An Overview of Complementary and Alternative Medicine for the Primary Care Provider
An Overview of Complementary and Alternative Medicine for the Primary Care Provider
Author: Felise Milan, MD, Associate Professor of Clinical Medicine, Albert Einstein College of Medicine, Bronx, NY; Clinical Practice, Montefiore Medical Center, Bronx, NY.
Editor’s Note—Complementary and alternative medicine (CAM) is one of the most visible and fastest growing areas of health care. It is well documented that patients are actively seeking and using a wide variety of alternative medicine therapies.1,2 At the same time, primary care providers (PCPs) may have a difficult time managing the burgeoning information from these disciplines. Since 1966, more than 38,000 publications related to this field have been referenced in Medline alone with the bulk being published in the last 10-15 years. The interest in this area on the part of the medical field has been largely driven by patient use and requests for information and not by the literature or new scientific discoveries.
Much of what we know of the use of CAM in this country comes from 2 large landmark studies done by David Eisenberg, a Harvard internist.1,2 He performed 2 random national telephone surveys of 1500 and 2000 people, respectively, which showed that the overall use of alternative therapies had increased from 34% in 1990 to 42% in 1997. Visits to alternative providers had increased 47%, and the total number of therapies used had increased 65% (from 577 per 1000 people to 953 per 1000) in the same period of time. Out-of-pocket money spent on alternative therapies increased 45% (from 14.6 billion in 1990 to 27 billion in 1997). The most commonly used therapies in the 1997 survey were relaxation techniques, herbal medicine, massage, and chiropractic. Some of the most compelling data for PCPs are that only 39% of alternative therapies used were discussed with the respondent’s medical doctor and among the adults taking prescription medications (44% of the sample), 1 in 5 reported the concurrent use of herbs or megavitamins. Much of these data had been confirmed in other smaller studies.3,4 These data must be interpreted, however, with the knowledge that it captures an exclusively English-speaking segment of the population and does not fully inform us about the use of more traditional and folk medicines.
The use of CAM worldwide reflects the same patterns as we have seen in the United States. There are differences among CAM products used and CAM providers seen from country to country, which vary depending on tradition, availability, and local preferences. In the United Kingdom, homeopathy is popular and a Faculty of Homeopathy appointed by the National Health Service now oversees its use. In Scotland, more than 20% of general practitioners have completed training in homeopathy and 25-35% of general practitioners use it in practice in France and Germany.5 Herbal medicine is extremely popular in Germany where Commission E in its Ministry of Health regulates it. This commission evaluates the safety and efficacy of herbal products, and "approved" herbal medicines are paid for by their national health insurance plan. (Herbal medicine will be the subject of a subsequent edition of Primary Care Reports). Chiropractic is popular throughout Europe, Canada, and Australia. Acupuncture, while practiced extensively in Asian countries, is also gaining popularity throughout Europe.
With the acknowledgment that many of our patients are using these alternative modalities comes the responsibility to both take the history and address the questions from our patients. This paper will describe what CAM is and how the health care industry and field of medicine has responded to it. We will also describe in more detail some of the most commonly used therapies, acupuncture and traditional Chinese medicine, chiropractic, homeopathy, and massage, and the evidence to support their use. Finally, we will address how to discuss the subject with our patients and how to make referrals.
Definitions
There has been much discussion on how to define alternative medicine and what is the most appropriate term to use. Some of the terms used include "unconventional," "holistic," and "integrative medicine." The National Institutes of Health (NIH) defines CAM as "a broad range of healing philosophies, approaches and therapies that are not taught widely in medical schools, not generally used in hospitals, and not usually reimbursed by medical insurance companies." This, however, is a definition of exclusion; it defines CAM by what it is not and not by what it is. At this point in time, this may be the best we can do. Perhaps it is more helpful to consider the NIH’s classification of CAM practices (see Table 1), which lists general categories of alternative practices and illustrates the enormous heterogeneity of the fields involved.
| Table 1. NIH Classification of CAM Practices |
| • Alternative Systems of Medical Practice (eg, acupuncture, ayurveda, homeopathy, traditional Chinese medicine) |
| • Bioelectromagnetic Applications |
| • Diet, Nutrition, Lifestyle changes |
| • Herbal Medicine |
| • Manual Healing (eg, chiropractic, massage, osteopathy, reflexology) |
| • Mind/Body Control |
| • Pharmacological and Biological Treatments (eg, antioxidant, chelation therapy) |
Who Uses CAM and Why?
The effect of CAM on the health care industry has been almost entirely patient driven. The explosion in patients’ use of CAM is a result of a confluence of factors including increasing patient autonomy, society’s changing view of health, and the growing recognition of traditional medicine’s limitations. While many have speculated that patients have turned to CAM and away from conventional medicine, one national survey6 found that the use of CAM was not predicted by negative attitudes or experiences with conventional medicine and that only 4% of that sample relied exclusively on alternative forms of health care. We do know that the CAM user is more likely to be female, not African-American, middle-aged, from a higher socioeconomic background with a higher education level, live on the West or East coasts,1,2 and does report a more "holistic health philosophy."6 The conditions for which CAM is used range from more benign chronic conditions (ie, back pain, allergies, headache, fibromyalgia, mood disorders, fatigue, etc) to more serious and incurable diseases like cancer, HIV, and multiple sclerosis.
Insurance Coverage of CAM
The insurance industry has responded to consumer demand by experimenting with new plans that provide some coverage for select modalities. Several large insurance companies, including Oxford Health Plans, Cigna, Kaiser Permanente, the Blue Crosses and Blue Shields of Washington, Alaska, California, Ohio, and Michigan now provide varying levels of coverage of acupuncture, chiropractic, and massage. A few plans cover homeopathy and herbal products. Some plans require referrals from PCPs.
