically ill with mild to moderate temporal wasting. He is cachectic. There is tachycardia at 120. No murmurs, gallops, or rubs on exam. No JVD. He is tachypneic at 35 with a mild to moderate amount of accessory muscle use. No retractions are noted. Lung sounds are decreased throughout and course in the bases. No peripheral edema is noted. The feet are cold and the plantar surfaces are mottled. The nurses are placing the patient on a monitor and getting a full set of vital signs, including pulse oximetry and a core temperature. You are prepared to intubate. What is the most appropriate next step in the management of this patient?
A Changing Culture
There has been a recent explosion of interest in emergency medicine to manage acute resuscitation in the context of defining goals of care.
The Rapid Palliative Care Assessment
When a critical patient arrives in the ED, there is a large mobilization of resources aimed at resuscitation. While the emergency physician always needs to focus on the primary assessment of the critically ill patient, he or she can integrate a Rapid Palliative Care Assessment that may further aid in establishing the patient’s goals of care. While concurrently conducting the airway, breathing, circulation assessment, the physician can be performing the ABCD assessment of emergency palliative care.
• A: Advance care plan. The physician should clarify whether the patient has any advance directives. If so, did they arrive with the patient or who has access to them? If the physician has access to a written advance directive, the physician should promptly review it to determine what the patient’s goals of care are in this emergency situation. This has become easier in recent years with the institution by many states of the Physicians Orders for Life Sustaining Treatment (POLST) form.
• B: Can we make the patient better with good symptom management? Whether advance directives have been identified or not, the physician should then quickly perform a symptoms assessment and treat the patient in an effort to make the patient feel better.
• C: Is there a caregiver? Ascertain whether or not there are caregivers who need to be involved in the decision-making process or whether they have important medical information that could be shared with health care providers at this time.
• D: Decision-making capacity. Finally, determine if the patient has decision-making capacity. Patients do not automatically lose decision-making capacity in the face of unstable vital signs. Determine if the patient can receive, process, contemplate, and verbalize a decision.
Table 2: Rapid Palliative Care Assessment

Common Presentations for Terminally Ill Patients
Emergency care providers need to ascertain why the patient is in the ED. Assuming that all patients come to the ED to seek life-sustaining aggressive medical interventions is a flawed assumption and leads to unwanted treatments, increased suffering, and unwanted resuscitations. Often, the emergency physician may be left wondering why a patient who is terminally ill, especially if he or she is receiving hospice services, presents to the ED. The rules for caring for a hospice patient in the ED can be confusing.20
There are five common reasons for terminally ill patients to present to the ED. The first and foremost reason for presentation to the ED is severe symptom burden. Second, patients experience problems with access to outpatient care, either in the form of too long of a wait to be seen or being too sick to be seen in the outpatient setting. Third, financial barriers prove to be another reason for ED presentation. Either patients could not afford to miss work or could not afford the outpatient care. Fourth, miscommunication between patients and health care providers, especially if the patient’s primary language is not English, causes patients to seek care in the ED. Fifth, mixed messages sent by health care providers prompt ED visits, especially when these mixed messages involve prognosis.21
A review of terminally ill patients found that when patients presented to the ED for symptom management issues, nearly all patients were advised to go to the ED by another physician, and all patients and caregivers felt either unprepared to manage the symptom at home or felt that the symptom could not be managed at home. During their ED visit, patients and caregivers noted a lack of communication between the emergency physician and the primary care physician, as well as lack of communication about what was happening during the ED stay. This led to increased anxiety on the part of the patient and caregiver.22
ED use within the last two weeks of life has been determined to be a marker of poor quality of life. Thus, research has been conducted to try and identify those patients who are at risk for making an ED visit. For patients with all diagnoses, weight loss, decrease in cognition, male gender, and overnight admission to a hospital within the previous two weeks have been identified as risk factors for making an ED visit.23 In a study of hospice patients with end-stage cardiac disease, patients were less likely to make an ED visit if they had a do-not-resuscitate order (DNR) in place, were older and Caucasian, had greater frequencies of home visits by nurses and chaplains, complied with medication, were taking morphine sulfate, had caregivers in the home, and had an emergency medicine kit in the home.24 For men with prostate cancer, receiving hospice services was associated with significantly fewer ED visits.25
