New guidelines warn: You may not be prepared to take care of sick children
New guidelines warn: You may not be prepared to take care of sick children
Many EDs lack appropriate equipment, and staff are not properly trained
Does your ED have equipment which is age- and size-appropriate for all pediatric patients, including premature infants? Do you have protocols for child maltreatment and consent? Are staff trained in pediatric resuscitation? If you answer "no" to any of these questions, you’re not in compliance with new guidelines for pediatric care. Care of Children in the Emergency Department: Guidelines for Preparedness was jointly published by the Dallas-based American College of Emergency Physicians (ACEP) and the Elk Grove Village, IL-based American Academy of Pediatrics (AAP).
If you’re not in compliance with these guidelines, you may not be able to care properly for sick and injured children, which can result in adverse outcomes, warns Marianne Gausche-Hill, MD, FACEP, FAAP, director of emergency medical services at Harbor-University of California at Los Angeles Medical Center in Torrance, CA. "To achieve preparedness simply takes commitment," she argues.
Compelling evidence shows that EDs nationwide may be unprepared for pediatric emergencies, reports Evelyn Lyons, RN, MPH, Emergency Medical Services for Children (EMS-C) director for the Illinois Department of Public Health, based at Loyola University Medical Center in Maywood. Significant differences between adult and pediatric care were determined when the EMS-C assessed the ability of Illinois EDs to care for children, Lyons says. EMS-C is a Washington, DC-based national program to ensure that state-of-the-art emergency medical care is available for all ill or injured children. (See Illinois EMS-C "Facility Recognition Criteria for the Emergency Department Approved for Pediatrics," in this issue.)
Lyons points to this disturbing statistic: While 91% of the Illinois ED physicians had taken an Advanced Cardiac Life Support (ACLS) course for adult resuscitation, only 63% had completed a pediatric equivalent such as Pediatric Advanced Life Support (PALS) or Advanced Pediatric Life Support (APLS). "Similarly, 90% of ED nurses had completed an ACLS course, but only 35% had completed a formal pediatric resuscitation course," she says. (See "Guidelines for Equipment and Supplies for Use in Pediatric Patients in the ED," in this issue.)
The problem is twofold: EDs often don’t have appropriate-sized equipment for all age groups, and ED staff are not trained in pediatric assessment, says Nancy Eckle, RN, MSN, program manager for emergency services at Children’s Hospital in Columbus, OH.
Resuscitation equipment missing
According to a recent study that surveyed Canadian EDs, essential pediatric resuscitation equipment was frequently unavailable.1 For example, 18% did not have pediatric pulse oximeters, 14.8% did not have infant blood pressure cuffs, and 10.5% did not have pediatric defibrillator paddles. "Often, EDs do not have all the equipment necessary to care for all ages of children," Gausche-Hill underscores.
Here are ways to comply with the new guidelines:
• Have pediatric appropriate equipment. The guidelines say that all ED nurses should ensure that pediatric-appropriate equipment, supplies, and medication is available and easy to access, says Gausche-Hill. For example, equipment could be color-coded, or labeled on doors and carts.2 "You must have easy access to different sizes of equipment," she advises. Because pediatric patients range in size from a tiny neonate to an adult-sized adolescent, you’ll need a range of items that are age- and size-appropriate, says Lyons.
A length- or weight-based system for medication dosing and equipment/supplies is an essential tool in the ED, she notes. "Color-coded supply systems ensure ease in accessing appropriately sized equipment and supplies for children," she adds. (For more information on color-coded dosage equipment, see ED Nursing, September 1999, p. 139.)
Use quick-reference materials
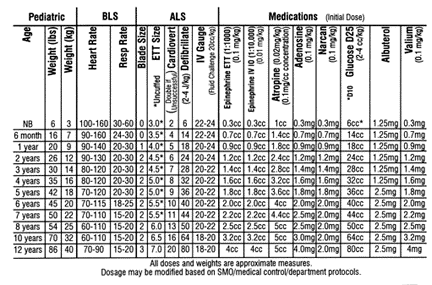
Have "quick-reference" materials available for staff that list normal vital signs by age and equipment sizes by weight and age, says Eckle. "Use length-based resuscitation tapes or precalculated drug lists based on weight," she advises. (See pocket quick-reference card, below, and "Resources," at the end of this article, for information.)
