Palliative Care Principles Primary Care Physicians Should Know
August 1, 2013
Reprints
Palliative Care Principles Primary Care Physicians Should Know
Authors: Ruth M. Thomson, DO, FACOI, FAAHPM, Chief Medical Officer, Innovative Care Solutions/Hospice of Dayton, Dayton, OH
Chirag Rajni Patel, MD, Medical Director, Innovative Care Solutions, Dayton, OH
Peer Reviewer:
Robert B. Taylor, MD, Professor Emeritus, Oregon Health & Science University, Portland, OR
Palliative is derived from the Latin palliare, which means to cloak. In the world of palliative care, cloak is quite representative of the many supportive functions a palliative care team member can provide for a patient and family. This article will help define how the field of palliative medicine has evolved, but it is important to understand some of its history first.
In September 2006, the American Board of Medical Specialties (ABMS) approved the creation of a subspecialty of Hospice and Palliative Medicine (HPM). In June 2006, the Accreditation Council for Graduate Medical Education (ACGME) defined a process to have existing HPM fellowship programs be accredited by ACGME and set a standard that after 2013 only fellowship-trained clinicians would be eligible to sit for the ABMS Board examination. Today, the ACGME Graduate Medical Education Data Resource Book lists 76 ACGME-accredited HPM fellowship programs in the United States. In February 2007, the American Osteopathic Association (AOA) Bureau of Osteopathic Specialists approved a Certificate of Added Qualification (CAQ) in hospice and palliative medicine, and the AOA Boards of Family Medicine, Internal Medicine, Neurology & Psychiatry, and Physical Medicine & Rehabilitation added the CAQ in hospice and palliative medicine. Currently, the AOA lists seven approved hospice and palliative care residency programs in the United States.
Even though palliative care is considered a young specialty with only recent acknowledgements by national governing medical boards, the concepts and principles used by palliative care practitioners find their roots in hospice care. The first hospices reported date back to the 11th century, where the incurable were given dedicated treatment.1 In 1967, nurse, social worker, and physician Dame Cicely Saunders founded the world's first modern hospice, St. Christopher's Hospice, in the United Kingdom. Since its inception, hospice has grown dramatically, and its growth has accelerated in recent years to become a multibillion dollar a year industry. In 2011, an estimated 1.65 million patients received hospice care in 5300 programs throughout the United States, with 44.6%2,3 of all deaths in the United States occurring within a hospice program, accounting for a total Medicare expenditure of $14 billion. To receive hospice services, a patient must be deemed terminally ill by two physicians, with the expected outcome of death within 6 months if the natural course of medical illness is left unaltered.
As medical management of so many illnesses has improved with better therapy and fewer side effects, life expectancy has increased as a result. The AARP Public Policy Institute released a fact sheet detailing expected growth of Medicare beneficiaries. In 2007, 44 million individuals (15% of the U.S. population) were enrolled in Medicare. Enrollment numbers are expected to rise dramatically, projected up to 79 million by 2030 as the baby boomer generation ages.4 This projected Medicare population is expected to have increasing numbers of chronic conditions that are expected to continue to drive costs higher.5 As reported in a statistical brief by the Medical Expenditure Panel Survey, 1% of the U.S. population accounted for 28% of total health care expenditures, and 5% of the U.S. population drove more than half of all medical costs.6
A report released by the Dartmouth Atlas of Healthcare looking at research from a large-scale, Robert Wood Johnson Foundation-funded study asked patients with serious illness where they would prefer to die at the end of life. A majority of the respondents listed home as their preference; however, 55% actually died in the hospital and the care these individuals desired rarely aligned with the care they received.7
A recent poll of Californians showed a large gap between the care patients want and the care received at the end of life. This survey, reported in the Final Chapter: Californians' Attitudes and Experiences with Death and Dying and released in February 2012 by the California Healthcare Foundation, finds that nearly 8 out of 10 individuals would prefer to die at home if seriously ill and reports that individuals would want to talk with their doctor about end-of-life care. Of concern, fewer than 1 in 10 individuals reported that they had such a conversation, including just a little more than 1 in 10 (13%) of those 65 years or older. When specifically asked about advanced directives, 82% of these individuals corroborated the importance of the documents but in actuality, fewer than one-fourth had completed them.8
As reported by the Center to Advance Palliative Care (CAPC) 2011 public opinion report, once patients and families understood the definition of palliative care, with language that best fit its principles and mission, the majority of polled individuals endorsed that if they had serious illness they would want access to palliative care.9 Certainly patients at the end of their life's journey should receive and have access to all measures of hospice and palliative care, to assure comfort, dignity, and quality of life until death. But one could argue that suffering is not only perceived for those who fit Medicare's defined end-of-life window; in fact, suffering is something patients with serious illness and their families battle every day. Research proves that patients want access to symptom management, clarity and alignment of their goals of care, and total support not only for themselves but also for their families. This is where palliative care and its principles can be effectively used to satisfy this need.
What Is Palliative Care?
One of the greatest challenges palliative medicine practitioners face is explaining to patients, families, health care administrators, and other health care workers what they really do. This point was proven by the CAPC public opinion strategies report, which received support from the American Cancer Society and the American Cancer Society Action Network in 2011. This survey set objectives to explore its targeted audiences' awareness and understanding of palliative care and to test the language by which the term was defined. Interpretation of what palliative medicine is or does is often defined by an individual's perceived understanding of what he/she feels. This survey polled 800 registered users (300 of these members were seniors ≥65 years of age) via telephone and asked, "How knowledgeable, if at all, are you about palliative care?"9
The report illustrated that palliative care is poorly understood. Seventy-eight percent of individuals who answered the survey said they were not at all knowledgeable. A more concerning finding is that physicians commonly equate palliative care to hospice or end-of-life care. A limitation of this report is that only eight physicians were polled, but those who were questioned were very resistant to believe that palliative care is nothing more than hospice care or end-of-life care. These physicians believed strongly that patients who receive palliative care should have comfort, symptom management, and maintenance of dignity at the end of life. One individual mentioned support of family, but again, directed toward the end of the continuum of care.
The language used to define palliative care makes a meaningful difference in what is perceived by patients and families. Simply using the word serious vs advanced to define the status of an illness was shown to have less negative emotion, and the medical care that would be needed was less connected to terminal care for individuals who were polled.