ED patients who ultimately receive a palliative care consultation most often have the chief complaint of shortness of breath, followed by neurological complaints. Most patients had an Emergency Severity Index of level 2. Only 14-17% of these patients presented to the ED with a DNR order in place.26 If the ED visit was made during the last two weeks of life, 72% of the time the patient was admitted, and 77% of the admitted patients subsequently died in the acute care setting.27
ED Deaths of Terminally Ill Patients
Studies have found that 35-56% of ED deaths are secondary to incurable chronic illnesses in which death is the expected outcome.28,29 When palliative care is defined as providing analgesia, sedation, hydration, mouth care, repositioning for comfort, and providing emotional support to the patient and family, only half of the patients who die in the ED get this level of care. Specifically, 55% of patients received analgesia, emotional support was provided to the patient’s family 51% of the time, 35% received mouth care, and 33% received repositioning and sedation; emotional support was provided to the patient in only 24% of cases.30 While patients state in interviews that they do not want aggressive end-of-life care,21 only 12.5% make this request known to emergency staff.28 It appears that a large focus of ED nursing staff is preparing the body for viewing after death and allowing family adequate time for viewing,31 in addition to self-care in terms of debriefing,32 as opposed to symptom management.
The ED is not the ideal place of death due to lack of privacy, staff shortages, and inexperience of the staff in managing patients at the end of life.33 Yet, despite patients making preferences known for no ED transfer or hospitalization at the time of death, it often happens.34 Care of the dying has been shown to improve with end-of-life order sets, and these order sets have also been shown to improve clinician communication with patients and their families.35
To this point, all of the data have focused on adults with terminal illnesses. The field of pediatric palliative care is in its infancy, with even less data available than for adults. The field of emergency palliative care for children is virtually nonexistent, but there are data available for children who died in the ED. Of all children who died, most died at home, while 14% died in the ED, with the rate climbing to 22% if the child was not hospitalized in the last week of life.36 Interestingly, children with cancer comprised less than half of ED deaths. Children with cardiovascular disorders were six times more likely to die in the ED, those children with metabolic and genetic disorders were five times more likely to die in the ED, and children with neuromuscular disorders were four times more likely to die in the ED.36
Avoiding ED Transfer of Terminally Ill Patients
Given the fact that ED transfers in the last week of life as well as the ED as a place of death are viewed as poor quality-of-life and quality-of-death indicators, respectively, much effort has been made to avoid ED transfers in terminally ill patients. Just as the ED has examined how it can improve the care of these patients,37 primary and palliative care have focused on how to avoid unnecessary ED visits.
One of the reasons cited by terminally ill patients for ED utilization is lack of access to care.21 The data on whether intense primary care can avoid unnecessary ED visits are mixed. It appears that just having a primary care provider is not sufficient to avoid ED utilization. Those patients who experienced a high degree of continuity with the same primary care provider were almost 4 times less likely to utilize the ED; however, patients who had access to primary care but did not have a high degree of continuity with the same provider were much more likely to utilize the ED.38
An area of great concern for emergency physicians is the number of ED visits made by those patients in residential nursing facilities. Indeed, last-minute transfers to the ED when a patient is dying are often avoidable and unwanted by patients.34 Reasons for transfer of the residential nursing patient to the ED include: transfer to the ED is initiated only after all other potential options have been exhausted by facility staff; inadequate staffing leads to increased demands on staff that may not be adequately trained; primary care providers were not timely in answering pages, so staff felt obligated to transfer the patient if the condition continued to deteriorate; and residential care staff felt pressured by families of patients to “do something.”39
Attempts by palliative care models to avoid ED utilization have been mixed. Patients enrolled in an integrated service model of palliative care were less likely to utilize the ED. However, although the results were statistically significant, there was only a 6% reduction in ED utilization, resulting in 29% of patients enrolled in the service making at least one visit to the ED.40 Ontario, Canada introduced a $115.5 million End-of-Life Care Strategy that spanned three years. The overarching goal of the initiative was to keep terminally ill patients in the home-care setting, thus avoiding placing demands on the acute care system. Unfortunately, results one year after the start of the initiative show that ED utilization among terminally ill patients held steady at 16%.41
Case Example Continued
As the EMS crew was transferring the patient to the ED stretcher, the physician began to perform the Rapid Palliative Care Assessment. “Are there advance directives?” The EMS crew responded with a firm “No.” The EMS paperwork was handed to the physician and he quickly found a POLST form that had been prepared only two weeks earlier. According to the POLST, the patient desired a natural death, comfort measures only, with no artificial nutrition or hydration.