The industry has also been investigating the financial feasibility of covering CAM services. Surveys of the insurance industry have confirmed that the expansion of coverage is being driven almost exclusively by market forces with minimal importance being placed on proven efficacy.7 Legislation of the insurance industry has also followed this trend. In 1996, a law was passed in Washington state requiring insurers to pay for visits to all categories of health care providers licensed by the state (including acupuncturists, naturopaths, etc). This law has survived legal challenges by the insurance industry and has been upheld by the Washington state Supreme Court.
Response of the Medical Field to CAM
The response of the medical field to CAM has been mixed. While the editors of some leading medical journals have written scathing editorials condemning any attention paid to CAM, others have supported a responsible and research-based inquiry into the area. The importance of CAM has been recognized by the NIH, which established an Office of Alternative Medicine in 1992 with a budget of $2 million, which was upgraded in 1998 to the National Center for Complementary and Alternative Medicine (NCCAM) with an annual budget of $68 million in 2000. The NCCAM serves as a free clearinghouse of information for the public, as well as those in medicine, and provides grants for basic science and clinical research in the field. It also funds 10 specialty centers for CAM research across the United States, including Bastyr University in Washington as an AIDS site and Columbia University in New York as a center for Women’s Health Research.
There has been an increasing presence of CAM in medical education. A 1997 survey found that 75 medical schools in the United States offered 123 courses (68% electives and 31% required).8 This was up from 27 schools offering the subject just 2 years earlier.9 Several schools offer comprehensive courses including lectures, demonstrations, case discussions and critical review of the literature. A 1995 survey revealed 75 family practice residencies were including CAM in their teaching.10 A few internal medicine residency programs have also begun to add CAM to their curriculum.9,11 Harvard University School of Medicine offers a CAM research fellowship and the University of Arizona offers a fellowship program in integrative medicine directed by Andrew Weil, MD.
Several academic institutions (ie, Harvard, Dartmouth, SUNY Stonybrook, etc) have started clinical CAM programs that offer a variety of CAM therapies on an inpatient and/or outpatient basis. Stanford Health Systems, which provides health services to students and employees in the Stanford University system, have started a complementary medicine clinic.
Several surveys done in Europe and Canada reveal support for CAM practices among physicians.12,13 Astin reviewed 10 international studies with a total of 3821 MDs surveyed, which revealed relatively high rates of referrals by physicians to CAM providers (43% referring to acupuncture, 40% to chiropractic, and 21% to massage).14 Even higher percentages of physicians rated various areas of CAM as useful with 58% rating massage as useful, 49% for acupuncture, 25% for chiropractic, and 15% for herbal medicine. The level of acceptance of CAM by individual physicians in the United States remains less clear but a few surveys reflect similar referral patterns. A survey of clinicians working for Kaiser Permanente found that 89% of adult PCPs and obstetricians had used or recommended to patients at least 1 of the 20 CAM practices listed in the survey during the previous 12 months.15
Acupuncture and Traditional Chinese Medicine
Background: Use in the United States
With a history spanning more than 4000 years, traditional Chinese medicine (TCM) is the oldest primary health care system. TCM takes a holistic and spiritualistic view of the human organism, seeing it as one small part of the larger universe. Therefore, any individual’s health cannot be easily extricated from their relationship with the natural world around them. TCM defines health as a balance between the complementary and contradictory forces of Yin and Yang and the flow of the vital energy force known as Qi ("chee"). In health, Qi flows freely along meridians or channels to all parts of the body (see Figure 1) and, conversely, disease results from an excess, deficient, or stagnant flow of Qi. The other component necessary for health is harmony between the five "phases" of energy or five "elements" (fire, earth, metal, water, and wood). A different balance of these components is optimal for each individual, and it is the job of the TCM doctor to tailor therapy accordingly. There is also a strong belief that physical and emotional aspects of health care are not only interrelated but also inseparable. Another stark contrast between TCM and Western medicine is the Eastern emphasis on prevention of disease. The Chinese medicine practitioner believes that if kept in good balance, the body will keep itself healthy and the role of the practitioner is to help their patients maintain that balance. They believe that once the body’s systems begin to fail and disease is evident by blood tests and radiological testing, it is much more difficult to treat and the practitioner has missed the boat.
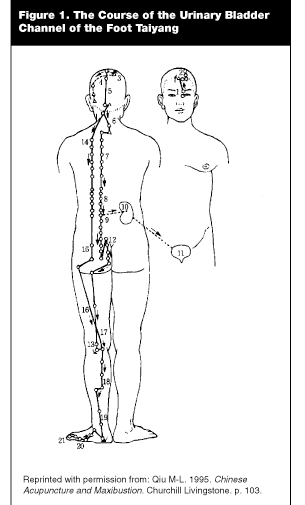 |
TCM was the exclusive form of health care in China until the turn of the 20th century, when the government welcomed a huge influx of western scientists and tried to outlaw TCM practice. Since the communist revolution 50 years ago, there has been an effort to integrate the practices of Eastern and Western medicine that currently exist side by side.
