Special Feature: Electrocardiographic Electrode Misconnection
Electrocardiographic Electrode Misconnection
By Richard A. Harrigan, MD
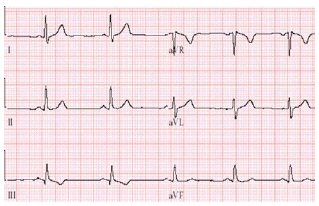
The adage "the best chest x-ray is an old chest x-ray" can be extended to the world of electrocardiography. With the myriad and subtle changes that may occur on the 12-lead surface electrocardiogram (ECG), at times the emergency physician’s (EP) best ally is an old tracing for comparison. Our residents, when asked to interpret an ECG, often will say, "It’s unchanged from the last one," rather than give a detailed interpretation, especially if the ECG is not stone-cold normal. Moreover, ECG changes plus a history of chest pain or an anginal equivalent invariably spells admission. Keeping all this in mind, the EP should be wary and knowledgeable of the changes associated with ECG limb electrode misconnection—inadvertently switching the placement of electrodes on the extremities of the patient. Such changes are, in most cases, predictably abnormal and should be considered when the EP is confronted with ECG changes confined to the limb leads. The circumstances surrounding the case depicted in Figure 1 led one EP initially to recommend admission and cardiology consultation. In this case, the ECG "changes" were due to limb electrode reversal. (See Figure 2.)
|
Figure 2. Correction of RA/LA Electrode Reversal
Limb leads from same patient as in Figure 1, |
Manifestations of Limb Electrode Reversal
There are many possible ways to inadvertently misconnect the four limb electrodes when performing a 12-lead ECG; usually such mistakes involve confusing the right and left sides or switching upper extremity and lower extremity electrodes on the same side. This discussion will be limited to the manifestations of the most common limb electrode reversal1,2 —right arm (RA) and left arm (LA) (See Figure 1 and Figure 2.)—as well as other commonly encountered misconnections: right leg (RL) / left leg (LL), RA/RL, and LA/LL. Other less common misconnections (e.g., RA/LL; LA/RL; misconnections involving three, or all four, electrodes), although rare, would result in bizarre tracings that should lead the EP to question the validity of the tracing and repeat the ECG. An understanding of the manifestations of limb electrode reversal begins with a review of the vector polarity of Einthoven’s triangle (leads I, II, and III) and the augmented limb leads (aVR, aVL, and aVF). (See Figure 3.)
|
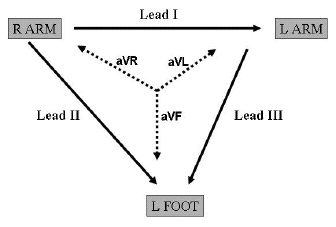
Figure 3. Standard and Augmented Limb Leads
Solid arrows depict leads I, II, and III, with arrowheads |
RA/LA Electrode Reversal. This limb electrode misconnection results in a change in appearance of all limb leads except aVF, and thus should be fairly easily suspected. The key change is an inverted P-QRS-T in lead I, due to the fact that the vector in that lead is reversed. (See Figure 1, Figure 2, and Figure 3.) Since the RA and LA electrodes are flipped, the ECG displays lead II as III (and vice versa), and displays lead aVR as aVL (and vice versa). (See Figure 1, Figure 2, and Figure 3.) Thus, a second key to detecting RA/LA electrode reversal is a normal appearing P-QRS-T in lead aVR. Since by convention the positive pole of lead aVR lies in the upper rightward quadrant of extreme axis deviation (virtually 180° opposite to the major vector of cardiac depolarization, which is in most cases into the lower leftward, or normal, axis quadrant), the P-QRS-T in lead aVR normally is upside down. Thus, a normal-appearing complex in that lead is a clue to possible limb electrode misconnection.
It should be remembered that a pattern similar to RA/LA reversal also is seen in patients with dextrocardia. Whereas dextrocardia will yield a negative P-QRS-T in lead I, it also will feature progressively smaller QRS complexes when moving from precordial leads V1 to V6, as the left-sided chest electrodes move further away from the right-sided heart. Normal R-wave progression across the precordial leads, coupled with an inverted P QRS-T in lead I, suggests limb electrode reversal.
