Abdominal Pain in the Elderly Patient
Abdominal Pain in the Elderly Patient
Authors: Joseph P. Martinez, MD, Departments of Medicine and Surgery, Division of Emergency Medicine, University of Maryland School of Medicine, Baltimore, MD; Amal Mattu, MD, Department of Surgery, Division of Emergency Medicine, Co-Director, Emergency Medicine/Internal Medicine Combined Residency Program, University of Maryland School of Medicine, Baltimore, MD.
Peer Reviewer: Thomas W. Lukens, MD, PhD, FACEP, Director of Clinical Operations, Department of Emergency Medicine, MetroHealth Medical Center, Cleveland, OH.
The elderly patient who presents to the emergency department (ED) with the complaint of abdominal pain represents one of the most challenging of all patient encounters. Elderly patients often present late in their course and have atypical symptoms. They may have seemingly normal vital signs despite life-threatening pathology, and the physical examination and laboratory testing may mislead the unwary physician into assuming a benign condition exists. Consequently, elderly patients with abdominal pain frequently are misdiagnosed during their initial physician evaluation, which results in significantly increased morbidity and mortality compared to their younger counterparts. Emergency physicians must have a sound understanding of these atypical presentations to assure prompt diagnosis and treatment, and therefore, improve the prognosis for these patients.
This article will review the epidemiology, general presentation, and evaluation of the elderly patient with acute abdominal pain. We also will review some of the most common and life-threatening entities affecting this patient population. While a comprehensive review of each disease entity is beyond the scope of this article, we will highlight the key differences and atypical features with which elderly patients often present to the ED. Gaining familiarity with these differences will help emergency physicians avert the significant morbidity and mortality that is associated with delayed or missed diagnoses.— The Editor
Introduction
The ED workup of the elderly patient with abdominal pain consumes more time and resources, on average, than that of any other ED patient presentation.1 Although they represent only 15% of ED visits, elderly patients undergo laboratory and radiographic testing at a rate 50% higher than that of younger patients with the same chief complaint, and their length of stay is 20% longer.1 Despite frequent lab testing and a longer length of stay in the ED, however, elderly patients fare significantly worse than younger patients with abdominal pain. Elderly patients have a higher rate of incorrect diagnosis than younger patients with abdominal pain, as well as a higher mortality rate. Overall, elderly patients have approximately an 8-14% mortality rate from their acute cause of abdominal pain—nine-fold higher than that of younger patients.2 When elderly patients with abdominal pain initially are misdiagnosed in the ED, they have twice the mortality rate of patients who are correctly diagnosed, even if they are admitted to the hospital for observation.2
Elderly patients with abdominal pain also account for a significant amount of resource utilization beyond the initial ED encounter. Approximately one-half of all elderly patients that present to the ED with abdominal pain are admitted to the hospital, and 30-40% of those patients require surgical treatment. Of patients who are discharged home from the ED, nearly one-third return with continued symptoms. In contrast, younger patients with abdominal pain are admitted one-third as often, require surgery one-half as often, and "bounce back" to the ED for re-evaluation only one-half as often as elderly patients.2,3
The number of elderly patients presenting to the ED for evaluation is likely to increase as the population ages. Currently, it is estimated that approximately 12% of the U.S. population is age 65 or older, but this number is expected to grow to 20% by the year 2030.3 There is no question that all emergency physicians will need to be well-versed in evaluating and treating this growing segment of our society.
Physiologic Changes in the Elderly
The normal physiologic changes that accompany aging cause increased difficulty in the evaluation and treatment of elderly patients and contribute to a worse prognosis. An elderly patient’s immune system does not respond to infection as efficiently because of declining T-cell function.4 Physical barriers to infection (e.g., skin and mucous membrane integrity and strength) also are altered in the elderly, and malnutrition may further decrease immunocompetence. Elderly patients also may not respond as early as younger patients to usually painful intra-abdominal conditions. A 1960 study demonstrated a generalized decreased perception of pain in the elderly.5 Altered pain perception has been well-documented and is well-known in elderly patients with unstable angina and myocardial infarction,6,7 and more recent studies have now documented decreased pain perception of intra-abdominal conditions.3,8,9 As a result, elderly patients often present to the ED later in their course of illness; this delayed presentation contributes to a worse prognosis. Care of these patients is further complicated by memory deficits, which often make obtaining a history difficult or impossible and also may make it unreliable. Finally, the large number of comorbidities found in the elderly patient, combined with extensive medication use (e.g., non-steroidal anti-inflammatory drugs [NSAIDs], anticholinergics, cardiac medications, corticosteroids, etc.), may mask or even produce pathology that further confuses the clinical presentation.
General Evaluation
The initial evaluation of the elderly patient should be systematic and thorough. In the hemodynamically stable patient, a detailed history of any present illnesses should be obtained. Special attention should be paid to the rapidity of onset of the patient’s pain. Sudden onset of pain should alert the physician to the possibility of a vascular cause of the pain (e.g., mesenteric ischemia, ruptured abdominal aortic aneurysm [AAA], myocardial infarction). The patient also should be questioned regarding any associated lightheadedness, weakness, or near-syncope, as these symptoms also suggest the presence of a vascular etiology or rapid gastrointestinal blood loss. The patient’s previous medical history (especially with regard to any previous episodes of similar pain and any prior workup) and previous surgical history are important components of the initial history.
A complete medication history always should be obtained. Patients should be questioned regarding the use of prescription medications, as well as over-the-counter medications and herbal supplements. Elderly patients are particularly susceptible to side effects of medications. Anticholinergic medications, including antihistamines, phenothiazines, and some antidepressants, may induce abdominal pain through urinary retention or the production of an ileus. Opiates, especially codeine preparations, may induce severe constipation and result in abdominal pain. Many other medications, including NSAIDs, erythromycin, colchicine, and laxatives, also can induce abdominal pain. Certain medications can alter the initial evaluation process, as well. Corticosteroids, for example, can blunt the expected inflammatory response to peritonitis and result in reduced abdominal tenderness. They also can blunt the expected febrile response and alter the white blood cell count. Opiates and NSAIDs, if taken by the patient prior to the medical evaluation, also can reduce abdominal tenderness during the examination, and NSAIDs and acetaminophen preparations can temporarily decrease or eliminate a patient’s fever.
Close attention should be paid to the vital signs. However, "normal" vital signs in elderly patients may be misleading. Elderly patients may be normothermic even in the presence of severe intra-abdominal infections because they often have a blunted or delayed febrile response.8,10 In fact, elderly patients are four times more likely than their younger counterparts to be hypothermic in response to intra-abdominal pathology.10 The use of steroids, NSAIDs, or acetaminophen also may blunt the expected febrile response to serious illness. Other physiologic responses to illness also may be blunted by the patient’s medications. The expected tachycardia normally found in patients with serious disease may be absent in elderly patients because of the use of beta-adrenergic blocker or calcium-channel blocker medications. A "normal" blood pressure also may be misleading. Many elderly patients have chronic isolated systolic hypertension (ISH). As a result, a systolic blood pressure of 120 mmHg, while normal in a young patient, may represent significant hypotension in the elderly patient with ISH who normally maintains a systolic blood pressure of 180 mmHg.