While the concepts of TCM are unfamiliar to those trained in the Western, analytical model of medicine, acupuncture and other forms of Chinese medicine have been gaining use and acceptance in the United States. American interest in TCM was aroused in 1971 after New York Times correspondent James Reston returned from China. While in China covering Nixon’s negotiations with the Chinese government, he had acute appendicitis. Upon his return, he wrote about the successful treatment of his post-appendectomy pain with acupuncture and the extensive use of acupuncture anesthesia that he was able to observe while there.16
Since the 1970s, the practice of acupuncture and TCM in the United States has increased dramatically. An estimated 3000 MDs and DOs use it in their practice, while more than 7000 nonphysician practitioners use acupuncture exclusively. The number of acupuncturists in this country is projected to double by the year 2005. The FDA estimates that between 9-12 million treatments are now performed annually.17 There are more than 70 schools of acupuncture and TCM in the United States, of which 32 are accredited by the National Accreditation Commission (NCCA). The accredited programs require at least 2 years of college for admission and provide 2200 hours of training to graduate. Physicians can receive a certificate from the American Association of Medical Acupuncture with only 200 hours of training. However, at least 2 years of formal training or 4 years of apprenticeship is required to sit for the national certification exam, which is required for licensure in most of the states that license nonphysician acupuncturists (34 states and Washington, DC). All states except New Mexico, however, allow physicians to practice acupuncture and only 14 require any formal training.
Clinical Practice
TCM diagnostic methods include extensive observation of the patient (ie, facial expressions, patterns of speech, and movement) and thoughtful listening to the patient’s experience of their symptoms. The rest of the diagnostic methods and diagnostic framework used by traditional Chinese practitioners may seem almost like hocus pocus to Western physicians. Diagnoses are made based on observations of the face and tongue and palpation of the abdomen and the radial pulse. The tongue is observed for variations in color, coating, and texture. The pulse is measured using 3 different locations and at 2 different depths lengthwise along the radial artery, with a total of 6 pulses measured on each hand. Practitioners experienced in pulse diagnosis will glean information about many systems of the body using those different positions. After all these assessments are made, a patient who we might diagnose with irritable bowel syndrome may be described as having "lung-liver disharmony." Another patient diagnosed with stagnant Qi might meet the clinical criteria for fibromyalgia in a Western framework. The prescribed treatment is then tailored based on all the variables found in each individual patient.
The therapeutics of TCM in the United States has centered largely around the use of acupuncture. The treatment modalities might include a specific course of acupuncture with different needle techniques, moxibustion (burning the herb artemesia vulgaris at the end of the acupuncture needle or directly on the acupuncture point), electroacupuncture, or acupressure. The basic premise of acupuncture’s efficacy in the TCM model is that by inserting a needle (or applying pressure or burning an herb) in a specific acupuncture point along the effected meridian, one can manipulate the flow of Qi in the desired direction. It is believed that the further the acupuncture point is from the affected area, the more powerful the effect of the treatment. When a needle is inserted, it may be manipulated or twirled to provoke a sensation named de qi. This sensation, the de qi, is often described as numb, tingly, or heavy and is felt by some to be essential for the therapeutic effect. In addition to acupuncture, there are other essential components of treatment that include herbal medicine and exercise, diet, and lifestyle change. There are some practitioners, especially in Asian countries who rely exclusively on these treatment modalities.
"Modern" or "medical acupuncture" is practiced as a therapy within a Western medical context in more conventional medical settings in the absence of the theoretical basis of TCM. Using a more conventional diagnostic framework, medical acupuncture will use the insertion of needles proximal to the location of the symptom to achieve relief (eg, inserting needles in the low back to treat low back pain). There are several theories used to support this therapy—all of which involve explanations based in Western science such as release of endorphins or alterations of the neurological pain pathways. Acupuncture practiced in this manner is rarely done in conjunction with other Eastern modalities such as herbal medicine or dietary change.
Efficacy and Safety
Of all the areas of CAM, evaluating the efficacy of TCM and acupuncture has proved to be one of the most challenging. While there is a tremendous amount of literature on acupuncture dating back many years, much of the work has been done in Asia and Europe and remains untranslated. In addition, most of the studies that have been done are small and poorly controlled. With the renewed interest in acupuncture in the Western world has come greater effort to proving its efficacy with randomized controlled trials of high quality and an increasing number of publications in English language medical journals. Subjecting this Eastern health care model to Western scientific standards has proved challenging for a variety of reasons. The standard for good treatment in the TCM model is individualization of therapy. The diagnostic categories we use have no meaning in their framework and vice versa. It has been difficult to determine the most appropriate control group: placebo, sham needling, or comparison therapy. Blinding of both acupuncturist and patient is problematic.
In November 1997, the NIH held a consensus conference on acupuncture that concluded, "There is clear evidence that needle acupuncture is effective for postoperative and chemotherapy induced nausea of pregnancy and postoperative dental pain."18 This group also stated that there was promising but inconclusive evidence to support the use of acupuncture for several other medical conditions (back pain, asthma, headache, dysmenorrhea, addictive disorders, stroke rehabilitation, fibromyalgia, tennis elbow, carpal tunnel, osteoarthritis, and myofacial pain).
The literature supporting acupuncture as an anti-emetic is unique and by far the strongest. Stimulation of a single acupuncture point (pericardium 6) on the anterior aspect of the wrist has been found to reduce the incidence and severity of nausea and vomiting and the need for anti-emetics in pregnant patients and patients receiving anesthesia and chemotherapy.19 It is an example of standardized vs. individualized acupuncture therapy.