Many national and global health care governing organizations have reported definitions and support for palliative care. The World Health Organization defines palliative care as "an approach that improves the quality of life of patients and their families facing the problem associated with life-threatening illness, through the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain and other problems, physical, psychosocial and spiritual."10
The National Hospice and Palliative Care Organization defines palliative care as "extending the principles of hospice care to a broader population that could benefit from receiving this type of care earlier in their illness or disease process. No specific therapy is excluded from consideration. An individual's needs must be continually assessed and treatment options should be explored and evaluated in the context of the individual's values and symptoms. Palliative care, ideally, would segue into hospice care as the illness progresses."11
The National Comprehensive Cancer Network (NCCN) has specific palliative care guidelines, and it defines this field as "both a philosophy of care and an organized, highly structured system for delivering care to persons with life-threatening or debilitating illness. Palliative care is patient- and family-centered care that focuses on effective management of pain and other distressing symptoms, while incorporating psychological and spiritual care according to patient/family needs, values, beliefs, and culture(s). The goal of palliative care is to prevent and relieve suffering and to support the best possible quality of life for patients and their families, regardless of the stage of disease or the need for other therapies. Palliative care can be delivered concurrently with life-prolonging care or as the main focus of care."12
The American Academy of Family Physicians has the following definition: "Palliative care serves patients of all ages who have a chronic illness, condition, or injury that adversely affects daily functioning or reduces life expectancy. This care is given by an interdisciplinary team that encompasses several fields and may include volunteer coordinators, bereavement coordinators, chaplains, psychologists, pharmacists, nursing assistants, home attendants, dietitians, therapists (e.g., physical, occupational, art, play, child life, music), case managers, and trained volunteers. In addition to the physical aspects of illness, palliative care addresses psychological, spiritual, and practical matters. The unit of care comprises the patient and his or her family as defined by the patient or a surrogate; family members are not necessarily related to the patient but have a significant relationship and provide support."13
The CAPC updated the language in its definition after public opinion research showed a significant positive impact of this definition. "Palliative care is the specialized medical care for people with serious illness. This type of care is focused on providing patients with relief from the symptoms of pain and stress of a serious illness whatever the diagnosis. The goal is to improve the quality of life of both the patient and family. Palliative care is provided by a team of doctors, nurses, and other specialists who work with a patient's other doctors to provide an extra layer of support. Palliative care is appropriate at any age and at any stage in a serious illness, and can be provided together with curative treatment."9
In gist, palliative care can be accessed at any stage of serious illness, using a multidisciplinary team of health care professionals looking at aspects of a patient's care including input from family at every level. The team works collaboratively with the primary medical team to maximize symptom control, improve quality of life, and support patients and families.
Where Can I Find Palliative Care?
The nation's hospitals are still the most prevalent site for palliative medicine delivery. Since 2000, the number of palliative care programs within hospital systems has grown by 148.5%, and as of 2011, 65.7% of U.S. hospitals reported having palliative care programs.14,15 Since hospitals are the site for the most acutely ill patients, a frequent site of death, and a place where fragmented communication to patients and families is common, it is not surprising that hospital palliative care programs have grown so rapidly.
Data for outpatient penetration for palliative care is not as evident. The National Cancer Institute (NCI) looked at the percentage of palliative care programs in NCI-accredited cancer hospitals and found that although there was almost uniform access (92%) in the inpatient setting to palliative care, greater variability existed for outpatient services. Fifty-nine percent of NCI cancer centers reported outpatient palliative care, compared to 22% of non-NCI cancer centers endorsing availability of outpatient palliative care. Another key finding was that the services offered by these outpatient palliative care programs also had quite a bit of variability.16-18 The American Society of Clinical Oncology also has established a position statement regarding outpatient palliative care services. It recommends increased integration of palliative care with goals to achieve high-quality comprehensive cancer care by 2020.20
Gaps in the Continuum of Care
One of the most evident flaws with the current delivery of palliative medicine is that it often occurs at end-of-life care and, in fact, commonly for hospice-eligible patients. With Medicare's new focus on the patient experience, looking at pain and other symptom scores linking reimbursement to outcomes as a part of the Affordable Care Act,20,21 hospitals remain a necessary site for palliative care delivery. It has been argued and proven that earlier palliative care intervention improves quality of life, and palliative care even improved length of life for patients with metastatic non-small cell lung cancer.
Figure 1 illustrates the idea of accessing palliative care and its principles earlier in the disease trajectory. It can be imagined that the amount of support palliative care will offer this patient and his/her family will ebb and flow as needs dictate, with the goal to maximize quality of life and to reduce suffering while being offered concurrently with curative, restorative, aggressive medical/surgical care.
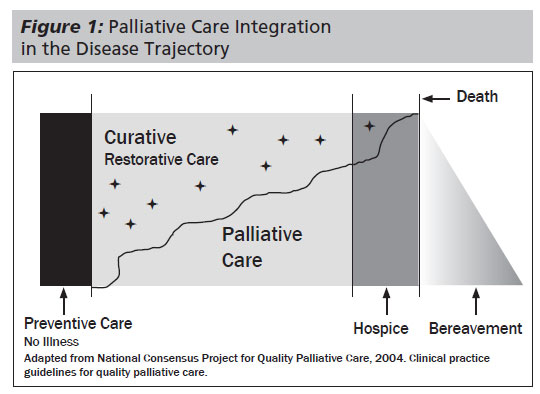
The benefit of providing integrated palliative care across the entire continuum of care specifically for high-risk, late-stage, chronically ill patients is seen clearly by the Advanced Illness Management (AIM®) program offered by Sutter Health in northern California. This systems-based model of palliative care delivery has shown an increased use of hospice care after properly aligning patient/family goals using advance directives and medical/physician orders for life-sustaining treatment documents (MOLST/POLST). Data also showed less ambulatory care and inpatient usage by patients enrolled in the AIM® program. For patients who survived more than 90 days after enrollment, data showed a 54% decline in hospitalization compared to the 90-day interval period prior to AIM® enrollment. ICU days and length of stay on subsequent hospitalizations both were reduced. Visits to physician's offices also declined, with a small uptick in physician telephone calls.23 These accomplishments were achieved with improved patient, family, and physician satisfaction when measured.24
Workforce Shortage
Despite palliative care's rapid growth since 2000, there is an expected shortage of trained palliative medicine physicians. As health care reform continues to evolve, demand for integrated palliative care models across the continuum of care will continue to place pressure on existing palliative care providers. To put things into perspective, data reported by CAPC's national report card found that for every 71 patients facing a heart attack, there is one cardiologist available to treat them. There is one oncologist for every 141 newly diagnosed cancer patients. Frighteningly, for every 1200 patients facing life-threatening, serious illness, there is only one certified palliative medicine physician available to serve their needs.26 As the baby boomers age and start to bear more symptoms of their comorbid conditions, this service gap will continue to widen, placing even more strain on those individuals trained in the principles of palliative medicine.
New palliative care physicians entering the workforce, albeit increasing in numbers, are not expected to meet the demand for palliative care services. Data from 2011 show that only 86 new palliative medicine physicians will be trained per year through accredited fellowship programs in HPM.25 Another limiting factor reported by the CAPC national report card is that current Medicare-funded graduate medical education slots are capped, reflecting the effect of the 1997 Balanced Budget Act. Many academic centers large enough to provide the variability and caseload numbers to provide adequate exposure to palliative care patients to produce competent physicians are at or above their GME resident cap. Medicare dollars, which are used to train most other physicians in this country, are not available to train future palliative medicine physicians. Also, as the grandfather period to be able to sit for the ABMS and AOA CAQ certification test has already closed or is fast closing, patient access to Board-certified physicians in palliative medicine will remain at a premium for the foreseeable future.
Primary Palliative Care
"When does primary care turn into palliative care?" This question is the title of a recent paper14 that corroborates the importance of the primary care physician's role in today's fragmented health care delivery system. A perception illuminated in this discussion was that many primary care physicians are not on the front lines when it comes to end-of-life care. Often, a letter of condolence or a death summary is sent from the end-of-life responsible care party confirming the death of a patient. As the prevalence of the site of death has moved from home to institutions, it is easy to see why primary care physicians feel less engaged in participating in end-of-life discussion with patients and their families.