A detailed physical examination is important in elderly patients with abdominal pain. The physician should assess the patient’s abdomen for any evidence of distension, abnormal bowel sounds, organomegaly or pulsatile masses, tenderness, and peritonitis. However, the absence of classic peritoneal findings does not eliminate the possibility of significant intra-abdominal disease. Abdominal guarding and rigidity may be absent even in the presence of peritoneal irritation, and be partially attributable to the decreased pain perception mentioned previously, and also attributable to thin abdominal wall musculature in elderly patients.10,11 Elderly patients more frequently have prior surgeries, with resulting intra-abdominal adhesions. These adhesions may cause localization of tenderness from peritonitis rather than diffuse tenderness, even in the presence of a perforated viscus.10
The cardiothoracic examination is very important as well. Lower lobe pneumonias, pulmonary emboli, pericarditis, acute coronary syndromes, and other cardiac and pulmonary diseases may cause abdominal pain. The genitourinary examination is equally important. Inguinal and femoral hernias can cause bowel obstruction. Acute testicular or ovarian pathology can cause abdominal pain. Finally, the rectal examination may reveal important clinical information. Occult or gross blood may suggest mesenteric ischemia, rapid gastrointestinal bleeding, or the presence of an AAA with an aortoenteric fistula. Significant prostate tenderness may be the only clue to a diagnosis of prostatitis.
It is prudent to obtain an extended database of laboratory studies, although laboratory values often are normal in elderly patients despite the presence of surgical disease.2 Plain radiographs of the abdomen have a poor sensitivity and specificity for detecting most abdominal pathology, and they are indicated only if there is clinical suspicion of perforation, obstruction, or bowel ischemia.11,12 Elderly patients often will require extended work-ups, and as previously noted, require surgery more often than younger patients. Therefore, surgical consultation should be obtained early in the ED course of patients with symptoms and signs indicating a disease that may require surgical attention.11 (See Table 1.)
| Table 1. Signs and Symptoms Indicating Possible Surgical Disease11 | |
| • | Pain duration > 6 hours and < 48 hours |
| • | Sudden onset of pain |
| • | Pain aggravated by movement (suggests peritoneal irritation) |
| • | Pain preceding vomiting |
| • | Maximal abdominal tenderness in right upper quadrant or right lower quadrant |
For patients who are hemodynamically unstable, attention to the basic ABCs (airway, breathing, circulation) of resuscitation is vital. High-flow oxygen should be administered and the airway secured. Large-bore intravenous access should be obtained, and the patient should be placed on a cardiac monitor. Blood should be typed and crossmatched. The most immediately life-threatening conditions should be considered first. In the patient with abdominal pain, these conditions include mesenteric ischemia, ruptured AAA, perforated viscus, and myocardial infarction. A focused physical examination should be performed; physicians should pay special attention to the heart, lungs, abdominal aorta, and peripheral pulses.11 An electrocardiogram and upright chest radiograph should be rapidly obtained as well. A general surgeon should be consulted emergently for these patients, even when the initial diagnosis is unclear.
Specific Entities
The list of specific conditions that cause abdominal pain in the elderly is quite extensive (see Table 2) and involves not only intra-abdominal pathology but also pathology from many other organ systems. The following section reviews some of the most common and clinically important causes of abdominal pain in elderly patients, with emphasis on potential pitfalls in the evaluation process.
| Table 2. Common Causes of Abdominal Pain in the Elderly | |
| • | Cholecystitis |
| • | Bowel obstruction (small or large bowel) |
| • | Diverticular disease |
| • | Peptic or duodenal ulcer |
| • | Gastritis |
| • | Abdominal pain of unclear etiology |
| • | Pancreatitis |
| • | Cholelithiasis |
| • | Hepatitis |
| • | Cholangitis |
| • | Malignancy |
| • | Appendicitis |
| • | Vascular disease (mesenteric ischemia or aortic aneurysm) |
| • | Gastroesophageal reflux disease |
| • | Constipation |
| • | Pseudo-obstruction (Ogilvie’s syndrome) |
| • | Gastrointestinal ileus |
| • | Gastroenteritis |
| • | Extra-abdominal causes (cardiac, pulmonary, endocrine, genitourinary) |
| • | Medications |
Bowel Obstruction. Bowel obstruction includes both small bowel obstruction (SBO) and large bowel obstruction (LBO). The causes are different depending on the site of the obstruction. SBOs usually are the result of post-surgical adhesions or hernias. Carcinomas cause SBOs less often.13,14 Gallstone ileus also may lead to SBO, and is reported to be the cause of SBO in 20% of elderly women.15,16 In contrast, LBO in the elderly is predominantly due to colon cancer. Volvulus (sigmoid or cecal) and diverticulitis are other frequent causes of LBOs.
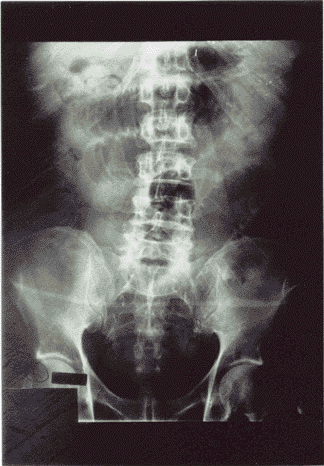
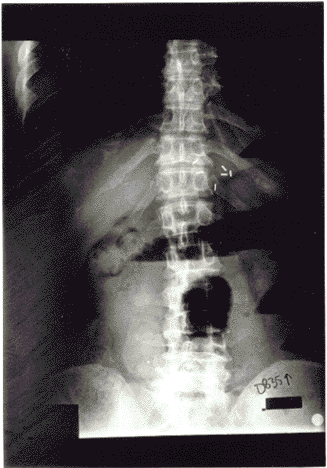
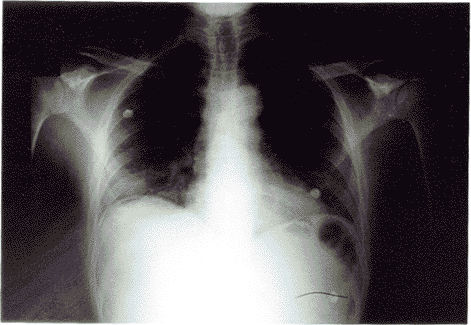
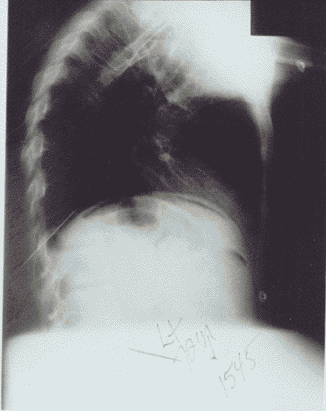
SBO (see Figures 1A and B) presents with symptoms that are similar to those seen in younger patients: Abdominal pain, vomiting, and abdominal distention. These symptoms usually are present to some extent, and a history of previous abdominal surgery is more likely to be obtained in the elderly patient.
