Qigong Reduces Depression in Women with Breast Cancer Receiving Radiotherapy
Qigong Reduces Depression in Women with Breast Cancer Receiving Radiotherapy
Abstract & Commentary
By Melissa Quick, DO, and David Kiefer, MD, Dr. Quick is PGY-2 Family Medicine Resident, Beth Israel Medical Center, New York, NY; Dr. Kiefer is Research Fellow, Department of Family Medicine, University of Wisconsin, and Clinical Assistant Professor of Medicine, Arizona Center for Integrative Medicine, University of Arizona, Tucson. Dr. Quick and Dr. Kiefer report no financial relationships relevant to this field of study.
This article originally appeared in the May 2013 issue of Integrative Medicine Alert.
Synopsis: Ninety-six women with breast cancer undergoing radiotherapy during a 5- to 6-week interval were randomized to either a qigong group or a wait-list control group. The results indicate that the women in the qigong group had clinically significantly less depressive symptoms and better quality of life than the control group.
Source: Chen Z, et al. Qigong improves quality of life in women undergoing radiotherapy for breast cancer: Results of a randomized controlled trial. Cancer 2013; Jan 25. doi: 10.1002/cncr.27904. [Epub ahead of print].
A recent study performed at the Fudan University Shanghai Cancer Center in Shangai, China (with collaboration from faculty at the University of Texas MD Anderson Cancer Center in Houston, Texas) identified women with breast cancer (stages 0-III) who had undergone breast surgery and were about to undergo radiotherapy (RT). Ninety-six eligible women participated in this study and were randomized to either a qigong group or a wait-list control (WLC) group. Specific inclusion criteria required that eligible women were 18 years or older; able to read, write, and speak Mandarin; and scheduled to receive 5-6 weeks of either inpatient or outpatient RT.
Baseline characteristics of the women were reported to be similar with regard to inpatient vs outpatient treatment, income, type of surgery, and prior chemotherapy. For the outpatient RT group, a form of adaptive randomization called minimization was used to randomly assign the women to either a qigong group or a WLC group. The inpatient RT group was assigned to cohorts to minimize bias. Women were excluded from this study if they self-reported prior regular qigong or tai chi practice in the last year.
The qigong program — a modified version known as “walking qigong” — involved five 40-minute qigong classes, all taught by the same government-licensed traditional Chinese medicine physician and qigong master, each week during the women’s 5 or 6 weeks of RT. Additionally, the treatment group was given a DVD and printed qigong materials, and the women were encouraged to practice qigong individually on days when they did not train with the qigong master and after they completed RT. The study reports adherence to the qigong program as high, with 30.4% of women attending 100% of the sessions, 65.2% attending 80% or more of the sessions, and 78.3% of women attending 50% or more of the sessions. Only 13% of women attended less than 20% of the sessions. The WLC group received the standard of care during the study and was offered access to a qigong program after the study ended.
Five major endpoints were assessed in this study via four separate questionnaires (validated and translated into Mandarin) and by saliva samples. Each endpoint was assessed before RT was initiated (T1), in the middle of RT (T2), during the last week of RT (T3), and finally, 1 and 3 months post-RT (T4 and T5). In brief, the endpoints were: symptoms of depression, assessed using the 20-item Center for Epidemiologic Studies Depression Scale (CES-D); fatigue, assessed using the 9-item Brief Fatigue Intervention (BFI); sleep disturbances, assessed via the 18-item Pittsburgh Sleep Quality Index (PSQI); overall quality of life (QOL), evaluated by the 28-item Functional Assessment of Cancer Therapy-General (FACT-G); and cortisol rhythm, evaluated via four saliva samples (waking, 45 minutes later, 8 hours later, and at bedtime) per day for 2 consecutive days.
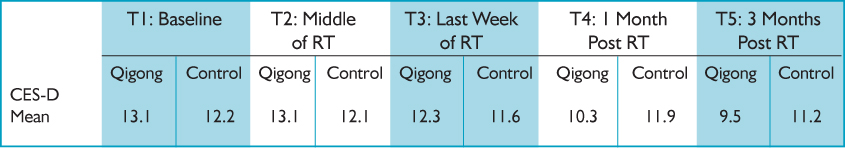
The main results of the study demonstrate statistically significant differences in changes in symptoms of depression over time for the qigong group but not for the WLC group (P = 0.05). Of note, both groups did demonstrate that depression scores decreased over time, regardless of intervention.
Interestingly, the results of the study display a consistent theme for all endpoints: the groups with high baseline depressive symptoms displayed a significant difference between treatment and control groups at T4 (P < 0.001) and T5 (P < 0.005). Conversely, women with low baseline depressive symptoms showed no significant differences between the qigong and WLC group for any assessment point.
With regard to the endpoints of fatigue and overall QOL, significant differences were only appreciated during the later assessments (T4 or T5), and only in the groups who, as mentioned above, presented with high baseline depressive symptoms. Additionally, with regard to the endpoint of fatigue, controlling for stage at diagnosis demonstrated a significant group × time × baseline depression interaction effect (P = 0.01). There were no significant differences observed between groups for sleep disturbances or cortisol rhythm.
Table: Raw Means of Depression Scores Using the CES-D in Qigong vs Control Groups Over Time
Commentary
Qigong is pronounced “chee-gung” and translated from Chinese roughly means “cultivating energy.”1 A modern offspring of ancient healing and medical practices in Asia, qigong now exists as one of the pillars of contemporary traditional Chinese medicine.2 Though there are thousands of variations of qigong practice, this study looked at the form most commonly tested in health research — a blend of generally repetitive flowing movements and postures, a focused state of relaxed calmness, and accompanying breathing techniques.3
Stress-reduction techniques, such as meditation, progressive relaxation, guided imagery, yoga, and qigong, are emerging as modalities that may improve QOL and reduce physiological stress in cancer patients.4 Recent review articles analyzing the effects of qigong have pointed to promising results for patients struggling with depression and psychological well-being.5,6 Breast cancer patients, specifically, comprise a large population that undergoes significant psychological and physical stress — both from the cancer itself and from side effects of multimodal treatments.