Primary care physicians hold extreme value in helping patients and families transition during critical phases in their clinical life.26 No one is better suited to discuss patient goals, desires, and quality-of-life outcomes than the physician who best knows and has the trust of that patient and his/her family. Numerous studies have shown that patients with chronic illness want to talk about their choices, align goals of care, and have frank discussions about prognosis earlier in the disease trajectory. The groundbreaking SUPPORT study showed that patient end-of-life wishes and goals were not satisfied.21 A lack of discussion of do not resuscitate (DNR) preferences was shown in this study, with 46% of DNR orders in the hospital written within 2 days of a patient's death. From a symptom standpoint, this study also showed that 50% of dying patients experienced severe pain.21 A study of cancer patients found there are consequences if discussions are not held, especially when communication with physicians was lacking, which in this case led in part to these patients having unrealistic expectations of their prognosis and being more likely to die in intensive care, supported by life-sustaining therapy after cardiopulmonary resuscitation.27
Primary care physicians can use some palliative care principles, such as improving symptom assessment and management; using patient and family goals vs problem-focused care as the directive; learning improved understanding of prognosis; delivering this message with compassion and empathy; and recognizing that spiritual, psychosocial, and cultural elements play a relevant role in creating suffering in patients with serious illness. It is important for primary care physicians to remain active in this process for families during their clinical journey.
An approach that can be used to introduce families to the idea of palliative care is to draw an analog to an insurance policy. Palliative care helps families plan for worst-case clinical scenarios. This can be further defined as supporting them by providing clarity on what this scenario would look like, tying elements of their loved one's life story to help define goals of care, and then appropriately utilizing clinical tools to support the desired outcome. In the end, it is best to try to limit the surprises families face during end-of-life care. When a palliative care team delivers bad news and attempts to transition families to end-of-life care, common emotions are shock and surprise. The emotion that seems to haunt these families the most is regret, which often can be seen clearly in their faces, many times mixed with anger and disbelief. In the end, from a family's perspective, the missed opportunity to cherish each day that was given, treat it as a blessing, reminisce on their life's story, and find gratitude remembering elements that made them a family hurts the most.
Guiding and supporting patients and their families with life-defining decisions is rewarding and is the impetus to incorporate palliative care principles into primary medical care delivery.
Benefits of Implementing Palliative Care Principles
The benefits of using palliative care principles in primary care practices are clear (See Table 1). Implementing a structured approach to define what factors make up the characteristics of a patient and his/her family in the context of understanding specific domains of concern to individuals facing serious and possibly life-limiting illness can help assure focus remains on what is relevant to that patient and his or her family.

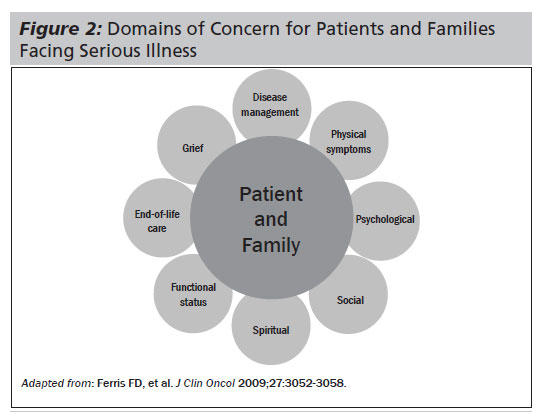
Physicians can use established patient and family characteristics including understanding demographics, culture, personal views, beliefs, and values to identify eight key domains (see Figure 2) that can cause suffering for patients and their families with serious illness.28 Using knowledge obtained from a patient's life story, a provider who understands the interplay that occurs between these domains that cause suffering and interprets the patient's value and support system will be better suited to deliver care tailored specifically to their patients.
Defining the Population
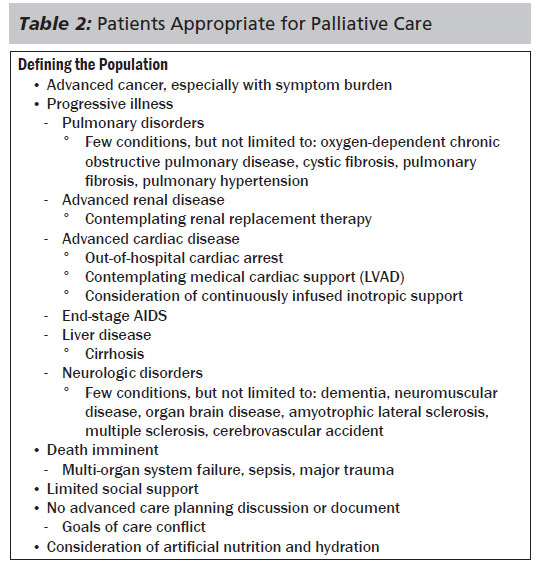
Palliative care can be delivered to any patient of any age with a serious, potentially life-limiting or life-threatening illness. Disease can be in any organ system. Table 2 lists examples of conditions that could lead to palliative care intervention. Any patient with serious illness for whom recovery back to baseline function is routine and expected would not be included in this defined population.
Certain characteristics of patients with serious illness can help define their eligibility for palliative care. Research shows that individuals with multiple hospitalizations, especially with less interval time between, are at risk of decline and possibly may need palliative care.29 Other functional or clinical changes such as weight loss, decrease in functional status, more dependence on others for activity of daily living support, and refractory symptoms despite medical intervention can further reinforce to the clinical team that there could be unmet palliative care needs for this patient and/or his/her family. Another clarifying question to ask with every palliative care encounter is, "Would you be surprised if this patient died within 12 months?" This "surprise" question has proven to be remarkably valid in predicting poor outcomes.30-32
Using symptom assessment scales also can identify symptom risk, incorporating not just physical, but psychological and spiritual distress as well. NCCN has established guidelines for distress management using a thermometer linked to practical problems as well as physical problems.33 The National Palliative Care Research Center has multiple screening tools available for use, including pain and symptom management, functional status, psychosocial care, caregiver assessment, and quality-of-life measuring tools.34
Models of Palliative Care Delivery
The Institute of Medicine defines primary care as "the provision of integrated, accessible health services by clinicians who are accountable for addressing a large majority of personal health care needs, developing a sustained partnership with patients, and practicing in the context of family and community."35 It is important to recognize that there is significant overlap in the skill sets of primary care providers and palliative medicine providers. Some commonalities include using excellent communication skills; involving the patient-family unit; establishing goals of care; practicing care integration; and addressing psychosocial, spiritual, and cultural concerns.35,36
As health care continues to become more complex and fragmented, a reasonable option would be to defer implementing palliative care to specialists. A report published in the Journal of the American Medical Association showed that during a 10-year period, the probability of a referral to another physician from a primary care physician increased by 94%.37 Patients, however, preferred to see their primary care physician despite perceptions that specialists were more competent in care for that specific medical condition.38
As previously stated, given that the number of Medicare beneficiaries is expected to significantly increase and that many will be living with multiple chronic conditions, primary care clinicians will be paramount to meet their care needs. With the described workforce shortages for palliative care personnel and increasing growth of at-risk populations, understanding and implementing basic palliative care principles by primary care physicians makes theoretical sense.39 It is important, however, for primary care clinicians to be aware of their limitations, be aware of community resources, recognize when they can meet the palliative care needs of their patients, and recognize when they should consider referral to a palliative medicine specialist.35
A recent article in the New England Journal of Medicine discussed the importance of primary palliative care, citing the specialist palliative care workforce shortage, the need to maintain and protect the primary team relationship with the patient and family, and ongoing recognition that the provision of basic symptom management and psychosocial support is a primary care responsibility as reasons why it is so important.39 The authors stress that core palliative care duties, such as basic pain and symptom management and aligning the plan of care with the patient's goals, should be standard care provided by all clinicians. They further explain this concept by delineating primary palliative care skills vs skills that should be referred to palliative care specialists (See Table 3).39
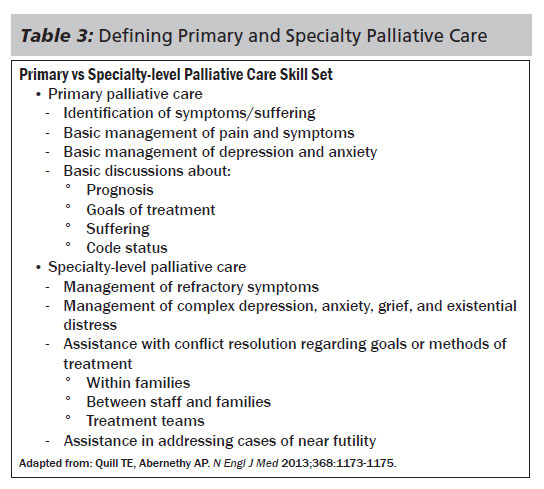
Education is key, and although educational resources have been available since the 1990s, including Education in Palliative and End-of-Life Care (EPEC) and End-of-Life Nursing Education Consortium (ELNEC), more focused efforts to expand palliative care are needed.39 Individual specialties and institutions should develop expectations with prescribed outcomes for basic palliative care skills and screening tools to guide specialty palliative care consultations.39
Weissman and Meier take palliative care skill set delineation one step farther by identifying three levels of palliative care: primary palliative care, secondary palliative care, and tertiary palliative care. They define primary palliative care as "the basic skills and competencies required of all physicians and other health care professionals." Secondary palliative care is provided by specialists in the form of consultation or specialty care. Tertiary care centers offer the provision of tertiary palliative care, utilizing specialists to address the most complicated cases. These centers also focus on research and teaching in palliative care.29 They also discuss a menu of primary palliative care services including pain and symptom management, psychosocial and spiritual assessment, prognosis and treatment options, goal setting and advance directives, and transition care.29 Primary care physicians who have access to palliative medicine experts in community specialty programs or tertiary academic centers can rely on these experts as valuable resources to assist with complicated symptom management and palliative care needs. Specialized palliative medicine services should complement the palliative care provided by primary care clinicians.
