Pediatric Foreign Body Ingestions
Pediatric Foreign Body Ingestions
Authors:
Katherine M. Shea, MD, Stanford/Kaiser Emergency Medicine Residency Program, Stanford/Santa Clara, CA.
N. Ewen Wang, MD, Associate Professor of Surgery/Emergency Medicine, Associate Director, Pediatric Emergency Medicine, Stanford University School of Medicine, Stanford, CA.
Peer Reviewer:
Dennis A. Hernandez, MD, FAAP, FACEP, Medical Director, Pediatric Emergency Services, Florida Hospital for Children, Walt Disney Pavilion, Orlando, FL.
I started my emergency medicine practice prior to the widespread availability of pediatric-sized fiberoptic endoscopes. At that time, esophagoscopy using rigid endoscopes was a therapeutic option, but the availability of trained practitioners was limited in many communities. I remember with vivid detail wrapping the toddler in the papoose board, passing the Foley catheter through the nose, turning the child face down with the head lower than the feet, then inflating the Foley balloon and pulling it down the nose in an effort to extract the impacted object. It often took several passages, but was usually successful. But the experience was traumatic for all involved.
During that period, the impacted objects in the esophagus were coins, and we did not see button battery ingestions. If we had, then the Foley catheter extraction technique might have been dangerous. Fortunately, retrieval techniques have dramatically improved and such procedures are rarely necessary. But the increased availability of button batteries makes it important to identify and localize ingested foreign bodies. This article provides a comprehensive review of pediatric foreign body ingestions.
— J. Stephan Stapczynski, MD, Editor
This article is adapted from one that originally appeared in the November 2012 issue of Pediatric Emergency Medicine Reports.
Case Scenario
A 15-month-old presents to the emergency department for difficulty feeding and irritability. The child was noted to be unwell appearing, drooling, and sitting up and leaning forward. Vital signs were notable for tachypnea and tachycardia. The mother reported a symptom duration of about 12 hours and said the child had been well prior to that time. The radiograph of the patient is shown in Figure 1.
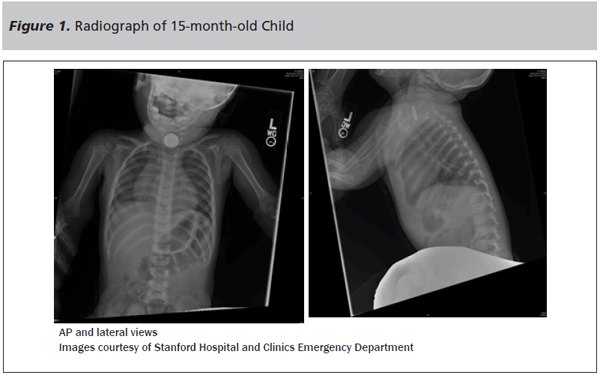
Introduction
The ingestion of foreign bodies by children is a common problem, with an estimated 86,426 cases reported to poison control centers in 2010.1 The exact incidence of the problem is unknown and is likely much greater than reported. The great majority of these cases occur in children between 6 months and 3 years of age, and the most common ingested object in the United States is a coin. Thankfully, most cases result in uneventful outcomes, with either the spontaneous passage of the object or prompt removal by a physician. However, there exists the potential for serious complications and even death if managed incorrectly. Associated morbidity is estimated at less than 1%, with an average of 1500 deaths per year.2 Complications include perforation, fistula, stricture, mediastinitis, and exsanguination. There has been a great deal of literature on this topic and varying guidelines regarding methods of removal and criteria for doing so. Despite this, management has remained relatively unchanged, with most guidelines supporting a short period of observation for benign objects in asymptomatic patients and early endoscopic removal for caustic items, prolonged impaction, or symptomatic patients.
