Case Management Insider: Managing Length of Stay Using Patient Flow Part 4
Case Management Insider: Managing Length of Stay Using Patient Flow – Part 4
By Toni Cesta, PhD, RN, FAAN
As with any process, it is necessary to track and trend the metrics associated with the process and its expected outcomes. In the last three Parts of “Managing Patient Flow,” we reviewed all the issues and elements associated with understanding patient flow in the hospital setting. This month we will review some examples of patient flow report cards that you can use to track and trend your patient flow processes as well as identify performance improvement opportunities.
The report card should have the following components:
1. The desired direction of the measure.
Each measure is expected to improve by either increasing or decreasing in direction. For example, the hospital would expect to see the length of stay go down, so the desired direction is a down arrow (↓). The number should be decreasing if the outcomes are met.
Conversely, some of the measures’ desired direction is an increase in the number.
When developing the measure, consider whether you expect to see the metric increase or decrease and provide that direction on the report card.
2. The measure.
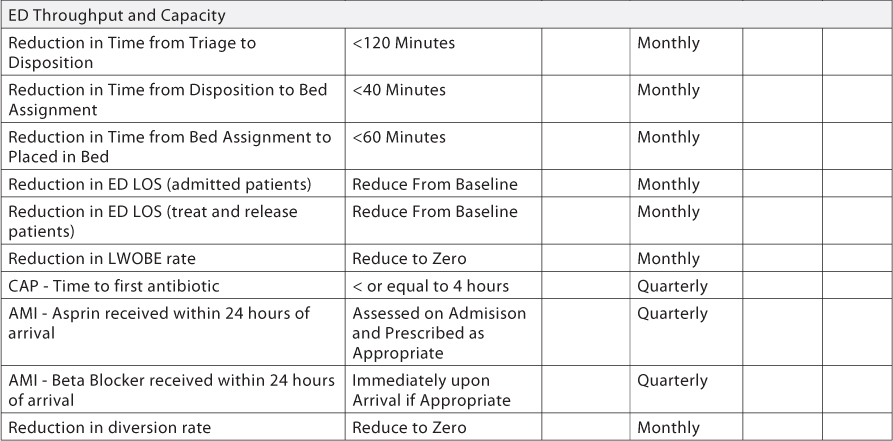
The measures should be based on the categories you are monitoring. The common categories can be found in the report card example above. They include the issues most directly related to patient flow:
a. Length of stay
b. Emergency department
c. Peri-operative services
d. Housekeeping
e. Laboratory
f. Radiology
You may find that in your hospital you need the addition of other categories. These other categories can always be added on as you find the need.
Within each broad category you will need to select the processes appropriate to that category. As you can see above, each section has a series of metrics that break that broad category into measurable components. The more specific you can be with these components, the easier they will be to measure. Each measure that is selected must have a measurable metric associated with it. If it cannot be measured, it should not be included.
Since we are measuring patient flow processes, the majority of these measures are going to be in time intervals. It is critical that these timeframes make sense and therefore you will most likely need to develop the measures with the department in question. The Joint Commission is interested in how your organization measures and monitors patient flow and is very interested in flow in the emergency department, so let’s use that as our example.
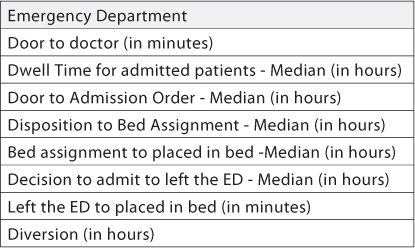
The measures listed above for the emergency department each have a time frame in hours or in minutes. In some instances these may be averages, medians or totals. Be sure to cross-walk the measures against any standards, either national, regulatory or internal, so that you are collecting meaningful data. In the case of the emergency department, work with the leadership in that department so that you can avoid duplicating data collection that is already taking place. For example, the ED may already be monitoring many of these metrics for their own internal use. Be sure they understand that these metrics will become part of an inter-departmental report card that includes data from many other departments and processes.