Current leaders in palliative medicine39 also are petitioning for increased research to find a sustainable delivery model for primary palliative care, blending in ready access to specialty-level support when primary interventions fail. Requests are being made for leaders in various outpatient specialty groups to define primary palliative care skills from their perspective. Once these skills are defined, basic training programs need to be constructed and delivered to all members, including mid-career practitioners. These programs should be linked to performance measures with expected target goals for completion, including remediation plans. For example, the Agency for Healthcare Research and Quality funded a grant to the American Society of Clinical Oncology in partnership with the American Academy of Hospice and Palliative Medicine (AAHPM) for Oncotalk, a program developed to improve training for oncology fellows in basic primary palliative care principles. Part of the curriculum includes improving the awareness among future oncologists to recognize complex symptoms, to attempt to manage the symptoms, and to consider palliative care support if symptoms cannot be controlled.40 Continued efforts to increase access for education in palliative care are being explored41 .
One example of a blended primary/palliative care delivery model is at the Fairview Health System in Minneapolis.42 This outpatient program was a natural progression from the inpatient program. As seen by many inpatient palliative care providers, not all patients they see die or reach hospice care, so some form of outpatient follow-up is required. This was the driving force behind creation of this program's ambulatory presence. This blended delivery is unique because the palliative care group has partnered with two primary care clinics to educate their physicians on outpatient palliative care and their role to identify complex cases. They developed a script for the primary care physicians to use to help introduce palliative care and to discuss their role in their patients' care.
Primary Palliative Care Components
Symptom management. Symptom management encompasses addressing pain and other distressing physical and/or psychosocial symptoms or medical problems patients experience as a result of their advanced illness. In a 2004 study, Paice et al performed a retrospective chart review of all adult patients who died in the hospital setting over a 6-month period in the ICU, oncology, and medical unit settings. Of 213 patients who met inclusion criteria, 195 were included in the final analysis. They noted that most of the patients in this population experienced one or more distressing symptoms: pulmonary congestion (92%), confusion (86%), fever (78%), dyspnea (78%), pain (77%), fatigue (42%), sedation (36%), constipation (32%), agitation (32%), and decubitus ulcers (26%).43 This symptom analysis provides a fairly complete list of the typical distressing symptoms patients experience in their last few days to weeks of life. Other common symptoms warranting palliation include nausea, vomiting, anxiety, depression, and anorexia.
In 2009, the NCCN released Palliative Care Clinical Practice Guidelines in Oncology, which addresses pain, dyspnea, anorexia/cachexia, nausea/vomiting, constipation, malignant bowel obstruction, delirium, as well as advance care planning and post-death support.44 Although the guidelines are intended for oncology patients, they are applicable to patients with noncancer advanced illness. The guidelines also embrace the spirit of palliative care by addressing symptoms and needs early in the disease course rather than only focusing on end-of-life. This is accomplished by categorizing palliative interventions based on projected prognosis into years, years to months, months to weeks, and weeks to days.44
Pain. It is important to recognize that most patients with any serious illness will experience at least some degree of pain during the course of their disease. Pain may be directly related to the advanced illness itself, the dying process at end-of-life, or unrelated, in the form of chronic pain as a comorbid condition. Regardless of cause, relief of suffering from pain for patients with advanced illness is globally considered a patient right. The Joint Commission released pain management standards in 2001 that resulted in the designation of assessing pain as "the fifth vital sign." The standards require that assessment and treatment of pain is a patient's right, pain should be assessed at every initial encounter and reassessed periodically as clinically appropriate, and pain management education should be available for all patients suffering from pain and their families.45 Despite the Joint Commission standards and incorporation of pain as the fifth vital sign, improvement of pain management has been questioned. The results of a small VA comparison study by Mularski et al showed no difference in management of pain before and after implementation of eliciting and documenting pain as the fifth vital sign.46 All clinicians are responsible for continuing to strive to make an impact on relief of suffering from pain related to advanced illness. Assessment and routine reassessment of pain control is critical to achieving good outcomes in pain management.
The basis of modern pain management is built on the World Health Organization stepladder, first described in 1986. The pain ladder recommends a systematic approach of matching the strength of analgesics to the level of pain, titrating analgesics in a stepwise manner in response to uncontrolled pain, administering analgesics around-the-clock rather than as needed, and utilizing adjuvant medications to aid in pain relief.47
Typical nonopioid analgesics include acetaminophen, ibuprofen, and other nonsteroidal anti-inflammatory drugs (NSAIDs). These are most effective for mild pain, particularly nonmalignant pain. Acetaminophen is a good initial choice for pain relief in the elderly who are struggling with advanced noncancer illness, since their source of pain is often musculoskeletal related to osteoarthritis and may be compounded by decreased mobility. For ongoing pain, acetaminophen is most effective if it is administered on a routine schedule, being mindful not to exceed 3 g in 24 hours for geriatric patients and exercising caution in patients with hepatic or kidney disease. NSAIDs can be helpful for mild malignant or nonmalignant bone pain. In the palliative care patient population, NSAIDs are most commonly used as adjuvants to opioids for bone pain relief. Caution should be used when prescribing NSAIDs to geriatric patients and patients with renal, hepatic, hematologic, and cardiovascular disease, and a history of GI bleeding. Consideration should be given to prescribe GI prophylaxis for prolonged NSAID administration or concomitant steroid use.
Opioid/nonopioid combination medications are very commonly prescribed in all areas of pain management. In the palliative care setting, they are most effective for mild-to-moderate pain. If utilized as the sole medication for ongoing pain, they are most effective if prescribed on a routine schedule. If they are prescribed as short-acting therapy for breakthrough pain in addition to a long-acting opioid, as-needed dosing is appropriate. Clinicians must remember to exercise the same caution with these combination medications as with acetaminophen and ibuprofen alone.
