Identifying the Subtle Signs of Pediatric Physical Abuse
Identifying the Subtle Signs of Pediatric Physical Abuse
Part I: Bruises, Fractures, Burns, and Head Trauma
Author: Kirsten Bechtel, MD, Associate Medical Director, Child Abuse Evaluation Team, Yale-New Haven Children’s Hospital, CT.
Peer Reviewer: Georges Ramalanjaona, MD, DSc, FACEP, Associate Professor of Emergency Medicine; Associate Chairman for Academic Affairs, Department of Emergency Medicine, Seton Hall University, South Orange, NJ.
Child abuse has been documented in the United States for more than a century. The first well-publicized case occurred in 1874 and lead to the establishment of the New York Society for Prevention of Cruelty to Children.1 Despite the extensive research and education devoted to this issue, maltreatment of children continues to be a significant problem. Early identification of children with inflicted injuries is critical to optimize each child’s outcome and to prevent future injuries to both the patient and other children in the home.
The emergency department (ED) physician frequently is faced with deciding whether an injury or bruise is consistent with or excessive for the history. Understanding typical patterns of abuse, diseases, and underlying medical problems that may mimic abuse not only increases diagnostic accuracy, but also enables the physician to better protect and defend the abused child.
The author carefully reviews the characteristic patterns for physical abuse and practical clinical ways to differentiate inflicted injuries from other disease processes. This article, the first in a two-part series, gives an extensive review of bruises, fractures, burns, and inflicted head trauma. Part II of this series will address injuries to the brain, thorax, and abdomen.
— The Editor
Definitions
The term "child abuse" is interchangeable with several different terms, including child maltreatment and child victimization. The central premise of child abuse is that a child’s caregiver (i.e., a parent, guardian, or foster parent), fails to provide for that child’s health and well being, either through acts of omission or commission. Such acts can lead to future deleterious effects on the child’s health, development, and psychological well being. The Child Abuse Prevention and Treatment Act (PL 93-247), which was passed by Congress in 1974, defines child abuse as:
"The physical or mental injury, sexual abuse, negligent treatment, or maltreatment of a child under the age of 18 by a person who is responsible for the child’s welfare under circumstances which indicate that the child’s health and welfare is harmed or threatened thereby."
Between 1963 and 1968, mandated reporting laws were passed in all 50 states. A mandated reporter is an individual who is routinely responsible for a child’s health or well-being, and includes teachers, day care workers, medical personnel, and law enforcement professionals. Such individuals are required to report cases of suspected child abuse to child protective service agencies. A mandated reporter needs reasonable suspicion, not proof, of child abuse to make a report, and such individuals are protected from litigation for libel in most states. In fact, a mandated reporter may be prosecuted for failing to report suspected child abuse in some states.
Epidemiology
The purpose of the Child Abuse Prevention and Treatment Act was to establish consistent standards with respect to identification and management of child abuse. However, the incidence of child abuse in the United States continues to be difficult to ascertain because of differences in definitions of child abuse, investigation protocols, and data collection systems from state to state. This underscores the need for a uniform federal system of reporting and investigating child abuse.
In 1999, based on reports from 49 states and the District of Columbia, an estimated 3,244,000 children (47 of 1000 children) were reported to child protective service agencies for suspected abuse or neglect.2 Families who are most likely to be reported to child protective service agencies are those with a history of substance abuse, domestic violence, socioeconomic constraints (such as poverty), inadequate housing, unemployment, and poor parenting skills. Poor parenting skills may be secondary to young parental age, mental health problems, and unrealistic expectations of a child’s development.
Of these reports of suspected child abuse, an estimated 1,070,000 (15 of 1000 children) were substantiated as cases of child abuse or neglect. Of these substantiated cases, 46% were due to neglect; 18% to physical abuse; 9% to sexual abuse; 4% to emotional maltreatment and domestic violence; and 23% to other types of maltreatment, such as abandonment, threat of harm, or a combination of abuse and neglect. In 1999, based on data collection from 44 states, an estimated 1,401 children died from child abuse or neglect. The majority (80%) of these deaths were children younger than 5 years.
Unfortunately, there are numerous ways in which children are maltreated. Therefore, this article will focus on the most frequent manifestations of physical abuse: bruises, burns, fractures, and abusive head trauma, which also is referred to as "shaken baby syndrome."
Cutaneous Manifestations of Physical Abuse
Bruises. Bruises are the most common injury in physically abused children, and are a common accidental injury of childhood. There are several historical and physical features that help distinguish between accidental and inflicted bruises, but there still may be considerable overlap. Understanding the pathophysiology of bruises may help the practitioner make this distinction.
Pathophysiology. A bruise occurs when an impact to the skin’s surface results in disruption of underlying capillaries, which leads to extravasation of blood into the dermis. The force and location of impact and the complexion of the child’s skin all may contribute to the appearance of a bruise. The force of the impact may determine when a bruise is first noted. For example, superficial impacts may immediately discolor the skin, while forceful impacts that penetrate more deeply into the dermis may not appear for several days. The location of impact also plays a role in the appearance of a bruise. Bruises in locations on the body where the supporting tissue is loose and areolar, such as the genitalia and periobital regions, may appear immediately. Bruises in areas of significant muscle mass, such as the thigh, may not appear until days later, after extravasated blood has traversed the quadriceps or hamstring muscles to reach the dermis. Additionally, a child’s complexion may affect the appearance of a bruise, as bruises on children with darker complexions may not be noticable unless the skin is closely inspected.
Bruises undergo a sequence of color changes during healing, but this process may not be absolute. It was previously thought that the process of color changes was orderly and uniform, but this premise recently has been challenged.3 Many of the initial studies evaluating the sequence of color changes in bruises were performed in adult cadaver models, and the applicability of these results to that in living children has been questioned. Researchers performed a prospective analysis of the evolution of color changes in children with bruises.4 They systematically recorded the color of bruises in children who were admitted to an inpatient pediatric unit with accidental trauma. These researchers noted that the color red was apparent in bruises up to one week after injury, yellow was seen in bruises that were 1-12 days old, and green was not present in injuries fewer than 2 days old. Many of the tables regarding the age estimation of bruises that are printed in numerous textbooks have been adapted from Wilson, who recognized the imprecise nature of dating bruises and recommended that practitioners refrain from stating the precise age of a bruise.6 Acute bruises may have palpable edema and tenderness, but the precise timing of resolution of such edema and tenderness is not known. Post-inflammatory hyperpigmentation or hypopigmentation may be present for months to years after resolution of a bruise.
