Outpatient Pediatric Skin Rashes
Outpatient Pediatric Skin Rashes
Authors:
N. Ewen Wang, MD, Associate Professor of Surgery, Associate Director, Pediatric Emergency Medicine, Stanford University School of Medicine, Stanford, CA.
Alice Chao, MD, Stanford/Kaiser Emergency Medicine Residency, Stanford, CA.
Peer Reviewer:
Dennis A. Hernandez, MD, FAAP, FACEP, Medical Director, Pediatric Emergency Services, Florida Hospital for Children, Walt Disney Pavilion, Orlando.
Rashes can be really difficult. For the most part, we rely on our pattern recognition — "Oh, yes, I have seen this before." However, that only works if you are experienced or are working with someone who has seen that rash before. Further, skin tone differences and duration of the rash can make pattern recognition more difficult. While ideally all of our patients would have ready access to a dermatologist, at least in my practice, that is not an option.
This issue of EM Reports deals with pediatric rashes, some of the more difficult to diagnose. And because rash, particularly in this age group, may be a manifestation of systemic disease, a correct diagnosis is important.
— Sandra M. Schneider, MD, FACEP, Editor
Introduction
Skin rashes are a common chief complaint in any pediatric emergency department (ED). In 2008, skin rash was among the top 10 principal reasons for ED visits in the United States in patients younger than the age of 15 years.1 The most important role of the emergency physician is to recognize serious or life-threatening illnesses that require emergent treatment and admission. Also important, however, is the diagnosis and treatment of common rashes, which can reassure worried parents and provide patient comfort.
For the purposes of this review, this article will focus on some of the common rashes that present to the ED that can be managed on an outpatient basis. Specifically, this article will cover neonatal rashes, regional dermatitis, and scaly and vesicular rashes. This article will discuss the differential diagnoses and treatments of these common rashes. Life-threatening rashes and drug rashes are beyond the scope of this review and will not be covered.
It is essential for any emergency physician to be knowledgeable about the basics of dermatology. Therefore, we will start with a review of basic dermatologic terminology that is crucial to characterizing any rash.
Evaluating the Rash
History. A thorough history is important in the diagnosis of many skin conditions. Important features of the history include, but are not limited to, the following:
- onset of the rash/lesion;
- duration of symptoms;
- changes in the appearance over time;
- associated symptoms, such as fever, sore throat, headaches, arthralgias, pruritus;
- exposures such as new soaps, detergents, animals, plants, and insects;
- medications, especially antibiotics and anti-epileptic drugs;
- travel to areas with endemic diseases or outside the United States;
- food exposures such as milk, nuts, egg, and seafood.
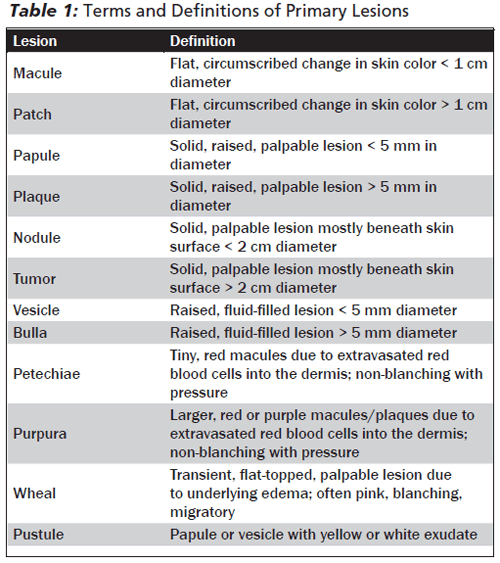
Primary Lesions. Primary lesions are the initial lesions caused by the disease process itself. The terminology is determined by the color of the lesion, whether the lesion is raised, the presence of fluid or blood within the lesion, as well as the size of the lesion. Table 1 lists the standard vocabulary and definitions used to describe primary lesions.2,3
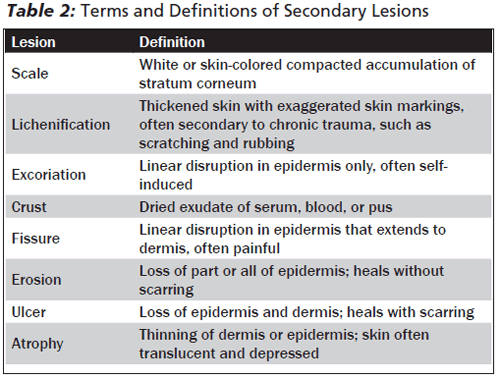
Secondary Lesions. Secondary lesions are the result of factors such as scratching, rubbing, infection, or treatment. Table 2 lists the standard vocabulary and definitions used to describe secondary lesions.2,3
Distribution/Configuration. Certain conditions present with eruptions in a characteristic distribution over the body (e.g., extremities, trunk, face, scalp, dermatome, or mucous membranes). These locations may or may not vary over time after onset of the rash.