|
|
|
|
|
|
| Source: Illinois Emergency Medical Services for Children, a collaborative program between the Illinois Department of Public Health and Loyola University Medical Center, Maywood, IL. |
Eckle also recommends consulting with pediatric experts in your area to review pediatric and crash cart supplies, and plan strategies for staff education, she says. "These experts may be available to provide inservices or share resources they have used," she adds. Contact a local pediatric nurse practitioner or a manager at a local children’s hospital, tertiary pediatric center, or pediatric intensive care unit, Eckle recommends. "Staff in the hospital nursery can be a great resource for newborn and neonatal emergencies," she adds. Also consider the special-needs children who come to your ED frequently, says Eckle. "Consider what specialized equipment that may be needed in an emergency for that child," she advises. (For more information about caring for children with special needs, see ED Nursing, May 2000, p. 86.)
Your ED may not have certain-sized items in stock because of minimum ordering requirements, such as 10 items per order, notes Lyons. She recommends having reciprocal purchase agreements with other hospitals, with one ED placing a bulk order, and splitting the cost and items. "That way, you don’t need to have a large quantity of an item that may not get used very frequently," she says.
• Make sure your training is up to date. You should be trained in recognizing pediatric emergencies, stabilization procedures, and pediatric-appropriate approaches to care, says Eckle. The guidelines recommend having staff available on all shifts who are trained in pediatric emergency care, says Eckle. She recommends the Emergency Nursing Pediatric Course (ENPC), which addresses a variety of pediatric emergency conditions, resuscitation, assessment, and triage. The course is offered by the Des Plaines, IL-based Emergency Nurses Association (ENA). (See "Resources," at the end of this article, for more information.)
Nurses who provide emergency care to the pediatric population should be current in appropriate assessment, triage, and management of the emergency needs of the pediatric patient, says Lyons. She recommends taking standardized courses such as the ENPC, the Pediatric Advanced Life Support course (PALS) from the Dallas-based American Heart Association, or the Advanced Pediatric Life Support course (APLS) from the Dallas-based American College of Emergency Physicians, and the Elk Village, IL-based American Academy of Pediatrics. These courses contain essential core content on appropriate management of the pediatric patient in an emergency setting, says Lyons. (See "Resources" for information about these courses.)
These courses incorporate skill stations to allow for the practice of advanced practice skills, says Lyons. "At a minimum, at least one nurse per shift who is responsible for the care of the pediatric patient should maintain current recognition in one of these standardized pediatric courses," she adds.
You also should maintain pediatric emergency care continuing education, says Gausche. "If you care for children, you have an obligation to be sure that your pediatric knowledge and skills are updated on a yearly basis," she stresses.
Have separate protocols
• Don’t treat children like adults. According to the guidelines, separate protocols are needed for children, notes Eckle. (See list of recommended policies, procedures, and protocols in "Guidelines for Equipment and Supplies for Use in Pediatric Patients in the ED.") There are anatomic and physiologic differences in children that can affect how procedures are performed as well as the signs and symptoms the child exhibits, says Eckle. She gives the following examples:
— The early stages of shock in a child can be missed if you don’t know the signs and symptoms typically exhibited first in a child, warns Eckle. "These include tachycardia and subtle changes in mental status/level of consciousness such as agitation, irritability, and restlessness," she notes. Hypotension is a very late sign, adds Eckle. "A child may maintain a normal blood pressure until over 25% of the circulating blood volume is lost," she says. Not recognizing and treating shock early can result in death or complications due to tissue hypoxia, she adds.
— Infants and children have a higher body surface to weight ratio, which increases the rate of heat loss, which increases the risk for the development of hypothermia and cold stress, says Eckle. Hypothermia has a significant physiologic impact and affects the child’s response to resuscitative efforts, she adds.
— Infants and children have limited glycogen stores, so they are at increased risk for the development of hypoglycemia, says Eckle. "This is especially true when the body is stressed due to a serious illness or injury," she adds.
References
1. American College of Emergency Physicians and the American Academy of Pediatrics. Care of children in the emergency department: Guidelines for preparedness. Ann Emerg Med 2001; 37:423-427.
