Palliative Care in the ICU: Benefits and Controversies
Palliative Care in the ICU: Benefits and Controversies
Special Feature
By Leslie A. Hoffman, RN, PhD, Professor Emeritus, Nursing and Clinical & Translational Science, University of Pittsburgh.
The quality of care provided to patients and their families at end-of-life has become a key element in discussions on U.S. health care system reform. Palliative care focuses on symptom management, communication about the goals of care, matching the care delivered with patient values and preferences, and support for the family.1 The Institute of Medicine and societies representing critical care clinicians support palliative care as a priority area for ICU quality improvement.1-4 However, guidance on how this can best be accomplished remains limited. The purpose of this article is to review support for the introduction of palliative care, models for structuring a clinical initiative to enhance palliative care, and literature supporting the success and challenges of attempts to accomplish this goal.
Supporting Evidence
Despite widespread enthusiasm, evidence supporting positive outcomes from unit-wide initiatives to implement palliative care or increase use of components of this care is sparse.5 Trials using a randomized design are difficult to implement and quality-of-life outcomes can be difficult to measure. There is, however, compelling evidence of the success of this approach from studies conducted in the outpatient setting. In a study of 151 patients with metastatic non-small lung cancer, those randomized to early palliative care reported a better quality of life and fewer depressive symptoms.6 Fewer patients in the early palliative care group received aggressive end-of-life care (33% vs 54%), but median survival was longer (11.6 vs 8.9 months). A recent editorial7 shared the experience of a patient with pulmonary fibrosis who, as a consequence of her diagnosis, lived a “bed to chair” existence. Her past history included 21 hospital admissions within 2 years for varied symptoms. Referral to palliative care resulted in a prescription for low-dose opioids to help with her dyspnea, low-dose benzodiazepines to help with her anxiety, and scheduled home care visits. Hospitalizations and frequent phone calls to her pulmonologist stopped and she started going out with friends because she felt better. Regular visits by home care nurses, not tied to her symptoms, provided support and she died 2.5 years later due to a ruptured aortic aneurysm.
Models for Initiating Palliative Care
Two models have been described for integrating palliative care into critical care practice — the “consultative” model, which focuses on use of an institutional-based consult service, and the “integrative model,” which focuses on interventions directed by the critical care team.5 When using the consultative model, palliative care is provided on a consultation basis for patients viewed at highest risk of death or at high risk for poor functional or cognitive outcomes at ICU discharge. Those who provide palliative care vary but consultation most commonly involves assessment by an advanced practice nurse or interdisciplinary team that includes members with diverse experience, e.g., physician, nurse, social worker psychologist, and/or chaplain. Some ICUs use “triggering criteria” that lead to initiation of a palliative care consultation.5 When the integrative model is used, palliative care is imbedded in the daily management of all patients in the ICU and initiated by the critical care team when deemed necessary. To promote ability to provide this care, clinicians have access to several online programs for advanced training. Examples include the End of Life Nursing Education Consortium (EL-NEC) Critical Care training program,8 Initiative for Pediatric Palliative Care program,9 and Critical Care Communication Skills program (C-3) for critical care fellows.10 A National Institutes of Health initiative, the IPAL-ICU Project, is designed to provide a comprehensive online repository of resources for providing palliative care in the ICU.10
Evaluation of Success
Several studies have evaluated outcomes of initiatives designed to integrate palliative care into the critical care setting, with varying success. Curtis and colleagues reported no improvement of family-assessed quality of dying or family satisfaction with care following introduction of an intervention that consisted of clinician education, local champions, academic detailing, feedback to clinicians, and system support.11 However, nurse-assessed quality of dying improved significantly and ICU length of stay decreased. The study enrolled 253 patients/families in the pre-phase and 337 patients/families in the intervention phase.
Penrod and colleagues conducted a prospective multisite study that evaluated how extensively clinicians employed a care and communication bundle designed to promote palliative care in two academic ICUs and one community hospital ICU.1 This study enrolled 518 patients and 336 family members. Initiation of bundle measures varied substantially. Highest ratings were achieved for pain assessment and management (80%) and lowest for distribution of an informational brochure (8%) regarding palliative care. Less than 20% of families participated in interdisciplinary family meetings by ICU day 5, as advocated in the bundle.1
White and colleagues conducted a single-center trial testing outcomes of a nurse-led intervention designed to improve integration of palliative care in the ICU.12 The intervention, titled Four Supports, involved adding a nurse to the critical care team to facilitate integration of palliative care. In this small trial, outcomes were highly successful. The nurse, who was titled a family support specialist, met an average of 48 ± 36 minutes per day with clinicians and patient/families. The intervention was positively rated by > 90% of physicians and families in regard to improving timeliness of communication, facilitating discussion of patient values and preferences, and improving care.12
Palliative Care in Daily Practice
As indicated by these findings, the goal of integrating palliative care into critical care practice is not easily accomplished. New tools can make this goal easier to achieve.8-10 Willingness to designate a unit-based care provider can improve integration, with highly positive ratings from physicians, nurses, and patients/families.12 However, unfortunately, studies continue to suggest that clinicians are not fully addressing patient values and preferences as part of daily care. In a study of cystic fibrosis physicians, those surveyed described numerous barriers to communicating with patients, including concern for taking away hope and uncertainty about when to initiative such discussions.13 From a survey of 278 elderly patients (80 ± 9 years), Heyland and colleagues reported that before hospitalization, most patients (76%) had thought about end-of-life care and only 11.9% preferred life-prolonging care.14 Most (73%) had formally named a surrogate decision maker. Of patients who discussed their wishes, only 30% had done so with the family physician and 55% with a health care team member. Agreement between patient preferences and medical record documentation was 30%.