Furthermore, certain rashes have characteristic patterns, such as linear, nummular (coin-like), or annular (circular).
Diagnosing the Rash
The majority of rashes are diagnosed empirically from a detailed history and a thorough physical exam. Most commonly, we know a rash because we have seen it before. However, just like other diseases, it is important to consider a differential diagnosis so that important etiologies are not missed. This article will review common dermatologic chief complaints in pediatric patients in the emergency department.
Neonatal Rashes
Neonatal rashes are common and can be very anxiety provoking to parents. This section provides a brief description and illustration of common, benign rashes in neonates.
Miliaria. Miliaria is a common finding in newborns, particularly in warm climates. It is rarely present at birth, often arising in the first few weeks of life. It is due to obstruction of eccrine sweat ducts by keratin, resulting in an accumulation of sweat within the ducts. Thus, lesions are often associated with occlusive dressings or clothing, fever, or use of an incubator, and are classically distributed on the face, scalp, and intertriginous regions.
Several types of these lesions have been described based on the level of obstruction within the sweat gland. Miliaria crystalline is characterized by 1 to 2 mm vesicles without surrounding erythema or inflammation; lesions typically occur on the head, neck, and trunk. Miliaria rubra consists of erythematous papules and pustules due to localized inflammation from obstructed sweat leaking into the surrounding dermis. (See Figure 1.) Miliaria profunda is characterized by papular, skin-colored lesions that both spread and disappear rapidly.
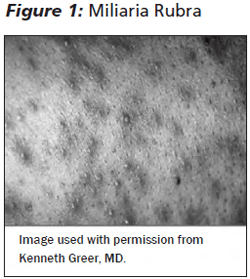
The diagnosis of miliaria is based on clinical findings. The differential diagnosis includes infantile scabies, neonatal herpes simplex, Candida, neonatal acne, or bacterial infection such as Staphylococcus aureus. If there is suspicion for alternative diagnoses, pustule contents should be sampled for bacterial culture or herpes simplex virus (HSV) polymerase chain reaction (PCR). Miliaria lesions are self-limited and should resolve quickly with techniques to decrease sweating, such as cool baths or loose clothing.4,5
Erythema Toxicum Neonatorum. Erythema toxicum neonatorum (ETN) occurs in up to 72% of full-term infants, although the etiology is unknown. Lesions are usually present within 24 to 48 hours, and sometimes they are even present at birth. ETN is characterized by erythematous macules and papules that progress to pustules on an erythematous base. (See Figure 2.) Lesions are approximately 1-3 mm in diameter and distributed over the proximal extremities and trunk. Palms and soles are typically spared.
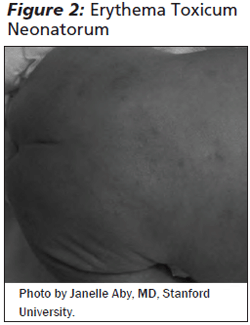
ETN is a clinical diagnosis; however, confirmation with a Wright-stained smear of pustule contents will reveal numerous eosinophils. The differential diagnosis includes miliaria, neonatal acne, neonatal herpes simplex, neonatal varicella, or bacterial infection such as Staphylococcus aureus. Similar to miliaria, if there is suspicion for alternative diagnoses, pustule contents should be obtained for further testing. ETN lesions are self-limited and resolve by day 5 to 7 of life without intervention.6
Acne. Neonatal acne occurs in approximately 20% of infants. Onset occurs at age 3 weeks. Inflammatory papules and pustules are characteristically distributed over the face, especially the cheeks and occasionally the scalp. Lesions may appear very similar to miliaria and are often confused with that condition. Most cases are mild and resolve with daily cleansing with soap and water. Neonatal acne usually resolves within 4 months without scarring.7
Seborrheic Dermatitis. Seborrheic dermatitis occurs between the ages of 3 weeks and 12 months, with peak prevalence at age 3 months.8 It is an eruption of erythematous plaques with greasy, yellowish scales in areas rich in sebaceous glands. The most common presentation in infants is an accumulation of these scales on the scalp, often referred to as "cradle cap." The retroauricular areas, cheeks, nasolabial folds, and forehead are often affected. Seborrheic dermatitis may also involve the intertriginous areas, diaper area, or the trunk. (See Figure 3.) Pruritus is mild, and infants are generally not bothered by the rash.