|
Figures 1A and B. Small Bowel Obstruction |
| 1A |
|
|
| 1B |
|
|
However, early in the course, symptoms often are very non-specific and the physical exam may not be helpful at all. This may account, in part, for the high rate of misdiagnosis of SBO. In one older, but oft-quoted study of 1000 consecutive cases of abdominal pain, it was the second most common abdominal surgical condition (following appendicitis) to be discharged home inappropriately from the ED.2 Delays in diagnosis and misdiagnosis contribute to a high mortality rate (14-35%) in elderly patients with SBO.11,14
LBO in the elderly is predominantly due to carcinoma. The presentation may reflect the insidious nature of the underlying disease. Patients often complain of poorly localized abdominal pain, with abdominal distention progressing over several days.17 The classic description of LBO is that of a patient with abdominal pain that is associated with severe constipation or obstipation and persistent vomiting. However, 19% of elderly patients with LBO actually will complain of diarrhea, only one-half of all patients will report vomiting, and only one-half will report severe constipation or obstipation.17 The absence of vomiting and obstipation and the presence of diarrhea may contribute to initial misdiagnosis, resulting in delays in proper diagnosis and an increased incidence of perforation, bowel infarction, and/or sepsis with a worse outcome. In fact, the mortality for elderly patients with LBO averages 40%.17 All patients with evidence of obstruction should be carefully questioned for symptoms of weight loss, change in bowel habits, rectal bleeding, and fatigue, as these may suggest the diagnosis of colorectal cancer.18,19
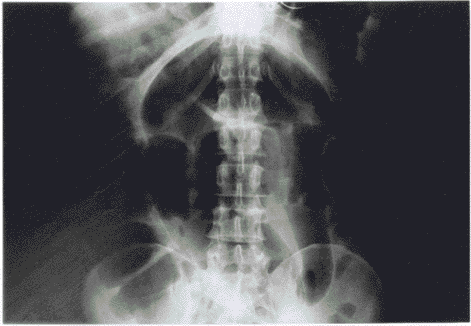
LBO that occurs as a consequence of volvulus (15% of cases) presents somewhat differently depending on the site of the affected segment of colon. Sigmoid volvulus (see Figure 2) is far more common than cecal volvulus, and accounts for almost 80% of cases.20
|
Figure 2. Large Bowel Obstruction Due to Sigmoid Volvulus |
|
|
The onset of pain is more gradual in patients with sigmoid volvulus. Nausea and vomiting are found in only one-third of patients and constipation in one-half to three-fourths of patients.11,21 Abdominal distention commonly is found during the physical examination. The presentation of cecal volvulus contrasts this, in which the course is typically that of acute onset of severe abdominal pain associated with nausea and vomiting.22 Treatment of volvulus depends on the type; most cases of sigmoid volvulus can be successfully treated non-operatively with rectal decompression using a sigmoidoscope, whereas virtually all cases of cecal volvulus require surgical intervention.3 Colonic volvulus may be associated with compromised blood supply to the involved segment of bowel. Delays in proper diagnosis and treatment can result in bowel infarction.
Biliary Tract Disease. Biliary tract disease remains the leading indication for intra-abdominal surgery in the elderly patient.23,24 Mortality from acute cholecystitis is 10-14% in this group of patients, and mortality from emergent cholecystectomy is almost four-fold higher than when the same procedure is performed electively.25-27
Elderly patients with acute cholecystitis (see Figure 3) usually will have right upper quadrant pain or epigastric pain and localized tenderness over the gallbladder. However, other signs and symptoms usually found in younger patients may be delayed or absent. For instance, more than one-half of elderly patients with acute cholecystitis have no nausea or vomiting, and more than one-half may be afebrile.28 Even in the presence of gallbladder empyema, perforation, or gangrene, more than one-third of patients may be afebrile.25
|
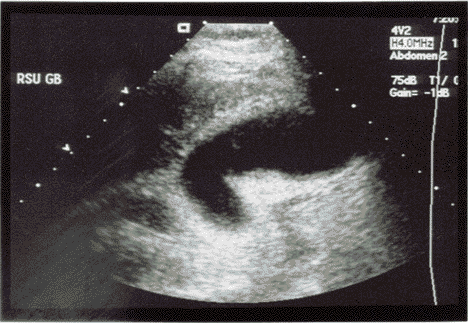
Figure 3. Acute Cholecystitis on Ultrasound |
|
|
| Ultrasound demonstrates markedly enlarged gallbladder with thickening of the gallbladder wall. |
Laboratory studies in elderly patients with acute cholecystitis are often unreliable as well. More than 30% of elderly patients have a normal white blood cell count,25,28 and a significant number also have normal liver function tests and normal alkaline phosphatase levels.28 The elderly have a higher prevalence of complications of acute cholecystitis as well, such as emphysematous cholecystitis, gallbladder gangrene, and gallbladder perforation. In these patients, hypotension and septic shock may be the initial presentation of biliary disease. Once the diagnosis is made, it must be treated rapidly. Broad-spectrum antibiotics should be initiated in the ED, and prompt surgical consultation should be obtained, as delayed surgical treatment is associated with an increased morbidity and mortality.29
Choledocholithiasis also is more common in elderly patients, which in turn increases the prevalence of ascending cholangitis in this age group.30 Fever, jaundice, and right upper quadrant pain (Charcot’s triad) are the classic findings, and these patients rapidly progress to septic shock and death if not treated rapidly. Acute suppurative cholangitis is an entity rarely found in patients before the seventh decade of life that is caused by gallbladder obstruction (either by stone, stricture, or malignancy), with subsequent development of frank pus behind the obstruction.31 Prompt decompression is imperative. Disseminated intravascular coagulopathy (DIC) occurs frequently in the setting of either ascending cholangitis or acute, suppurative cholangitis; therefore, coagulation studies should be closely monitored in these conditions.3
Pancreatitis. While pancreatitis may occur at any age, there is a 200-fold increase in the incidence of acute pancreatitis after the age of 65.32 It is, in fact, the most common non-surgical abdominal condition requiring admission to the hospital in this age group.33,34 Various predisposing factors leading to acute pancreatitis in the elderly population have been postulated.3 (See Table 3.) Signs and symptoms of pancreatitis may range from the classic penetrating, mid-epigastric pain associated with low-grade fever, vomiting, and dehydration, to a dynamic, hypermetabolic state resembling the sepsis syndrome or systemic inflammatory response syndrome.33
| Table 3. Common Predisposing Factors to Acute Pancreatitis in the Elderly3 | |
| • | Alcoholism |
| • | Biliary disease |
| • | Penetrating ulcer |
| • | Infection: Viral, Escherichia coli, Staphylococcus, Pseudomonas, Klebsiella |
| • | Hypertriglyceridemia |
| • | Drug reactions: Thiazides, furosemide, NSAIDs, corticosteroids, etc. |
| • | Hypercalcemia |
| • | Carbon monoxide exposure |
| • | Hypothermia |
Ten percent of patients will present without abdominal pain or vomiting but merely with unexplained hypotension and altered mental status.3 As with most other abdominal processes, the mortality rate for acute pancreatitis in elderly patients is much higher than that found in younger patients, with rates approaching 40% in those age 70 and older.34
Peptic Ulcer Disease. Asymptomatic peptic ulcer disease is well documented in the elderly population. Studies have demonstrated that 35% of patients older than age 60 with endoscopically proven peptic ulcer disease report no pain, compared to only 8% of those younger than age 60.8,35 Often, the diagnosis is not made until a life-threatening complication of the ulcer occurs. In fact, 50% of elderly patients will present with an acute abdomen as their first manifestation of peptic ulcer disease, which is frequently due to a perforation.3 Hemorrhage also is a common complication of peptic ulcer disease. Other complications include penetration into an adjacent viscus and gastric outlet obstruction.
Patients with perforation from peptic ulcer disease may present very atypically. In one study, fewer than one-half of patients older than age 70 reported the classic sudden onset of abdominal pain.24 Most patients are afebrile. Abdominal tenderness may not be localized to the epigastrium; it may be generalized or absent. One large study reported that epigastric rigidity is absent in nearly 80% of patients with perforated ulcers.24 Importantly, while the demonstration of free intraperitoneal air on plain radiograph may aid in diagnosis (see Figures 4A and 4B), up to 40% of elderly patients with perforated ulcers will not demonstrate this finding.10,11
|
Figures 4A and B. Pneumoperitoneum Due to Perforated Peptic Ulcer |
| 4A |
|
|
| 4B |
As noted previously, hemorrhage is a frequent complication of peptic ulcer disease. Elderly patients are more likely to hemorrhage from their ulcers than younger patients. The use of NSAIDs or corticosteroids increases the risk of bleeding. Ten to 20 percent of patients who develop hemorrhage will have no preceding symptoms of an ulcer.36 When elderly patients bleed from ulcer disease, they are more likely to require surgery to control the bleeding, more likely to rebleed, and more likely to require blood transfusions than younger patients.37 Early signs of bleeding may be masked or absent in the elderly because of an altered physiologic response to stress or medication effects (e.g., beta-adrenergic blocker or calcium-channel blocker medications blunting the tachycardia of acute blood loss).
