The Quality=Cost Connection: Performance measures depend on effective use of good data
The Quality=Cost Connection
Performance measures depend on effective use of good data
Part 1 of a 2-part series
By Patrice Spath, RHIT
Brown-Spath Consultants
Forest Grove, OR
"Is performance acceptable?" is an important and fundamental question that can be asked of any health care process. Performance measures can help answer this question, but only if the data are used effectively. Too often, performance is judged by whether standards are achieved. Suppose the nursing department sets the standard, "we will not have more than 10 patient falls in any month." Typical actions that might come from this standard are:
• soliciting reasons why some months have more than 10 patient falls;
• comparing data on months with more than 10 falls to the data on the "good" months;
• having celebrations for months where the standard is met;
• taking disciplinary action on people who are deemed responsible for patient falls or on supervisors when expectations are not met;
• reducing the number of patient falls that are reported to supervisors.
While the intention of keeping the number of patient falls to a minimum is good, any of these actions can be harmful. They can lead to fear, cover-up of problem areas, and breakdown of teamwork.
While standards play an important role in defining correct actions individuals should take when caring for patients, standards may not be the best way to evaluate the results of performance measures. Measures tell us how a process is performing. To judge the quality of process performance we must study the pattern of variation revealed by the measurement results. If the process is controlled, meaning observations or results fall seemingly at random within some overall natural pattern, then the process is performing at its natural capability. Measurement variation in a stable process is termed, "common cause variation." For a manager or committee to react to normal process variation and expect explanations or "quick-fix" corrective actions is wasteful.
Well-intentioned actions made to correct common cause variation can potentially increase variation and negatively impact process performance. Adjusting a process when adjustments are not needed is called "tampering." Consider a hospital pharmacy technician who monitors the completeness of incoming physicians’ orders. Every day, he tallies the number of incomplete orders that require pharmacy intervention prior to filling the request.
Avoiding unnecessary variation
If in one month the total number of incomplete orders goes up, the pharmacy director asks the nursing staff to add a double-check into the process for obtaining physician orders. If the number of incomplete orders goes down, the nurses are told it’s OK to relax their vigilance. The pharmacy director sounds like a conscientious person when in fact, he is unnecessarily adding variation to the process.
If the process is out-of-control or unstable, meaning the observations fall in patterns that seem to defy the laws of probability, then special causes of variation are present. People involved in the process ought to be able to identify these special causes because of their closeness to the process. For example, if the number of patient falls significantly rises in one month, one possible cause of this variation might a short-term change in the nurse/patient ratio on a particular unit. The methods used to prevent patients from falling (the process) have not changed; however, something out of the ordinary occurred. Random or special causes tend to cluster by person, place, and time.
The goal of performance improvement is to eliminate special cause variation in a process, and where desirable, reduce common cause variation. The less the process varies, the more confidant you can be about the output. Furthermore, variation in clinical process is associated with a higher risk of error or patient harm.
To identify the extent of variation in a process, a technique known as statistical process control is used. This technique involves the use of control charts to plot measurement results. A control chart is a time-series graph of performance measurement data, similar to a run chart. See chart showing the rate of patient falls.
Control Chart: Rate of Patient Falls
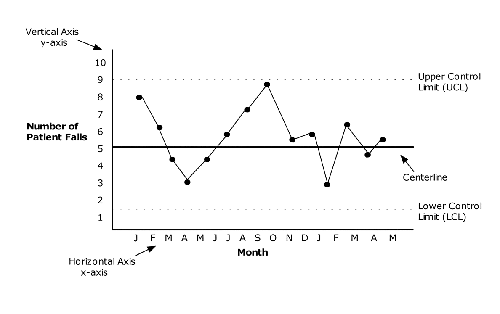 |
The number of patient falls is shown on the vertical or Y-axis. The horizontal or X-axis represents the time interval for taking measurements. In this example, measurements are taken monthly; however, the frequency for measuring or monitoring performance may be hourly, daily, or weekly. As data become available, they are entered chronologically onto the chart. The data points are connected with a line. A centerline is added as a visual reference for detecting process shifts or trends. The centerline represents the mean or median of the charted data. In addition, control limits computed from the data are placed at equal distances on both sides of the central line.
The control chart is a useful tool for displaying data in the order that they occur with statistically determined upper and lower limits of expected process variation. It is one of the best methods for identifying special causes of process variation, monitoring process performance, and determining if process changes have had the desired effect.
A control chart can be a very powerful performance management tool. The following is an example of how a control chart can be used by managers in day-to-day situations:
Using a control chart to monitoring test turn-around times, the laboratory staff know the process as it exists today. They know they cannot meet their test report turnaround expectations 100% of the time. At best, 1% of the test results they send out in a day will be late (more than one hour beyond the established threshold), and at worst, 13.4% of the results will be late. A team of laboratory staff reviews the special causes or the out-of-control points and identifies a common theme among them.
Every time someone is out sick, the process goes out of control. To eliminate this special cause of variation, the supervisor obtains permission to call in a temporary employee to cover for the absent regular employee. The control chart of test turnaround times helps the staff monitor whether special cause variation has been eliminated with this intervention.
To reduce common cause variation in the process, the laboratory must change the testing process. The laboratory director organizes another team to work on improving the overall process. Using process improvement techniques, the team will work to identify and reduce common causes of variation in the process. If they are successful, they will have to have new control charts made up, because the mean turnaround times will have decreased and the upper and lower control limits will be lower and closer together than the ones used on the old control chart.
It is in detection of situations where the process appears to act differently from its predicted pattern that the control chart proves its value. If the process output (in this case, test report turn-around times) exceeds a control limit (upper or lower) or reveals suspicious trends or patterns, those situations need to be investigated and resolved. Once the process output remains within the control limits and is stable, it does not necessarily mean that the process is acceptable — only that the process output is more predictable and that further reduction of variation will require a significant process revision.
(Next month’s Cost-Quality Connection column will discuss the use of the individual and moving range chart to evaluate the results of common health care performance measures.)
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