The ED nurse had already established an IV and was obtaining blood. The physician advised to draw labs but not to send them. He then called the emergency contact number as listed on the POLST and spoke with the patient’s wife. She stated that the patient had a brain tumor and “has really gone downhill in the past month.” The patient had not been eating or drinking, except sips, for one week. They physician briefly clarified the current POLST form and the family reiterated the desires as listed on the POLST. The family was advised to come to the ED to see the patient. With this new information, the physician was able to determine that the patient was on the terminal illness trajectory and likely only had hours to days to live.
The Role of Advance Directives
If attempts by primary and palliative care have failed to consistently reduce the rate of ED utilization by terminally ill patients, then these patients should have advance directives in place to guide the emergency physician. Caring for a terminally ill patient without advance directives in place continues to be a source of frustration for many emergency physicians. Unfortunately, the rate of advance directive ownership remains low. The National Center for Health Statistics reports that 28% of home-care patients, 65% of nursing home residents, and 88% of discharged hospice patients have at least one advance directive on record, with patients aged 85 years and older having the highest percentage of ownership.42 Fifty-six percent of nursing home patients had a DNR order, compared with 7% for home-care patients.42 Thus, large numbers of patients elect not to express their wishes in the form of advance directives.
Surveys of ED patients have shown varying levels of ownership and understanding of advance directives. Only 22-27% of ED patients have advance directives, and of those who have advance directives, only 23% brought them to the ED at the time of their visit.43-45 Factors associated with higher ownership rates of advance directives were having a primary care doctor, advanced age, and having a life-threatening disease or considering oneself to be very ill.43-45
While historically emergency physicians have felt that obtaining a DNR order or enforcing an advance directive is outside of the scope of practice,46,47 attitudes are changing. Clarifying patients’ advance directives or inquiring about forming advance directives has been well received by patients’ families. When families were contacted about a patient’s advance directive or code status, 85% of those conversations led to a DNR order in the ED, and 97% of the families contacted felt that it was appropriate for the emergency physician to contact them and have the conversation, regardless of the decision that was made.48 If the emergency physician does not contact the family regarding advance directives, then most of the time the task falls to a resident in academic institutions.49
Unfortunately, approximately 30% of ED patients have expressed their desire not to have advance directives in place.50 The reasons given for not wanting to form an advance directive include always wanting to have aggressive life-sustaining treatment, fear of not getting enough or proper treatment if an advance directive were in place, and fear of being allowed to die.50
Studies show that the use of advance directives in patients who live in residential care facilities varies from as little as 0% to 90%, with facilities that have more transfers to the ED having advance directives in place more often.51 Interestingly, requests for limited care or DNR are often documented in the medical record in more than one place, while a request for full resuscitation is documented in only one place in the medical record.52 Obtaining timely information continues to be a problem for emergency physicians, resulting in calls that residential nursing facilities standardize communication of advance directives and include the date when the information was last updated with the patient.53 Emergency physicians have reported difficulty in interpreting advance directives in the middle of an emergent visit, but have also reported being able to contact family in 90% of the cases in which they felt family input was important.51,52
Case Example Continued
After returning to the resuscitation room, the patient remained tachypneic. All monitoring was discontinued. In keeping with the patient’s and family’s goals of care, no labs were sent and no radiographic studies were performed. The patient was moved from the resuscitation bay to a private room in the ED.