Pure opioids are most appropriate for moderate-to-severe pain. Available formulations include immediate-release, "short-acting" and sustained-release, "long-acting" forms. As mentioned above, immediate-release opioids are most effective for treating pain with an ongoing source if prescribed on a routine schedule. As-needed dosing is appropriate if prescribed for breakthrough pain in addition to a long-acting opioid. Commonly prescribed immediate-release opioids include oxycodone, morphine, and hydromorphone. Sustained-release opioid choices include oxycodone CR, morphine ER, and fentanyl patch. Unfortunately, when managing ongoing pain in the palliative care patient population with long-acting opioids, most patients will still experience breakthrough pain at least some of the time; therefore, clinicians should always prescribe a short-acting opioid as needed for rescue dosing.
Possessing unique pharmacokinetics, methadone exhibits both short-acting and long-acting properties. In addition to binding to the μ-opioid receptor, methadone also blocks the NMDA receptor, resulting in effectiveness in managing somatic or visceral pain and neuropathic pain. Because of its long and highly variable half life and multiple drug-drug interactions, methadone is best reserved to be prescribed by clinicians with a good working knowledge of the potential implications of its pharmacokinetics and experience with the drug. Specialists trained in pain management or hospice and palliative medicine can serve as a resource to primary care clinicians without experience prescribing methadone.
For patients with renal failure, it is best to avoid morphine because of the potential for its active metabolite, morphine 6-glucuronide, to accumulate, resulting in undesirable side effects including sedation and respiratory depression.48
There are a multitude of published equianalgesic dosing tables for opioids. Shaheen et al published a literature review study in 2009 comparing and contrasting available equianalgesic dosing tables from various sources including pharmaceutical companies, the Physician's Drug Reference, and online resources. They defined equianalgesic dosing as "the dose at which two opioids at steady state produce approximately the same pain relief." They found significant variability in conversion ratios as it pertained to route changes (i.e., oral to parenteral) and opioid rotation. They explained that equianalgesic tables are formulated primarily from single-dose studies in noncancer patients and often do not account for variables such as age and organ dysfunction. They recommended using available equianalgesic tables to estimate doses, but noted that clinical experience and judgment must be applied to each individual situation.49 Clinicians should choose an equianalgesic table with which they are comfortable and use it consistently to estimate dosing when opioid rotation is needed.
Clinicians must be familiar with and proactively address common side effects of opioids. Constipation is one of the most common side effects of chronic opioid administration. Opioids exert this effect in the gut by binding to μ-opioid receptors in the enteric nervous system, resulting inhibition of both excitatory and inhibitory neurotransmitters and leading to peristalsis interruption and decreased mucosal secretion.50 It is a routine recommendation to prescribe a bowel regimen for all patients newly initiated on routine dosing of an opioid. Nausea and vomiting is another common GI side effect thought to be caused by same mechanism of action as constipation. Proactive treatment of opioid-induced nausea and vomiting by concomitant administration of an antiemetic can be effective to allay this distressing symptom. Most patients will develop tolerance to the side effect of nausea and vomiting after a few days of opioid administration, but tolerance to the side effect of constipation rarely develops and thus must be continually addressed.
Many clinicians have an ever-present concern for opioid-induced respiratory depression. Opioid respiratory depression is defined as a decrease in effective ventilation following opioid administration. Multiple factors weigh into the potential for opioid-induced respiratory depression including dose, formulation, duration of therapy, and other medications being taken. It is important to recognize that sedation precedes respiratory depression and can be used as predictor of the potential for respiratory depression. However, clinicians must guard against overreacting to sedation, since sedation is a commonly expected side effect of opioids, especially with the first 24-48 hours of initial therapy or dose titration. Individual factors for increased risk of respiratory depression include advanced age, obesity, sleep apnea, and end organ dysfunction.51 If concerns arise about significant sedation, dose reduction should be considered if appropriate to the clinical situation, as well as assessment of concomitantly administered medications, such as benzodiazepines, that may also contribute to sedation. If sedation progresses to hypoventilation and impending respiratory depression, consideration should be given to administration of naloxone. Judicious dosing is imperative for patients on chronic opioids to avoid the dramatic distressing effects of acute opioid withdrawal. Recommended dosing of naloxone can be easily remembered by repeating a rhyme coined by one of our colleagues, "1 in 9, 1 at a time" diluting 1 ampule of naloxone in 9 mL of saline and administer 1 mL via the parenteral route every 1-2 minutes until the respiratory rate increases and the level of sedation lightens. The goal is not full alertness. Naloxone administration may need to be repeated or continuous infusion may be necessary to reverse significant sedation secondary to long-acting opioids, especially transdermal fentanyl and methadone.
At end-of-life, clinicians should weigh pain relief and sedation in an attempt to find the best balance based on the level of comfort and the patient's wishes. In this patient population, clinicians should avoid the urge to dose reduce or administer naloxone simply based on sedation, respiratory rate, or hypotension.45 The principle of double effect is commonly applied at end of life, explaining that comfort medications at doses necessary to control pain and ease suffering at end of life may potentially hasten death; this care is morally justified as long as the intent is not meant to cause harm or hasten death.
Nausea and vomiting. Nausea and vomiting is another common distressing symptom patients with serious illness may experience over the course of their disease trajectory. A variety of mechanisms contribute to nausea and vomiting in advanced illness including treatment-related (i.e., chemotherapy and radiation), GI dysmotility, bowel and gastric outlet obstruction, CNS disease, metabolic, and psychogenic. Treatment aimed at relieving nausea and vomiting should be guided by the underlying cause. Figure 3 maps out the common causes, neural pathways, and receptors involved, which help guide antiemetic therapy.52
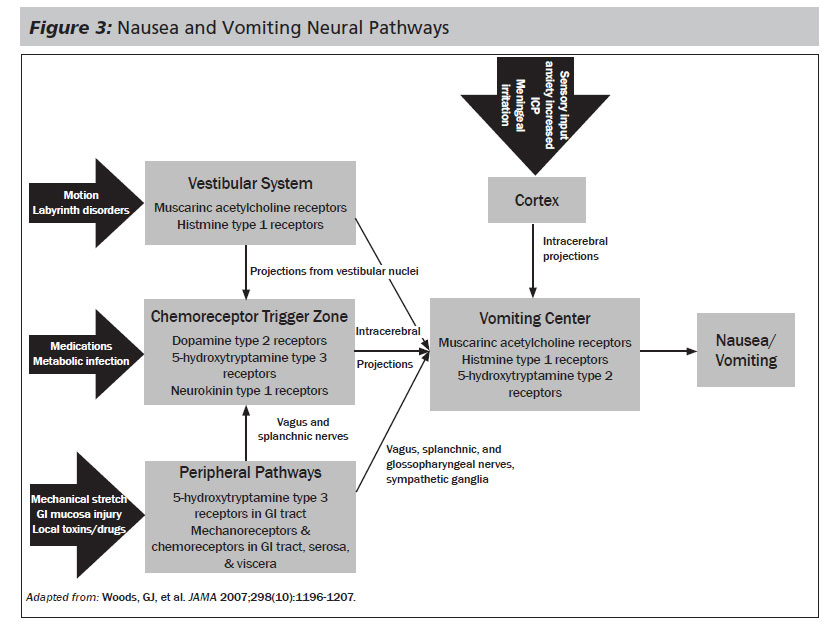
Standard antiemetic therapy includes the dopamine antagonists promethazine and prochloperazine. Many clinicians are not aware that haloperidol is also a dopamine antagonist and, thus, when used off-label is an effective antiemetic. In fact, haloperidol is a very potent dopamine type-2 receptor antagonist and exhibits an antiemetic effect, even at low doses of 0.5-1.0 mg. Sedation can be a side effect at higher doses. Extra-pyramidal side effects typically are not seen unless prescribed in high doses over a prolonged time frame. Metoclopramide is also a dopamine receptor antagonist and exerts its effect by increasing peristalsis. Caution must be exercised in patients with complete bowel obstruction because the increased peristalsis effect may result in the negative result of increased colicky abdominal pain and can increase the risk of catastrophic intestinal perforation. Metoclopramide can be used in partial bowel obstruction, but can have the potential negative side effect of increasing colicky abdominal pain.