Diverticular Disease. Diverticular disease is present in only 5% of the general population, but it increases in incidence with advancing age: it is present in 50% of Americans older than age 60 and its incidence increases thereafter.3,38 Diverticular disease can be complicated by diverticulosis, which may manifest as painless lower gastrointestinal bleeding, and diverticulitis, which may be associated with bowel obstruction or ileus, abscess formation, perforation, and sepsis.
Diverticulosis is the most frequent cause of massive lower gastrointestinal bleeding in the elderly population.38 Approximately 15% of patients with diverticular disease will have at least one episode of significant hemorrhage. The bleeding is usually painless and typically resolves spontaneously. However, 25% of patients will have recurrent episodes of bleeding, and some of these patients can develop shock.39 Diverticulosis should be a diagnostic consideration in any patient with painless rectal bleeding.
Diverticulitis eventually develops in 30% of patients with diverticular disease.40 The classic presentation is that of left lower quadrant pain with nausea, mild abdominal distention and a tender, left lower quadrant mass, low-grade fever, and leukocytosis. However, many of the expected examination findings are sometimes absent, and leukocytosis is absent in one-half of patients. Diverticulitis is misdiagnosed in 50% of cases.25,41 Inflammation in close proximity to the urinary bladder or ureter can induce pyuria or hematuria, mistakenly leading to the diagnosis of urinary tract infection or renal colic. In women with diverticulitis, when a mass is palpated it is often misdiagnosed as a pelvic mass of gynecologic origin.3,11,42 When diverticulitis occurs on the right side of the abdomen, it often is misdiagnosed as appendicitis. Liberal use of computerized tomography (CT) in elderly patients with lower abdominal pain or tenderness can help distinguish among these various entities.
Appendicitis. Once thought to be a disease only of young patients, appendicitis is now also recognized to occur frequently in the elderly population. Appendicitis is the third most common abdominal surgical emergency in the elderly, accounting for 5-7% of all abdominal emergencies in this population.16,43,44 However, it is commonly associated with delays in diagnosis or misdiagnosis. In one report, nearly one-fourth of all elderly patients with documented appendicitis were initially evaluated in an ED and subsequently discharged home.45 A 1990 study of elderly patients with surgically proven appendicitis showed that only one-half of patients were thought to have appendicitis at the time of admission, and in only 70% was the diagnosis even a consideration at the time of surgery. In the same study, 72% had perforated by the time of surgery.47 Delays and missed diagnoses are associated with a higher rate of complications from appendicitis, including abscess formation, gangrene, and perforation, and these complications are associated with a higher mortality rate. In part because of the frequency with which these patients are misdiagnosed and develop complications, elderly patients account for 50% of all mortalities from acute appendicitis.47-49
The large number of delayed and missed diagnoses of appendicitis is the result of various factors. The elderly often present to the ED in a delayed fashion, which often is due to poor access to care, communication problems, dislike of hospitals, or a belief that pain is a part of aging.47-49 Up to 20% will present after three days of symptoms, and as many as 5-10% will present after one week of symptoms.10,11,47-50 Elderly patients may mistakenly attribute their symptoms to a more benign diagnosis (e.g., constipation) and attempt home remedies (e.g., enemas) before presenting to the ED, further delaying prompt diagnosis and treatment.
A second factor in the high rate of delayed and missed diagnoses relates to the atypical symptoms and signs with which patients present. Only one-third of elderly patients have the "classic" presentation of acute appendicitis: Pain migrating to the right lower quadrant, nausea, vomiting, anorexia, and low-grade fever.47 Furthermore, the elderly patient’s description of the pain is often vague and poorly localized.11,47,49 Although tenderness in the right lower quadrant is found in most patients with appendicitis, it is absent in as many as 20% of patients.11 Up to 50% of patients are afebrile, and the classic peritoneal signs (rebound and involuntary guarding) are seen in fewer than one-half of patients in some studies, despite the very high prevalence of perforations in this population.10,11,47,50
Potentially misleading laboratory data compose the third factor that leads to increased delays and misdiagnoses. Studies have demonstrated a normal white blood cell count in 20-45% of elderly patients with appendicitis.47,49,50 Laboratory values may, in fact, falsely suggest alternative diagnoses and contribute to delays in proper diagnosis. For instance, 17% of elderly patients have hyperbilirubinemia, suggesting a biliary cause of the patient’s abdominal pain. An additional 19-40% have an abnormal urinalysis with pyuria and/or microscopic hematuria, which suggests a genitourinary process.11,47,51 Plain radiographs may be misleading as well. Up to 25% of radiographs demonstrate a pattern consistent with an ileus or SBO, or demonstrate incidental nephrolithiasis or cholelithiasis.46,47 These radiologic findings may lead to inappropriate non-operative management and observation rather than prompt surgical treatment. This delay is associated with an increased risk of appendiceal gangrene or perforation.
Delays in diagnosis significantly increase the risk of complications and mortality. Overall, mortality in this age group from acute appendicitis is approximately 8%, but increases to 20-30% after perforation has occurred.46,47,49 These statistics should encourage the ED physician to maintain a high index of suspicion in any elderly patient with abdominal pain who still possesses an appendix. The liberal use of abdominal CT (see Figures 5A and B) to aid in diagnosis is warranted and has been shown to be significantly more cost-effective than plain abdominal radiography.52
|
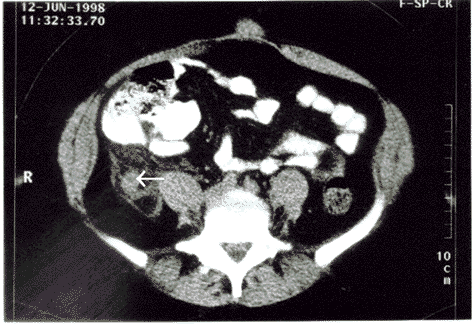
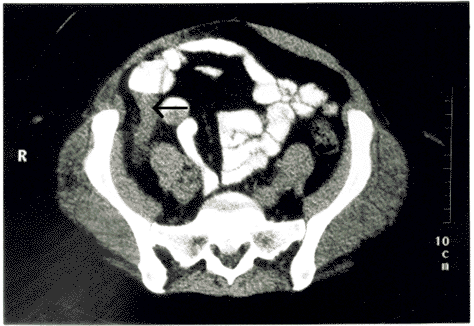
Figures 5A and B. CT Scan Demonstrating Acute Appendicitis |
|
|
|
A. An enlarged appendix in transverse section (see arrow) that is not filling with contrast. Extensive infiltration of the adjacent fat is present, consistent with active inflammation. |
B. The markedly enlarged, non-contrast-filled appendix (see arrow) in longitudinal section, extending to the cecum.
Urgent surgical consultation should be obtained in suspicious cases, as numerous recent studies have demonstrated considerable decreases in morbidity and mortality when rapid diagnostic laparotomy is pursued rather than a course of watchful waiting.53-55
Mesenteric Ischemia. Mesenteric ischemia is one of the most challenging of all diagnoses because there are usually minimal, if any, early objective examination findings.56 Despite increased physician awareness of this condition, improved understanding of its pathophysiology, and refined imaging studies during the past 10 years, mortality has remained in the range of 70-90%.57 Any delay in diagnosis and treatment is associated with a worse prognosis. Therefore, any chances for a good outcome are dependent on early consideration and aggressive workup of this diagnosis.