What are the next steps? Does “comfort measures/DNR” imply no treatment is needed in the ED? Do you admit this patient to the hospital? How are you going to manage his dyspnea and respiratory distress without intubation or BIPAP?
Managing the Dying Patient
As previously noted, the three most cited reasons for presenting to the ED in terminally ill patients are pain, dyspnea, and neurological complaints. It can be frustrating for the emergency physician to manage these symptoms in the dying patient.
A pain crisis at the end of life can be unbearable for families to witness and for patients to experience. While the emergency physician cannot be expected to know all of the opioid conversions, a few key conversions are important to know. (See Table 3.) Some physicians get nervous when dispensing large doses of opioids.
Table 3: Equipotent Opioid Conversions (Approximate)
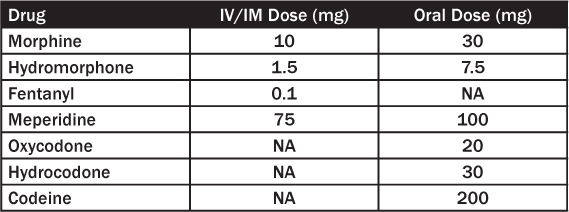
During a pain crisis, calculate the total daily morphine sulfate or hydromorphone dose and then convert to the IV equivalent (by dividing by 3 in both cases). Start by giving 10% of the total daily dose as an IV bolus. If you do not know the patient’s home medications, a safe starting dose of IV morphine sulfate is 0.1 mg/kg. The time to maximum concentration of IV opioids, and therefore maximum effect, is 10 minutes. Therefore, if the patient is still in severe pain after 10 minutes, double the initial IV bolus. Repeat this process of doubling the dose every 10 minutes until the patient is reporting pain improvement.
Dyspnea is the subjective feeling of not getting enough air. Patients describe this sensation as drowning, choking, or suffocating. Dyspnea does not equal respiratory distress, hypoxia, or tachypnea. Dyspnea is purely the patient’s experience of his or her breathing.
Managing the ABCs is the mantra of emergency medicine. However, outside of intubation and BIPAP, many emergency physicians are not trained in managing the subjective sensation of dyspnea. Researchers have identified that the same areas of the brain that control pain also control the sensation of dyspnea.54 Therefore, the mainstay treatment for dyspnea is opioids.54
Oxygen has been proven ineffective for the treatment of dyspnea in multiple studies, even in those patients who are hypoxic.55,56 A household fan that blows air across the patient’s face has been proven more effective than medical oxygen. Unless a patient has a reason to have bronchoconstriction as a cause of dyspnea, nebulizers have proven ineffective. All opioids, not just morphine sulfate, have been proven effective in the management of dyspnea.54,56,57
Patients at the end of life often experience an episode of delirium. Delirium is an acute change in a patient’s mental status. Delirium can be reversible (due to infections, medications, constipation) or irreversible (unknown cause or terminal delirium). If it is within the patient’s goals of care, an investigation for delirium should be focused on known reversible causes. Review the medication list and correlate new medications with the timing of delirium, obtain a chest X-ray to exclude pneumonia, obtain a urine sample to exclude urinary tract infection, and obtain an abdomen series to rule out constipation.
The mainstay of treatment for a presumed reversible delirium is antipsychotics, particularly haloperidol. If a patient is actively dying and has a presumed terminal delirium (hallmarks include talking to the deceased and picking at air), then the mainstay of treatment is benzodiazepines. The intent is to sedate the patient to retard the psychomotor agitation of the terminal delirium.58
Patients at the end of life may develop audible upper airway secretions, known by most family members as the “death rattle.” Anticholinergic medications are the treatment for terminal secretions. In the ED, glycopyrrolate 0.4–1.2 mg IV q 1-hour PRN secretions is the treatment of choice. Alternatively, atropine 1% ophthalmic solution can be administered two drops buccally q 1 hour PRN. Scopolamine patches can also be used to dry secretions, but this is not a realistic treatment in the ED given the 12-hour delay in onset of action.