2. McGillivray D, Nijssen-Jordan C, Kramer MS, et al. Critical pediatric equipment available in Canadian hospital emergency departments. Ann Emerg Med 2001; 37:371-376.
Sources
For more information about the American College of Emergency Physicians/American Academy of Pediatrics guidelines, contact:
• Nancy Eckle, RN, MSN, Emergency Services, Children’s Hospital, 700 Children’s Drive, Columbus, OH 43205. Telephone: (614) 722-4353. Fax: (614) 722-6890. E-mail: [email protected].
• Marianne Gausche-Hill, MD, FACEP, FAAP, Harbor-UCLA Medical Center, 1000 W. Carson St., Box 21, Torrance, CA 90509. Telephone: (310) 222-3501. Fax: (310) 782-1763. E-mail: [email protected].
• Evelyn Lyons, RN, MPH, EMSC Director, Loyola University Medical Center, 2160 S. First Ave., Building 110, Room 0244, Maywood, IL 60153. Telephone: (708) 327-2556. Fax: (708) 327-2548. E-mail: [email protected].
Resources
A copy of the American College of Emergency Physicians/American Academy of Pediatrics (ACEP/AAP) policy statement, Care of Children in the Emergency Department: Guidelines for Preparedness (published in the April 2001 issue of Pediatrics and Annals of Emergency Medicine) is available. AAP policy statements can be downloaded free from the web site: www.aap.org. (Click on "Policy Statements." Under heading "C," click on "Care of children in the emergency department: Guidelines for preparedness.") Also, they can be purchased for $1.95 each, including shipping and handling. To order materials, contact: AAP Publications Department, P.O. Box 747, Elk Grove Village, IL 60009-0747. Telephone: (800) 433-9016 Ext. 4776 or (847) 981-7924. Fax: (847) 228-1281.
The Emergency Nurses Association offers an Emergency Nursing Pediatric Course (ENPC), a 16-hour course that addresses a variety of pediatric emergency conditions, resuscitation, assessment, and triage. For a list of ENPC courses in your area, go to the ENA web site (www.ena.org), click on "Programs and Meetings" then "Continuing Education," then "ENPC Schedule." For more information, contact: ENA, Department of Trauma and Pediatric Services, 915 Lee St., Des Plaines, IL 60016. Telephone: (800) 900-9659. E-mail: [email protected].
A Pediatric Advanced Life Support Course (PALS) is offered by the American Heart Association (AHA). To contact AHA staff at a local level, call (888) 352-3824 or send an e-mail to [email protected]. For more information about the course, go to the AHA site for Emergency Cardiovascular Care Programs (www.cpr-ecc.org). Click on "About Courses," then "Healthcare Provider Course Descriptions," then "PALS provider." The Advanced Pediatric Life Support Course (APLS) is offered by ACEP and AAP. To find a course in your area, go to the AAP web site (www.aap.org). Click on "Professional Education," then "Life Support Programs," then "APLS: The Pediatric Emergency Medicine Course," then "Find an APLS Course or Course Director." Or contact: AAP, 141 N.W. Point Blvd, Elk Grove Village, IL 60007-1098. Telephone: (847) 434-4000. Ext. 4795. Fax: (847) 228-1350. E-mail: [email protected].
A Pediatric Resource Kit is available from Emergency Medical Services for Children. The kit covers illness and injury prevention, patient care training and safety, equipment guidelines, public policy, and special populations. A free copy is available in CD-ROM format by contacting EMS-C Clearinghouse at (703) 902-1203 or sending an e-mail to [email protected].
A Pediatric Drug Chart quick reference guide is available. The fifth edition (Product Code IN094A) is a 7- x 10-inch chart that includes drug dosages for 37 medications, cardiac arrest medications, pediatric Advanced Cardiac Life Support (ACLS) algorithms, paralytics, and anticonvulsants. The cost is $9 including shipping. A set of pocket-sized, color-coded plastic cards, "Crash Cards — Pediatric Resuscitation" costs $18 (Product Code ETA124). To order, contact: Emergency Training Associates, 105 Glen Hill Court, Union Bridge, MD 21791. Telephone: (800) 367-0382 or (410) 775-7663. Fax: (410) 775-0691. Web: www.emsbooks.com. (Click on "Bookstore" and then "Reference.")
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.