The use of acupuncture for addictive disorders is fairly widespread. Auricular acupuncture for heroin and cocaine addiction was developed by Dr. Michael Smith at Lincoln Hospital in Bronx, NY, and has been used worldwide. Bullock’s work using acupuncture to prevent relapse in alcohol dependence is well respected.20 However, most of the other studies on addiction treatment are not done as rigorously as these. So, while the use of acupuncture has been widely accepted in the treatment of substance abuse, there remains controversy over whether its efficacy has been proven. The data looking at acupuncture for nicotine addiction in smoking cessation have been largely negative.
With the exception of postoperative dental pain, the literature evaluating the use of acupuncture for various types of pain has been more mixed. While there are some promising studies supporting the use of acupuncture for headache and low back pain, there are only a few of varying quality looking at other pain syndromes.21 In general, the methodology for most of the studies differs so greatly as to prevent any meaningful meta-analysis.
Another promising area is the use of acupuncture to improve outcomes in the rehabilitation of victims of stroke. Again, while the studies have been of varying quality, acupuncture has been shown to be consistently better than standard treatment alone. It has also been shown to reduce the damage to motor pathways on CT scan as compared to a sham acupuncture group.
With regard to the safety of acupuncture, it is useful to clarify which of the adverse events reported in the literature are due to negligence on the part of the practitioner (pneumothorax, transmission of viral hepatitis, cardiac injury) and which are adverse reactions observed in standard practice. One hundred ninety-three adverse events were reported worldwide from 1981 to 1994.22 A small percentage of those events were serious and all of those were deemed due to inappropriate or negligent practice. A recent study in Japan that monitored for adverse events found that the most common events were tiredness (8% of patients), drowsiness (3%), minor bleeding on withdrawal of the needle (2.6%), and itching of the insertion sites (1%).
With increased support from the NIH and increased interest in this area, there has been a steady increase in the number of and improvement in the methodology of studies on acupuncture. This will hopefully help to clarify which medical indications will warrant treatment with acupuncture.
Chiropractic
Background
Spinal manipulation as a technique for treating musculoskeletal pain has been documented as far back as ancient China and Greece. The profession of chiropractic was developed in 1895 by Daniel David Palmer, a grocer and magnetic healer in Davenport, Iowa (see Figure 2). Chiropractic (Greek for done by hand) was founded on the principle that joint dysfunction and malaignment of the spine may play a significant role in heath and disease. Spinal manipulation, therefore, can correct these problems and facilitate the return of health and equilibrium. Early in its history, the profession experienced a theological split between two factions. While the "straight" chiropractors insisted on remaining true to the original theories proposed by Palmer, the "mixers" felt that it was more realistic to incorporate other theories of health and disease, such as infection, which were being adopted by the scientific community of the time. This lack of uniformity within the field of chiropractic continues today.
 |
With 60,000 practicing chiropractors, they are the third largest group of health care providers in the United States after physicians and dentists. They are the largest group of CAM providers in the United States and the fastest growing. Their ranks are projected to nearly double in size by the year 2010. One in 3 persons with low back pain see a chiropractor with 192 million patient visits per year. This figure has doubled in the past 15-20 years. Most patients self-refer, with only 3% of chiropractic patients being referred by MDs. Multiple studies have shown that while the costs might be greater, patient satisfaction is higher in those seeing chiropractors for their back pain as compared to primary care providers. Most insurance carriers, including Medicare, cover chiropractic. Some plans now require a referral from a MD for coverage of the service.
There are 17 accredited colleges of chiropractic in the United States, with a total of 2000 graduates per year. Two years of college are required for admission and the curriculum takes 5 years to complete with 4000 hours of basic science instruction and 1000 hours of clinical internship required for graduation. The National Board of Chiropractic Examiners administers a 3-part licensing exam. Most states also require a practical exam for state licensure. All 50 states require licensure but individual states vary with regard to their permitted scope of practice. For example, all states allow a spine-focused history and physical exam, x-rays, and spinal manipulation, and 90% also permit a more general history and physical, health advice, and ordering tests (ranging from bloodwork to CT scans). It is advisable for any physician to find out from their own state’s licensing body what their state allows.
Clinical Practice
As mentioned above, the field of chiropractic is not unified in the philosophies that it promotes. This manifests itself in varying practice styles and practices among different chiropractors. Before making a chiropractic referral, it is useful to find out what you and your patient can expect from the practitioner (see Table 2). There are several areas of difference that, once aware of them, can aide the referring physician. While some chiropractors limit their practice to spinal manipulation (the "crackers"), others may use any variety of other therapeutic interventions including exercise, dietary changes, dietary, and nutritional supplements. While some promote the idea of routine spinal manipulation on an ongoing basis ("maintenance therapy"), others feel that it is inappropriate and focus on successfully treating the presenting problem. While some will tout the use of chiropractic for any and all physical problems, others will use it almost exclusively for musculoskeletal problems and perhaps for other problems for which chiropractic has been proven efficacious. There is a faction within chiropractic that publicly promotes staunch views against routine vaccination for both children and adults.
| Table 2. What to Ask a Chiropractor |
| • What therapies do you incorporate into your practice? |
| • Do you prescribe any supplements? If so, what kind? |
| • Do you believe in the usefulness of "maintenance therapy"? Do you recommend it for your patients? |
| • What problems do you feel comfortable treating? What would be a welcomed referral? |
Efficacy
The literature for chiropractic has undoubtedly been the most scrutinized of all the CAM fields. Chiropractic research has faced the same challenge as other therapies that involve strong doctor-patient interactions and "hands-on" individualized therapy with criticism of its methodology. The techniques that have been most widely studied include spinal manipulation therapy and spinal mobilization therapy. Spinal manipulation therapy is defined as the application of high-velocity, low-amplitude manual thrusts to the spinal joints slightly beyond the passive range of joint motion. Spinal mobilization therapy is defined as the application of manual force to the spinal joints within the passive range of joint motion that does not involve a thrust. In most of the literature, the two techniques are discussed together simply as spinal manipulation.
