ECG Review
What a Difference a History Makes
By Ken Grauer, MD, Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
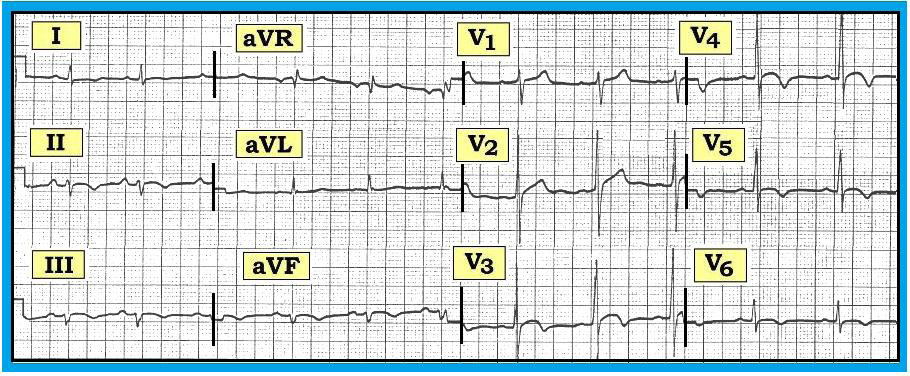
Figure - Does this ECG suggest acute ischemia and/or infarction?
Scenario: How would you interpret the ECG shown above? Does it reflect acute coronary syndrome and/or acute ST elevation myocardial infarction? What clinical information is lacking?
Interpretation: Our descriptive analysis of this tracing begins as follows: Sinus arrhythmia; normal intervals; left axis deviation consistent with left anterior hemiblock. At this point, further interpretation requires some information about the patient (namely patient age, brief medical history, and whether the patient is symptomatic).
It is easy to overlook that this 12-lead ECG was obtained at half standardization. Note that the standardization rectangle (seen at the very beginning of the tracing) is only 5 mm (= 1 large box) tall. Actual amplitude is therefore double that seen in the Figure (i.e., the S wave in lead V2 is really 24 mm in depth - not the 12 mm that we count on this tracing).
Regarding Q-R-S-T Changes: No Q waves are seen. Transition occurs early (between V1-to-V2). That said, the most remarkable finding on this tracing relates to the ST-T waves, which show ST segment coving with slight elevation and symmetric T wave inversion in many leads.
Interpretation of the above noted findings depends on the clinical setting. This ECG was in fact obtained as part of a "pre-participation physical" performed on an otherwise healthy 20-year-old football player. Past medical history was negative, and physical exam was normal (no heart murmur). In this context, the ST-T wave changes seen in this healthy and asymptomatic 20-year old almost certainly reflect a normal repolarization variant. That said, the surprisingly tall R wave already by lead V2 suggests that there may be prominent septal forces. Given generous QRS amplitude (the tracing is recorded at half standardization), an echocardiogram was recommended prior to clearing this individual for active sports participation to rule out anatomic abnormality, such as hypertrophic cardiomyopathy.
An entirely different interpretation would be in order if the ECG was instead obtained from an older adult with chest pain. In this case, the ST segment coving, slight elevation, and symmetric T wave inversion in multiple leads might clearly reflect acute ischemia/infarction.