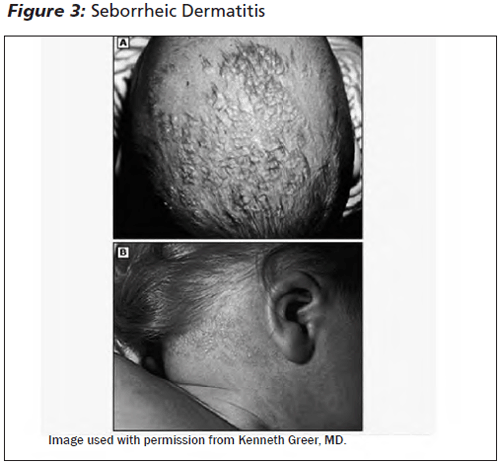
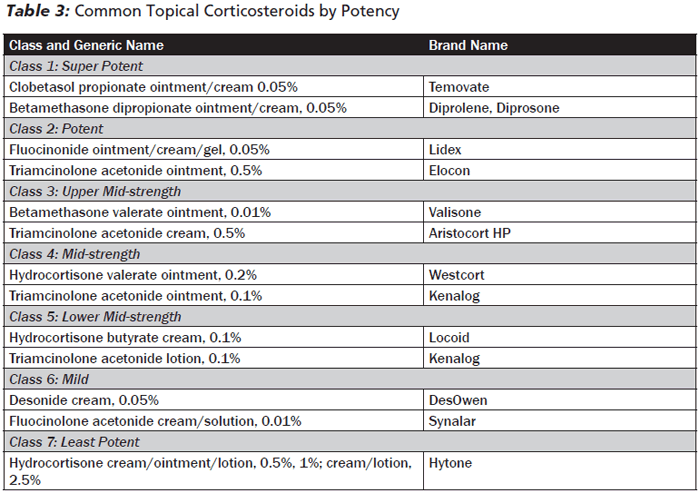
The differential diagnosis includes atopic dermatitis, diaper dermatitis, psoriasis, tinea capitis, and Langerhans cell histiocytosis. Seborrheic dermatitis is self-limited and should resolve spontaneously or with minimal intervention in weeks to months. Emollients such as baby oil or white petrolatum should be used liberally to loosen the scales. In more severe cases, a low-potency topical corticosteroid once daily for 1 week can be used.9 (See Table 3.) If lesions do not resolve with treatment, an alternative diagnosis should be considered. In cases of refractory seborrheic dermatitis, patients should be referred to pediatric dermatology for further work-up and treatment.
Neonatal Scabies. Scabies can present as early as 3-4 weeks of age. Infants present with diffuse erythematous papules, often affecting the palms of hands, soles of feet, and wrists. The back and head are often involved, in contrast to scabies in adults. (See Figure 4.) Widespread involvement is due to a hypersensitivity to mites. Infants may develop vesicles, pustules, and crusting, unlike older children. They may be asymptomatic or present with fussiness (due to intense pruritus), poor feeding, and failure to thrive.
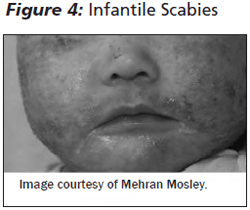
The differential diagnosis includes infantile acropustulosis, impetigo, or insect bites. However, the combination of a characteristic distribution and involvement of other family members should raise suspicion for scabies. Scrapings from burrows or papules may reveal mites or eggs. Treatment involves application of permethrin 5% cream at bedtime to all skin surfaces; this should be washed off after 8-14 hours. If symptoms persist after 1 week, a second application may be necessary. As in older patients, all lesions should be assessed for secondary bacterial infection.
Regional Rashes
Often, rashes are confined to a certain region of the body. This in itself may provide a clue to the diagnosis, along with the clinical history and appearance of the rash. Examples include diaper dermatitis and dermatophyte infections. We will review several regional rashes here, including diagnostic strategies and management.
Contact Dermatitis
There are two broad classes of contact dermatitis: allergic and irritant. Both are due to inflammation of the dermis and epidermis from direct contact with a specific substance.