Pathophysiology
Foreign body ingestion is largely a problem of childhood. Younger children are more likely to ingest foreign bodies as part of normal developmental “exploratory behavior,” with 80% of cases occurring in children, commonly between the ages of 6 months and 3 years.3 The great majority of these cases result in uneventful outcomes, as the object passes spontaneously and without harm through the gastrointestinal tract. In the pre-endoscopy era, 93-99% of blunt foreign bodies would pass spontaneously through the GI tract and only 1% of cases required surgery. Today, 10-20% of patients undergo endoscopy, with 1% undergoing surgical management.4 Children with developmental delays and psychiatric disorders are more likely to ingest foreign bodies, and those children with preexisting esophageal disease such as eosinophilic esophagitis or stricture are at higher risk of subsequent complications.
Children ingest a variety of objects from simple coins to more dangerous items such as magnets, button batteries, and needles. It is estimated that coins make up 31-46% of all ingestions, the most common of which is the penny.5,6 Other common objects include small toys, needles, pins, batteries, jewelry, magnets, bones, and food boluses (most commonly meat).
Button batteries are a unique subcategory of foreign body and made up 13% of all ingestions in one study.7 Early recognition of these objects is crucial in the appropriate management of affected children, as they cannot be simply observed, as is the case in many other types of ingestions. Due to unique mechanisms of injury involving pressure necrosis, hydrolysis, and liquefaction necrosis, both button batteries and magnets carry greater morbidity and mortality and should prompt consideration of immediate removal. The narrow end of a button battery, known as the “anode” or negative terminal, is the location at which tissue damage occurs. Hydroxide ions build up, resulting in a chemical burn on surrounding structures. This can be remembered as “narrow-negative-necrotic.” It is also worth noting that certain button batteries carry greater risk than others. According to Litovitz et al, while the number of button battery ingestions has remained relatively constant during the past 20 years, there has been a 6.7-fold increase in the number of major and fatal outcomes associated with these ingestions. The authors identified a correlation between major outcomes and an increase in the number of 20- to 25-mm-diameter cell batteries, as well as an increase in the number of lithium battery ingestions.8 It is suggested that lithium is a particularly harmful substance, as it has the potential to carry a much higher current than other metals and, thus, cause greater damage.
While most gastrointestinal foreign bodies pass spontaneously, at times this natural progression can be interrupted, leading to an object lodged in the gastrointestinal tract.
Common sites of obstruction include the proximal esophagus at the level of the cricopharyngeus muscle (in line with the clavicles on X-ray, also known as the thoracic inlet), the mid-esophagus at the level of the aortic arch (at the carina on X-ray), the lower esophageal sphincter (2-4 vertebral levels above the gastric bubble on X-ray), the pylorus, and the ileocecal valve. Of these, the most common location for pediatric obstructions is the criocopharyngeus, which accounted for up to 77% of esophageal foreign body obstructions in one study.9 Objects in the esophagus have been noted to have spontaneous passage rates of 28% in children without preexisting esophageal disease.10 There is a greater likelihood of spontaneous passage if the object is located in the distal esophagus. Waltzman et al found that up to 56% of objects in the lower third of the esophagus would pass spontaneously within 16 hours, compared to 23-30% for objects higher up. Spontaneous passage was also noted to be more likely in males and older children.11 (See Figure 2.)