An expert panel assembled for the RAND Corporation critically reviewed the literature on the efficacy of spinal manipulation for acute and chronic low back pain, neck pain, and headache. Although several of the studies had poor research design, the consensus of the panel was that for acute, uncomplicated low back pain, manipulation hastens recovery and decreases work time lost. Its long-term effect either in preventing chronic low back pain or a recurrence of acute low back pain is unknown at present.23 Two more recent reviews24,25 concluded that there was limited evidence to suggest that spinal manipulation is better than placebo, physical therapy, and exercise in the treatment of acute low back pain. These same authors, however, felt that there was strong evidence of efficacy in the treatment of chronic low back pain. The US Agency for Health Care Policy and Research (AHCPR)26 and its British equivalent, the Clinical Standards Advisory Group (CSAG),27 have both suggested that spinal manipulation is better documented as an effective treatment for acute mechanical low back pain than any other save nonsteriodal anti-inflammatory drugs (NSAIDs).
There are far fewer studies evaluating the efficacy of cervical spinal manipulation for the treatment of neck pain. There have been at least 10 randomized, controlled trials and one meta-analysis. A literature review by the RAND team concluded that the results supported but did not prove that cervical manipulation provides short-term benefit to patients with neck pain.28 The Quebec Task Force on Whiplash-Associated Disorders stated that spinal manipulation had weak evidence and recommended that a short regimen may be used for whiplash associated disorders.29
While there are some promising data, there are not enough methodologically sound studies on the use of spinal manipulation for headache to draw any firm conclusions. The same is true for several other nonmusculoskeletal disorders including primary dysmenorrhea and asthma.
Safety
One of the myths about chiropractic is that spinal manipulation, especially cervical, is actually dangerous. In fact, the estimated risk of a major complication from cervical spine manipulation is 6.39 per 10 million manipulations and 1 per 100 million manipulations for lumbar spine manipulation. This compares favorably to the other forms of therapy for the same conditions. The rate of serious complications for spinal surgeries is 15.6 per 1000 surgeries and 3.2 per 1000 subjects for NSAIDs.28 One review reported 135 case reports of serious complications, including 18 deaths, from spinal manipulation. Many of those, however, can be attributed to the use of chiropractic in inadvisable situations.28 Contraindications to manipulative therapy include: severe rheumatoid arthritis with ligamentous laxity, bleeding disorders or anticoagulation therapy, and conditions that render the bony structures susceptible to trauma such as acute fractures, bone tumors, and severe osteoporosis. It is not unusual for patients to report benign effects from manipulation such as increase in symptoms, myalgias, and fatigue. These effects are usually transient and need not prohibit further manipulation treatments.
Homeopathy
Background: Use in the United States
The field of homeopathy was developed 200 years ago by the German physician Samuel Hahneman, MD (1755-1843). He was no longer practicing medicine at the time but was working as a translator of medical texts. He became interested in the use of Peruvian bark or Cinchona (the source of quinine) for the treatment of malaria, and he noticed that the symptoms of cinchona poisoning were similar to the symptoms of malaria. After ingesting a therapeutic dose, he indeed felt like he had malaria. He then went on to experiment with and record the detailed experiences of normal healthy people to some number of substances, which he called "provings." From these experiments, he developed the three major tenets of homeopathy (see Table 3). The law of similars proposes that patients with particular signs or symptoms can be cured if given a drug that produces these same symptoms in a healthy individual. The principle of potentization holds that remedies gain greater biological activity if they are repeatedly diluted and shaken ("succussion") between each dilution. In preparing a remedy, substances are often diluted beyond Avagadro’s number or beyond the point where any of the original molecules remain. The theory is that the solution "remembers" the original substance and is altered by it in a way that retains biological activity. In addition, homeopathy contends that in these tiny amounts, these substances can stimulate the body to heal itself as in the immunological model of vaccines, where in larger amounts they could cause the problem itself. The totality of symptoms describes the approach of applying homeopathy individually to any given patient. Homeopathy teaches that illness is primarily a disturbance of the "vital force" and will manifest itself uniquely in any given individual with a different set of physical, mental, and emotional symptoms.
| Table 3. Three Tenets of Homeopathy |
| • Law of similars or "like cures like" |
| • Potentization-dilutions increase potency of the remedy |
| • Totality of Symptoms-Individualized therapy of the whole person |
Homeopathy grew rapidly in the United States in the beginning of the 19th century. The first school of homeopathy in the United States opened in 1835. Despite its lack of acceptance by conventional physicians at the time, its use flourished among the people who often chose homeopathic remedies over the therapies offered by physicians at that time (ie, leeches and blood letting). Many schools and hospitals were opened during the 1800s, and homeopathy’s popularity spread to Europe. However, the AMA took greater control over health care with the Flexner Report in 1914 and convinced many state legislatures to license only physicians to practice medicine. Homeopathic schools and hospitals either closed or conformed to the conventional model. The practice of homeopathy was all but lost until the 1980s when it began to flourish once again on the tide of the growing self-care and the alternative medicine movement.
Homeopathy is currently estimated to be used by 3.4% of the population in the United States and practiced by 2500 MDs and 4000 nonphysician practitioners.2 Sales of homeopathic remedies have increased by 1000% since the 1980s with $250 million in sales in 1996 in the United States and $1.15 billion in sales worldwide.30 Homeopathic remedies are sold without prescription and are not regulated by the FDA due to an exemption negotiated in 1938.