Sample Patient Flow Report Card
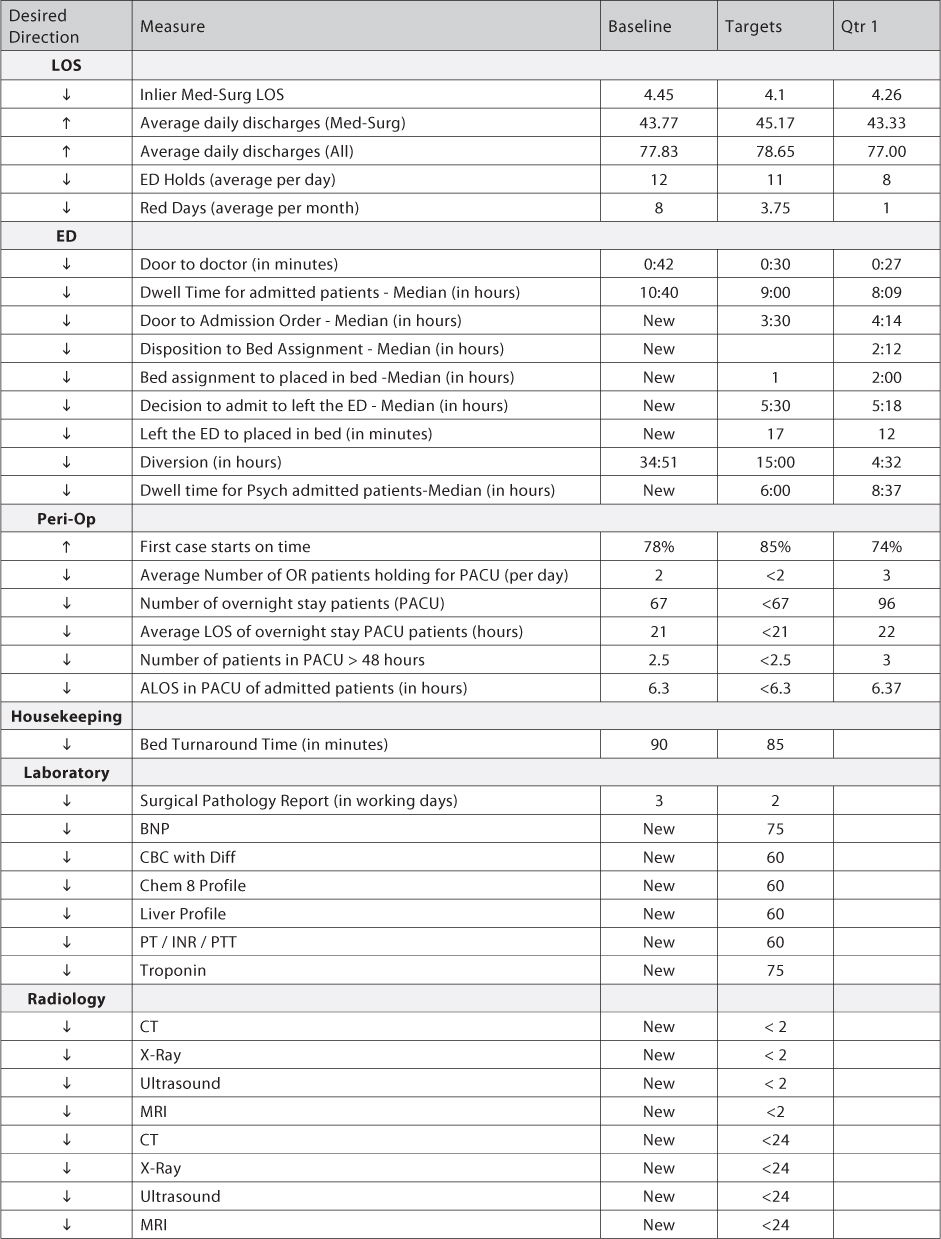
It is important to understand that patient flow is affected by all departments and disciplines in the hospital. Therefore, a report card must be all-encompassing and take into account all the relevant work processes that affect it.
The Baseline
The baseline data should reflect the prior year’s performance in the category listed. If a particular measure was not captured the prior year, then baseline can be listed as NA (not available). In all other instances, the baseline should reflect the hospital’s own internal results. These results will set the minimum acceptable level for that measure.
Targets
The targets are the goals or outcomes that you want to reach for the time period of the report card. The targets can be selected based on a number of different indicators:
• An improvement from the prior year’s hospital baseline
• A national standard or target
• A regional standard or target
• A regulatory standard such as Joint Commission, state department of health, CMS
• Same as prior year’s target
Targets should always be practical and reasonable. Even though the improvements you are looking for may be way beyond your current performance, do not select a target that is far beyond your reach. If your performance improvement need is very great, you may want to select incremental improvements that take place over a period of time. For example, you may want to set quarterly improvement targets that have smaller incremental improvements or even bi-annual targets. Whatever you select, you do not want to make it so far beyond reach that staff become frustrated and lose momentum.