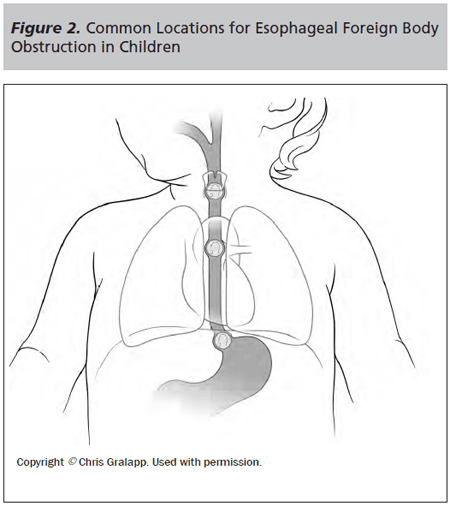
Once objects pass into the stomach, 90% will complete their course without complications. The majority of objects pass within 4 to 6 days, but some may take up to 4 weeks.4 Objects larger than 2 cm in diameter or longer than 5 cm (or a length greater than 3 cm in infants) are exceptions. They typically require GI consultation and endoscopic removal due to the higher potential for obstruction at the pylorus, duodenal sweep, or ileocecal valve.4
History and Physical
Because the potential complications of a retained foreign body can be quite severe, prompt diagnosis and appropriate management are essential. However, this is made difficult by the fact that, in a substantial number of cases, patients are asymptomatic and ingestions were unwitnessed. The physician, therefore, must always consider the possibility of a foreign body ingestion in a child with “sore throat,” dysphagia, increased secretions, and drooling, especially if the child is ill-appearing. Studies have shown anywhere from 7% to 64% of patients with esophageal foreign bodies are asymptomatic at the time of presentation.5,12 Furthermore, anywhere from 8% to 40% of foreign body ingestions are unwitnessed.4,6 And while the age range of 6 months to 5 years represents both the innate curiosity of young children and the development of a pincer grasp, foreign body ingestions can occur even in children younger than 6 months of age. In such cases, it is often an older sibling who is responsible for “administering” the foreign body. Children with development delay and pre-existing esophageal disease are at a higher risk for foreign body ingestion and subsequent complications, and a higher index of suspicion should be maintained in these patients.
For those patients who are symptomatic, the most common presenting symptoms are vomiting and regurgitation.9 Other symptoms include dysphagia, odynophagia, drooling, respiratory symptoms, pain in the throat, neck, or chest, or foreign body sensation. (See Table 1.) Patients with unwitnessed ingestions and no initial symptoms, or those who were not appropriately diagnosed and treated at the time of initial presentation, may go on to develop “chronic” foreign body, defined as an object retained for greater than 7 days. These children are more likely to have respiratory symptoms at the time of presentation due to trachea compression or esophageal erosion. A study by Miller et al looked at 41 cases of chronic foreign body and found that 76% of patients presented with respiratory symptoms, including respiratory distress, asthma-like symptoms, and cough.13 Respiratory symptoms typically stem from the compression on the trachea from a neighboring foreign body against the posterior wall of the airway (which is not protected by tracheal rings). This can often confuse the picture when it is unclear whether a child aspirated or ingested the object in question.

Differential Diagnosis
Although the differential for an ill-appearing child is broad, in the appropriate clinical setting, foreign body ingestion should always be on the differential diagnosis for any ill-appearing or septic child without an obvious source. Perhaps the greatest diagnostic error is failing to have foreign body on the differential in the septic child who presents without a clear source of infection. In a study of button battery ingestions, 27% of the major outcome cases and 54% of the fatal cases were misdiagnosed, usually because of the non-specificity of presenting symptoms and no history of a foreign body ingestion.8
Diagnostics
In any child in whom a foreign body is suspected, a diagnostic evaluation, including radiographs, should be conducted. Both PA and lateral views of the chest and neck should be obtained. Even in cases where caregivers are certain a child ingested a particular, seemingly benign object, the physician may be surprised to find either multiple objects or an object the parents never suspected the child of ingesting. In one case, parents were convinced a child had ingested a small plastic house from the game of Monopoly. The radiograph instead showed the image in Figure 3.
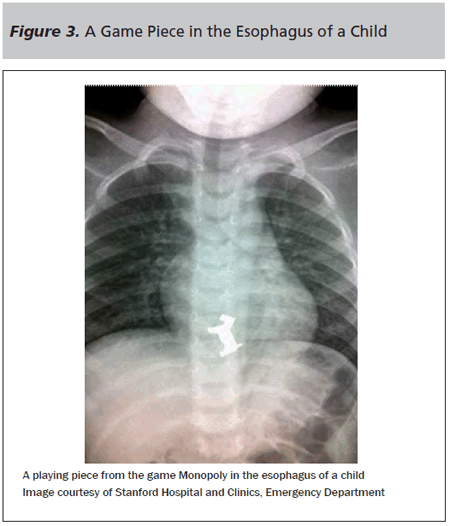
As a general rule, coins that appear “en face” on the PA view are lodged in the esophagus, and coins with the edge alone showing are lodged in the trachea. This is considered to be due to the anatomy of the trachea, wherein the cartilaginous rings are not fully circumferential, forcing the coin into a perpendicular orientation. At times, this rule is not met, and esophageal coins may appear as though they are in the trachea on a PA view.8 (See Figure 4.) This is commonly seen when a coin is at the level of the aortic arch. To avoid misdiagnosis, a lateral view should also be obtained, as an esophageal foreign body will be seen posterior to the airway in this projection.