The 5-hydroxytryptamine receptor antagonists, such as ondansetron and granisetron, have gained popularity in mainstream management of nausea and vomiting, likely related to their favorable side effect profile. However, they are only FDA-labeled to treat postoperative and chemotherapy- or radiation-induced nausea and vomiting. Also, even though generics are available globally, cost is still an issue and should be considered in palliative use.
Corticosteroids, particularly dexamethasone, remain the crux of treatment for nausea and vomiting secondary to increased intracranial pressure or meningeal irritation from CNS disease. Liberal dosing is usually required to achieve an antinausea effect, generally 4-8 mg, 3-4 times per day. Dexamethasone also may be effective for nausea and vomiting related to malignant bowel or gastric outlet obstruction by decreasing inflammation and peritumoral edema.
An additional antiemetic consideration is the use of benzodiazepines, particularly lorazepam, for pre-
chemotherapy anticipatory nausea and vomiting as well as for patients with a significant psychogenic component to their symptoms.
Clinicians should always seek to define the etiology of nausea and vomiting and address contributing or concomitant medical conditions. Treating dehydration by administration of parenteral hydration solutions may act in conjunction with medication therapy to improve nausea and vomiting. Identifying and treating underlying metabolic disturbances, such as hypercalcemia, may have a significant positive impact on symptom control. Adequately assessing for and treating constipation also can positively impact symptom control.
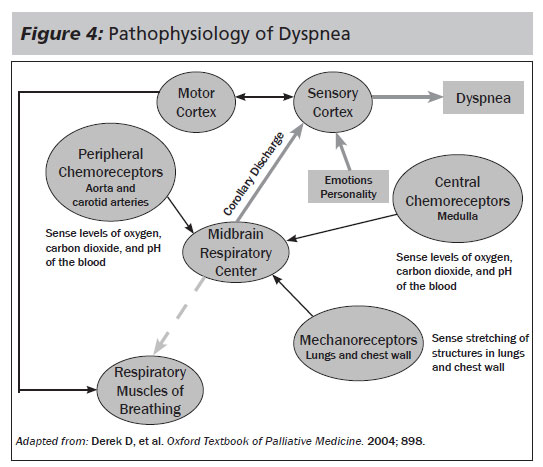
Dyspnea. One of the most difficult to manage symptoms in serious illness is dyspnea, which is defined by the American Thoracic Society as "a subjective experience of breathing discomfort that consists of qualitatively distinct sensations that vary in intensity. The experience derives from interactions among multiple physiological, social, and environmental factors." Dyspnea remains a widespread symptom experienced by patients with serious illness. A study reported that in cancer patients, 21-78% of patients experienced dyspnea days or weeks before death, with increased prevalence in the last 6 weeks of life.53 This symptom is not limited to cancer patients, with multiple studies proving that individuals with advanced chronic obstructive pulmonary disease,54 cardiac55 or neurologic disorders,56,57 or HIV/AIDs58 also face debilitating dyspnea at the end-of-life. Figure 4 shows the pathophysiology of how the sensation of dyspnea is generated.
As shown, dyspnea has a biochemical etiology, but a key regulatory component on how debilitating it can become is moderated by a person's sensory cortex. Using traditional dyspnea medical management may not be effective if a person's emotional state is altering his/her coping ability. This is where gentle sedatives, counseling, distraction therapy, spiritual or psychosocial support, or other input from multidisciplinary team members can be effective in moderating the effect of this disabling symptom in patients.
 `
`
The key strategy in managing this symptom is that it is always acceptable and desirable to use standard therapy to treat or reverse the underlying cause if possible. However, if an individual has failed dyspnea management while maximizing traditional therapy, consideration of opioid use is reasonable. Opioids have been used to treat dyspnea for centuries; however, their exact mechanism of action is unclear. One thought is that opioids decrease the perception of dyspnea centrally, at the sensory cortex. Other data show increased pulmonary artery dilation facilitating blood flow to the lungs post opioid administration.59-61 With the respiratory sedation risk, many clinicians feel when initiating opioids in a patient with compromised respiratory status, one can be easily convinced that opioids are not being used with any regularity for patients with dyspnea with serious, life-limiting illness unless they are enrolled in hospice care. The risk for respiratory depression and failure is nominal when opioids are used at the lowest therapeutic dose for dyspnea control. If opioids are used to manage dyspnea, dosing must be tailored to the individual patient's clinical situation, taking into account their comorbidities, contraindications, and history of opioid use.
Maximizing non-pharmacologic measures remains valuable. Providing adequate air circulation around patients with dyspnea, with a fan for example, has proven benefit in reducing anxiety and the patient's sense of breathlessness.63 Intensity of a patient's dyspnea is magnified by life experiences, surrounding environment, culture, and psychological and spiritual distress.52 Understanding why a patient is short of breath and being aware of his/her life story and family/support structure can be instrumental in finding the most efficient way to help find relief.
Life Planning. The SUPPORT study demonstrated that end-of-life preferences often are not honored.21 A 2011 prospective study by Nicholas et al examined regional variations in the relationship between advance directives, Medicare expenditures at end of life, and treatments received for Medicare beneficiaries between 1998 and 2007. The premise was that many patients do not want aggressive interventions at end of life; however, often these wishes go undocumented and thus do not impact the end-of-life plan of care. Data showed that Medicare beneficiaries receiving care in regions of the country with high end-of-life care expenditures spent fewer heath care dollars, died less often in the hospital setting, and exercised the Medicare hospice benefit more often if they had documented advance directives in place indicating the wish to avoid aggressive care at end-of-life.64
Eliciting patient input and honoring patients' wishes are principles most clinicians strive to accomplish in the day-to-day care they provide. Primary care clinicians are particularly tuned in to these principles as part of the relationship they have with their patients in the spirit of patient-centered care and the medical home model. Often, clinicians fear that eliciting patient input and wishes may drive health care spending upward; however, as demonstrated in the study referenced above, the contrary may actually be true. Clinicians also may worry that conversations about patient preferences at end of life may be perceived as negative by patients and their families; however, again, the contrary actually may be true. A 2012 study in Chest examined the perceptions of patients with COPD following discussions about end-of-life care. Although the number of patients (14.6%) who reported having had discussions with their physicians about end-of-life wishes was small, those who had discussions were significantly more likely to rate their satisfaction as "the best care imaginable."
The standard "menu" of advance directives includes the living will, health care power of attorney, and DNR order, all of which are independent legal documents. The living will documents a patient's wishes for care at end of life as it pertains to life-sustaining measures including artificial hydration and nutrition (AHN). The living will essentially serves as the patients "insurance policy" that their end-of-life wishes are documented and honored. The health care power of attorney, also known as durable power of attorney or health care proxy, designates a person or persons to carry out the patient's health-related wishes if they are unable to do so themselves. Lay people often mistake a power of attorney for financial matters as also granting health care decision-making capacity; however, these are two unique documents addressing two different areas of decisional authority. Unlike the former, which is executed by the patient, the DNR is a physician or clinician order addressing cardiopulmonary resuscitation wishes in the event of cardiac and/or pulmonary arrest. Many states have now enacted MOLST/POLST, which address resuscitation wishes as well as more specific wishes such as AHN, cardiac drips, and antibiotic therapy.