Practitioners of homeopathy can be licensed in 4 states (Arizona, Connecticut, Nevada, Washington). Certification for physicians is offered by the American Board of Homeotherapeutics and involves course training, 3 years of practice treating cases, preparation of case reports on patients, and written and oral examinations. There are a multitude of courses offered to the public, some of which are mail order, which include a huge variety of preparation to practice with no real standardization for training.
Clinical Practice
The clinical practice of homeopathy is unique from other fields of both conventional and alternative medicine in that diagnosis and therapy is based entirely on history. No physical examination is done. To determine the appropriate remedy, the practitioner will engage in "case-taking." This involves both observation of the patient (speech, posture, dress, facial expression, etc) and an exquisitely detailed description of the symptoms. The symptoms that are most specific and unique to the case are then looked up in The Homeopathic Pharmacopoeia of the United States. A remedy that is most common to the group of symptoms is chosen taking into account the characteristics of the patient. This method of prescribing is called classical homeopathy. For more acute and less complicated problems (ie, traumatic injuries), there are some more universally prescribed remedies. For example, Arnica is a very popular remedy for sprains and strains. Using a single remedy in all patients with the same symptom or diagnosis is called clinical homeopathy. Homeopathic remedies are of plant, mineral, and animal origin and are diluted and dropped onto lactose pellets. The pellets are dissolved in the mouth. Depending on the acute vs. chronic nature of the illness, the remedy may be taken only once or repeatedly over the course of weeks.
Efficacy
It is only in the last 15 years or so that any methodologically sound trials have been done to evaluate homeopathy. The tradition of homeopathy views Hahnemann’s system of provings as the core research of the field. In 1988, there was a highly controversial study published in the journal Nature that demonstrated degranulation of human basophils by dilute solutions (up to 10-120) of IgE antibodies.31 Attempts to replicate these findings have seen mixed results.
There have been several meta-analyses done trying to evaluate the efficacy of homeopathy in general when used to treat a variety of conditions. Kleijnen32 concluded that the methodology of these studies was of such poor quality that no real conclusions could be drawn. Linde33 combined the data of 89 studies and found that while there was insufficient evidence that homeopathy is clearly efficacious for any single clinical condition, the evidence was "not compatible with the hypothesis that the clinical effects are completely due to placebo." An updated review by 2 of the same authors included 32 trials looking only at classical homeopathy. While they found that the methodological quality was still variable, it was markedly improved from their previous review. They concluded that while overall homeopathy was statistically significant to placebo, the methodologically better trials had less positive results making the case for homeopathy less convincing.34 Some of the more promising areas of research are in the use of homeopathy for allergy symptoms, asthma, and diarrhea in children. Safety is not considered to be an issue given the "homeopathic doses" used.35,36
Massage Therapy
Background
Therapeutic massage has been used in models of health and wellness for thousands of years as documented in oriental and Ayurvedic traditions, biblical references, and the folklore of many populations.37 The philosophy of massage therapy is based on several principles. The benefits of massage therapy are affected by enhancing the body’s ability to go through the phases involved in restoration and normalization of anatomic and physiologic function. Additionally, psychological benefits occur subjectively and individually in response to massage therapy with secondary effects that influence sensation and pain perception.
The first written medical reference to massage therapy dates to 2000 bc in the writings of Hippocrates. Swedish massage, still the most commonly technique used in Western settings, was developed in the late 1700s and ultimately led to the development of the field of physical therapy. Used in hospitals, medical offices, and sanitaria in the United States until the turn of the century, massage was often a first-line approach in the treatment of disease and dysfunction. With the emergence of the practice and profession of physical therapy and modern pharmaceuticals, the practice of massage in the Western medical model faded. It then returned to Western culture in red light districts and as fronts for illicit sexual activity. Massage therapy was reintroduced into the United States from Sweden by the Taylor brothers.37 Since the early 1960s, the use of massage as a therapeutic modality has gained in popularity. In one nationwide survey, massage therapy was found to be the third most used method of alternative health care after relaxation techniques and herbal medicine.2 There are an estimated 50,000 licensed massage therapists in the United States, delivering 45 million hours of massage therapy per year. Currently, 20,000 therapists are certified by the National Board for Therapeutic Massage, which administers a national certification exam. Licensure for massage therapy exists in only 24 states and the District of Columbia. Most states providing licensure require 500 hours of training from one of the 60 school accredited by the American Massage Therapy Association.
Clinical Practice
In both regulated and unregulated states, the scope of practice of massage therapists is not uniformly defined. Some states consider massage a health care modality, while others consider it a personal care service. Just as the regulations governing the practice of massage therapy varies widely, the scope of practice varies from therapist to therapist depending on setting, training, and interest. Several primary categories of massage therapy exist. The most popular are European massage techniques (Swedish massage), which involve long gliding strokes (effleurage), kneading (petrissage), striking (tapotement), and vibration (shaking). There are also deeper tissue techniques (Rolfing), sports massage, neuromuscular massage, and manual lymph drainage.