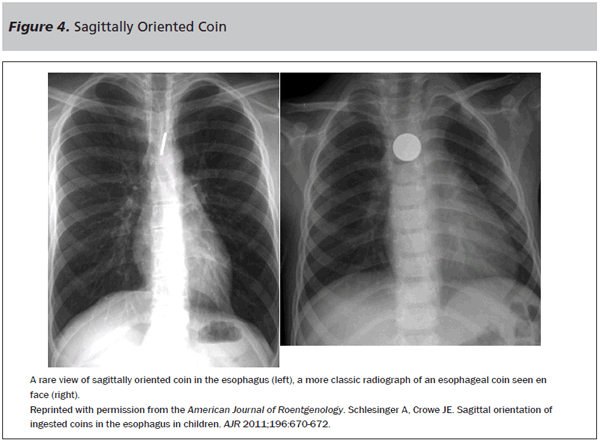
The value of X-ray in foreign body ingestions cannot be overstated. Many times, an X-ray will show a foreign body in a completely asymptomatic child. Radiographs have the advantage of localizing an object and giving some characterizations of its size and shape. Button batteries have a unique appearance on X-ray, as is highlighted. (See Figure 1.) While coins will appear as a singular rectangular opacity on the lateral view, a button battery will have a subtle step-off, with the negative terminal diameter being somewhat smaller than the positive terminal’s diameter. On the PA view, a “double ring” can sometimes be seen representing this same step-off. Plain films of the entire GI tract, from the neck to the abdomen, should be done at the time of initial presentation. Follow-up studies are often done at various intervals (depending on the object and the initial location), in addition to caregiver monitoring of the stool for passage. Of note, only 64% of foreign bodies are radiopaque and, thus, identifiable on X-ray. Therefore, if suspicion is high, further studies should be pursued.7 It is important for providers to remember that not all metals are radiopaque and common objects such as can pull-tabs and small toys may not show up on X-ray.
Hand-held metal detectors (HHMDs) have shown promise as a cost-effective, safe way of identifying and locating an ingested metallic foreign body. Unlike X-rays, they are able to identify aluminum objects, thus increasing their sensitivity.14 In one study of 172 patients, HHMDs were 100% sensitive and 92% specific for foreign body. They have the added advantage of being a tool that can be used by inexperienced operators (for example, in a triage situation). In the same study, HHMDs were 96% sensitive and 81% specific in the hands of inexperienced operators.15
Computed tomography can be used in patients with negative X-rays in whom suspicion remains high, as many items are not radiopaque. In addition, they provide more information in regard to the condition of surrounding structures in hospitals where endoscopy is not readily available.12
Endoscopy is the diagnostic and therapeutic modality of choice in patients who have ingested a dangerous object such as a button battery or sharp item, in whom both removal and local inspection of surrounding tissues is desired. In addition, in patients who have had resolution of foreign body but continue to be symptomatic, endoscopy is warranted for inspection of local structures. Two types of endoscopy are available, both flexible and rigid. Both methods are safe and effective; however, rigid endoscopy is generally considered to be better at visualizing the upper cervical esophagus.16 It does, however, have the disadvantage of requiring general anesthesia and having a greater risk of perforation. Flexible endoscopy has the advantage of visualizing as far distal as the duodenum, can be done under simple sedation, and has a lower complication rate.
In addition to imaging, laboratory evaluation including a CBC and septic work-up in an unwell-appearing child should be pursued. Pediatric ENT or GI consultation should be obtained early and, if the child presents to a hospital where urgent endoscopy is unavailable, transfer to a higher level of care should be arranged.