Communication
Assisting patients with advance directives is a duty all clinicians should embrace. However, advance directives may have little meaning if the patient and family have not had discussions about the patient's wishes, hopes, fears, values, definition of quality of life, and life goals. Too often, the health care power of attorney may feel conflicted about critical decisions because they never had clear detailed discussions about what their loved one really wants at end of life. Establishing goals of care and aligning those goals with the patient's care plan is the "bread and butter" of good palliative care and good primary care. Within our current health care landscape, a common challenge for most clinicians is finding the time to have a robust discussion about goals of care, inclusive of the family unit. Another common challenge is clinicians' lack of confidence in their communication skills as they pertain to having serious, often emotional discussions with patients and their families.
The "ask, tell, ask" method of communication is well documented66,67 and suitable for this type of communication. This strategy begins by eliciting the patients' understanding of their situation and allowing the clinician to assess knowledge base, educational level, emotional state, and any misperceptions. The next step is to deliver the information in a clear, concise, understandable manner typically divulging important information in bite-sized morsels to allow time for patients to process what they are hearing. The last step is to inquire about the patients' understanding of the information and, if needed, ask them to restate what was said to assess their understanding.
EPEC defines a seven-step protocol for having a successful goals-of-care discussion with patients and their family unit.68 This model, discussed below, incorporates the "ask, tell, ask" strategy.
Beginning these discussions with patients and their family units is not easy. Implementing a structured process for delivering "bad" news will assist in assuring this conversation will hold value and meaning to patients. This is an emotional discussion. We are taught in medicine to disregard or remove the emotion in the care that we deliver, but in the instance when a patient may be in need of palliative care, recognizing and acknowledging emotion and using it in conversation will be a powerful tool in developing trust with the patient and family. Part of this protocol teaches us to be prepared for this meeting. This is one of the most important discussions patients and families will ever have, so the deliverer of this message must be prepared and organized. It is important to set the stage with a proper venue, for example, selecting a large enough room in advance to accommodate the family, treatment team, and patient. It is important not to make the family feel rushed, so the clinician should sit down and talk directly with them. Clinicians should always introduce, by name and role, themselves and any other team members participating in the meeting and describe what goals the meeting hopes to accomplish.
It is relevant to assess what the patient and family know about the illness. This initial "ask" step helps reemphasize to the patients and family that their understanding of their disease process has value and is important to the treatment team. It is important to define what the patient and family wants to know about the disease and prognosis and to define their hopes and goals.
The next step is "tell." It is imperative to disclose this information to the patient and family in straightforward, understandable language with sincere honesty. It is important to suggest realistic goals as a medical expert, and to remain patient while working through unrealistic expectations. If emotions arise, it is important to recognize and acknowledge them in an empathic way, but attempt to remain focused.68
The final "ask" comes after development of the plan of care and summary review. Ask if there are any questions, define next steps and a follow-up plan, and lastly ask the patient and family for buy in, for example, "Does this plan of care that we developed together suit your needs and goals, and is it one you would be willing to follow?"
Prognosis
All experienced clinicians recognize that prognostication is far from an exact science. Some diseases, such as advanced cancer, may be more predictable than others, such a cardiac or pulmonary disease. Depending on the specific disease, various criteria may be used to help with prognostication, the details of which are outside of the scope of this article. Several interesting articles discuss perspectives on the overarching issue of addressing mortality. One 2011 perspective article attempts to address the value of discussing overall prognosis in the elderly patient population.69 Given that life expectancy decreases with age, the authors cite the paradox that most clinicians do not discuss prognosis with elderly patients unless they have a serious illness. They suggest a change in practice standards to include offering to routinely discuss prognosis with all elderly patients with a projected life expectancy of 10 years or less or by age 85, whichever comes first. The authors qualify their position by explaining that priorities in medical decision-making may vary based on potential prognosis; one must consider the potential immediate risks of some medical interventions and the potential lack of short-term gains in some preventive interventions. They suggest that by reframing the focus in the very elderly patient population toward quality of life, the primary clinician can help with more informed medical decision-making, as well as decisions around life goals.69 Another recent commentary article from The American Journal of Medicine broaches the issue of the U.S. "death-denying culture." The author courageously states "immortality is not something to be pursued."70 He suggests that when physicians have realistic discussions with patients about prognosis and death rather than accepting the default of death-denial, the rewards include patients actually receiving the care they desire, patients and families gaining the opportunity for life planning and closure, and decreased health care spending at end-of-life.69
Hospice Care
All hospice care is palliative care, but not all palliative care is hospice care. Hospice is a Medicare benefit that can be elected as a choice by all Medicare beneficiaries who meet eligibility criteria. The crux of eligibility is that the patient has a terminal illness with a projected life expectancy of ≤6 months if the disease runs its natural course. Given the understanding that prognostication is not an exact science, this 6-month projection should be based on the clinician's best estimate considering the natural history of the specific terminal disease in context with the individual patient's clinical condition and comorbid medical conditions. Many patients outlive this 6-month window and still remain eligible for hospice care based on continued decline, albeit at a slower trajectory than 6 months. Hospice programs and hospice and palliative medicine specialists are the experts in eligibility and should be utilized by primary care clinicians as a resource if eligibility is unclear. Rather than choosing to postpone or not refer a patient who may benefit from the care and support hospice offers, clinicians should make the referral and collaborate with the hospice program to help determine eligibility. Even if patients are determined not to be eligible for hospice, they likely would be appropriate for palliative care interventions in the primary care setting and they may be eligible for home health services until they reach a point in their illness that they do become hospice eligible.
Educational Resources for Primary Care
Most primary care clinicians care for only a few terminally ill patients each year;35,71 however, providing care for chronic illness, geriatric patients, and psychosocial support are daily occurrences in primary care practice. We have found in our practice that many clinicians lack some degree of confidence in their skills regarding prognosis determination and discussion, end-of-life discussions and decision-making, and pain and symptom management in patients with serious illness. This is not surprising since it has only been over the last few years that medical schools and residency programs in the United States have begun to incorporate hospice and palliative medicine principles into their education curriculum. This type of education is increasing, but there are still gaps for which clinicians must seek resources to fill.
Several excellent resources where primary care clinicians can access palliative care information include EPEC, ELNEC, CAPC, and AAHPM. A good information resource for patients and families is http://www.getpalliativecare.org.
How does Palliative Care fit into Health Care Reform?
Many changes have been proposed or implemented since the passage of the Patient Protection and Affordable Care Act (PPACA) in 2010. Included in the PPACA, hospital admission recidivism is a current focus of Medicare with potential penalties enacted for readmission within 30 days for acute myocardial infarction, pneumonia, and congestive heart failure. Under the PPACA, Medicare is also focusing on quality, outcomes, and patient satisfaction and includes Hospital Consumer Assessment of Healthcare Providers and Systems as one of the measures used to calculate value-based incentive payments to hospitals. Utilizing palliative care principles potentially can impact both of these areas in a positive way. Documentation of advance directives, meaningful goals of care conversions, hospice referral when appropriate, and diligent symptom management have the potential to decrease hospital readmissions. Honest, empathetic, patient-centered communication can improve patient satisfaction.