Case Example Continued
The patient received morphine sulfate 2 mg IV as needed for tachypnea. He received a total of four doses over a two-hour period in the ED. The patient was also treated with lorazepam 1 mg IV. Lorazepam was given for tachypnea as well as signs of terminal delirium. On repeat exam, the patient was moving his right arm and picking at the air. Although the emergency physician educated the family about nonverbal signs of discomfort, the family interpreted this motion as discomfort and therefore requested treatment. The tachypnea resolved with both the morphine and lorazepam, the respiratory rate decreased from 35 to 20, and there was no accessory muscle use. Faint audible secretions began to develop in the ED, and the patient was treated with glycopyrrolate 0.4 mg IV. Secretions diminished and were no longer audible.
Models of Emergency Palliative Care
There is no one ideal model identified for providing emergency palliative care. Palliative care in the ED can be provided in one of three ways. First, care can be provided to ED patients by an established palliative care service. Second, a champion of palliative care in the ED can serve ED patients. This is usually an emergency physician who is either dually trained in EM and hospice and palliative medicine or has attended EPEC-EM. Finally, EDs have successfully partnered with local hospice agencies to provide care to patients in need. There are success stories using each model, and the model used in any particular community is usually dictated by the availability of local resources.59
A model that has been proposed but not yet validated is to define early goal-directed therapy for palliative care in the ED. EDs across the country already use early goal-directed therapies in a number of emergency situations, including acute myocardial infarction, acute coronary syndrome, pneumonia, sepsis, and stroke. Presumably, EDs could identify early therapies needed for patients’ overall comfort and symptom control and then ensure that these goals are at least started, if not met, in the ED.60 Using an approach that is already familiar to the emergency physician may improve compliance with established goals instead of creating new processes that have been shown to have poor compliance in the treatment of pain.61
Barriers to Emergency Palliative Care
Research to date has focused on which patients can best be served by providing palliative care in the ED, what the ideal role of the emergency physician should be, how providing palliative care in the ED affects health care utilization, and educating emergency providers on the fundamentals of palliative care.62 Identified barriers to providing palliative care in the ED include lack of education of emergency physicians in the key concepts in palliative care, lack of knowledge of available resources, time constraints of the ED, challenges of the physician-patient relationship, family dynamics, overstepping the traditional role of the ED, and legal concerns and comfort level of the treating physician.14,63 (See Table 4.)
Table 4: Barriers to Providing Palliative Care in the ED

Case Example Concluded
In our case example, the emergency physician treated this patient in an exemplary manner. The emergency physician did not get stuck in following the traditional ABC model of care when faced with an obtunded patient in respiratory distress. The physician performed the Rapid Palliative Care Assessment quickly, which led to the rapid identification of the patient’s goals of care. ED providers then gave care in a compassionate manner that was consistent with the patient’s stated goal of comfort.
After the emergency physician identified and complied with the goals of care and treated the patient accordingly, he contacted the local hospice agency. The hospice nurse responded to the ED, where she met the patient and provided psychosocial support to the family. She arranged for the patient’s pastor to visit him at the bedside. After she confirmed that the family wanted to take the patient home with hospice services, medical transport was arranged and the patient was discharged from the ED to home. The patient died peacefully surrounded by his family two days later.
Conclusion
Our case example highlights how palliative care could and should be incorporated into emergency medicine. Although many emergency physicians currently lack formal training in end-of-life care, studies show that this gap in knowledge is correctable. Unwanted resuscitations can be avoided if emergency personnel use the Rapid Palliative Care Assessment and aim to identify the patient’s goals of care early in the ED course rather than at the time of disposition.
Due to the increased numbers of patients with chronic disease and lack of access to care, the ED will remain the entry point for these patients when crises arise. Emergency physicians need training in symptom management for patients at the end of life since pain, dyspnea, and neurological complaints drive most ED visits. Partnering with local palliative care and hospice resources can reduce unnecessary and unwanted admissions to the acute care setting at the end of life.