History and Physical Examination. The location of bruises on a child is helpful when determining whether the mechanism is accidental or inflicted. Typically, children who are not ambulatory rarely will have bruises, as their activity does not predispose them to falls unless they are left unattended. One study prospectively evaluated 973 young children who received care in several pediatric practices and found that bruises rarely were encountered in pre-ambulatory children who presented for routine well-child visits.6 Ambulatory children, such as toddlers, will frequently have bruises on areas of bony prominences, such as the forehead, knees, and elbows, as these are the regions that will be first impacted during a fall. In contrast, there are regions of the body that are well-protected in normal household falls, such as the neck, groin, and inner thigh. A history that does not include direct impact to these regions during a fall should raise the suspicion of inflicted injury.
Bruises that consist of certain highly defined patterns are suggestive of inflicted injury. (See Figure 1.) Frequently, the pattern of the bruise conforms to the implement that was used to strike the child. Implements commonly used include the hand, belts, cords, ropes, and rulers. Cords, belts, and ropes can be looped, leading to U-shaped bruises. Rigid, linear objects, such as rulers or cooking utensils, will inflict linear bruises. If the implement is applied to the child with high velocity, there may be a "negative" image of the implement, with skin that is not bruised outlined by a fine rim of petechiae that conforms to the shape of the implement.7
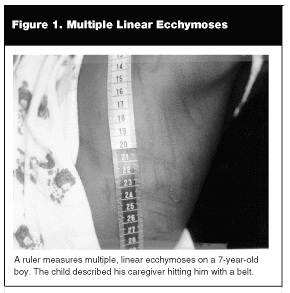 |
Bite marks lead to a highly distinctive pattern of bruises. They may appear as an arched pattern of individual tooth prints that conform to the central and lateral incisors and to the canines. If both mandibular and maxillary teeth are used to bite a child, then there will be two arched patterns that appear as a mirror image of the other. Forensic dentistry may be helpful to aid in the identification of the perpetrator based on the pattern of the bite injury. The typical distance between the mandibular canines in children is approximately 2.5 cm, while in adults this distance is usually greater than 3 cm.8 This distance between the canines should be used only as an estimate, as it may increase only 5 mm between childhood and adulthood.7 If bites are recent and the child has not bathed, they can be swabbed with a saline-soaked cotton swab and sent for DNA analysis that could potentially identify the perpetrator. Dental impressions also can be taken from alleged perpetrators and compared to the bite mark itself.
Children may be restrained during beatings, which may lead to bruises around the extremities. If the child is physically restrained, there may be isolated, circular bruises of the volar and dorsal surfaces of the arms and legs. If ligatures are used, there may be circumferential, linear bruises around the ankles or upper arms, which are occasionally accompanied by abrasions and lacerations if the ligature was tightly applied.
Conditions That May Be Confused with Inflicted Bruises. Some conditions may be confused with inflicted bruises. For example, several religious or folk medicine practices are used medically and may result in a distinctive pattern of bruising.7 One is coin-rubbing, or Cao Gaio. A coin is dipped in hot oil and rubbed vigorously over the child’s back as a treatment for medical illness. A distinctive pattern of petechial bruising on the paraspinal region of the back may result. A second healing method involves heating a glass and applying it to the skin; when removed, there can be circular petechial bruises. While these practices result in skin lesions, the caregiver’s intent was to treat the underlying medical condition, not to inflict injury.
Mongolian spots are a congenital variation in skin color and most frequently are seen in infants and children with darkly pigmented skin. They most commonly appear as slate-blue or brown-black macules on the sacrum, but also can be present on the lower extremities or forehead. Unlike bruises, there is no accompanying tenderness or edema. They fade over a period of months to years, and are distinguished from bruises by their stable, chronic appearance.
Other medical conditions associated with increased skin fragility and subsequent bruising include connective tissue disorders, such as osteogenesis imperfecta and Ehler-Danlos syndrome. Children with these disorders tend to have other suggestive stigmata, such as hypermobility of the joints and skin laxity. Systemic disorders associated with diminished coagulation, such as immune thrombocytopenic purpura (ITP), hemophilia A and B, and VonWillebrand’s disease, may result in either extensive petechiae or ecchymosis, but laboratory evaluation can distinguish these disorders from inflicted bruises. Other disorders associated with vascular inflammation, such as Henoch Schönlein purpura, results in purpuric, palpable lesions of the lower extremities and torso, the pattern of which also can be helpful to distinguish from inflicted injury.
Burns
Inflicted burns result in significant morbidity and mortality. Inflicted burns account for 25% of all hospital admissions of children with burns.9 They can be due to scald injury (in which a hot liquid is thrown at a child or a child is forcibly immersed in hot liquid) or secondary to contact injury (in which a hot implement is forcibly held against the child’s skin).
Pathophysiology. The depth and extent of a burn depends on the temperature of the implement or liquid that makes contact with the skin, as well as the duration of this contact. Burns can be characterized by the depth to which they penetrate the epidermis, dermis, subcutaneous tissue, muscle, and bone. A superficial thickness, or first-degree burn, is characterized by thermal injury to the epidermis. This typically appears as a "sunburn," with erythema of the skin and minimal pain and tenderness to palpation. As this heals, the skin may become dry and flaky; there is no scarring. Superficial thickness burns are not counted into the total body surface area of a child’s burns.
A partial-thickness, or second-degree burn, can be characterized by the depth of the dermis that is penetrated by the thermal injury. A superficial, partial-thickness burn is characterized by injury to the upper half of the dermis. These burns typically form blisters. If the roof of the blister was removed, the skin underneath would be very pink, with brisk capillary refill, and glistening, due to the exudation of serum from capillary damage. With deep, partial-thickness burns, which penetrate into the lower half of the dermis, the skin underneath the blister is paler and drier, due to more extensive capillary damage, which results in thrombosis and a speckled appearance of the skin. Both superficial and deep partial-thickness burns are uniformly painful, due to injury to cutaneous sensory nerves within the dermis. Partial-thickness burns may heal with or without scarring, depending on the extent of damage to dermal appendages (such as hair follicles and sweat glands) and result in re-epithelialization of the burn.10 Extensive damage to these dermal appendages precludes this process, resulting in the formation of granulation (scar) tissue; grafting may be necessary.
Full-thickness, or third-degree, burns are caused by thermal injury that results in destruction of both the epidermis and dermis. These burns are pale, dry, and not as painful as partial-thickness burns, due to destruction of cutaneous nerves within the dermis. These burns almost always heal with scarring and require grafting to cover the epidermal and dermal defect.
Duration of exposure and temperature has been determined to predict the likelihood of a full-thickness burn caused by hot water. (See Figure 2.) Young children typically tolerate bath water that is less than 101°F.7 Hot tub temperatures can vary between 104°F and 108°F, while water that is 110°F often will be painful to an adult.7 Water that is 120°F will cause full-thickness burns in approximately 10 minutes, while water that is 150°F will cause full-thickness burns within 2 seconds.11-12 Similar formulations for duration of exposure and temperature have not been determined for hot objects.