Some targets may have plateaued, meaning that the performance cannot be improved. If that performance level is maintained for a period of time, you may want to consider removing that target and re-checking in a year or so. If you opt to do this, just remember to re-check that indicator the following year. If there has been slippage in its performance, then you may want to put it back on the report card again.
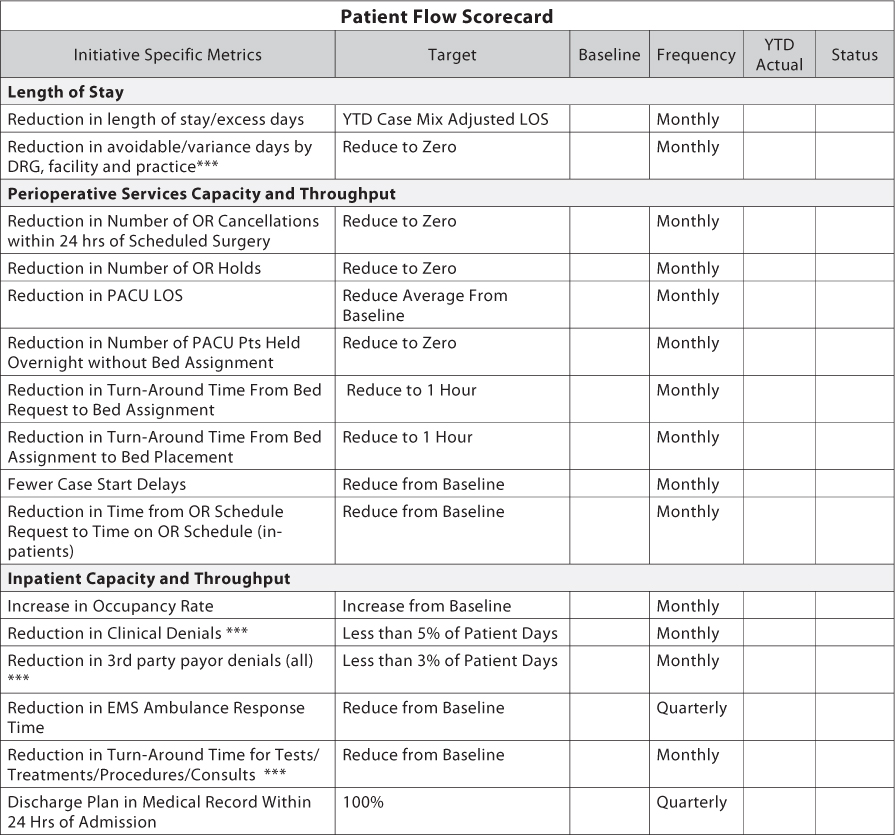
There are a variety of models to use for a patient flow report card. Above is another example of a format you may want to consider using.
Regardless of which format you choose, or which data sets you opt to measure, you should always remember to be consistent to and to pick measures for which data is available. It may take you some time to gather all the information the first few times you put the report card together and it will seem like a lot of work. If you stick with it, the departments that have to feed you the data will come on board. Be sure to share the information with them so that they can see its value and be part of the process.
Summary
Managing patient flow is a complex process that includes the daily management of patient throughput and capacity issues, and also the measurement and management of monthly data indicators. These indicators touch on every department and discipline in the hospital and should be readily shared and discussed. Because patient flow management is so complicated, it will require the active participation of a steering committee as well. The department of case management cannot manage patient flow alone. No department can. It is an interdisciplinary issue and the solutions must come from the interdisciplinary team.
Be sure to keep track of your daily admissions and discharges, available beds and daily bottlenecks. At the same time, look for patterns and opportunities in the data you collect to continuously improve flow over time. Stay current with The Joint Commission standards on patient flow which can be found in the leadership section of the standards. Patient flow is an old problem with a new name. Reductions in payment, and the need to continuously manage length of stay require a deep dive look at all the elements affecting your hospital’s flow.
In the last three Parts of Managing Patient Flow, we reviewed all the issues and elements associated with understanding patient flow in the hospital setting. This month we will review some examples of patient flow report cards that you can use to track and trend your patient flow processes as well as identify performance improvement opportunities.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