Management
Given that a certain percentage of gastrointestinal foreign bodies will pass spontaneously, the physician first must decide whether a foreign body warrants intervention. Endoscopic removal, while generally considered to be a safe procedure, does carry with it risks such as bleeding, infection, perforation, and complications associated with sedation or anesthesia and, therefore, should be avoided unless absolutely necessary.
Any child who is symptomatic at the time of presentation warrants consideration of urgent endoscopic removal. Indications for emergent removal are airway compromise, sepsis, and complete esophageal obstruction, which manifests as a child’s inability to manage his or her secretions. In addition, button batteries in the esophagus, long or sharp objects, and multiple magnets should all be removed urgently. Damage from a button battery can occur in as few as 2 hours, and prompt removal is paramount. For those children who are asymptomatic, more conservative treatment options are available. (See Figure 5.) In children without any pre-existing esophageal disease who are asymptomatic at the time of presentation, an observation period up to 24 hours is appropriate, with a repeat radiograph in 12-24 hours.2 Patients with reliable caregivers may be discharged home with follow-up and strict, time-specific return precautions. Caregivers should be instructed to return to the emergency department immediately if the child develops a fever, is unable to tolerate food or liquids, or becomes symptomatic in any way. They should be instructed to monitor the child’s stool for passage of the object. Furthermore, they should be told that if the coin does not pass in 24 hours from the time of ingestion, they should return to the primary care physician or emergency department for repeat radiographs.
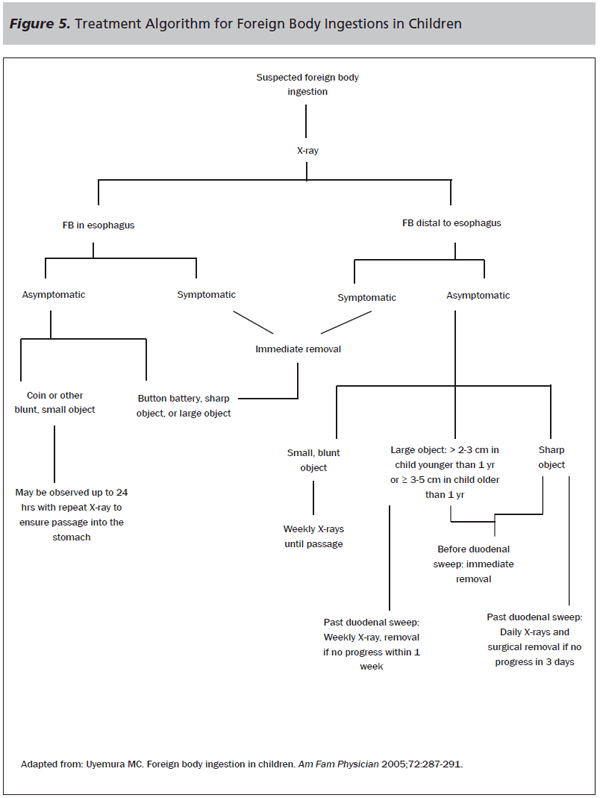
Once the object has passed into the stomach, the asymptomatic child may be safely discharged, with repeat radiographs every week. There are two exceptions to this, namely considerably large or sharp objects located before the duodenal sweep. Objects greater than 2-3 cm in diameter in children younger than 1 year and objects greater than 3-5 cm in older children should be removed immediately, as should any sharp object. If these dangerous items are located distal to the duodenal sweep, serial radiographs may be done until passage is confirmed. For large objects, serial X-rays are done every 3-4 days and objects are removed if no progress is made within one week. For sharp objects, daily X-rays are done and the object is removed if no progress is made in 3 days.4
Button batteries are managed somewhat differently due to their higher potential for morbidity and mortality. The provider should first make an attempt to determine the type and size of the battery either by determining which device the battery came from or by having caregivers bring in the original packaging or matching battery. The code printed on the battery gives an idea as to the size and composition of the battery in question. The first letter indicates the composition of the anode, or negative terminal (with “C” referring to lithium, “L” indicates alkaline, and “S” indicates silver), and the second letter indicates the shape of the battery (with “R” standing for round). The trailing numbers refer to size, with the first one or two numbers indicating the battery diameter rounded up to millimeters, and the second two numbers indicating the battery thickness or height. A CR2030 battery, for example, refers to a lithium battery that is 20 mm in diameter and 3.0 mm in height. This information helps guide management and predict prognosis.