Mesenteric ischemia comprises four distinct entities. (See Table 4.) Superior mesenteric artery (SMA) embolus represents the most common cause, and accounts for one-half of all cases of mesenteric ischemia.58 Emboli usually occur in patients with underlying cardiac disease, dysrhythmias such as atrial fibrillation, or ventricular thrombi in post-myocardial infarction patients.59,60 SMA thrombosis causes approximately 15% of cases and usually is found in patients with chronic vascular disease and long-standing atherosclerosis.61
| Table 4. Etiologies of Mesenteric Ischemia58 | |
| Etiology | Percentage of cases |
| Superior mesenteric artery embolus | 50% |
| Superior mesenteric artery thrombosis | 15% |
| Non-occlusive mesenteric ischemia (NOMI) | 20% |
| Mesenteric venous thrombosis (MVT) | 15% |
Non-occlusive mesenteric ischemia (NOMI) is found in patients with low-flow states such as congestive heart failure, sepsis, or severe dehydration, and has been reported to cause nearly one-fifth of all cases of mesenteric ischemia.62 Numerous medications also have been associated with NOMI.63,64 (See Table 5.) Lastly, mesenteric venous thrombosis (MVT) accounts for the remaining 15% and is found in patients with hypercoagulable states, malignancies, sepsis, and liver disease.65
| Table 5. Medications Associated with Non-Occlusive Mesenteric Ischemia63,64 | |
| • | Amitryptiline |
| • | Dextroamphetamine |
| • | Pitressin |
| • | Cocaine |
| • | Ergot alkaloids |
| • | Propranolol |
| • | Digitalis |
| • | Estrogen/oral contraceptives |
| • | Vasopressors |
| • | Diuretics |
| • | Methamphetamine |
The triad of abdominal pain, gut emptying, and underlying cardiac disease often is used to describe mesenteric ischemia.66 Classically, the pain is severe and described as being of sudden onset and out of proportion to physical findings. Patients may present writhing, unable to localize the pain. Associated nausea and anorexia is present in 80% of cases, and some form of gut emptying (either vomiting or diarrhea) is present in more than one-half of the cases.67 Abdominal palpation frequently reveals minimal reproducible tenderness until after infarction and peritonitis have developed. Occult or gross blood on the rectal examination frequently is absent until late in the course of the disease as well.60 Unfortunately, the presence of non-specific gastrointestinal symptoms (e.g., nausea, vomiting, anorexia, diarrhea) and a non-diagnostic abdominal examination may result in an initial misdiagnosis of gastroenteritis and lead to catastrophic delays in arriving at the proper diagnosis. Further complicating diagnostic efforts, not all cases of mesenteric ischemia are associated with the classic sudden onset of abdominal pain. SMA thrombosis, NOMI, and MVT all are often associated with a more gradual onset of symptoms. In fact, pain associated with SMA thrombosis is quite different and is described as postprandial ("intestinal angina"), associated with chronic weight loss and gastrointestinal symptoms that progress over the course of months.68
Laboratory values may help raise the clinical suspicion for this diagnosis. Though a normal white blood cell count cannot exclude the diagnosis, a markedly elevated count should heighten the physician’s concern for this disease. In one study, for example, 90% of patients with confirmed mesenteric ischemia had white blood cell counts of greater than 15,050/mL, and many patients had counts of greater than 20,000/mL.69 Similarly, 90% of patients with mesenteric ischemia have elevated serum lactate levels, and this elevation correlates with the extent of ischemia noted at surgery.70,71 Although not specific, the sensitivity of serum lactate in the diagnosis of mesenteric ischemia makes it the best measurable laboratory indicator of mesenteric ischemia currently available.63,71 Other reported laboratory findings of mesenteric ischemia include metabolic acidosis, hyperphosphatemia, hyperamylasemia, and elevated creatinine phosphokinase levels, although none are considered to be sensitive or specific for this disorder.72 Plain radiographs may sometimes demonstrate air within the bowel wall, thickening of the bowel wall, or air within the portal system.73,74 However, it should be noted that all of these laboratory and radiographic abnormalities occur late in the disease course, and often after bowel infarction has already occurred.66,67
For patients in whom mesenteric ischemia is suspected, rapid evaluation is guided by clinical suspicion. Those patients with a high likelihood (based on history, risk factors, and physical examination) of ischemia should have emergent mesenteric angiography performed in conjunction with immediate surgical consultation. Angiography can demonstrate reliably the presence or absence of an obstructive lesion and also distinguish between the four main etiologies of mesenteric ischemia. In addition, angiography demonstrates the extent of ischemia as well as collateral circulation and is therefore helpful in surgical planning. Angiography also can be used therapeutically; in selected cases, a potent local vasodilator (e.g., papaverine) can be infused with some benefit.3 For patients judged to have a low probability of this diagnosis, some authors have advocated the use of CT. CT has been demonstrated in a recent study to be 83% sensitive and 93% specific for diagnosing mesenteric ischemia secondary to bowel obstruction.74 Typical findings include bowel wall thickening, pneumatosis (air within the bowel wall), blurring of mesenteric fat, and visualization of the actual arterial or venous embolus/thrombosis. (See Figure 6.)
|
Figure 6. CT Scan Demonstrating Mesenteric Infarction. |
|
|
|
There is extensive air present within thickened loops of bowel wall. |
|
(Photo reprinted courtesy of Dr. Barry Daly, Department of Radiology, University of Maryland Medical Center, Baltimore, MD.) |
Often, however, these CT findings will not be seen until late in the disease course. Another study found that detection of one of these signs by CT scan was only 64% sensitive.73 However, given its general availability, good reliability, and these accepted diagnostic findings, CT scan is an ideal initial test for stable patients with a low to moderate clinical suspicion for suspected mesenteric ischemia.65 Additionally, CT scanning also may be useful to evaluate for alternative diagnoses.73,74
It is clear that the key prognostic factor is time between symptom onset and intervention. Survival has been shown to be increased when this interval is 12 hours or less.75 One study reported that when diagnostic angiography was performed prior to the onset of peritonitis, the mortality was reduced from greater than 70% to 10%.57 These findings highlight the importance of early consideration and aggressive workup of this diagnosis in order to insure the best possible outcome from this deadly disease.
Ruptured Abdominal Aortic Aneurysm
Ruptured AAA is the 13th leading cause of death in the United States, accounting for 10,000-15,000 deaths annually.76 That as many as 30% of cases initially are misdiagnosed causes concern.77,78 Any delay or missed diagnosis is associated with a tremendous increase in the risk of mortality. Even when a prompt diagnosis is made and the patient is immediately taken to surgery, the prognosis is still grim. A 1991 study demonstrated a mortality rate of 70% in cases of ruptured AAA despite an average ED time of only 12 minutes prior to surgery.79 It should be noted that many of these cases were associated with initial hemodynamic instability, a poor prognostic sign from the outset. In ED practice, however, many patients with a ruptured AAA will present with a (temporarily) stable blood pressure. These are the patients that afford the emergency physician an opportunity to make a difference and save lives. Unfortunately, these also are the patients in whom a proper diagnosis may be delayed or missed by the unwary physician.