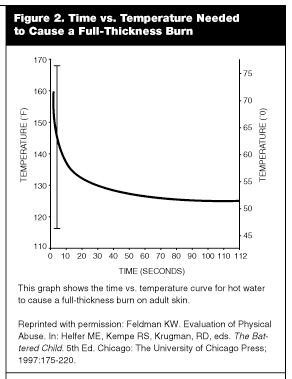 |
History. Several aspects of the history may be helpful for distinguishing accidental from inflicted burns. Accidental burns will have a clear history of contact with a hot object or liquid. Accidental burns usually occur in children whose behavior can place them within reach of potentially dangerous objects. Children who can sit and reach well may easily pull containers of hot liquid toward and onto them, especially while seated on a caregiver’s lap. Toddlers can reach up to pull such containers of hot liquid from the table, stove, or microwave down onto themselves. Older children who have the dexterity to play with and ignite matches or lighters may cause contact burns on the hands and face, and more seriously, ignite clothes or furniture.
Historical hallmarks of inflicted burns include those with no identifiable or explained mechanism, or those purported to have been inflicted by a young child who, developmentally, is incapable of performing the activity. Victims of inflicted burns tend to lack the behavioral and motor skills that place them within reach of hot objects or liquids. When such children encounter hot objects or liquids, they will try to remove themselves from contact by pulling or turning away, or attempting to climb out of a tub or sink filled with hot liquid. Victims of inflicted burns may have a history of performing a task of which they are not capable, such as a very young infant manipulating a lighter or turning on a hot water faucet.
Physical Examination. Children with accidental scald burns from hot liquids most often will have burns that are on the anterior plane of the body and will have concentric radiation of the depth of the burn.9 For example, a child who reaches up and pulls a hot liquid down onto himself may have burns on the face, chest, and arm. The point of contact of the hot liquid on the body will have the deepest burn. As the hot liquid travels down the body, it cools, leaving burns that are not as deep.9 The demarcation between normal and burned skin tends to be irregular, depending on the path that the hot liquid travels down the body. Accidental scald burns also can be caused by hot foods, which tend to be more viscous and adherent; they may prolong the time of contact with the skin and occasionally cause deeper burns than would be caused by water at a similar temperature. Clothing does not protect against the degree of burn injury, as hot liquids can soak into the fabric and prolong contact with the skin.
Scald burns that are suggestive of inflicted injury include those with clear demarcation lines, especially around the hands and feet, so called "stocking-glove" burns, as well as those that involve protected areas of the body, such as the genitalia.7,9,13 (See Figure 3.) A pattern of burn injury that is pathognomic for inflicted injury is that which involves the genitalia and lower extremities. This occurs when a child is forcibly restrained or dunked into a bathtub of hot water. As children are lowered into the water, they reflexively pull up their hips and knees, protecting the creases in the groin and popliteal fossa. The resultant burn will, therefore, involve the anterior and, to a lesser extent, posterior aspects of the lower extremities and the lower half of the torso. If the buttocks are pressed against the floor of the sink or tub, the area around the gluteal cleft may be spared, resulting in a "doughnut" burn pattern.7,13 Similarly, if the soles of the feet are pressed against the floor of the sink or tub, they may be spared as well. If the child struggles, the watermark level (the highest level to which the water immerses the body) may be irregular and wavy on the lower abdomen.7 If any part of the child’s body is rigidly restrained in the hot water, the watermark level will be rather straight.7 Children who accidentally enter a tub of hot water will not typically sit down in the water, and may alternately stand on one leg or the other until removed from the hot water. The resulting burns may involve the lower extremities only, with splash burns scattered elsewhere on the body.
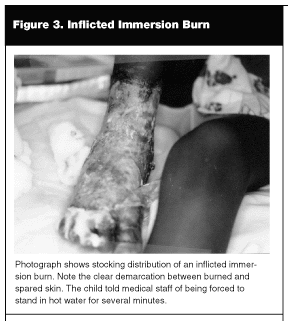 |
Accidental contact burns, as well, tend to be on the anterior plane of the body and often are solitary. When school-age children experiment with matches or cigarette lighters, there tends to be a single burn on the palmar aspect of the thumb or index fingers. When children reach out or up to touch an iron, there may be burns on the palms. If the child reached up to pull the iron down and the iron fell onto the child, there may be burns on the face, hand, arm, or foot, depending on the trajectory of the iron as it fell. Contact burns on the posterior portions or well-protected areas of the body (i.e., the genitalia, neck, axillae) are suggestive of inflicted contact burns.
Medical Conditions That May Be Confused with Abusive Burns. There are a few medical conditions that may be mistaken for abusive burns. Dermatological conditions that cause the formation of bullae or blisters include bullous impetigo and epidermolysis bullosa. In bullous impetigo, which most often is caused by Staphylcoccus aureus or Streptococcus pyogenes, bullae that are several millimeters in diameter may form. These bullae may appear in crops and coalesce together. When these bullae rupture, the base may appear as an erythematous, glistening macule that may be mistaken for partial-thickness burns due to cigarettes. The yellow crust that may appear on top of ruptured impetiginous lesions is easy to remove with water, while that of a partial-thickness burn due to a cigarette is much more adherent.13 Cigarette burns also tend to be smaller in diameter, and the center of cigarette burns often will be deeper than the periphery.
Epidermolysis bullosa is a rare, inherited condition in which large bullae can form either spontaneously or over areas of friction. Again, when these bullae rupture, they appear similar to partial-thickness burns. Both impetigo and epidermolysis bullosa are not painful, as are partial-thickness burns. Some forms of candidal and ammoniacal diaper dermatitis may be similar in appearance to a partial-thickness burn, but can be characterized by diffuse, nontender erythema of the skin surrounding the area of skin sloughing.13
Fractures
Fractures are common injuries in children who have been physically abused. Researchers found that, of 39 young children with humeral and femoral fractures, 23% were inflicted.14 A subsequent study by these same investigators of 253 fractures in children younger than 3 years of age demonstrated that 24% were due to abuse.15 While there are some fracture patterns that are pathognomic for inflicted injury, such as posterior rib fractures in a young infant, there can be much overlap among fracture patterns for both inflicted and accidental injuries. Although the fracture pattern may provide some information about the mechanism of injury, the key elements in distinguishing between accidental and inflicted fractures most often are the history of the mechanism of injury and the developmental level of the child.