As a general rule, a button battery in the esophagus is an emergency and should be removed immediately regardless of whether or not the child is symptomatic. An exception to this is a child older than 12 years who has ingested a battery known to be less than 12 mm in diameter. Provided these children are asymptomatic, have no pre-existing esophageal disease, and have reliable caregivers, they may be observed as outpatients. Caregivers should be instructed to inspect the stools for passage and, if no battery is seen in 10-14 days or if the child develops symptoms, a repeat X-ray should be done.8
Removal
Button Batteries. For batteries in the stomach, asymptomatic children may be observed, provided there was no magnet co-ingestion. For most situations, a repeat radiograph should be done in 10-14 days, or earlier if the child becomes symptomatic. However, in a child younger than 6 years of age who ingested a battery greater than 15 mm, a repeat X-ray should be obtained in 3 days. If the battery is still in the stomach, it should then be removed.8 If the true diameter of the battery is not known, the more conservative observation plan should be chosen. It is estimated that in 40% of battery ingestions, a definitive determination of battery diameter cannot be made.8
Options for Foreign Body Removal. Once the decision is made to remove the object in question, multiple treatment options are available. By and large, endoscopy is the mainstay of therapy and is readily available in many clinical settings. Other options include the use of Magill forceps, Foley balloon extraction, and esophageal bougienage. As mentioned previously, 1% of cases will ultimately require surgical removal.
For objects located in the proximal esophagus, some authors have described a technique involving removal of the object using Magill forceps under direct visualization. Cetinkursun et al describe placing 164 children under general anesthesia (with mask ventilation), examining the upper esophagus using direct laryngoscopy, and removing coins. They reported a 96.4% success rate using this technique, with an average time to removal of 33 seconds. No complications were reported.17 Some authors have criticized this technique, given the potential for vomiting and laryngospasm with an unprotected airway. This risk can be mitigated by first endotracheally intubating the patient. Advantages of this technique are its high reported success rates and relative simplicity without the need for advanced equipment. Disadvantages are that it is only useful for objects in the upper esophagus and the potential for complications related to an unprotected airway.
Another technique described in the literature is esophageal bougienage. This technique involves passing a semi-rigid Hurst bougie dilator into the esophagus through the mouth and pushing the object into the stomach. This technique is reserved for small, smooth objects such as coins and is contraindicated in patients with pre-existing esophageal disease. A single pass alone is attempted. Traditionally, this procedure was described as safe when performed by surgeons. However, Emslander et al conducted a prospective study in which emergency medicine physicians performed the bougienage technique and concluded it was as safe and effective in the hands of non-surgeons with no observed complications.18 The advantages of this technique are its relative simplicity and cost-effectiveness. One study compared bougienage to traditional endoscopy and found that the average treatment time and cost of bougienage were 2 hours and $1210, respectively. In comparison, endoscopy length of stay was estimated at 8 hours, with an average cost of $3100.19
Foley balloon removal has also been described in the literature. It involves placing the patient in Trendelenberg position and passing a catheter past the foreign body under fluoroscopic guidance. The balloon is then inflated and the catheter is pulled back, dragging the object out of the esophagus. The advantage of this technique is it is also cost-effective, fast, and only requires simple equipment that is readily available in most emergency departments. However, once the object is pulled out of the esophagus, the proceduralist has little control over the object and it has the potential to then move into the airway. There has been at least one reported case of complete airway obstruction leading to death resulting from this technique.2
A newer method utilizes endoscopic forceps known as “penny pincers.” Under fluoroscopic guidance, the device is advanced to the coin, grasps it, and then withdraws, maintaining control of the coin the entire time. This procedure can be performed without sedation and has been shown to be highly effective and efficient in multiple small studies, with an average treatment time of 41 seconds.2,20 The disadvantage is it requires a fairly specialized tool that may not be readily available in all clinical settings.