The diagnosis of a ruptured AAA is relatively simple when the patient presents with the classic triad of hypotension, abdominal pain, and a pulsatile abdominal mass. However, this classic presentation is found in only 30-50% of cases.80,81 Hypotension is absent in 65% of patients, presumably because of tamponade of the bleeding in the left retroperitoneal space.82 This tamponade delays exsanguination and gives the emergency physician an opportunity to prevent an otherwise certain death. As many as 20-30% of patients have no abdominal pain at all and may instead have back pain. Approximately 25% of patients have no palpable abdominal mass even with aneurysms that are greater than 5 centimeters in diameter.83
Misdiagnosis of ruptured AAA is quite common, especially when the elderly patient presents with non-specific abdominal, back, or flank pain. Radiation of the pain toward the groin, in combination with microscopic hematuria from compression of the ureter, often leads to the misdiagnosis of renal colic. Renal colic is, in fact, the most common misdiagnosis in ruptured AAA cases.77,78 Flank pain or back pain also occasionally is misdiagnosed as musculoskeletal strain. Left lower quadrant pain from the AAA frequently is misdiagnosed as diverticulitis. Patients present with syncope in 15-20% of cases, and these patients often are misdiagnosed as having a cardiac dysrhythmia or acute coronary syndrome.78 Erosion into the gastrointestinal tract may lead to upper or lower gastrointestinal (GI) bleeds. This entity, an "aortoenteric fistula," usually occurs in patients who have previously had an AAA repair performed and should be considered immediately in any patient presenting with a GI bleed who has a history of such a repair. Any delay in diagnosis (e.g., mistakenly diagnosing these patients with diverticulosis) and treatment further increases the 50% mortality found with this presentation.78 Another common mistake is to inappropriately attribute hypotension in an elderly patient with abdominal pain to sepsis rather than to a ruptured AAA.76,77
On physical examination, the patient should be rapidly assessed for the presence of abdominal mass, abdominal bruit, signs of peripheral embolization ("blue toe syndrome"), and signs of gastrointestinal bleeding. Femoral pulses should be assessed as well. However, because the physical examination can be unreliable, risk stratification should be performed based on history and examination of risk factors.84
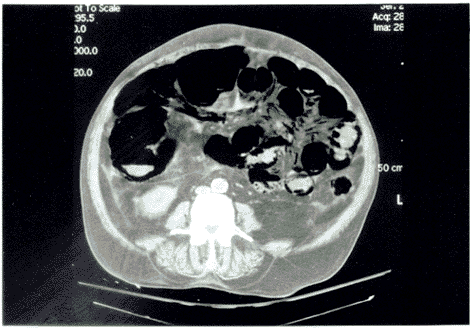
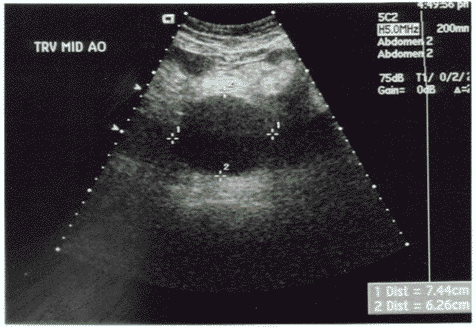
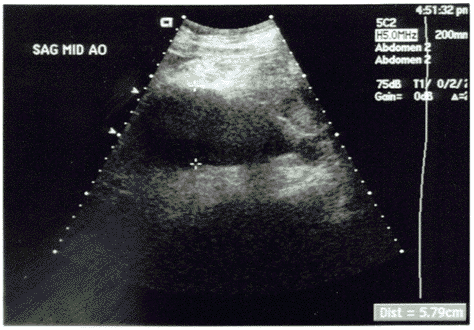
The work-up of a patient with a suspected ruptured AAA is determined by the stability of the patient. Unstable patients with abdominal pain and diagnostic physical findings (e.g., pulsatile abdominal mass) or with a previous diagnosis of an AAA should be immediately taken to the operating room, as their mortality with any delays exceeds 70%.79 For patients who are hemodynamically stable and in whom the diagnosis is still in question, CT generally is recommended.85 CT is the most sensitive imaging study for detecting both the presence of an aneurysm and the presence of rupture.86 However, in patients who are considered at high risk for decompensation if they leave the ED, or for those in whom active resuscitation is underway, bedside ultrasound is the modality of choice.86 (See Figures 7A and B.)
|
Figures 7A and B. Ultrasound of an Abdominal Aortic Aneurysm |
| 7A |
|
|
| 7B |
|
Abdominal aortic aneurysm demonstrated in cross section (see A) and sagital section (see B). |
Ultrasound is fast, easy to use, can be done at the bedside simultaneous with ongoing resuscitative efforts, and has outstanding sensitivity for detection of an AAA even in the hands of relatively inexperienced personnel.87,88 Although ultrasound has poor sensitivity for detection of aneurysm rupture, merely documenting the presence of the aneurysm in a symptomatic patient usually is sufficient to justify emergent operative intervention. Surgical consultation should be obtained rapidly in the ED for all patients when the diagnosis of ruptured AAA is strongly considered.
Non-Abdominal Causes of Abdominal Pain
Numerous extra-abdominal entities can present with isolated abdominal pain in elderly patients. Perhaps the most important extra-abdominal cause of abdominal pain is the acute myocardial infarction (AMI). Elderly patients with AMI often do not have chest pain. For example, one study found that 33% of women older than age 65 exhibit abdominal pain as the main presentation of their AMI.89 Other cardiac causes of abdominal pain can include congestive heart failure with hepatic congestion, pericarditis, and endocarditis.
Acute pulmonary conditions, such as pneumonia, pulmonary embolism, pneumothorax, effusions, or empyema, all may produce abdominal pain as well. Endocrine conditions that may result in non-specific abdominal pain include acute adrenal crisis, hypercalcemia, and diabetic ketoacidosis. Genitourinary and gynecologic causes of abdominal pain include renal colic, urinary tract infection, pyelonephritis, testicular or ovarian torsion, hernias, epididymitis, ovarian masses, and uterine masses. A genital examination in men and pelvic examination in women should be performed with these entities in mind. Other causes, such as herpes zoster, acute porphyria, and medication effects, should be considered as well.
Disposition
The ED workup and final diagnosis should guide the management and proper disposition of elderly patients with abdominal pain. Emergency physicians treating this high-risk group of patients should be liberal in obtaining ultrasound and/or CT imaging because of their high sensitivity for detection of most serious types of intra-abdominal pathology. Surgical consultation should be obtained emergently or urgently in all but the most benign presentations. Realizing that some serious diseases initially may present in a benign fashion, emergency physicians also should be cognizant of the importance of serial examinations over the course of the patient’s ED stay. Often, the disease process presents in a vague manner but then "declares itself" over the course of several hours. These patients are ideal candidates for admission to an ED observation unit. This certainly is not a group of patients in whom rapid ED discharge is the goal.
Even when the full ED workup has been non-diagnostic ("abdominal pain of unclear etiology") and the surgical consultant has declined admitting the patient, the emergency physician should still recognize that some serious diagnoses may not become clinically obvious in the ensuing hours to days. With this in mind, the physician has several options. The patient may benefit from admission to an ED observation unit or to the primary care physician’s service for close monitoring and continued serial examinations. Alternatively, the patient may be discharged with instructions for outpatient follow-up, if the patient has the means to return immediately should problems arise, is subjectively and objectively showing signs of improvement and tolerating oral liquids, and has a benign abdominal examination at discharge. Patients should be discharged with specific follow-up instructions and arrangements (either with the primary care physician, the consulting surgeon, or in the ED). These patients also should be instructed to return to the ED immediately if fevers, worsening or localizing abdominal pain, lightheadedness, vomiting, or new problems develop.11 Patients also should be in the company of a reliable caretaker. Finally, patients with abdominal pain of unclear etiology should never be labeled with a benign diagnosis (e.g., gastroenteritis). Explaining to the patient the uncertainty of the diagnosis helps convey to them the need for further re-evaluation as part of the ongoing diagnostic process.
Summary
The elderly patient with abdominal pain often harbors serious intra-abdominal or extra-abdominal disease. Delays or missed diagnoses of serious diseases are common in the elderly population for various reasons. Elderly patients often present to the ED in a delayed fashion and with atypical presentations of their diseases. The classic historical features of the disease that physicians expect to find often are absent. Elderly patients often, instead, present with non-specific symptoms. The physical examination may initially appear benign, even in the presence of peritonitis or vascular catastrophes. Laboratory studies can be deceiving as well: They may appear normal in the presence of significant disease, or they can falsely suggest an alternative diagnosis. Plain abdominal radiographs may be helpful if they demonstrate an obvious bowel obstruction pattern or free air under the diaphragm, but they, too, can frequently be non-diagnostic or falsely suggest an alternative diagnosis. CT has excellent sensitivity for defining the most serious intra-abdominal conditions. However, CT can be unreliable for detecting evidence of early mesenteric ischemia, and its use is inappropriate and dangerous in the unstable patient with a ruptured AAA. Bedside ultrasound, however, has good utility in the diagnosis of biliary disease and AAA.