As with most problems, the solution may lie in the middle. In a recent editorial, Quill and Abernethy advocated merging the two proposed models (consultative and integrative) for providing palliative care.15 To expand palliative care delivery, they propose a model that distinguishes primary palliative care (skills that all clinicians should have) from specialist palliative care (skills for managing more complex and difficult cases), so that they can coexist and support each other. Representative skills that might be required in each situation are listed in the table.
Table. Examples of Skills Included in Primary and Specialty Palliative Care
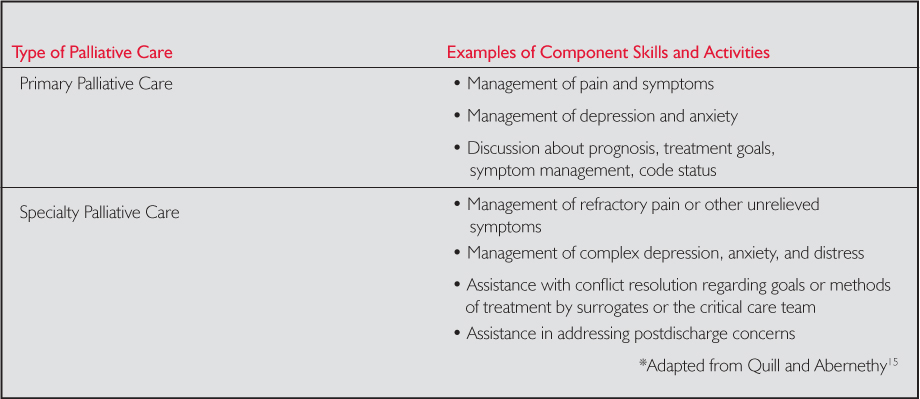
The model proposed above addresses three concerns. First, it is unclear whether there is sufficient availability of those specializing in the provision of palliative care to meet current and future needs. Second, many of the components of palliative care are within the current skill set of the critical care team and therefore can be easily included in the plan of care on a daily basis. Third, there is a concern that delegation of palliative care to a group of “specialists” risks further fragmenting care by diverting concern for symptom management and psychosocial support to others. As with changes in other aspects of care practices, understanding of how to best accomplish goals in a highly complex environment is evolving and strategies for ensuring integration of palliative care are becoming more clearly defined.
References
1. Penrod JD, et al. Meeting standards of high-quality intensive care unit palliative care: Clinical performance and predictors. Crit Care Med 2012;40:1105-1112.
2. Lanken PN, et al. An official American Thoracic Society clinical policy statement: Palliative care for patients with respiratory diseases and critical illnesses. Am J Respir Crit Care Med 2008;177: 912-927.
3. Davidson JE, et al. American College of Critical Care Medicine Task Force 2004-2005. Clinical practice guidelines for support of the family in the patient-centered intensive care unit. Crit Care Med 2007;35:605-622.
4. Selecky PA, et al. Palliative and end-of-life care for patients with cardiopulmonary diseases: American College of Chest Physicians position statement. Chest 2005;128:3599-3610.
5. Nelson JE, et al. Models for structuring a clinical initiative to enhance palliative care in the intensive care unit: A report from the IPAL-ICU Project (Improving Palliative Care in the ICU). Crit Care Med 2010;38:1765-1772.
6. Temel JS, et al. Early palliative care for patients with metastatic non-small cell lung cancer. N Engl J Med 2010;363:733-742.
7. von Guten CF. Palliative care for pulmonary patients. Am J Respir Crit Care Med 2010;182:725-726.
8. End of life nursing education consortium (ELNEC) – Critical care train the trainer program. Available at: http://www.aacn.nche.edu/ELNEC/CriticalCare.htm.
9. Initiative for pediatric palliative care curriculum Available at: http://www.ippcweb.org/curriculum.asp.
10. Center to advance palliative care. Available at: http://www.capc.org.
11. Curtis JR, et al. Integrating palliative and critical care: Evaluation of a quality-improvement intervention. Am J Respir Crit Care Med 2008;178:269-275.
12. White DB, et al. Nurse-led intervention to improve surrogate decision making for patients with advanced critical illness. Am J Crit Care 2012;21:396-409.
13. Dellon EP, et al. Physician practices for communicating with patients with cystic fibrosis about the use of noninvasive and invasive mechanical ventilation. Chest 2012;141:1010-1017.
14. Heyland DK, et al; for the ACCEPT (Advance Care Planning Evaluation in Elderly Patients) Study Team and the Canadian Researchers at the End of Life Network (CARENET). Failure to engage hospitalized elderly patients and their families in advance care planning. JAMA Intern Med 2013; Apr 1. [Epub ahead of print.]
15. Quill TE, Abernethy AP. Generalist plus specialist palliative care: Creating a more sustainable model. N Engl J Med 2013;368: 1173-1175.
The quality of care provided to patients and their families at end-of-life has become a key element in discussions on U.S. health care system reform.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