Finally, endoscopy is the mainstay of therapy used in 20-30% of patients. It has the distinct advantage of visualizing the surrounding structures and is, therefore, both diagnostic and therapeutic. The procedure requires general anesthesia or sedation and carries with it both the risks associated with sedation, as well as procedural risks of bleeding, bronchospasm, esophageal perforation, and mediastinal infection. It is also more expensive than the aforementioned techniques, requires greater resources, and is associated with longer lengths of stay.
Endoscopy can be done with either a rigid or a flexible device, as mentioned previously. The most feared complication of the rigid approach is esophageal perforation, which has been noted in as much as 3.2% of cases.21 Many studies have shown similar success rates of both approaches for removing foreign bodies, with many authors suggesting flexible endoscopy should be the initial management choice. Advocates of flexible endoscopy report better visualization of esophageal mucosa, greater ease at biopsying, shorter treatment times, and faster recovery.21
Some pharmacologic agents have been described in the literature. Glucagon is the most common of these agents and has traditionally been used to relax the lower esophageal sphincter, thus allowing for passage of the item into the stomach. While there has been some evidence that this may be effective in adults (who typically have food bolus obstruction at the lower esophageal sphincter), similar results have not been found in children. In a placebo-controlled trial, the patients who received glucagon were shown to have a lower rate of spontaneous passage into the stomach than those who had received placebo, perhaps due to the fact that the majority of pediatric foreign bodies become obstructed at the level of the cricopharyngeus.22
Corticosteroids, usually given intravenously, have been used, advocated, and studied to prevent permanent damage in patients with caustic esophageal injuries after alkali ingestions.23 There is no evidence that steroids reduce damage or prevent complications from button batteries lodged in the esophagus.24
In summary, there are multiple options available for the treatment of esophageal foreign bodies. The physician must consider the patient, the type of foreign body, the time of ingestion, and the resources available when deciding which technique is most appropriate. For any child who is ill-appearing or in whom esophageal damage or perforation is suspected, the only treatment options that should be considered are endoscopy or surgery.
Complications
There is significant morbidity and mortality associated with foreign bodies retained in the esophagus. Complications can result from pressure necrosis, a sharp object perforating the mucosal wall, chemical irritation, and the extremely noxious tissue hydrolysis from a battery terminal. This can result in local tissue necrosis, perforation, mediastinitis, vocal cord paralysis (from damage to the recurrent laryngeal nerve), stricture, esophago-aortic fistula, and tracheoesophageal fistula. Ultimately, these can lead to sepsis, airway compromise, exsanguination, and death. The chance of complication is, in part, dependent upon the type of object ingested, with especially sharp, large, or noxious objects such as high-powered magnets and button batteries causing greater damage.
Button battery ingestions are unique in that they can cause local tissue damage in as little as two hours and, therefore, should prompt urgent removal. The mechanism of injury is a combination three factors, the primary of which is the generation of an electrical current at the battery’s negative terminal, which hydrolyzes tissue. Liquefaction necrosis through leakage of alkaline material and local tissue pressure also contribute.1 Multiple magnet ingestions have also been shown to be particularly problematic and have the potential for adhering two loops of bowel together and causing obstruction and pressure necrosis/perforation of local tissue.
Disposition
Many children who have a foreign body removed can be discharged home on the same day, provided there are no complications and the child is without any major symptoms. The parents should be instructed to follow-up with the child’s primary care physician in two to three days to ensure that the child has not developed symptoms that may portend an evolving complication. Parents should be given strict instructions to return to the emergency department if the child develops difficulty breathing, fever, dysphagia, speech changes, inability to tolerate secretions, or hemoptysis.
Case Conclusion
Upon identification of a button battery on radiographs, the ENT took the child to the operating room, and the button battery was retrieved. An injury was noted on the posterior esophagus with aortic pulsations. A femoral line was placed and the child was started on antibiotics and steroids. A CT angiogram was done, which showed no evidence of great vessel injury. The child was discharged home one week later and recovered well.