The elderly patient with abdominal pain deserves an aggressive, rapid workup for both intra-abdominal and extra-abdominal conditions. Most patients will require ED surgical consultation. Serial abdominal examinations and even admission may be helpful for patients with a non-diagnostic workup. In the patient with abdominal pain of unclear etiology, discharge home can be considered, but only in the most benign of patients with clear discharge instructions and clear plans for early follow-up. Table 6 lists pearls that will help minimize morbidity and mortality in this high-risk patient population.
| Table 6. Clinical Pearls for Evaluation of Abdominal Pain in the Elderly | |
| • | "Classic" presentations are uncommon. |
| • | Medications may cause pathology or mask its signs and symptoms. |
| • | A diagnosis should never be excluded simply based on "normal" laboratory data or abdominal radiographs. |
| • | Appendicitis is not uncommon in elderly patients, but classic presentations of appendicitis are. |
| • | Vascular catastrophes (mesenteric ischemia and ruptured AAA) must be considered early as they have a high morbidity and mortality, and any delay in diagnosis markedly worsens prognosis. |
| • | Severe pain in the elderly patient with a paucity of physical findings should suggest mesenteric ischemia until proven otherwise. |
| • | Symptoms resembling those of renal colic in an elderly patient should prompt early consideration of a ruptured AAA. |
| • | Always consider the possibility of extra-abdominal causes of abdominal pain, especially the acute myocardial infarction. |
References
1. Baum SA, Rubenstein Z. Old people in the emergency room: Age-related differences in emergency department use and care. J Am Geriatr Soc 1987;35:398-404.
2. Brewer RJ, Golden GT, Hitch DC, et al. Abdominal pain: An analysis of 1,000 consecutive cases in a university hospital emergency room. Am J Surg 1976;131:219-224.
3. Caesar R. Dangerous complaints: The acute geriatric abdomen. Emerg Med Reports 1994;15:191-202.
4. Evans R. Physiology of aging. In: Sanders AB, ed. Emergency Care of the Elder Person. St. Louis: Beverly Cracom Publications; 1996:11-28.
5. Sherman DE, Robillard E. Sensitivity to pain in the aged. Canad M A J 1960;83:944-947.
6. Bayer AJ, Chadha JS, Farag RR, et al. Changing presentation of myocardial infarction with increasing old age. J Am Geriatr Soc 1986;34:263-266.
7. Cocchi A, Franceschini G, Incalzi RA, et al. Clinico-pathological correlations in the diagnosis of acute myocardial infarction in the elderly. Age Ageing 1988;17:87-93.
8. Cooper GS, Shlaes DM, Salata RA. Intraabdominal infection: Differences in presentation and outcome between younger patients and the elderly. Clin Infect Dis 1994;19:146-148.
9. Clinch D, Banerjee AK, Ostick G. Absence of abdominal pain in elderly patients with peptic ulcer. Age Ageing 1988;13:120-123.
10. Fenyo G. Diagnostic problems of acute abdominal diseases in the aged. Acta Chir Scand 1974;140:396-405.
11. McNamara RM. Acute abdominal pain. In: Sanders AB, ed. Emergency Care of the Elder Person. St. Louis: Beverly Cracom Publications; 1996:219-243.
12. Eisenberg RL, Heineken P, Hedgcock MW, et al. Evaluation of plain radiographs in the diagnosis of abdominal pain. Ann Intern Med 1982;97:257-261.
13. Mucha P. Small intestinal obstruction. Surg Clin North Am 1987;67:597-620.
14. Bender JS, Busuito MJ, Graham C, et al. Small bowel obstruction in the elderly. Am Surg 1989;55:385-388.
15. Day EA, Marks C. Gallstone ileus. Am J Surg 1975;128:552-558.
16. Kauvar DR. The geriatric acute abdomen. Clin Geriatr Med 1993;9:547-558.
17. Greenlee HB, Pienkos EJ, Vanderbilt PC, et al. Acute large bowel obstruction. Arch Surg 1974;108:470-476.
18. Calabrese CT, Adam YG, Volk H. Geriatric colon cancer. Am J Surg 1973;125:181-184.
19. Curless R, French J, Williams GV, et al. Comparison of gastrointestinal symptoms in colorectal carcinoma patients and community controls with respect to age. Gut 1994;35:1267-1270.
20. Avots-Avotins KV, Waugh DE. Colon volvulus and the geriatric patient. Surg Clin North Am 1982;62:249-260.
21. Ballantyne GH, Brandner MD, Beart RW, et al. Volvulus of the colon: Incidence and mortality. Ann Surg 1985;202:83-92.
22. Andersson A, Bergdahl L, Van Der Linden W. Volvulus of the cecum. Ann Surg 1976;181:876-880.
23. Rosenthal RA, Anderson DK. Surgery in the elderly: Observations on the pathophysiology and treatment of cholelithiasis. Exp Gerontol 1993;28:458-472
24. Fenyo G. Acute abdominal disease in the elderly: Experience from two series in Stockholm. Am J Surg 1982;143:751-754.
25. Morrow DJ, Thompson J, Wilson SE. Acute cholecystitis in the elderly. Arch Surg 1978;113:1149-1152.
26. Huber DF, Martin EW, Cooperman M. Cholecystectomy in elderly patients. Arch Surg 1983;146:719-722.
27. Glenn F. Surgical management of acute cholecystitis in patients 65 years of age and older. Ann Surg 1981;193:56-59.
28. Parker LJ, Vukov LF, Wollan PC. Emergency department evaluation of geriatric patients with acute cholecystitis. Acad Emerg Med 1997;4:51-55.
29. Madden JW, Croker JR, Beynon GPJ. Septicemia in the elderly. Postgrad Med 1981;57:502-506.
30. Kahng U, Roslyn J. Surgical issues for the elderly patient with hepatobiliary disease. Surg Clin North Am 1994;74:345-373.
31. Pollock EW, Ring ER. Percutaneous decompression of benign and malignant biliary obstruction. Arch Surg 1979;114:148-151.
32. Yeo CJ, Cameron JL. The pancreas. In: Sabiston DC Jr, ed. Textbook of Surgery: The Bilogical Basis of Modern Surgical Practice. 15th Ed. Philadelphia: W.B. Saunders Company; 1997:1152-1165.
33. Martin SP, Ulrich CD II. Pancreatic disease in the elderly. Clin Geriatr Med 1999;15:579-605.
34. Hoffman E, Perez E. Acute pancreatitis in the upper age groups. Gastroenterology 1959;36:675-685.
35. Leverat M. Peptic ulcer disease in patients over 60: Experience in 287 cases. Am J Dig Dis 1966;11:279-285.
36. Cooper BT, Weston CF, Newmann CS. Acute gastrointestinal hemorrhage in patients aged 80 years or more. Q J Med 1988;68:765-774.
37. Borum ML. Peptic-ulcer disease in the elderly. Clin Geriatr Med 1999;15:457-471.
38. Sanson TG, O’Keefe KP. Evaluation of abdominal pain in the elderly. Emerg Med Clin North Am 1996;14:615-627.
39. Henneman PL. Gastrointestinal bleeding. In: Rosen P, et al, eds. Emergency Medicine: Concepts and Clinical Practice. 4th Ed. St. Louis: Mosby-Year Book, Inc.; 1998:1903-1917.
40. Chappuis CW, Cohn I Jr. Acute colonic diverticulitis. Surg Clin North Am 1988;68:301-313.
41. Ponka JL, Welborn JK, Brush BE. Acute abdominal pain in aged patients: An analysis of 200 cases. J Am Geriatr Soc 1963;11:993-1007.