Allergic contact dermatitis is a type 4 hypersensitivity reaction that requires prior exposure to the allergen. Often, the configuration and location of the rash are clues to the diagnosis. Plants such as poison ivy, oak, and sumac contain urushiol, a common allergen. Typical lesions are very pruritic, erythematous, and weeping, with vesicles that rupture and leave a crust. The rash is often in linear streaks from brushing against leaves/branches, although the plant's oils on the skin or clothing may spread to other areas of contact if not washed with soap and water. Nickel is another common allergen, causing pruritic, erythematous, scaly lesions where clothing, buttons, or jewelry contact the skin.10 Treatment of allergic contact dermatitis consists of eliminating exposure to the allergen and corticosteroids. Topical steroids of low or moderate potency may treat localized eruptions. (See Table 3.) When greater than 10% of the skin surface is involved, however, systemic steroids should be prescribed over a 2- to 3-week course to prevent rebound symptoms that may occur when steroids are stopped too early.11
Irritant contact dermatitis is due to exposure to substances that cause physical, mechanical, or chemical irritation. Diaper dermatitis is the most common irritant dermatitis in infants, with a prevalence of 7-35% in the United States.12 Findings range from asymptomatic erythema to painful scaling papules and erosions. The skin folds are typically spared, as they are not in direct contact with the diaper.13 The differential diagnosis includes candidal dermatitis, seborrheic dermatitis (rarely isolated to the diaper region and involves inguinal creases), psoriasis (may present initially to diaper region, but will be scaly), or HSV (lesions may be vesicular or pustular; a diagnosis of HSV in the diaper region should raise suspicion for abuse). Infants with so-called "diaper rash" should be allowed rest periods without a diaper to allow direct exposure to air. In addition, frequent diaper changes to limit prolonged contact with stool and urine are important. Topical barriers such as petrolatum gel, zinc oxide, or even sucralfate (in cases of severe or recalcitrant diaper rash) can be used to block chemical irritants from contacting the skin.14 Low-potency steroids may be used topically for brief periods of time for severely inflamed dermatitis (see Table 3); however, steroids should be used sparingly, as occlusion with the diaper increases absorption through the skin.15
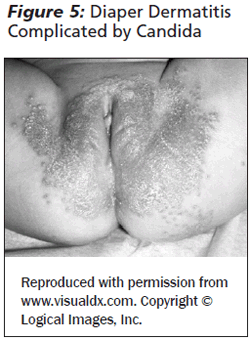
Irritant diaper dermatitis may become infected with organisms such as Candida albicans. These lesions are typically beefy, red plaques with satellite papules and superficial pustules. Skin folds may also become affected. (See Figure 5.) Antifungal agents such as nystatin ointment (100,000 units/g, apply topically 2-4 times per day) or ketoconazole 2% cream (apply topically 2 times per day) should be used beneath the barrier ointment until the rash has resolved.
Tinea
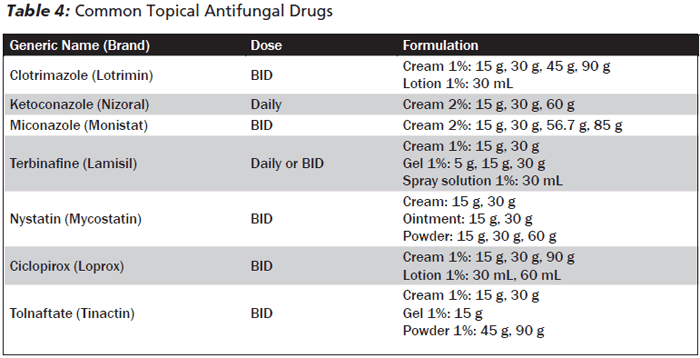
Dermatophytes are the most common cause of fungal infections of the skin. The major types of dermatophyte infections involve the scalp (tinea capitis), feet (tinea pedis), groin (tinea cruris), and other parts of the body (tinea corporis). In general, the diagnosis can be made clinically by the history, appearance of the rash, and location. Most infections can be treated with long courses of topical antifungals (see Table 4), although tinea capitis requires oral therapy.
Tinea capitis is a disorder of young children typically older than 1 year of age. African-American children are particularly susceptible. The most common form of tinea capitis in the United States is known as "black dot tinea capitis." It begins as an asymptomatic, erythematous, scaly patch on the scalp that slowly enlarges. Alopecia occurs as hairs within the patch break off at the scalp; follicles, thus, appear as black dots, in contrast to alopecia areata, in which there are no signs of broken hairs. In tinea capitis, painful lymphadenopathy may occur. Scarring with permanent alopecia can also occur if left untreated.
The diagnosis is made with KOH preparation of the hair shaft. A Wood's lamp exam of infected hairs reveals a characteristic silver-blue fluorescence. Oral griseofulvin (20 mg/kg/day divided BID for 6-12 weeks) is the first-line treatment for tinea capitis in children, as topical treatment is ineffective. Patients should avoid sharing fomites such as combs and hats. Occasionally, a kerion may form as an immune response in which lesions become boggy, elevated, and tender with exudate. Often, these are mistaken for a secondary bacterial infection presenting as an abscess. Treatment includes antifungals, although some advocate for the use of systemic glucocorticoids as well under the guidance of a dermatologist.16
Tinea pedis, more commonly known as athlete's foot, is the most common dermatophyte infection. It is spread by contact with spores shed by infected individuals (e.g., locker rooms) and more commonly affects adolescents. Acute infections are intermittent and recurrent; episodes are characterized by intensely pruritic erythematous vesicles between the toes and/or on the soles. There are usually sharp borders between affected and unaffected skin. Infection is most commonly mistaken for eczema or psoriasis; thus, it is important to confirm diagnosis with KOH preparation and culture so that topical steroids are not mistakenly prescribed, as this may alter the appearance of the rash and prevent accurate diagnosis in the future.
