OIG OKs cost-sharing arrangement for hospital
OIG OKs cost-sharing arrangement for hospital
Procedure changes maintain quality
Reversing a policy it had consistently pursued for years, the Health and Human Services Office of Inspector General (OIG) has given the green light to Saint Joseph’s Hospital of Atlanta to reward a cardiac surgery group for saving money during heart surgery. Under the proposal, the hospital would share up to half the money the surgeons saved. This ruling was not an overnight success. Both the hospital and the health care consulting firm that won over OIG have been involved with this issue for years.
"Saint Joe’s was one of the first four hospitals to participate in a program in 1991 called the HCFA [Health Care Financing Administration] Coronary Artery Bypass Graft demonstration project," recalls Marie Weissman, MB, MSW, the hospital’s vice president of operations. The project protocol called for the hospitals to receive a single payment for each Medicare patient, from which it had to compensate all physicians involved and cover all costs. "For the first time, we were able to economically align hospitals and physicians," notes Weissman, who adds that this approach saved Medicare $15 million "without any adverse impact on mortality and morbidity."
For Joane H. Goodroe, RN, MBA, president of Goodroe Healthcare Solutions, LLC, in Atlanta, cutting costs while maintaining quality has been an overriding concern since she founded her consulting and software company eight years ago. "When we began working throughout the country, we found that if you looked at 100 different cardiac surgery practices or cardiologists, you’d find at least that many differences in the way they did the same procedure. It became obvious to me that, in this country, we really have not studied the techniques of how physicians perform procedures," notes Goodroe. "As we began to collect data, we found practice patterns so varied that, although the majority of them resulted in excellent outcomes, there was a huge difference in the cost of providing services."
Goodroe and her firm have been seeking to find ways for hospitals to engage physicians in the tremendous amount of work and effort required to re-examine and relearn how to do their practices. "We wanted to find not only the best quality but the best practice from a cost standpoint," she explains.
The governmental hurdle
Goodroe’s company has developed software capable of measuring cost and quality, but the OIG has been staunchly opposed to any gainsharing programs, although they would clearly incentivize physicians to save money. "From the government’s perspective, they have a responsibility to make sure care is not withheld from a patient, and the laws in place are clear about that," says Goodroe. "That, of course, was never our intention, but the OIG needed to make sure there were safeguards in place."
Typically, she notes, previous plans proposed using a macro cost-accounting system to reward surgeons for reduced costs. "This was not specific enough," she points out. "The government felt it couldn’t sanction such an approach because it couldn’t guarantee what would happen with the patients."
Two other pieces of the puzzle were important to OIG, says Goodroe:
- A third party analyzes the data to ensure that quality indicators are maintained using national benchmarks.
- Patients are informed of the program.
The information Goodroe’s software reports is specific, highly measurable, and can be tracked specifically to what quality and cost component are in a particular initiative. "For example," she says, "one of the big areas we looked at is rewarding somebody for a substitution. Oftentimes, surgeons have a technical way of doing something that is very expensive."
By reviewing existing best practices, Goodroe has discovered substitutions for procedures as simple as the way sutures are used. "A very costly way to use them, and one that’s been used quite a bit in this country, is to use a new suture for every new area you sew. A more cost-effective way of doing it is to look and see if a suture you already have on the table is appropriate to use in another area."
Getting the job done
This may not sound like an impressive strategy for cost saving, but Goodroe says her benchmarking studies on coronary artery bypass surgery have found as much as a $700 differential per case depending on the way sutures are used. From a broader perspective, "We have always found in every place we’ve been there is more than $1,000 per case that can be saved very easily," she asserts.
Goodroe’s group came up with a template proposal and started meeting with the government three years ago. At that time, a third player had entered the picture: Peachtree Cardiovascular and Thoracic Surgeons, PC, a local firm and a Goodroe client. Headed by Doug Murphy, MD, "They were kind enough to work with us and Saint Joseph’s when we decided to submit something formal," says Goodroe.
Another part of the challenge was that HCFA was forced to abandon its successful program in 1997 when the Y2K scare arose. "HCFA reassigned all those folks," Weissman recalls. "So with the assistance of Goodroe Healthcare Solutions, Saint Joe’s submitted a formal request to OIG for an advisory opinion to continue a gainsharing program. At first, they said they would not condone any gainsharing programs."
Goodroe continued to have discussions with OIG and "modified and tweaked" their request. After an 18-month-long process, the approved version was formally submitted in November 1999 and approved officially on Jan. 11, 2001. After such a long wait, "It was a nice surprise," says Weissman.
Sharing the wealth
As a hospital executive, Weissman has a keen understanding of the dynamics at work in health care reimbursement, and of the arguments in favor of gainsharing. "I believe there’s a fundamental tension in the way individuals who provide health care are reimbursed," she asserts. "Physician reimbursement is oftentimes tied to doing more for the patient. On the other hand, because of DRGs, hospitals are rewarded by managing the cost of the patient’s care. That creates the fundamental tension. Add to that the fact that reimbursement for hospitals and physicians have been significantly decreased, and that heightens the tension."
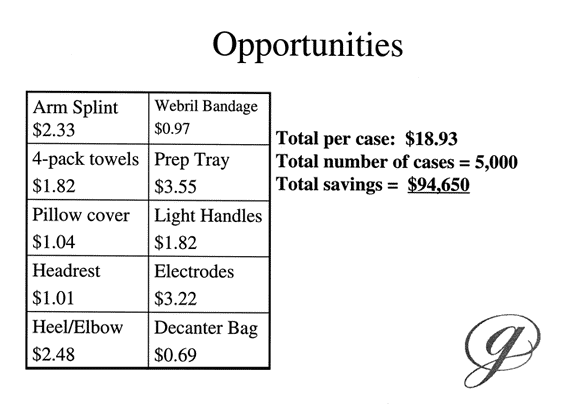
Weissman adds that there are known ways to decrease the cost of care and improve outcomes by eliminating unnecessary and/or inappropriate care. "We also can decrease cost by changing the way we do things," she says. "Sometimes, that requires an investment on the part of the physicians — learning new techniques they might adopt or participating in committee meetings with other caregivers. This requires more time, which takes money away from their practice. Gainsharing is a mechanism that tries to address those issues and minimize the tension by aligning the hospital and the physician in a single economic pool." (See example of Goodroe’s cost-saving opportunities, below.)
|
|
|
Source: Joane H. Goodroe, RN, MBA, President, Goodroe Healthcare Solutions, LLC, Atlanta. |
For her part, Goodroe says this focus on quality and savings in the surgical suite is long overdue. "What people focus on over and over are things that happen outside of surgery, but how can you standardize the aftercare if you don’t [standardize] the way you do surgery?" she argues.
For information, contact:
• Joane H. Goodroe, President, Goodroe Healthcare Solutions, LLC, 100 Crescent Centre Parkway, Suite 720, Tucker, GA 30084. Telephone: (770) 938-9686. E-mail: [email protected].
• Marie Weissman, Vice President for Operations, Saint Joseph’s Hospital of Atlanta, 5665 Peachtree Dunwoody Road, Atlanta, GA 30342. Telephone: (404) 851-7001. Fax 404-851-7339.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.