42. Walker JD, Gray LA Sr, Polk HC Jr. Diverticulitis in women: An unappreciated clinical presentation. Ann Surg 1977;185:402-405.
43. Bugliosi TF, Meloy TD, Vukof LF. Acute abdominal pain in the elderly. Ann Emerg Med 1990;19:1382-1386.
44. Reiss R, Deutsch A. Abdominal emergency procedures in patients above 70. J Gerontol 1985;40:154-158.
45. Rogers J. Abdominal pain. Foresight. Dallas, TX: American College of Emergency Physicians; 1986.
46. Sidman RD, Roche CN, Duggal S. Appendicitis in the elderly. Geriatr Emerg Med Reports 2000;1:91-100.
47. Horattas MC, Guyton DP, Wu D. A reappraisal of appendicitis in the elderly. Am J Surg 1990;160:291-293.
48. Hirsch SB, Wilder JR. Acute appendicitis in the hospital patients aged over 60 years, 1974-1984. Mt Sinai J Med 1987;54:29-33.
49. Owens BJ, Hamit HF. Appendicitis in the elderly. Ann Surg 1978;187: 392-396.
50. Freund HR, Rubinstein E. Appendicitis in the aged: Is it really different? Am Surg 1984;50:573-576.
51. Hals G. Acute appendicitis: Meeting the challenge of diagnosis in the emergency department. Emerg Med Reports 1999;20:71-84.
52. Rao PM, Rhea JT, Rao JA, et al. Plain abdominal radiography in clinically suspected appendicitis: Diagnostic yield, resource use, and comparison with CT. Am J Emerg Med 1999;17:325.
53. Graham A, Henley C. Laparoscopic evaluation of acute abdominal pain. J Laparoendosc Surg 1991;1:165-168.
54. Forde KA. The role of laparoscopy in the evaluation of the acute abdomen in critically ill patients. Surg Endosc 1992;6:219-221.
55. Koruda MJ. Appendicitis: Laparoscopic strategy in diagnosis and treatment. N Carol Med J 1992;53:196-198.
56. Klein HM, Lensing R, Klosterhalfen B. Diagnostic imaging of mesenteric infarction. Radiology 1995;197:79-82.
57. Boley SJ, Sprayregan S, Siegelman SS. Initial results from an aggressive roentgenological and surgical approach to mesenteric ischemia. Surgery 1977;82:848-855.
58. Stoney RJ, Cunningham CG. Acute mesenteric ischemia. Surgery 1993;114:489-490.
59. Ottinger LW, Austen WG. A study of 136 patients with mesenteric infarction. Surg Gynecol Obstet 1967;124:251-261.
60. Sachs SM, Morton JH, Schwartz SI. Acute mesenteric ischemia. Surgery 1982;92:646-653.
61. Kaleya RN, Boley SJ. Acute mesenteric ischemia: An aggressive diagnostic and therapeutic approach. 1991 Roussel lecture. Can J Surg 1992;25:613-623.
62. Boley SJ, Brandt LJ, Sammartano RJ. History of mesenteric ischemia: The evolution of a diagnosis and management. Surg Clin North Am 1997;77:275-288.
63. Newman TS, Magnuson TH, Ahrendt SA, et al. The changing face of mesenteric infarction. Am Surg 1998;64:611-616.
64. Sai Sudhakar CB, Al-Hakeem M, MacArthur JD. Mesenteric ischemia secondary to cocaine abuse: Case reports and literature review. Am J Gastroenterol 1997;92:1053-1054.
65. Manko JA, Levy PD. Mesenteric ischemia. Geriatr Emerg Med Reports 2001;2:1-12.
66. Balsano N, Cayten CG. Surgical emergencies of the abdomen. Emerg Med Clin North Am 1990;8:399-410.
67. Pierce CE, Brockenbrough EC. The spectrum of mesenteric infarction. Am J Surg 1970;119:233-239.
68. McAfee MK, Cherry KJ, Naessens JM. Influence of complete revascularization on chronic mesenteric ischemia. Am J Surg 1992;164:220-224.
69. Myer T, Klein P, Schweiger H, et al. How can the prognosis of acute mesenteric artery ischemia be improved? Results of a retrospective analysis. Zentrablatt fur Chirurgie 1998;123:230-234.
70. Murray MJ, Gonze MD, Nowak LR, et al. Serum D(-)-lactate levels as an aid to diagnosing acute intestinal ischemia. Am J Surg 1994;167:575-578.
71. Lange H, Jackel R. Usefulness of plasma lactate concentration in the diagnosis of acute abdominal disease. Eur J Surg 1994;160:381-384.
72. Kurland B, Brandt LJ, Delaney HM. Diagnostic tests for intestinal ischemia. Surg Clin North Am 1992;72:85-104.
73. Taourel PG, Deneuville M, Pradel JA. Acute mesenteric ischemia: Diagnosis with contrast enhanced CT. Radiology 1996;199:632-636.
74. Balthazar EJ, Liebskind ME, Macari M. Intestinal ischemia in patients in whom small bowel obstruction is suspected: Evaluation of accuracy, limitations, and clinical implications of CT in diagnosis. Radiology 1997;205:519-522.
75. Deehan DJ, Heys SD, Brittenden J, et al. Mesenteric ischemia: Prognostic factors and influence of delay upon outcome. J Royal Coll Surgeons Edinburgh 1995;40:112-115.
76. Gillum RF. Epidemiology of aortic aneurysm in the United States. J Clin Epidemiol 1995;48:189-1298.
77. Marston WA, Ahlquist R, Johnson G Jr, et al. Misdiagnosis of ruptured abdominal aortic aneurysms. J Vasc Surg 1992;16:17-22.
78. Salkin MS. Abdominal aortic aneurysm: Avoiding failure to diagnose. ED Legal Letter 1997;8:67-78.
79. Johansen K, Kohler TR, Nicholls SC, et al. Ruptured abdominal aortic aneurysm: The Harborview experience. J Vasc Surg 1991;13:240-245.
80. Ernst CB. Abdominal aortic aneurysm. N Engl J Med 1993;328:1167-1171.
81. Banerjee AK. Atypical manifestations of ruptured abdominal aortic aneurysms. Postgrad Med 1993;69:6-11.
82. Rutherford RB, McCroskey BL. Ruptured abdominal aneurysm: Special considerations. Surg Clin North Am 1989;69:859-868.
83. Lederle FA, Simel DL. Does this patient have abdominal aortic aneurysm? JAMA 1999;281:77-82.
84. Lederle FA, Walker JM, Reinke DB. Selective screening for abdominal aortic aneurysms with physical examination and ultrasound. Arch Intern Med 1988;148:1753-1756.
85. Siegel CL, Cohan RH, Korobkin M, et al. Abdominal aortic aneurysm morphology: CT features in patients with ruptured and nonruptured aneurysms. AJR Am J Roentgenol 1994;163:1123-1129.
86. Bessen HA. Abdominal Aortic Aneurysms. In: Rosen P, et al, eds. Emergency Medicine: Concepts and Clinical Practice. 4th Ed. St. Louis: Mosby-Year Book, Inc.; 1998:1806-1819.
87. Kuhn M, Bonnin RL, Davey MJ, et al. Emergency department ultrasound scanning for abdominal aortic aneurysm: Accessible, accurate, and advantageous. Ann Emerg Med 2000;36:213-219.
88. Shuman WP, Hastrup W, Kohler TR, et al. Suspected leaking abdominal aortic aneurysm: Use of sonography in the emergency room. Radiology 1988;168:117-119.
89. Luisani I, Perrone A, Pesavento R, et al. Prevalence, clinical features, and acute course of atypical myocardial infarction. Angiology 1994;45:49-55.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.