Treatment is typically with topical antifungal cream, such as terbinafine or an azole, once or twice daily for 4 weeks. (See Table 4.)
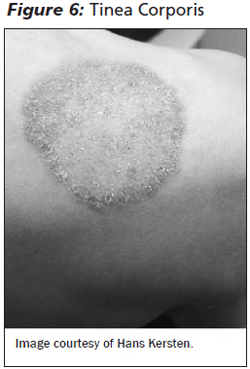
Tinea corporis begins as an erythematous, pruritic, circular scaling patch or plaque. Central clearing is present, while borders are erythematous and may be slightly raised. The lesion, thus, appears like a ring. (See Figure 6.) It often occurs in outbreaks among athletes with skin-to-skin contact. It may also be seen in adults caring for children with tinea capitis. Again, the diagnosis is made with a KOH preparation with increased sensitivity using scrapings from the border of the lesion. Other disease entities to consider are pityriasis rosea, psoriasis, nummular eczema, and erythema marginatum, all of which would have a negative KOH preparation.
Treatment involves daily application of topical antifungals, such as clotrimazole or ketoconazole. (See Table 4.) Systemic therapy should be used in cases refractory to topical agents, patients with extensive disease, or severely immunocompromised patients. Athletes should not be allowed to participate for 2 weeks after treatment begins to minimize spread of infection.
Tinea cruris, more commonly known as "jock itch," is a dermatophyte infection involving the inguinal region. It is much more common in adolescent boys than girls and begins after physical activity with copious sweating. The source of infection is usually a pre-existing tinea pedis infection.
It begins as an erythematous patch on the inner aspect of the upper thigh(s). Similar to tinea corporis, central clearing occurs with a slightly elevated border. It may spread down the thighs or up into the pubic region, extending onto the perineum and perianal areas. In boys, the scrotum is spared (in contrast to candidal intertrigo, in which scrotal skin is involved).
The differential diagnosis includes candidal intertrigo, seborrheic dermatitis, psoriasis, and erythrasma of the groin (a superficial bacterial infection). KOH preparation can be used to confirm the diagnosis. Topical antifungals, or oral griseofulvin if resistant to topical treatment, should be used for treatment. (See Table 4.) Concurrent tinea pedis should also be treated to prevent recurrence. Patients should also be educated to keep the area dry and to avoid tight-fitting clothing.
Scaly Rashes
There are many common scaly rashes in addition to the dermatophyte infections described above. However, they are not characteristically found in a specific region of the body, but rather can be more diffuse. This section will review other common scaly rashes.
Pityriasis Rosea. Pityriasis rosea (PR) is a skin condition of unknown etiology. Many believe it may be of viral etiology, as it is sometimes preceded by a prodrome and occurs in small local outbreaks. However, the cause is still unknown.
PR classically begins with a "herald" patch — a single, pink, oval/round lesion on the chest, back, or neck, approximately 2-5 cm in diameter. The lesion becomes scaly with central clearing. Within two weeks, smaller lesions appear on the trunk and extremities in a "Christmas tree" distribution on the back. The differential diagnosis includes tinea corporis, tinea versicolor, nummular eczema, guttate psoriasis, or secondary syphilis. Further testing may be done to exclude other diagnoses, such as a KOH preparation from lesions or serologic testing.
Patients with PR may complain of pruritus, which may be managed with antihistamines or medium-potency topical corticosteroids. (See Table 3.) Although some trials have suggested that erythromycin may help reduce the duration and severity of disease,17 other studies have shown conflicting findings and, thus, antibiotics are not recommended for treatment of PR at this time.18 In most cases, the rash should resolve in 4-6 weeks without intervention.19
Tinea Versicolor. Tinea versicolor is a common fungal infection that affects adolescents and young adults, but can affect children and infants as well. The highest incidence is found in tropical climates. It is due to a genus of saprophytic yeast known as Malassezia.
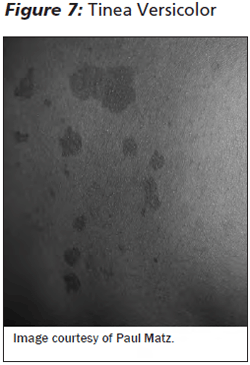
Patients present with variable changes in cutaneous pigmentation. (See Figure 7.) Lesions may be hyperpigmented, hypopigmented, or mildly erythematous. Hypopigmented lesions are often more noticeable during the summer, as affected areas do not tan after sun exposure relative to normal skin. Lesions are small, but may coalesce into larger patches. They are most commonly found on the upper trunk and upper extremities in adolescents. In children, however, lesions are often found on the face. A fine scale may be present, and lesions may be mildly pruritic.