History. A child who sustains a fracture most often will have a change in his or her demeanor. A child may cry, become irritable and difficult to console, or have limited use of the affected extremity. Caregivers may note that handling the infant or child in a particular way caused the child to cry or become irritable. Such a change in behavior helps pinpoint the time at which the fracture most likely occurred. Children who do not roll, pull to a stand, cruise, or walk are least likely to sustain fractures in general because their motor activity would not typically place them in a situation in which they would be at risk for fracture. Lack of witnesses, no provided mechanism of injury, or a mechanism of injury that suggests a developmental level more advanced than that which is expected are all historical factors that should raise concern for inflicted injury.
Physical and Radiological Examination. The fracture pattern may provide clues as to the mechanism of injury. Spiral fractures typically occur from twisting mechanisms. Such fractures of the long bones in children who are not ambulatory should strongly raise the possibility of inflicted injury. In some accidental cases, these fractures may occur as the caregiver grasped the child’s extremity during a fall. A history consistent with the injury should make one less suspicious of abuse.
In toddlers and younger children who are ambulatory, accidental spiral fractures of the tibia may occur when a child runs, trips, and twists the lower extremity while falling.14 Spiral humeral fractures in young, non-ambulating children historically have been considered abusive.16 There have been, however, recent case reports to suggest that such fractures may sometimes be accidental. For example, a case of a witnessed humeral fracture, which was videotaped, has been reported in an infant who rolled from the prone to supine position, entrapping the upper extremity in the process.16 In addition, linear skull fractures may be seen in short, vertical, household falls from beds, chairs, and changing tables onto firm surfaces, and when children tumble down flights of stairs.17,18
However, there are some fractures patterns that are highly suggestive for child abuse. (See Table 1.) Posterior rib fractures, such as those close to the rib neck and head, are caused by levering of the posterior rib neck over the transverse spinous process as the rib cage is vigorously squeezed.19 This fractures the inner cortex of the posterior rib neck and the postero-lateral arc of the rib. When the thorax undergoes severe anterior and posterior compression, the fracture line may extend to the anterior rib’s articulation with the sternum. (See Figure 4.)
| Table 1. Specificity of Radiologic Findings |
| High specificity |
| Classic metaphyseal lesions |
| Rib fractures, especially posterior |
| Scapular fractures |
| Spinous process fractures |
| Sternal fractures |
| Moderate specificity |
| Multiple fractures, especially bilateral |
| Fractures of different ages |
| Epiphyseal separations |
| Vertebral body fractures and subluxations |
| Digital fractures |
| Complex skull fractures |
| Common but low specificity |
| Subperiosteal new bone formation |
| Clavicular fractures |
| Long bone shaft fractures |
| Linear skull fractures |
| Reprinted with permission from: Kleinman PK. Skeletal Trauma: General Considerations. In: Kleinman PK, ed. Diagnostic Imaging of Child Abuse. 2nd Ed. St. Louis: Mosby; 1998:8-25. |
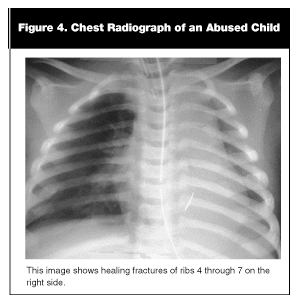 |
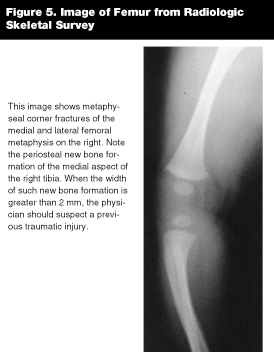
In addition, sternal fractures may be due to direct blows, and when there is no history of such trauma, are highly specific for inflicted injury.19 Metaphyseal corner fractures, also known as "bucket handle" fractures, occur due to axial traction on a child’s limbs. (See Figure 5.) As the ligamentous attachments are weaker than the ligaments themselves, the metaphsysis may be sheared, leaving the periosteum intact. Such a fracture appears as a "bucket handle."20 These fractures most often are seen at the distal regions of the long bones, such as the femur, tibia, and humerus.
 |
Multiple fractures in different stages of healing are highly suggestive of repetitive trauma and, therefore, child abuse, but also should prompt the physician to consider other causes of bony fragility that may result in a propensity for fractures. However, when multiple healing fractures are seen with other unexplained injuries, it becomes much more likely that the constellation of these injuries is due to child abuse. A further discussion of fracture healing and medical conditions with a propensity for fractures follows.
Dating of Skeletal Trauma. Fractures tend to undergo a predictable pattern of healing. This pattern, however, is dependent on the child’s age, the site of injury, and the severity of injury. When fractures first occur, there is attendant swelling due to hemorrhage and inflammation in the surrounding tissues. While symptoms of soft-tissue hemorrhage and inflammation may resolve in several days, it can be present on plain radiographs up to 10 days after the fracture occurred. Subperiosteal new bone formation can be apparent on plain radiographs as early as 4-7 days after injury, followed by loss of definition of the fracture line within 10-21 days after injury. The peak of soft callus formation is most often apparent radiographically within 10-21 days after the injury. Hard callus most often is seen within 14-42 days after injury, with complete remodeling evident at three months to one year after the injury.21
Diagnostic Imaging Strategies for the Detection of Skeletal Trauma. Occult skeletal trauma most often is seen in children younger than 2 years of age and, in this age group, a skeletal radiographic survey will have the greatest yield of detecting such trauma. A skeletal radiographic survey should not be confused with a "baby-gram" or "body-gram." These previously utilized surveys employed a one- or two-exposure study that captured the child’s entire skeleton and are inadequate to assess for occult fractures, such as metaphyseal corner fractures or posterior rib fractures. Table 2 lists the views included in a properly executed radiographic skeletal survey.
| Table 2. Views in a Radiographic Skeletal Survey22 |
| Axial skeleton |
| • Thorax (anterior/posterior [AP] and lateral views) |
| • Pelvis (AP view) |
| • Lumbar and cervical spine (lateral views of each) |
| • Skull (frontal and lateral views) |
| Appendicular skeleton |
| • Humeri (AP view of each) |
| • Forearms (AP view of each) |
| • Hands (Oblique posterior/anterior view of each) |
| • Femurs (AP views of each) |
| • Lower legs (AP views of each) |
| • Feet (AP views of each) |
It may be useful to repeat the skeletal survey several weeks after the initial study, as some fractures can be detected only when healing. One study found that a second skeletal survey demonstrated additional injuries in 14 of 23 (61%) young children evaluated for suspected abuse.23 Many of these additional injuries included metaphyseal and rib fractures.