It is known that complementary and alternative medical modalities are widely used by breast cancer patients to cope with symptoms of their disease.7 Although previous clinical trials have demonstrated positive effects of qigong in cancer patients receiving chemotherapy,8 the authors of this study note that theirs is the first to specifically assess its effect on women undergoing RT.
Perhaps the most striking aspect of this study was the stark — and statistically significant — difference in outcomes between women who initially presented with high (vs low) baseline depressive symptoms. As mentioned, the qigong intervention group experienced a reduction in depressive symptoms and improved perceived QOL over time. This result is likely multifactorial. First, and perhaps most evident, is the simple fact that women with worse symptoms have more potential to improve. Second, careful analysis of the data related to both of the study’s main outcomes demonstrates that both qigong and WLC groups improved over the course of the 3-month study. This suggests that time itself should also be considered as a healing mechanism, independent of other variables.
Another feature of this study that may have influenced the above outcomes relates to the purported “evenly balanced” qigong and WLC groups. The authors attest that the groups were randomized based on a technique called “minimization” to ensure that groups were similar with regard to age, staging, and type of surgery performed — factors that surely influence emotional and physical response. However, closer examination of the data on women’s demographics and clinical characteristics could lead one to conclude that the groups were not as homogenous as the authors claim. With regard to staging, there are a greater number of women with stage III breast cancer in the qigong group vs the WLC group (n = 17 vs 7). Furthermore, fewer women had stage I cancer in the qigong group vs the WLC group (n = 8 vs 14) — stage 0 describes non-invasive cancers that remain within their original location, and stage III describes invasive cancers that have not spread outside the breast to other parts of the body.9 Therefore, the women in the qigong group may have been predisposed to higher levels of depression at baseline than women in the WLC group, who principally had less invasive cancer diagnoses.
Additionally, this study’s analysis and results of cortisol levels was, surprisingly, not statistically or clinically significant, despite the authors’ hypothesis that women in the qigong group would demonstrate a steeper diurnal cortisol slope and a smaller cortisol awakening response. Measuring saliva cortisol levels was arguably the most “scientifically precise” assessment method in this study, since, unlike answers to questionnaires, these results could not be compromised by bias, disinterest, or survey-fatigue that might occur after answering 75 questions. The authors of this study assert, and most medical providers would agree, that psychological stress has a considerable impact on cancer patients. Psychological stress, along with the physical stress of surgery and RT, can contribute to hypothalamic-pituitary-adrenal axis dysregulation. Indeed, previous research studying the stress hormone, cortisol, during cancer treatment has shown that cortisol fluctuations may affect tumor progression, overall recovery, and even survival rates.10 It is unfortunate that no measurable differences in cortisol levels were demonstrated in this study, as perhaps this would be more likely to convince more “Western-minded” medical practitioners and patients that qigong is in fact a validated treatment tool.
As the authors admit, bias and patient expectation were not controlled in this study. Obviously, the individuals in the WLC group knew they were not in the treatment group, and vice versa. An argument against the benefits of any mind-body technique is that the participant must be willing to participate in the technique. With this in mind, contrarily, the women in the qigong group may have anticipated a positive affect from the treatment, therefore potentially influencing their questionnaire responses. Additionally, because this study, and the majority of research examining the effects of qigong takes place in China, its applicability to a more diverse, North American population may be limited.
Ultimately, the authors of this study admit their findings are “too preliminary” to be able to provide sound clinical recommendations. Indeed, further studies are needed to evaluate endpoints once more time has passed after individuals have completed RT and qigong treatments. Due to the widespread prevalence of breast cancer and the potential for qigong to decrease associated depressive symptoms and improve overall quality of life, it would be worthwhile to perform additional studies. Qigong is generally considered a safe practice, and should be considered among other mind-body techniques as part of an integrated treatment strategy for breast cancer patients.
References
1. Sancier, KM. J Altern Complement Med 1999;5:383-389.
2. Jahnke R. The Healing Promise of Qi: Creating Extraordinary Wellness through Qigong and Tai Chi. Chicago, IL: Contemporary Books; 2002.
3. Jahnke R. Am J Health Promot 2010;24: e1-e25.
4. Phillips KM, et al. Psychosom Med 2008;70:1044-1049.
5. Wang F, et al. Evid Based Complement Alternat Med 2013;152738. doi:10.1155/2013/152738 [Epub ahead of print].
6. Oh B, et al. Evid Based Complement Alternat Med 2013;134737 doi:10.1155/2013/134737 [Epub ahead of print].
7. Fouladbakhsh JM,Stommel M. Oncol Nurs Forum 2010;37:E7-15.
8. Oh B, et al. Integr Cancer Ther 2012;11:101-110.
9. Breastcancer.org. Stages of breast cancer. Available at: www.breastcancer.org/symptoms/diagnosis/staging. Accessed March 31, 2013
10. Sephton SE, et al. J Natl Cancer Inst 2000;92:994-1000.
Ninety-six women with breast cancer undergoing radiotherapy during a 5- to 6-week interval were randomized to either a qigong group or a wait-list control group. The results indicate that the women in the qigong group had clinically significantly less depressive symptoms and better quality of life than the control group.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