The differential diagnosis includes pityriasis rosea, seborrheic dermatitis, vitiligo, or secondary syphilis. A KOH preparation can be used to confirm the diagnosis of tinea versicolor using scrapings from lesions. Both hyphae and yeast cells, often described as "spaghetti and meatballs," are usually present in tinea versicolor.
The first-line treatment includes topical therapy. Topical antifungals such as ketoconazole 2% cream once daily for 2 weeks have been shown to be effective treatments compared to placebo.20 (See Table 4.) Selenium sulfide 2.5% lotion for 1 week has also been shown to be superior to placebo.21 Systemic therapy should be reserved for patients with widespread tinea versicolor, or those who have failed topical therapy.
Atopic Dermatitis. Commonly known as "eczema," atopic dermatitis is a common presenting complaint in any pediatric ED, with a prevalence of 11% in the United States.22 It is characterized by a chronic course with intermittent flares, which bring patients into the emergency department.
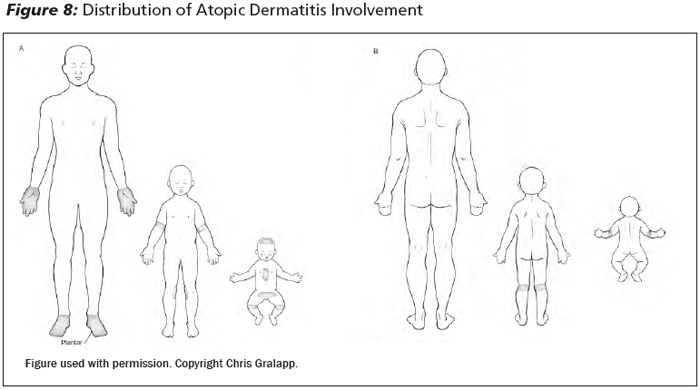
The rash typically begins by 2 years of age, and distribution varies by age. (See Figure 8.) Skin findings include erythema, scale, and occasionally serous oozing/crusting. It is severely pruritic, which helps to distinguish it from conditions such as seborrheic dermatitis and psoriasis. Other disorders to consider include scabies, Wiskott-Aldrich syndrome, hyperimmunoglobulin E syndrome, and other nutritional deficiencies, particularly in infants. When the diagnosis is uncertain, in cases refractory to standard treatment, or if an underlying disorder is suspected, referral to a specialist may be warranted.
Treatment includes a multi-step approach. Eliminating exacerbating factors (e.g., heat, low humidity, stress, excessive bathing, and exposure to irritants) and skin hydration using thick creams with low water content or ointments with no water content are crucial components to overall management.23 During flares, patients may be treated with topical corticosteroids. A low-potency steroid cream or ointment, such as 1% or 2.5% hydrocortisone, is effective for mild atopic dermatitis. A medium-potency steroid ointment, such as 0.025% fluocinolone or 0.1% triamcinolone, may be needed for more severe disease. Use of such higher-potency steroids should be limited to 10 days and should not be applied to the face.24,25
Complications of atopic dermatitis include superinfection of lesions, most commonly with Staphylococcus aureus. Chronic dermatitis may progress to include worsening erythema, pustules, and the classic honey-colored crust of impetigo. Treatment may include topical mupirocin or oral antibiotics for 10-14 days.26 Patients are also at higher risk when exposed to herpes simplex virus (HSV) and may develop eczema herpeticum (see Vesicular Rashes).
Vesicular Rashes
Varicella Zoster Virus. Primary infection by varicella zoster virus (VZV) causes a highly contagious vesicular rash known as varicella, or more commonly, chickenpox. It is typically a benign, self-limited disease in immunocompetent children. Transmission occurs via aerosolized droplets or direct contact with vesicle fluid. The average incubation period is approximately 14 days. Patients are considered to be infectious from 48 hours prior to onset of the rash until the skin lesions have fully crusted.
Patients typically present with a prodrome of fever and malaise. Within 24 hours, a generalized vesicular rash develops on the face, trunk, and extremities. Lesions begin as pruritic macules that become papules and vesicles (classically described as a "dew drop on a rose petal"), eventually forming crusted papules. (See Figure 9.) Lesions occur in crops and, thus, are present at different stages in development. Most lesions are fully crusted by day 6 in healthy patients.27 "Breakthrough" disease occurs in approximately 20% of vaccinated children with exposure to VZV. In these cases, the disease is milder and consists of an atypical maculopapular rash with an atypical pattern.