Emergency palliative care is a rapidly evolving field. Emergency and palliative care physicians alike now see the benefits of providing palliative care in the emergency department. The model of emergency medicine is now shifting to providing the right level of care for the right patient at the right time for the life stage of the patient.
Barriers to providing palliative care in the ED will be overcome. Future research will focus on the impact that providing palliative care in the ED has on health care utilization, quality of life, and quality of death. Just as emergency medicine was born out of the necessity to quickly diagnose and treat patients with emergent life-threatening conditions, it will continue to evolve to be able to provide the necessary, quality end-of-life care that an aging, chronically ill population needs and deserves.
Additional Resources
There are two initiatives currently dedicated to emergency medicine providers. The Education in Palliative and End of Life Care-Emergency Medicine (EPEC-EM) project is dedicated to the education of emergency providers. The Center to Advance Palliative Care’s Improving Palliative Care in Emergency Medicine Project (IPAL-EM) has tools and resources for emergency providers to implement palliative care practice in their emergency medicine setting. For more information on these initiatives visit: EPEC-EM, http://www.epec.net/epec_em.php, and IPAL-EM at http://www.capc.org/ipal/ipal-em.
References
1. Kompanje EJ. The worst is yet to come. Many elderly patients with chronic terminal illnesses will eventually die in the emergency department. Intensive Care Med 2010;36:732-734.
2. Rosenwax LK, McNamara BA, Murray K, et al. Hospital and emergency department use in the last year of life: A baseline for future modifications to end-of-life care. Med J Aust 2011;194:570-573.
3. Katelaris AG. Time to rethink end-of-life care. Med J Aust 2011;194:563.
4. Pitts SR, Niska RW, Xu J, et al. National Hospital Ambulatory Medical Care Survey: 2006 emergency department summary. Natl Health Stat Report 2008:1-38.
5. Smith AK, Fisher J, Schonberg MA, et al. Am I doing the right thing? Provider perspectives on improving palliative care in the emergency department. Ann Emerg Med 2009;54:86-93, 93 e81.
6. Ethical issues in emergency department care at the end of life. Ann Emerg Med 2006;47:302.
7. EPEC. EPEC for Emergency Medicine. Chicago, IL: Northwestern University, 2011.
8. Lamba S, Pound A, Rella JG, et al. Emergency medicine resident education in palliative care: A needs assessment. J Palliat Med 2012;15:516-520.
9. Meo N, Hwang U, Morrison RS. Resident perceptions of palliative care training in the emergency department. J Palliat Med 2011;14:548-555.
10. Waugh DG. Palliative care project in the emergency department. J Palliat Med 2010;13:936.
11. Grudzen CR, Richardson LD, Morrison M, et al. Palliative care needs of seriously ill, older adults presenting to the emergency department. Acad Emerg Med 2010;17:1253-1257.
12. Mahony SO, Blank A, Simpson J, et al. Preliminary report of a palliative care and case management project in an emergency department for chronically ill elderly patients. J Urban Health 2008;85: 443-451.
13. Quest TE, Marco CA, Derse AR. Hospice and palliative medicine: New subspecialty, new opportunities. Ann Emerg Med 2009;54:94-102.
14. DeVader TE, Albrecht R, Reiter M. Initiating palliative care in the emergency department. J Emerg Med 2012;43: 803-810.
15. 2011 public opinion research on palliative care: A report based on research by public opinion strategies. 2011.
16. Chan GK. Trajectories of approaching death in the emergency department: Clinician narratives of patient transitions to the end of life. J Pain Symptom Manage 2011;42:864-881.
17. Lamba S, Nagurka R, Murano T, et al. Early identification of dying trajectories in emergency department patients: Potential impact on hospital care. J Palliat Med 2012;15:392-395.
18. Chan GK. End-of-life models and emergency department care. Acad Emerg Med 2004;11:79-86
19. Ting SM, Li P, Lau FL, et al. Acute bereavement care in the emergency department: Does the professional-supported volunteers model work? Eur J Emerg Med 1999;6:237-243.