Skeletal scintigraphy, or radionuclide bone scans, may be a helpful adjunct to plain radiography. Skeletal scintigraphy may be more sensitive in detecting acute fractures that are not well seen on plain radiographs, such as rib fractures. However, there are several disadvantages to skeletal scintigraphy. Any abnormality detected on skeletal scintigraphy requires a plain radiograph of that region to further delineate the abnormality. Skeletal scintigraphy frequently requires a motionless patient, and sedation may be necessary. The dose of radiation, especially to the gonads, is much higher with skeletal scintigraphy than with plain radiography. In addition, inter-observer agreement with respect to the findings on skeletal scintigraphy may be only as high as 68%, while that of plain radiographs can be as high as 80%.24 Finally, the cost of skeletal scintigraphy can be as much as 300% of that of plain radiography used in a skeletal survey.25
Medical Conditions with Propensity to Fractures. There are several acquired and congenital medical conditions that may lead to bony changes or fractures that could be confused with abusive fractures.26 One such condition is osteogenesis imperfecta, a rare, inherited condition that results in bony fragility and propensity for fractures with routine handling or minor trauma. Children with such medical conditions may present with radiographic findings of multiple fractures in different stages of healing. The hallmark of this disorder is a genetic mutation resulting in the abnormal synthesis of Type 1 collagen. Most cases are inherited in an autosomal dominant fashion, though cases due to spontaneous mutation also may occur.7 Other clinical features, such as ligamentous laxity, skin elasticity, and an increased tendency for bruising often are present. Osteogenesis imperfecta Type I is the most common manifestation, occurring in 3.5 of 100,000 births.7 Affected children often will have wormian bones of the skull, grayish blue sclera, hearing abnormalities, and dental maldevelopment.26 Osteopenia often will be present on skeletal radiographs. Osteogenesis imperfecta Type 4 is the type most often confused with inflicted trauma, but also is quite rare and accounts for fewer than 5% of all cases. Such children may not have osteopenia, gray-blue sclera, or dental maldevelopment, but most often will have a triangular facies with prominent temporal regions.26 In cases in which it is difficult to distinguish osteogenesis Type 4 from child abuse, serial radiographic surveys may be helpful. Children with any type of osteogenesis imperfecta will continue to develop fractures, while those who have been abused will not. Fibroblast assays for Type 1 collagen may be useful in questionable cases, but rarely are more helpful than a thorough history and physical examination by a knowledgeable practitioner.27
Another cause of increased bony fragility and propensity for fractures is osteopenia of prematurity. This propensity for fractures is due to low intake, poor absorption, or renal excretion of calcium and phosphorous. Researchers evaluated 973 hospitalized premature infants younger than 6 months of age and found the incidence of fractures to be 1.2%.28 Infants at highest risk for fractures were those who weighed fewer than 1500 grams at birth, received prolonged parenteral nutrition or furosemide therapy, or had cholestatic jaundice or bronchopulmonary dysplasia. Fractures typically involved the long bones, ribs, or metaphyses.
Nutritional rickets can lead to bony lesions that may be confused with metaphyseal fractures. A recent study demonstrated that the infants typically affected were African-American, breast-fed, and between 5 and 25 months of age. They typically did not receive supplemental vitamin D.29 All of the infants in this sample had radiological findings of widening of the growth plate; fraying, cupping and irregularity of the metaphysis; and osteopenia. In addition, all patients were hypophosphatemic as well.
A normal radiographic variant that may be confused with a healing fracture is physiologic subperiosteal new bone formation of young infants. This finding has been well documented and most often involves the long bones. The incidence of such findings in healthy infants has been estimated to be as high as 47%.30 Radiographic findings include a smooth band of mineralized density separated from the underlying cortex of the shafts of long bones by a band of radiolucency. This finding most often is seen in infants between 1 and 4 months of age, and can be distinguished from healing fractures when the width of such new bone formation is fewer than 2 mm.30 Other medical conditions that result in bony lesions and can be confused with inflicted fractures include congenital syphilis, osteomyelitis, and myelodysplasia.
Abusive Head Trauma
While trauma is the most common cause of death in childhood, abusive head trauma is the most common cause of traumatic death in infancy. Since the 1940s, the features of abusive head trauma, also known as shaken baby or shaking-impact syndrome, have been well established.
In 1946, pediatrician Robert Salinger characterized the original "battered babies."31 He described a nurse who confessed to killing three infants and injuring many more in her care. She would become angry and frustrated about an infant’s crying and proceeded to grab the child about the chest or between the shoulders and elbows and shake him violently until the infant ceased to cry. Autopsies on two of these infants revealed diffuse subdural hemorrhage over both cerebral hemispheres.
The biomechanical forces necessary to cause this spectrum of injuries only recently have been understood. In 1972, one author described the "whiplash shaken infant syndrome," and attributed the pathogenesis of the injuries, subdural hemorrhage and retinal hemorrhage, to rotational deceleration forces of the head.32 Such forces cause the dura to slide along the surface of the brain, rupturing the vessels in the subdural space. Similarly, the vitreous humor slides along the surface of the retina, disrupting the vessels that course between the layers of the retina, resulting in diffuse retinal hemorrhages.33
There has been some disagreement among those who care for children with abusive head trauma as to whether shaking alone or shaking and impact is necessary to cause this spectrum of injuries. In 1987, researchers constructed a biomechanical infant model and demonstrated that the forces necessary to cause concussion and subdural hemorrhage were generated only when the infant model was shaken and impacted a fixed, hard surface.34 Such evidence of impact injury to the head may not be apparent on initial examination, and only may be recognized when the scalp is shaved or the galea exposed during surgery.35 Other investigators have suggested that vigorous, violent shaking alone generates the force necessary to cause these injuries. One group reviewed the autopsies of children who died from abusive head trauma and found that 9% did not have any evidence of focal injury to the scalp, skull, or dura.36
History. Caregivers who inflict these injuries are sometimes unaware that they injured the child. However, a competent observer to such injuries would realize that the caregiver’s actions would injure the child. Infants and children often are shaken due to a caregiver’s unrealistic expectations of the infant or child or as a disproportionate response to increasing levels of frustration. In some instances, it may be difficult to determine if the caregiver’s intent was to inflict harm or to simply stop the infant or child from crying. Recent studies have demonstrated that perpetrators who injure children in this manner are most likely to be fathers, male paramours, female babysitters, or mothers, in descending order.37
The histories provided by caregivers may be vague, such as "I found him like this when he awoke from a nap." There may be suggestion of a remote, poorly defined event, such as "He may have fallen off the couch yesterday" or to a minor fall, such as " He fell and hit his head on the ground" or " He hit himself in the head with a toy." There is a large body of literature to support the concept that household falls or falls down stairs rarely result in life-threatening brain injury, except if a space-occupying lesion, such as an epidural or large intracranial hemorrhage, is present.10,17,38
Children with abusive head trauma can have a wide spectrum of symptoms and signs. Children with milder injuries may have only irritability, vomiting, poor feeding or sleepiness. These are symptoms that overlap with myriad common pediatric illnesses, and thus these children might not be recognized to have sustained an inflicted head injury. Children with more severe injuries often present with more ominous symptoms and signs, such as apnea, unresponsiveness, seizures, or cardiopulmonary arrest. The highest incidence of abusive head trauma is in children younger than 6 months of age, due to their proportionally larger head, weak neck muscles, and poor head control; however, varying degrees of injury can be seen in children up to 2 years of age.35 Older, but physically smaller, children with developmental delays also can suffer from these injuries.