Efficacy and Safety
Until recently, there was little to no quality research on massage in US medical journals. Most of the research had been done in the former USSR and East Germany and remains untranslated. For the past several years, research done at the Touch Therapy Institute at the University of Miami has drastically changed this situation. Tiffany Fields, the director of the institute, has produced some impressive data using massage therapy in children. There are several randomized, controlled studies showing that massage therapy done on premature babies in the neonatal intensive care unit resulted in significantly greater weight gain, earlier discharge, and cost savings per baby as compared to controls. These babies were also found to have increased gastrin and insulin levels that are theorized to have resulted in improved absorption of food.38 A more recent study by this group has shown that asthmatic children who were massaged by their parents for 20 minutes each night for 1 month had significantly improved pulmonary function tests when compared to their counterparts who were randomized to relaxation therapy. The group receiving massage was also found to have lower cortisol levels and behavioral anxiety.39 In addition to the work done at the University of Miami, we can look forward to more research in this area as the NCCAM has granted massage therapy one of the largest block of grants given to any field of alternative health care.
Discussing Alternative Medicine with Patients
As PCPs, our patients look to us for advice about their health care. With the recent emergence of CAM onto the health-care scene, these requests will ever increasingly be about CAM (see Table 4). As we know from the literature, many of our patients are already using CAM, and it is also our obligation to ask all of our patients if they are visiting alternative providers or using some form of CAM on their own. Patients might be reluctant to tell, expecting their physician to disapprove. It is important to ask with a nonjudgmental attitude and to show interest (giving "permission" to discuss the issue). It might be helpful for practitioners to become familiar with local patterns of use and more frequently visited alternative providers. As with most other subjects in medicine, it is key to acknowledge the limits of your knowledge without embarrassment. When disagreements over how to proceed occur and negotiation fails to produce a consensus, agree to disagree without condescension. If patients do decide to go ahead with an alternative therapy, be frank about your level of involvement, be comfortable with whatever promises you make or requests you deny, and avoid an unintended message of abandonment.
| Table 4. Discussing Alternative Medicine with Patients |
| • Ask with nonjudgmental attitude, show interest |
| • Give "permission" to discuss |
| • Become familiar with local patterns of use |
| • Acknowledge the limits of your knowledge |
| • Agree to disagree without condescension |
| • Be frank about your level of involvement |
| • Avoid an unintended message of abandonment |
Evaluating/Making Referrals
After careful consideration of the evidence, some practitioners may find it useful to make referrals to CAM providers for a variety of medical problems, especially those problems for which conventional medicine has no easy or effective treatment (ie, chronic fatigue syndrome, fibromyalgia, back pain, insomnia, etc). The best way to find practitioners in your community to whom you may want to refer is to ask your colleagues and patients. Another way to find practitioners in your area is to contact the national organization that governs certification or education of that field (see Table 5). It may also be useful to help the patient evaluate a practitioner that the patient may already be seeing. You or the patient should verify their credentials with whatever state agency governs their licensing and find out how much the therapy is likely to cost if it is not covered by the patient’s insurance plan. It should be clear to both you and the patient what can be expected throughout the course of treatment during an office visit and how long the therapy is expected to last. There are some steps that the patient can take to evaluate the usefulness of the therapy. You can suggest that they keep a symptom diary to track their progress and monitor for side effects. A conversation with the practitioner might prove educational to the PCP and useful for the patient. At some point during the course of the therapy, there should be some follow-up with the physician to help the patient evaluate how things are going and to review the treatment plan. Throughout the entire process, it is essential to document all conversations with both the patient and the alternative provider.
| Table 5. Information Resources for State Licensing |
| Chiropractic National Board of Chiropractic Examiners 901 54th Avenue Greely, CO 80634 970-356-9100 www.sni.net/nbce
Homeopathy
Acupuncture
American Academy of Medical Acupuncture
Massage Therapy |
Summary
The reality in primary care is that many of our patients are using CAM therapies and we probably don’t know about it. It is the obligation of all PCPs to ask the questions and gather the relevant information. Each physician, however, needs to decide for himself or herself what role they are comfortable playing for their patients with regard to CAM. The information is out there for those who wish to be educated. The CAM providers are out there and willing to communicate for those who wish to refer. The health care industry is responding rapidly and probably one of the only things we can know for sure is that CAM is here to stay.
References
1. Eisenberg DM, et al. Unconventional medicine in the United States-prevalence cost and patterns of use. N Engl J Med 1993;328:246-252.
2. Eisenberg DM, et al. Trends in alternative medicine use in the U.S. 1990-1997. JAMA 1990;280:1569-1575.
3. Hughes EF. Alternative medicine in family practice: It’s already mainstream. Fam Pract Recertification 1997;19:24-44.
4. The Integrator for the Business of Alternative Medicine. Sacramento, Calif: Landmark Health Care; 1999:3.
5. Reilly D. The evidence for homeopathy. Paper presented at: Meeting of Grampian Health Board; March 2000; Grampian, Scotland.
6. Astin JA. Why patients use alternative medicine. JAMA 1998; 279:1548-1553.
7. Pelletier KR, Astin JA, Haskell WL. Current trends in the integration and reimbursement of complementary and alternative medicine by managed care organizations and insurance providers. Am J Health Promotion 1999;14:125-133.
8. Wetzel MS, Eisenberg DM, Kaptchuk TJ. Courses involving complementary and alternative medicine at US medical schools. JAMA 1998;280:784-787.
9. Daley D, Eisenberg D. Alternative Medicine: Implications for Clinical Practice [curriculum]. Boston, Mass: Department of Continuing Education, Harvard Medical School; March 30, 1995.
10. Carlston M, Stuart MR, Jonas W. Alternative medicine instruction in medical schools and family practice residency programs. Fam Med 1997;29:559-562.
11. Milan FB, et al. Teaching residents about complementary and alternative medicine in the U.S. Journal of Global Information Management 1998;13:562-567.