Conclusion
Palliative care, especially when implemented early, has proven benefits that are well documented by research. If palliative care principles are implemented, they have value, improve outcomes, and make a meaningful difference in the experience patients and their families face when battling serious illness. Many national organizations have endorsed and acknowledged the benefit of palliative care, which has created the momentum to improve access to its principles earlier in the disease trajectory. Evidence is clear that patients and families desire palliative care. Where early access to palliative care is available, research has proven value from both the patient experience and the treatment delivery team perspective. Specialty palliative care is still limited, especially in the outpatient setting, and will likely remain strained for the foreseeable future. Palliative care leaders continue to evaluate different models of ambulatory palliative care, but no single model currently stands out. In our current health care landscape, basic palliative care in the primary care setting has value and is appreciated by patients and families. Primary care clinicians can reduce suffering and improve the quality of life of their patients and families. Primary palliative care can have a real impact, both clinically and financially, on patient care in the United States, particularly as it pertains to our rapidly growing Medicare population.
References
- Connor SR. Hospice: Practice, Pitfalls, and Promise. London: Taylor & Francis. 1998; 4.
- NHPCO National Data Set and/or NHPCO Member Database. Available at: www.nhpco.org/sites/default/files/public/Statistics_Research/2012_Facts_Figures.pdf.
- Hoyert DL, Xu J. Available at: www.cdc.gov/nchs/data/nvsr/nvsr61/nvsr61_06.pdf.
- MedPAC Report to the Congress: Promoting Greater Efficiency in Medicare. Washington, DC: Medicare Payment Advisory Commission. June 2007.
- Thorpe KE, Howard DH. Health Aff 2006;25:w376-388.
- Cohen SB, Yu W. Available at: http://meps.ahrq.gov/mepsweb/data_files/publications/st354/stat354.pdf.
- The Dartmouth Atlas of Healthcare. Key Issues. End-of-Life Care. Available at: www.dartmouthatlas.org/data/topic/topic.aspx?cat=18.
- Final Chapter: Californians' Attitude and Experiences with Death and Dying. Available at: www.chcf.org/~/media/MEDIA%20LIBRARY%20Files/PDF/F/PDF%20FinalChapterDeathDying.pdf.
- Center to Advance Palliative Care. Available at: www.capc.org/tools-for-palliative-care-programs/marketing/public-opinion-research/2011-public-opinion-research-on-palliative-care.pdf.
- World Health Organization. Available at: www.who.int/cancer/palliative/definition/en/.
- National Hospice and Palliative Care Organization. Available at: www.nhpco.org/about/hospice-and-palliative-care.
- The National Comprehensive Cancer Network. Available at: www.nccn.org/professionals/physician_gls/pdf/palliative.pdf.
- Smith L. Am Fam Physician 2006;73:1104-1111.
- Morrison RS, et al. J Palliat Med 2011;14:1094-1096
- Center to Advance Palliative Care. Available at: www.capc.org/capc-growth-analysis-snapshot-2011.pdf.
- Hui D, et al. JAMA 2010;303:1054-1061.
- Berger GN, et al. Arch Intern Med 2011;171:2057-2059.
- Rabow MW, et al. Arch Intern Med 2010;170:654-655.
- Ferris FD, et al. J Clin Oncol 2009;27:3052-3058.
- Whelan CT, et al. Arch Intern Med 2004;164:175-180.
- The SUPPORT Principal Investigators. JAMA 1995;274:1591-1598.
- Temel JS, et al. N Engl J Med 2010;363:733-742.
- Ciemins EL, et al. J Palliat Med 2006;9:1401-1411.
- Meyer H. Health Aff (Millwood). 2011;30:390-393.
- Accreditation Council for Graduate Medical Education. Available at: www.acgme.org.
- Back AL, Curtis JR. West J Med 2001;175:150-151.
- Weeks JC, et al. JAMA 1998;279:1709-1714. [Erratum in JAMA 2000;283:203].
- Ferris FD, et al. J Clin Oncol 2009;27:3052-3058.
- Weissmann DE, Meier DE. J Palliat Med 2011;14:17-23.
- Lynn J. Available at: www.thehastingscenter.org/Publications/SpecialReports/Detail.aspx?id=1344.
- Moss A, et al. Clin J Am Soc Nephrol 2008;3:1379-1384.
- Moss AH, et al. J Palliat Med 2010;13:837-840.
- The National Comprehensive Cancer Network. Available at: www.nccn.org/professionals/physician_gls/f_guidelines.asp#distress.
- National Palliative Care Research Center. Available at: www.npcrc.org/resources/resources_list.htm?cat_id=1246.
- McCormick E, et al. Mt Sinai J Med 2012;79:579-585.
- Block SD, et al. J Gen Intern Med 1998;13:768-773.
- Barnett ML, et al. Arch Intern Med 2012;172:163-170.
- Lewis CL, et al. J Gen Intern Med 2000;15:75-83.
- Quill TE, Abernethy AP. N Engl J Med 2013;368:1173-1175.
- Back AL, et al. J Clin Oncol 2009;27:1137-1141.
- Quill TE, et al. J Palliat Med 2003;6:365-380.
- Meier DE, Beresford L. J Palliat Med 2008;11:823-828.
- Paice JA, et al. Am J Hosp Palliat Care 2004;21:19-27.
- Levy MH, et al. J Natl Compr Canc Netw 2009;7:436-473.
- The Joint Commission. Available at: http://www.jointcommission.org/assets/1/18/pain_management.pdf.
- Mularski RA, et al. J Gen Intern Med 2006;21:607-612.
- World Health Organization. Available at: www.who.int/cancer/palliative/painladder/en/.
- Osborne RJ, et al. Br Med J (Clin Res Ed) 1986;292:1548-1549.
- Shaheen PE, et al. J Pain Symptom Manage 2009;38:409-417.
- Panchal SJ, et al. Int J Clin Pract 2007;61:1181-1187.
- Jarzyna D, et al. Pain Manag Nurs 2011;12:118-145.
- Wood GJ, et al. JAMA 2007;298:1196-1207.
- Ripamonti C, Bruera E. J Pain Symptom Manage 1997;13:220-232.
- Claessens MT, et al. J Am Geriatr Soc 2000;48(5 Suppl):S146-S153.
- McCarthy M, et al. J R Coll Physicians Lond 1996;30:325-328.
- Addington-Hall J, et al. Stroke 1995;26:2242-2248.
- Voltz R, Borasio GD. J Neurol 1997;224(Suppl 4):S2-S10.
- Greenberg B, et al. J Urban Health 2000;77:150-165.
- Thomas JR, von Gunten CF. J Support Oncol 2003;1:23-32; discussion 32-34.
- Del Fabbro E, et al. J Palliat Med 2006;9:422-436.
- Campbell ML. Crit Care Clin 2004;20:403-417.
- Marciniuk DD, et al. Can Resp J 2011;18:69-78.
- Booth S, et al. Am J Respir Crit Care Med 1996;153:1515-1518.
- Nicholas LH, et al. JAMA 2011;306:1447-1453.
- Leung JM, et al. Chest 2012;142:128-133.
- Arnold RM. Available at: www.capc.org/palliative-care-professional-development/Training/c3-module-ipal-icu.pdf. Accessed July 1, 2013.
- Boxer H, Snyder S. Fam Pract Manag 2009;16:12-16.
- Robert Wood Johnson Foundation. Available at: http://endlink.lurie.northwestern.edu/goals_of_care/module7.pdf. Accessed July 1, 2013.
- Smith AK, et al. N Engl J Med 2011;365:2149-2151.
- Webster J. Am J Med 2013;126:
368-369. - Mitchell GK, et al. Med J Aust 2004;180:207-208.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