20. Lamba S, Quest TE. Hospice care and the emergency department: Rules, regulations, and referrals. Ann Emerg Med 2011;57:282-290.
21. Grudzen CR, Stone SC, Mohanty SA, et al. “I want to be taking my own last breath”: Patients’ reflections on illness when presenting to the emergency department at the end of life. J Palliat Med 2011;14:293-296
22. Smith AK, Schonberg MA, Fisher J, et al. Emergency department experiences of acutely symptomatic patients with terminal illness and their family caregivers. J Pain Symptom Manage 2010;39: 972-981.
23. Brink P, Partanen L. Emergency department use among end-of-life home care clients. J Palliat Care 2011;27:224-228.
24. Schonwetter RS, Clark LD, Leedy SA, et al. Predicting emergency room visits and hospitalizations among hospice patients with cardiac disease. J Palliat Med 2008;11:1142-1150.
25. Bergman J, Kwan L, Fink A, et al. Hospice and emergency room use by disadvantaged men dying of prostate cancer. J Urol 2009;181:2084-2089.
26. Grudzen CR, Hwang U, Cohen JA, et al. Characteristics of emergency department patients who receive a palliative care consultation. J Palliat Med 2012;15: 396-399.
27. Barbera L, Taylor C, Dudgeon D. Why do patients with cancer visit the emergency department near the end of life? CMAJ 2010;182:563-568.
28. Tardy B, Venet C, Zeni F, et al. Death of terminally ill patients on a stretcher in the emergency department: A French specialty? Intensive Care Med 2002;28: 1625-1628.
29. Beynon T, Gomes B, Murtagh FE, et al. How common are palliative care needs among older people who die in the emergency department? Emerg Med J 2011;28:491-495.
30. Le Conte P, Riochet D, Batard E, et al. Death in emergency departments: A multicenter cross-sectional survey with analysis of withholding and withdrawing life support. Intensive Care Med 2010;36:765-772.
31. Beckstrand RL, Smith MD, Heaston S, et al. Emergency nurses’ perceptions of size, frequency, and magnitude of obstacles and supportive behaviors in end-of-life care. J Emerg Nurs 2008;34:290-300.
32. Norton CK, Hobson G, Kulm E. Palliative and end-of-life care in the emergency department: Guidelines for nurses. J Emerg Nurs 2011;37:240-245.
33. Clarke R. Improving end-of-life care in emergency departments. Emerg Nurse 2008;16:34-37.
34. Purdy W. Nursing home to emergency room? The troubling last transfer. Hastings Cent Rep 2002;32:46-48.
35. Paterson BC, Duncan R, Conway R, et al. Introduction of the Liverpool Care Pathway for end of life care to emergency medicine. Emerg Med J 2009;26:777-779.
36. Guertin MH, Cote-Brisson L, Major D, et al. Factors associated with death in the emergency department among children dying of complex chronic conditions: Population-based study. J Palliat Med 2009;12:819-825.
37. Pines JM, Asplin BR. Conference proceedings-improving the quality and efficiency of emergency care across the continuum: A systems approach. Acad Emerg Med 2011;18:655-661.
38. Burge F, Lawson B, Johnston G. Family physician continuity of care and emergency department use in end-of-life cancer care. Med Care 2003;41:992-1001.
39. Arendts G, Reibel T, Codde J, et al. Can transfers from residential aged care facilities to the emergency department be avoided through improved primary care services? Data from qualitative interviews. Australas J Ageing 2010;29:61-65.
40. Lawson BJ, Burge FI, McIntyre P, et al. Can the introduction of an integrated service model to an existing comprehensive palliative care service impact emergency department visits among enrolled patients? J Palliat Med 2009;12:245-252.
41. Seow H, Barbera L, Howell D, et al. Did Ontario’s end-of-life care strategy reduce acute care service use? Healthc Q 2010;13:93-100.
42. Jones AL, Moss AJ, Harris-Kojetin LD. Use of advance directives in long-term care populations. NCHS Data Brief 2011:1-8.