The observation that the diagnosis of abusive head trauma may be overlooked in children with milder symptoms was supported by a study in 1999.39 These investigators reviewed the medical records of 173 children younger than 3 years of age with inflicted head trauma. They found that 54 children (31%) had a medical evaluation shortly after sustaining inflicted head trauma, but the clinician failed to recognize that the child had been injured in this manner. Children who were most likely to have a missed diagnosis of abusive head trauma were very young (< 6 months), Caucasian infants who came from families in which both parents lived in the home. This group of infants had less dramatic symptoms, as they did not have respiratory compromise or seizures, and were more likely to have only irritability or vomiting.
Physical Examination. On physical examination, there may not be obvious signs of trauma to the head, neck, or chest. Scalp contusions may be seen only when the head is shaved or when the scalp is exposed during craniotomy.35 The extent of brain injury largely determines the signs and symptoms a child may have. There may be focal neurological signs, such as hypertonicity or flaccidity, gaze palsies, or unequal pupils. The child may be irritable or unresponsive to pain. Focal or generalized seizures may be apparent. Cardiopulmonary arrest may be due to significant brain injury, either from direct deceleration injury to the brainstem and upper cervical cord or from subsequent hypoxia and ischemia from cerebral edema.35
Retinal hemorrhages are present in anywhere from 60% to 95% of patients with abusive head trauma.33,35 They may sometimes be appreciated on direct ophthalmoscopy without mydriatics, but often the true extent of such may only be appreciated with dilated, indirect ophthalmoscopy. Typically, retinal hemorrhages seen in those children with abusive head trauma are multiple and often extend to the periphery.33,35 They can occur in multiple layers of the retina, most often in the nerve fiber and ganglion cell layers, and appear to be flame-shaped. Intraretinal and preretinal hemorrhages more are often dot-, blot-, or boat- shaped hemorrhages.33 Retinal hemorrhages may either be unilateral or bilateral. Retinoschesis, internal splitting of the retina, macular folding, and vitreous hemorrhage are other retinal abnormalities often associated with abusive head trauma.33,35
On occasion, retinal hemorrhage may be seen in head injuries associated with accidental mechanisms. A recent case series by one group documented three cases of accidental falls and found that retinal hemorrhages were present on the same side as the subdural hemorrhage.40 However, the retinal hemorrhages noted in this case series were isolated to the posterior pole of the retina, did not cover a significant surface area of the retina, did not extend to the periphery, and were not accompanied by retinal folds or detachment. In contrast, retinal hemorrhages seen in cases of abusive head trauma are diffuse and extend to the periphery of the retina. When such hemorrhage is associated with retinal folding or detachment or retinoschesis, this is thought to be highly suggestive of abusive injury.
Cardiopulmonary resuscitation typically does not cause retinal hemorrhages. Researchers performed dilated indirect ophthalmoscopy on hospitalized children who underwent at least one minute of closed chest compressions during cardiopulmonary resuscitation. Of the 43 patients studied, only one patient had retinal hemorrhages, which were few in number. This patient also had evidence of activated coagulation at the time of the ophthalmoscopic examination.41 Retinal hemorrhage may be seen in up to 30% of infants shortly after birth, but typically resolves by 6 weeks of age.42
Radiographic Evaluation. Computed tomography (CT) is the most rapid, reliable tool in the diagnosis of abusive head trauma. Acute subdural and subarrachnoid hemorrhages, the most common brain injuries seen in children with abusive head trauma, can be readily appreciated on CT by experienced clinicians. Typically, a subdural hemorrhage can be thin and extensive, but occasionally be large enough to cause mass effect.43 There is a high propensity for the subdural hemorrhage to involve the interhemispheric fissure, but it also can involve the convexities and be unilateral or bilateral.35,43 Subarachnoid hemorrhages usually are multifocal and most often can be seen along the falx or the tentorium.7 Skull fractures also can be detected by CT scan and suggest impact of the head onto a fixed, hard surface. Skull fractures most often are linear, but also can be stellate or diastastic.
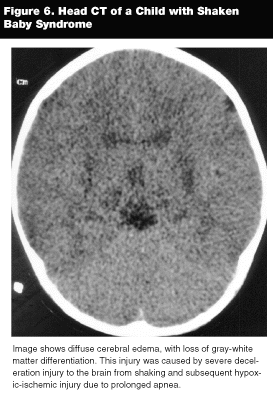
Children with more severe deceleration injury to the brain may have evidence of diffuse cerebral edema and diffuse axonal injury. This may appear as a reversal of the differentiation between the gray and white matter, also known as the "reversal sign."20 (See Figure 6.) The gray matter will, therefore, appear less dense than the deeper gray matter structures of the basal ganglia and brain stem, as well as the white matter. Diffuse axonal injury arises from shearing injuries to the structures along the gray-white matter interface. Acute, punctate hemorrhage may be present along the gray-white matter junction of the gyri, the corpus callosum, or the basal ganglia.20
 |
Magnetic resonance imaging (MRI) may be useful to detect small, extra-axial fluid collections not appreciated on CT scans, diffuse axonal injury, and to narrow the window of time in which the injury occurred.20 MRI can be difficult to obtain in children requiring mechanical ventilation and inotropic support, and should be considered as an adjunct to CT scans.
Other hallmarks of shaking injury include posterior and anterolateral rib fractures and metaphyseal fractures. When children present acutely with brain injury due to shaking, these injuries may not be readily detected on plain radiographs. At the time of the acute injury, such fractures may not have overlying tenderness, edema, or crepitus, and there may not be loss of function of the involved extremity. Such fractures may be detected only with skeletal scintigraphy, which can be difficult to obtain in children who have significant brain injury that requires mechanical ventilation and inotropic support. Plain radiography obtained within 10 days of initial presentation may be the only modality to demonstrate these fractures in this sicker group of patients with abusive head trauma.20 When these fractures are present with the previously described central nervous system and retinal findings, this constellation of injuries is pathognomic for abusive head trauma.