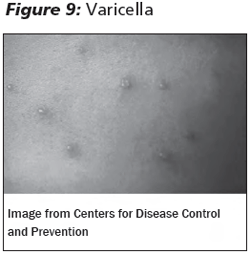
Complications of varicella in children have decreased dramatically since introduction of the vaccine in 1995. The most common complication remains bacterial superinfection, typically group A streptococcus. Other complications include pneumonia, encephalitis, and hepatitis. Immunosuppression, older age, and pregnancy are risk factors for developing complications from varicella.
Treatment includes symptomatic management, including antihistamines for pruritus and acetaminophen for fever in otherwise healthy hosts. Oral acyclovir (20 mg/kg, up to 800 mg per dose, four times daily for 5 days) can be used if given during the first 24 hours of rash in the following groups of individuals at increased risk of moderate to severe varicella: older children (> 12 years of age), secondary household cases, children taking inhaled or oral steroid therapy, or patients with a history of chronic cutaneous or cardiopulmonary disorders.28 Immunosuppressed children have a mortality rate of 7-14% from chickenpox and should be given IV acyclovir (10 mg/kg every 8 hours for 7 days) to reduce the risk of visceral dissemination, even if it is more than 24 hours since the onset of symptoms.29
Herpes Simplex Virus. A significant percentage of the population is infected with herpes simplex virus (HSV) types I and II. Most infections are asymptomatic. Once infection occurs, however, the virus lies dormant in the nerve ganglia and can reactivate to cause recurrent infection. HSV infections present differently depending on the age of the patient and site of infection. This section will review common HSV infections of various pediatric ages.
Neonatal herpes of the skin can present as vesicular lesions of the skin, mouth, or eyes. It typically presents within the first week of life and should prompt immediate evaluation, laboratory confirmation, and treatment with systemic acyclovir. Without treatment, herpes of the skin may progress to CNS involvement or disseminated herpes.
Herpetic gingivostomatitis is the result of most primary HSV-I infections in children between 6 months and 5 years of age. Patients may present with high fever and cervical lymphadenopathy. Lesions include small vesicles on an erythematous base. The perioral skin, tongue, gingival mucosa, and anterior palate may be involved, in contrast to herpangina (caused often by enteroviruses), which involves only the posterior palate. Lesions persist for 7-14 days and progress to painful erosions and ulcerations that may result in poor oral intake.
Herpes labialis, also known as "cold sores" and "fever blisters," is the result of recurrent HSV infection of the lips. A prodrome occurs of tingling, burning, or pain in the distribution of where lesions will appear. This is followed by painful grouped erythematous vesicles, which rupture and crust on the upper and/or lower lip. Recurrences are often triggered by stress, acute illness, or sun exposure and resolve in 5-10 days.
Whitlow. Herpetic whitlow occurs in thumb-sucking children with herpetic labialis or gingivostomatitis. It is an infection of the fingertip with white, clustered vesicles on an erythematous base and is very painful. (See Figure 10.) It is often mistaken for a bacterial infection, such as a paronychia; antibiotics and incision and drainage are not necessary, however.
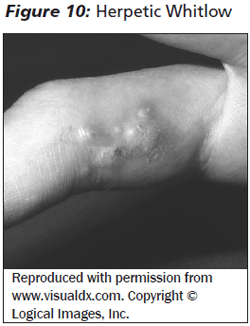
Eczema herpeticum occurs in patients with atopic dermatitis when skin lesions become superinfected with HSV I or II. Punched-out erosions, vesicles, or hemorrhagic crusts develop and require prompt treatment with acyclovir, depending on severity. (See Figure 11.) A clue to the diagnosis of eczema herpeticum is worsening eczema that does not respond to standard therapy. Diagnosis should be confirmed with viral PCR, and admission is often required in the young, as the infection can disseminate.
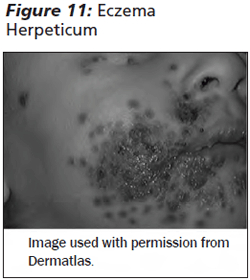
Treatment. HSV infections are diagnosed clinically and with viral PCR/culture of lesions. Most HSV infections are benign in healthy children and can be managed as an outpatient. Primary gingivostomatitis and herpetic whitlow should be treated with oral acyclovir 15 mg/kg per dose (max 200 mg/dose), 5 times daily for 7-10 days if treatment is started within the first 72 hours of infection. Treatment decreases the duration of the lesions and decreases viral shedding. Neonates and immunosuppressed patients may require admission for treatment. In addition, some patients with oral lesions may become dehydrated as a result of decreased oral intake and may require admission for IV hydration.
Conclusion
Pediatric dermatology is an extensive field in which the emergency physician must be comfortable. The history and physical exam are crucial in the diagnosis of most skin rashes. The emergency physician should be well versed in standard dermatologic terminology to describe skin findings, both for documentation and for discussions with consultants.