References
- Bronstein AC, et al. 2010 Annual Report of the American Associate of Poison Control Centers’ National Poison Data System (NPDS): 28th Annual Report. Clinical Toxicology 2010;49:910-941.
- Waltzman ML. Management of esophageal coins. Curr Opin Pediatr 2006;18:571-574.
- Kay M, Wyllie R. Pediatric foreign bodies and their management. Curr Gastro Reports 2005;7:212-218.
- Uyemura MC. Foreign body ingestion in children. Am Fam Physician 2005;72:287-291.
- Binder L, Anderson WA. Pediatric gastrointestinal foreign body ingestions. Ann Emerg Med 1984;13: 112-117.
- Yalcin S, Karnak I, Ciftci AO, et al. Foreign body ingestion in children: An analysis of pediatric surgical practice. Pediatr Surg Ing 2007;23:755.
- Arana A, Hauser B, Hachimi-Idrissi S, et al. Management of ingested foreign bodies in childhood and review of the literature. Eur J Pediatr 2001;160:468.
- Litovitz T, et al. Emerging battery-ingestion hazard: Clinical implications. Pediatrics 2010;125:1168-1177.
- Al-Qudah A, Daradkeh S, AbuKhalaf M. Esophageal foreign bodies. Eur J Cardio-thoracic Surgery 1998;13;494-499.
- Soprano JV, Fleisher GR, Mandi KD. The Spontaneous passage of esophageal coins in children. Arch Pediatr Adolesc Med 1999;153(10): 1073-1076.
- Waltzman ML, Baskin M, Wypij D, et al. A randomized clinical trial of the management of esophageal coins in children. Pediatrics 2005;116: 614-619.
- Kazam JK, Coll D, Maltz C. Computed tomography scan for the diagnosis of esophageal foreign body. Am J Emerg Med 2005;23:897.
- Miller RS, Willging JP, Rutter MJ, et al. Chronic esophageal foreign bodies in pediatric patients: A retrospective review. Int J Oed Oto 2004;68; 265-272.
- Doraiswamy NV, Baig H, Hallam L. Metal detector and swallowed metal foreign bodies in children. J Accid Emerg Med 1999;16:123.
- Seikel K, Primm PA, Elizondo BJ, et al. Handheld metal detector localization of ingested metallic foreign bodies: Accurate in any hands? Arch Pediatr Adolesc Med 1999;153:853.
- Revadi G, Philip R, Gurdeep S. Removal of foreign bodies under general anesthesia. A review of rigid endoscopy for foreign bodies of the hypopharynx and oesophagus. Med J Malaysia 2010;65(2):143-145.
- Cetinkursun S, Sayan A, Demirbag S, et al. Safe removal of upper esophageal coins by using Magill forceps: Two centers experience. Clin Pediatr 2006;45:71-73.
- Emslander H. Efficacy of esophageal bougienage by emergency physicians in pediatric coin ingestion. Ann Emerg Med 1996;27(6):726-729.
- Dahshan AH, Kevin DG. Bougienage versus endoscopy for esophageal coin removal in children. J Clin Gastroenterol 2007;41:454.
- Gauderer MW, DeCou JM, Abrams RS, et al. The “penny pincher”: A new technique for fast and safe removal of esophageal coins. J Pediatr Surg 2000;35:276.
- Popel J, El-Hakim H, El-Matary W. Esophageal foreign body extraction in children: Flexible versus rigid endoscopy. Surg Endosc 2011;25:919-922.
- Mehta D, Attia M, et al. Glucagon use for esophageal coin dislodgment in children: A prospective, double-blind, placebo-controlled trial. Acad Emerg Med 2001;8(2):200-203.
- Fulton JA, Hoffman RS. Steroids in second degree caustic burns of the esophagus: A systematic pooled analysis of fifty years of human data: 1956-2006. Clin Toxicol (Phila) 2007;45:402.
- Marom T, Goldfarb A, Russo E, et al. Battery ingestion in children. Int J Pediatr Otorhinolaryngol 2010;74:849.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