Outcome. Long-term outcome of survivors of abusive head trauma tends to be poor, and is dependent on the severity of symptoms on initial presentation.44-46 Children who present with apnea, seizures, and coma are more likely to have long-term neurologic sequelae such as developmental delay, seizures, and static encephalopathy. The overall mortality from such injuries can be as high as 25%.44
Closed Head Trauma That May Be Confused with Abusive Head Trauma. Some children who have contact injuries to the head, either from short vertical falls or blows to the head, may sustain an epidural hemorrhage, subdural hemorrhage, or cerebral contusion. When there is a contact injury to the head, the point of impact causes the inner table of the skull to bend inward, putting it under compression, which may injure blood vessels within the epidural or subdural space, as well as the parenchyma of the brain itself.47 These focal injuries may be accompanied by a skull fracture. At the same time of this inbending of the skull, there also is simultaneous outbending of the skull around the site of impact.47 This puts the outer table of the skull under tension, and a skull fracture may result, either proximate to or remote from the site of impact. As the skulls of infants are somewhat more elastic, the tension on the outer table of the skull as it bends outward from an impact site may not always result in a fracture.47
These children typically do not present with significant alterations in mental status, unless the epidural hematoma or subdural hematoma is large enough to cause mass effect and focal cerebral edema.47 In contrast to children who have head injury due to shaking, the outcome of children with subdural hemorrhage due to impact injury is typically good, as the hemorrhage most often is not extensive and spontaneously resolves within 48 hours after injury, with little neurological sequelae.48
ED Management of Children
with Suspected Abuse
When an ED clinician suspects that a child’s injury is due to maltreatment, it is helpful to have an objective approach and to have clear, concise documentation. When obtaining a history from the caregiver, it is important to be thorough and deliberate. One can begin by asking such questions as:
1. When did the caregiver note that the child was injured?
2. What was the child doing immediately before the injury?
3. How did the child behave immediately after the injury?
4. What were the caregiver’s actions after the injury?
5. When did the caregiver decide to take the child to the ED?
6. What factors made the caregiver take the child to the ED?
7. Were there any witnesses to the child’s injury?
For verbal children, it also is helpful to question them separately about how they were injured, using open-ended, developmentally appropriate questions. Such questions allow the child to explain what happened in a narrative form. Good examples of such open-ended questions are:
1. Can you tell me what happened (to your head, arm, etc.)?
2. Why did you have to come to see the doctor today?
3. Is there anything that is worrying you right now?
Try to avoid leading or suggestive questions, such as, "Did Mommy hit you?" These are questions that typically result in a yes or no answer. On occasion, such questions may be necessary if a child does not respond to open-ended questions.
When it becomes clear that abuse or neglect is the most likely cause of a child’s injuries, it is helpful to have a plan to ensure the child’s safety in the ED. On some occasions, the caregiver may attempt to flee the ED with the child and, therefore, appropriate personnel should be stationed at nearby exits. It is sometimes helpful to meet with the caregiver independently and provide a clear explanation for why abuse is suspected. Preparations should be made to deal appropriately with the caregiver’s response. Simultaneous notification of child protective services should be done, and information regarding the severity of the child’s injuries, the discrepant history, and the clinician’s assessment of the risk of further injury to the child should be concisely conveyed to child protective services workers and law enforcement personnel. In addition, the child’s primary care provider can be a useful source of information and also should be notified of referral of the child and family to child protective agencies.
Clear, concise, and legible documentation of the history, physical examination, and radiological and laboratory findings should be part of the ED medical record. It also is helpful to document the caregiver’s or child’s statements about the injury, putting quotation marks around the exact words of their statements. In many jurisdictions, any statements made to medical personnel during the course of evaluation and treatment of a medical condition are exempt from hearsay laws. When possible, all physical examination findings should be clearly documented, with attention to the shape, color, and dimensions of the injury. It also is helpful to note the child’s growth parameters and when possible, to review primary care records, noting any delays in immunizations or missed well-child care appointments. The child’s primary care provider can confirm such information. Medical photography also is helpful to depict accurately injuries at the time of the ED evaluation. The photograph should include identifying information of the child, such as name, date of birth, and date of the photograph. A size standard, such as a ruler, or a well-recognized object, such as a coin, is helpful to depict the size of an injury in the photograph.
When child abuse is thought to be the most likely cause of a child’s injury, the ED clinician must make a determination, in conjunction with child protective service workers, as to the child’s safety and the likelihood of further injury if the child returns home. In some cases, when immediate placement into foster care, either with a relative or designated foster care parent, is not possible, it may be necessary to admit the child to the hospital until such a safe environment is secured for the child. Such decisions as to imminent risk of injury should the child remain with the caregiver thought to have caused the injuries and appropriate placement of the child into a safe environment should be concisely documented in the ED medical record.
Summary
Child abuse continues to be a significant problem in the United States. When children present to ED with injuries, one must consider child abuse as part of the differential diagnosis. The diagnosis of child abuse can be difficult to make, as the history of the mechanism of injury may be false or misleading, especially in young children who are not capable of providing such history themselves. The spectrum of inflicted injury is large, but the most common inflicted injuries are bruises, burns, fractures, and head injuries. In rare instances, some medical conditions share clinical features with inflicted injuries, and evaluation to exclude such conditions should be undertaken when necessary. Documentation in the ED medical record of the history and physical examination in cases of suspected child abuse must be legible and complete. Photographic or diagrammatic representation of injuries should be done, with attention to size, location, and color of injuries. As mandated reporters, ED clinicians must have reasonable suspicion, not proof, of child abuse to make a report to child protective service agencies. It is easy to fail to recognize child abuse if one does not consider it as part of the differential diagnosis of a child’s injuries.
References
1. Ten Bensel RW, Rheinberger MM, Radbill SZ. Children in a World of Violence: The Roots of Child Maltreatment. In: Helfer ME, et al, eds. The Battered Child. 5th Ed. Chicago: The University of Chicago Press; 1997:3-28.
2. Peddle N, Wang CT. Current Trends in Child Abuse Reporting and Fatalities: The Results of the 1999 Annual Fifty State Survey. Chicago, Ill: National Committee to Prevent Child Abuse; 2001.
3. Schwartz AJ, Ricci L. How accurately can bruises be aged? Pediatrics 1996; 97:254-256.
4. Stephenson T, Bialas Y. Estimation of the age of bruising. Arch Dis Child 1996;74:53-55.
5. Wilson EF. Estimation of the age of cutaneous contusions in child abuse. Pediatrics 1977;60:750-752.
6. Sugar NF, Taylor JA, Feldman KW, et al. Bruises in infants and toddlers: Those who don’t cruise rarely bruise. Arch Pediatr Adolesc Med 1999;153:
399-403.
7. Feldman KW. Evaluation of Physical Abuse. In: Helfer ME, et al, eds. The Battered Child. 5th Ed. Chicago: The University of Chicago Press; 1997:
175-220.