12. Verhoef MJ, Sutherland LR. Alternative medicine and general practitioners. Can Fam Physician 1995;41:1005-1011.
13. Himmel W, et al. Complementary medicine: Are patients’ expectations being met by their general practitioners? Br J Gen Pract 1993;43:232-235.
14. Astin JA, et al. A review of the incorporation of complementary and alternative medicine by mainstream physicians. Arch Intern Med 1998;158:2305-2310.
15. Gordon NP, et al. Use of and interest in alternative therapies among adult primary care clinicians and adult members in a large health maintenance organization. West J Med 1998;169:153-161.
16. Moyers B. Healing and the Mind. New York, NY: Doubleday Publications; 1993.
17. Lytle CD. An Overview of Acupuncture. Washington, DC: Center for Devices and Radiological Health, US Dept. of Health and Human Services; May 1993.
18. NIH Consensus Conference on Acupuncture. JAMA 1998;280: 1518-1524.
19. Vickers AJ. Can acupuncture have specific effects on health? A systematic review of acupuncture antiemesis trials. J R Soc Med 1996;89:303-311.
20. Bullock ML, et al. Controlled trial of acupuncture for severe recidivist alcoholism. Lancet 1989:8659:1435-1439.
21. Mayer DJ. Acupuncture: An evidence-based review of the clinical literature. Ann Rev Med 2000;51:49-63.
22. Norheim AJ. Adverse effects of acupuncture. A study of the literature for the years 1981-1994. J Altern Complement Med 1996;2:291-297.
23. Shekelle PG, et al. The Appropriateness of Spinal Manipulation for Low-back Pain: Project Overview and Literature Review. Santa Monica, Calif: RAND; 1992.
24. van Tulder MW, et al. Conservative treatment of acute and chronic nonspecific low back pain. Spine 1997;22:2128.
25. Bronfort G. Spinal manipulation: Current state of research and its indications. Neurol Clin 1999;17:91-111.
26. Bigos S, et al. Acute Low Back Pain Problems in Adults. Clinical Practice Guideline, No. 14. Rockville, Md: Agency for Health Care Policy and Research, Public Health Service, US Dept. of Health and Human Services; December 1994. AHCPR Publication 95-0642.
27. Rosen M, et al. Management Guidelines for Back Pain Appendix B in Report of a Clinical Standards Advisory Group Committee on Back Pain (CSAG). London, England: Her Majesty’s Stationary Office; 1994.
28. Coulter ID. Efficacy and risks of chiropractic manipulation: What does the evidence suggest? Integr Med 1998;1:61-66.
29. Cassidy JD, et al. Scientific monograph of the Quebec task force on whiplash-associated disorders. Spine 1995;20(8S)1S-74S.
30. Jacobs J, et al. Patient characteristics and practice patterns of physicians using Homeopathy. Arch Fam Med 1998;7:537-540.
31. Davenas E, et al. Human basophil degranulation triggered by very dilute antiserum against IgE. Nature 1998;333:816-818.
32. Keijnen J, et al. Clinical trials of homeopathy. BMJ 1991;302:316-323.
33. Linde K, et al. Are the clinical effects of homeopathy placebo effects? A meta-analysis of placebo-controlled trials. Lancet 1997;350:834-843.
34. Linde K, Melchart D. Randomized controlled trials of individualized homeopathy: A state of the art review. J Altern Complement Med 1998;4:371-388.
35. Jacobs J, et al. Treatment of acute childhood diarrhea with homeopathic medicine. Pediatrics 1994;93:719-725.
36. Reilly DT, et al. Is evidence for homeopathy reproducible? Lancet 1994;344:1601-1606.
37. US Government Printing Office. Alternative Medicine; Expanding Medical Horizons. A Report to the NIH on Alternative Medical Systems and Practices in the United States. Washington, DC: US Government Printing Office. S/N 017-040-00537-7.
38. Scafidi F, Field T. Massage stimulates growing in pre-term infants: A replication. Infant Behavior and Development 1993; 13:167-188.
39. Field T, et al. Children with asthma have improved pulmonary function after massage therapy. J Pediatr 1998;132:854-858.
Recommended Resources
Books
1. US Government Printing Office. Alternative Medicine; Expanding Medical Horizons. A Report to the NIH on Alternative Medical Systems and Practices in the United States. Washington, DC: US Government Printing Office. S/N 017-040-00537-7. (Best inexpensive resource for the health provider, costs $25 and can be ordered at (205) 512-1800, the Superintendent of Documents.)
2. Micozzi MS. Fundamentals of Complementary and Alternative Medicine. New York, NY: Churchill Livingstone; 1996. (In depth discussions of the history and ideology of each modality.)
3. Beinfeld H, et al. Between Heaven and Earth: A Guide to Chinese Medicine. New York, NY: Ballantine Books; 1991. (Easy and pleasurable to read. Has nice explanations and comparisons to Western medical system.)
4. Kaptchuk T. The Web That Has No Weaver: Understanding Chinese Medicine. New York, NY: Congdon and Weed; 2000.
5. Spencer JW, Jacobs JJ. Complementary and Alternative Medicine: An Evidence Based Approach. St. Louis, Mo: Mosby-Yearbook; 1999.
Miscellaneous
1. NCCAM Clearinghouse, P.O. Box 8218, Silver Spring, MD 20907-8218, 1-888-644-6226 http://nccam.nih.gov.
Web Sites
1. NCCAM (see above).
2. cpmcnet.columbia.edu/dept/rosenthal/ (information about medical school courses in CAM as well as CME available).
3. [email protected] (large acupuncture bibliography).
4. http://www.miami.edu/touch-research.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