43. Llovera I, Mandel FS, Ryan JG, et al. Are emergency department patients thinking about advance directives? Acad Emerg Med 1997;4:976-980.
44. Llovera I, Ward MF, Ryan JG, et al. Why don’t emergency department patients have advance directives? Acad Emerg Med 1999;6:1054-1060.
45. Ishihara KK, Wrenn K, Wright SW, et al. Advance directives in the emergency department: Too few, too late. Acad Emerg Med 1996;3:50-53.
46. Thewes J. Playing with fire: Advance directives in the emergency department. Acad Emerg Med 1997;4:83-84.
47. Ritchie KS, Rubenstein EB, Valentine AD. Do-not-resuscitate orders in the emergency department. Am J Med 1992;93:586-587.
48. Balentine J, Gaeta T, Rao N, et al. Emergency department do-not-attempt-resuscitation orders: Next-of-kin response to the emergency physician. Acad Emerg Med 1996;3:54-57.
49. Wrenn K, Brody SL. Do-not-resuscitate orders in the emergency department. Am J Med 1992;92:129-133.
50. Taylor DM, Ugoni AM, Cameron PA, et al. Advance directives and emergency department patients: Ownership rates and perceptions of use. Intern Med J 2003;33:586-592.
51. Lahn M, Friedman B, Bijur P, et al. Advance directives in skilled nursing facility residents transferred to emergency departments. Acad Emerg Med 2001;8:1158-1162.
52. Weinick RM, Wilcox SR, Park ER, et al. Use of advance directives for nursing home residents in the emergency department. Am J Hosp Palliat Care 2008;25:179-183.
53. Pauls MA, Singer PA, Dubinsky I. Communicating advance directives from long-term care facilities to emergency departments. J Emerg Med 2001;21: 83-89.
54. al. PMe. An official American Thoracic Society Statement: Update on the mechanisms, assessment and management of dyspnea. Am J Respir Crit Care Med 2012;185:435-452.
55. E. CKQIK. Use of oxygen and opioids in the palliation of dyspnea in hypoxic and non-hypoxic palliative care patients: A prospective study. Support Care Cancer 2009;17:367-377.
56. Kamal A. Dyspnea review for the palliative care professional: Treatment goals and therapeutic options. J Palliat Med 2012;15:106-114.
57. Currow DCea. Once daily opioids for chronic dyspnea: A dose increment and pharmacovigilance study. J Pain Symptom Manage 2011;42:388-399.
58. al. ZKe. Delirium in palliative care patients: Focus on pharmacotherapy. Am J Hosp Palliat Care 2011;28:501-510.
59. Grudzen CR, Stone SC, Morrison RS. The palliative care model for emergency department patients with advanced illness. J Palliat Med 2011;14:945-950.
60. Lamba S. Early goal-directed palliative therapy in the emergency department: A step to move palliative care upstream. J Palliat Med 2009;12:767.
61. Stone S, Rodriguez L, Calder K. Lack of pain assessment for patients with cancer presenting to the emergency department with pain complaints: Can we improve with a simple intervention? J Palliat Med 2006;9:7-9.
62. Quest TE, Asplin BR, Cairns CB, et al. Research priorities for palliative and end-of-life care in the emergency setting. Acad Emerg Med 2011;18:e70-76.
63. Grudzen CR, Richardson LD, Hopper SS, et al. Does palliative care have a future in the emergency department? Discussions with attending emergency physicians. J Pain Symptom Manage 2012;43:1-9.
The paradigm I grew up with in emergency medicine is that there are a limited number of ways to die, and our role was to intervene and prevent death using the principles of A, B, and C: airway, breathing, and circulation. This concept works well for the previously healthy acutely ill or injured patient. But for the patient nearing the end of a life-limiting illness, it is not appropriate and can even be cruel. The introduction of palliative care to the emergency department at first seems out of place; that is the place where patients are snatched from the jaws of death. But as the authors of this issue explain, the ABC of resuscitation can be revised to the ABCD of palliative care assessment to provide better care to patients and families in times of crisis.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