It is important for the emergency physician to be able to diagnose and treat common skin disorders to provide patient comfort, prevent transmission of disease, and alleviate parental concern.
References
- Pitts SR, et al, National Hospital Ambulatory Medical Care Survey: 2006 Emergency Department Summary. National Health Statistics Reports; 2008(7).
- Sanfilippo AM, et al, Common pediatric and adolescent skin conditions. J Pediatric Adolescent Gynecology 2003;16(5)269-283.
- Amieva-Wang N, et al. Amieva-Wang N, ed. A Practical Guide to Pediatric Emergency Medicine. Cambridge University Press; 2011.
- Feng E, Janniger CK, Miliaria. Cutis 1995;55(4):213-216.
- O'Connor NR, McLaughlin MR, Ham P. Newborn skin: Part I. Common rashes. Am Fam Physician 2008;77(1):47-52.
- Treadwell PA. Dermatoses in newborns. Am Fam Physician1997;56(2):443-450.
- Katsambas AD, Katoulis AC, Stavropoulos P. Acne neonatorum: A study of 22 cases. Int J Dermatol 1999;38(2):128-130.
- Sachdeva M, et al. Cutaneous lesions in new born. Indian J Dermatol Venereol Leprol 2002;68(6):334-337.
- Wannanukul S, Chiabunkana J. Comparative study of 2% ketoconazole cream and 1% hydrocortisone cream in the treatment of infantile seborrheic dermatitis. J Med Assoc Thai 2004;87(Suppl 2):68-71.
- Brasch J, Geier J. Patch test results in schoolchildren. Results from the Information Network of Departments of Dermatology (IVDK) and the German Contact Dermatitis Research Group (DKG). Contact Derm 1997;37(6):286-293.
- Hachem JP, et al. Efficacy of topical corticosteroids in nickel-induced contact allergy. Clin Exp Dematol 2002;27(1):47-50.
- Ward DB, et al. Characterization of diaper dermatitis in the United States. Arch Pediatr Adolesc Med 2000;154(9):943-946.
- Singalavanija S, Frieden IJ. Diaper dermatitis. Pediatr Rev 1995;16(4):142-147.
- Markham T, Kennedy F, Collins P. Topical sucralfate for erosive irritant diaper dermatitis. Arch Dermatol 2000;136(10):1199-1200.
- Humphrey S, Bergman JN, Au S. Practical management strategies for diaper dermatitis. Skin Therapy Lett 2006;11(7):1-6.
- Hussain I, et al. A randomized, comparative trial of treatment of kerion celsi with griseofulvin plus oral prednisolone vs. griseofulvin alone. Med Mycol 1999;37(2):97-99.
- Sharma PK, et al. Erythromycin in pityriasis rosea: A double-blind, placebo-controlled clinical trial. J Am Acad Dermatol 2000;42(2 Pt 1):241-244.
- Rasi A, Tajziehchi L, Savabi-Nasab S. Oral erythromycin is ineffective in the treatment of pityriasis rosea. J Drugs Dermatol 2008;7(1):35-38.
- Blauvelt A. Pityriasis rosea. In: Fitzpatrick's Dermatology in General Medicine, 7th ed. McGraw Hill; 2008:362.
- Savin RC, Horwitz SN. Double-blind comparison of 2% ketoconazole cream and placebo in the treatment of tinea versicolor. J Am Acad Dermatol 1986;15(3):500-503.
- Sanchez JL, Torres VM. Double-blind efficacy study of selenium sulfide in tinea versicolor. J Am Acad Dermatol 1984;11(2 Pt 1):235-238.
- Shaw TE, et al. Eczema prevalence in the United States: Data from the 2003 National Survey of Children's Health. J Invest Dermatol 2011;131(1):67-73.
- Ellis C, et al. International Consensus Conference on Atopic Dermatitis II (ICCAD II): Clinical update and current treatment strategies. Br J Dermatol 2003;148(Suppl 63):3-10.
- Kiken DA, Silverberg NB. Atopic dermatitis in children, part 1: Epidemiology, clinical features, and complications. Cutis 2006;78(4):241-247.
- Kiken DA, Silverberg NB. Atopic dermatitis in children, part 2: Treatment options. Cutis 2006;78(6):401-406.
- Koning S, et al. Interventions for impetigo. Cochrane Database Syst Rev 2004(2).
- Straus SE, et al. NIH conference. Varicella-zoster virus infections. Biology, natural history, treatment, and prevention. Ann Intern Med 1988;108(2):221-237.
- Kesson AM, et al. Acyclovir for the prevention and treatment of varicella zoster in children, adolescents and pregnancy. J Paediatr Child Health 1996;32(3):211-217.
- Nyerges G, et al. Acyclovir prevents dissemination of varicella in immunocompromised children. Journal Infect Dis 1988;157(2):309-313.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