RL/LL Electrode Reversal. RL/LL electrode reveral results in no change in the ECG, since there is little difference in the electrical potential between the two legs. On the 12-lead ECG, the RL electrode serves as a ground. Due to the relatively greater distance of the leg (vs the arm) electrodes from the heart, the potential difference is negligible. Remembering that the computer within the ECG recognizes the RL electrode as a ground with no potential difference from the LL electrode, one also can predict the changes seen when the RL electrode is switched with that of the RA.
RA / RL Electrode Reversal. This electrode misconnection is relatively easy to detect, because all limb leads are affected except lead III (because it represents the LA/LL vector). (See Figure 3.) Now getting input from the RL electrode—in the RA position—the ECG records this negligible potential difference between leg electrodes in lead II—the lead that normally demonstrates the vector of RA to LL electrical activity, but now must record the RL electrode situated on the RA. Thus, the key to detecting RA/RL electrode reversal is a near flat line in lead II. 1,3 Similarly, if the RL electrode was switched with that of the LA, lead III now would be nearly flat, as the computer reports no potential difference between the electrodes it "sees" on the left arm (placed incorrectly) and the left leg (placed correctly).
LA/LL Electrode Reversal. This is the most difficult limb electrode misconnection to detect without an old ECG; 3,4 furthermore, if an old ECG is used for comparison, any changes seen should not be ascribed reflexively to reversible cardiac ischemia. Although difficult to recognize as artifactual on any given single tracing, the changes associated with LA/LL electrode reversal should be suspected when unexpected limb lead changes are seen between one ECG and the next. These changes can be anticipated by viewing Figure 3 and mentally flipping the lead III vector from LA to LL. With LA/LL electrode reversal, leads I and II are interchanged; leads aVL and aVF are transposed; and lead III is inverted.
What makes this difficult to detect when considering a lone tracing is the fact that the inferior limb leads (leads II and aVF) are becoming lateral (now leads I and aVL, respectively), and the lateral limb leads (leads I and aVL) are becoming inferior (now leads II and aVF, respectively). Moreover, inverting the P-QRS-T in lead III does not render the tracing blatantly abnormal, as the principal vector of the complexes in lead III normally may be either positive or negative. Further hindering ready detection of LA / LL electrode reversal is that lead aVR is unchanged (remember, only the left-side electrodes are misconnected).
Scrutinizing the P waves in leads I, II, and III may help in detection of LA/LL electrode reversal. The P wave in lead II usually is larger than that seen in lead I, as the normal P wave vector is between +45° and +60°, and thus closely approximates the vector of lead II.3,4 Furthermore, if a biphasic P wave appears in lead III, the terminal portion usually has a negative deflection. Using these two features, reversal of LA and LL electrodes could be detected in 90% of cases (n = 70). 4 (See Figure 4.)
Conclusions
Inadvertent limb electrode misconnection results in artifactual alteration of the ECG. Although the true incidence is unknown, limb electrode reversal, anecdotally, is not uncommon. Understanding the vector forces behind the standard and augmented limb leads results in an improved ability to detect limb electrode reversal. Several telltale changes occur with the commonly encountered limb electrode misconnections; familiarity with these features may lead to better recognition of this phenomenon.
Dr. Harrigan, Associate Professor of Emergency Medicine, Temple University Hospital and School of Medicine, Philadelphia, PA, is Editor of Emergency Medicine Alert.
References
1. Surawicz B. Assessing abnormal ECG patterns in the absence of heart disease. Cardiovascular Med 1977; 2:629.
2. Kors JA, van Herpen G. Accurate detection of electrode interchange in the electrocardiogram. Am J Cardiol 2001;88:396.
3. Surawicz B, Knilans TK. Chou’s Electrocardiography in Clinical Practice. 5th ed. Philadelphia: WB Saunders; 2001.
4. Abdollah H, Milliken JA. Recognition of electrocardiographic left arm / left leg lead reversal. Am J Cardiol 1997;80:1247.
The adage the best chest x-ray is an old chest x-ray can be extended to the world of electrocardiography. With the myriad and subtle changes that may occur on the 12-lead surface electrocardiogram, at times the emergency physicians best ally is an old tracing for comparison.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.