8. Jessee SA. Recognition of bite marks in child abuse cases. Pediatr Dent 1994;16:336-339.
9. Giardino AP, Christian CW, Giardino ER. Bruises and Burns. In: Giardino AP, et al, eds. A Practical Guide to the Evaluation of Child Physical Abuse and Neglect. Thousand Oaks, CA :SAGE Publications; 1997:74-94.
10. Joffe M. Burns. In: Fleisher GR, et al, eds. Textbook of Pediatric Emergency Medicine. 4th Ed. Philadelphia: Lippincott, Williams and Wilkins; 2000:
1427-1434.
11. Moritz AR, Henriques FC. Studies of thermal injury: The relative importance of time and temperature in the causation of cutaneous burns. Am J Path 1947;23:695-720.
12. Katcher ML. Scald burns from hot tap water. JAMA 1981;246:1219.
13. Richardson A. Cutaneous Manifestations of Abuse. In: Reece R, ed. Child Abuse: Medical Diagnosis and Management. Malvern, PA: Lea and Febinger; 1994:167-184.
14. Thomas SA, Rosenfield NS, Leventhal LM, et al. Long-bone fractures in young children: Distinguishing accidental injuries from child abuse. Pediatrics 1991;88:471-476.
15. Leventhal JM, Thomas SA, Rosenfield NS, et al. Fractures in young children: Distinguishing accidental injuries from child abuse. Am J Dis Child 1993;147:87-92.
16. Hymel KP, Jenny C. Abusive spiral fractures of the humerus: A videotaped exception. Arch Pediatr Adolesc Med 1996;150:226-228.
17. Helfer RE, Slovis TL, Black M. Injuries resulting when small children fall out of bed. Pediatrics 1977;60:533.
18. Joffe M, Ludwig S. Stairway injuries in children. Pediatrics 1988;82:451-461.
19. Kleinman PK. Skeletal Trauma: General Considerations. In: Kleinman PK, ed. Diagnostic Imaging of Child Abuse. 2nd Ed. St. Louis: Mosby; 1998:8-25.
20. Smith WL. Imaging in Child Abuse. In: Helfer ME, et al, eds. The Battered Child. 5th Ed. Chicago: The University of Chicago Press; 1997:221-247.
21. O’Connor JF, Cohen J. Dating Fractures. In: Kleinman PK, ed. Diagnostic Imaging of Child Abuse. 2nd Ed. St. Louis: Mosby; 1998:168-177.
22. American Academy of Pediatrics. Diagnostic imaging of child abuse. Pediatrics 2000;105:1345-1348.
23. Kleinman PK, Nimkin K, Spevak MR, et al. Follow-up skeletal surveys in suspected child abuse. Amer Journ Roentgen 1996;167:893-896.
24. Conway JJ, Collins M, Tanz RR, et al. The role of bone scintigraphy in detecting child abuse. Semin Nucl Med 1993;23:321-333.
25. Kleinman PK. Skeletal imaging strategies. In: Kleinman PK, ed. Diagnostic Imaging of Child Abuse. 2nd Ed. St. Louis: Mosby; 1998:237-241.
26. Lachman RS, Krakow D, Kleinman PK. Differential Diagnosis II: Osteogenesis Imperfecta. In: Kleinman PK, ed. Diagnostic Imaging of Child Abuse. 2nd Ed. St. Louis: Mosby; 1998:197-213.
27. Steiner RD, Pepin M, Byers PH. Studies of collagen synthesis and structure in the differentiation of child abuse from osteogenesis imperfecta. J Pediatr 1996;128:542-547.
28. Amir J, Katz K, Grunebaum M, et al. Fractures in premature infants. J Pediatr Orthop 1988;8:41-44.
29. Kreiter SR, Schwarz RP, Kirkman HN, et al. Nutritional rickets in African American breast-fed infants. J Pediatr 2000;137:153-157.
30. Kleinman PK. Kwan DS. Differential diagnosis: Normal variants. In: Kleinman PK, ed. Diagnostic Imaging of Child Abuse. 2nd Ed. St. Louis: Mosby; 1998:178-196.
31. Caffey J. The whiplash shaken infant syndrome: Manual shaking by the extremities with whiplash induced intracranial and intraocular bleedings, linked with residual permanent brain damage and mental retardation.
Pediatrics 1974;54: 396-403.
32. Caffey J. On the theory and practice of shaking infants. Am J Dis Child 1972;124:161-169.
33. Annable WL. Ocular manifestations of child abuse. In: Reece R, ed. Child Abuse: Medical Diagnosis and Management. Malvern, PA: Lea and Febinger; 1994:138-149.
34. Duhaime AC, Gennarelli TA, Thibault LE, et al. The shaken baby syndrome. J Neurosurg 1987;66:409-415.
35. Duhaime AC, Christian CW, Rorke LB, et al. Nonaccidental head injury in infants—The "shaken baby syndrome." N Engl J Med 1998;338:1822-1829.
36. Gilliland MG, Folberg R. Shaken babies—Some have no impact injuries.
J Forens Sci 1996;41:114-116.
37. Starling SP, Holdern JR. Perpetrators of abusive head trauma: A comparison of two geographic populations. South Med J 2000;93:463-465.
38. Duhaime AC, Alario AJ, Lewander WJ, et al. Head injury in very young children: Mechanisms, injury types and ophthalmologic findings in 100 hospitalized patients younger than 2 years of age. Pediatrics 1992;90:179-185.
39. Jenny C, Hymel KP, Ritzen A, et al. Analysis of missed cases of abusive head trauma. JAMA 199;281:621-626.
40. Christian CW, Taylor AA, Hertle RW, et al. Retinal hemorrhages caused by accidental household trauma. J Pediatr 1999;135:125-127.
41. Odom A, Christ E, Ken N, et al. Prevalence of retinal hemorrhages in pediatric patients after in-hopsital cardiopulmonary resuscitation: A prospective study. Pediatrics 1997;99:E31-35.
42. Levin AV. Ocular manifestations of child abuse. Ophthalmol Clin North Am 1990;3:249-258.
43. Barnes PD, Robson CD. CT findings in hyperacute nonaccidental brain injury. Pediatr Radiol 2000;30:74-81.
44. Duhaime AC, Christian C, Moss E, et al. Long-term outcome in infants with shaking-impact syndrome. Pediatr Neurosurg 1996;24:292-298.
45. Haviland J, Ross RI. Outcome after severe non-accidental head injury. Arch Dis Child 1997;77:504-507.
46. Gilles EE, Neslon MD. Cerebral complications of non-accidental head injury in childhood. Pediatr Neuro 1998;19:119-128.
47. Hymel KP, Bandak FA, Partington MD, et al. Abusive head trauma? A biomechanics based approach. Child Maltreat 1998;3:116-128.
48. Duhaime AC, Christian C, Armonda R, et al. Disappearing subdural hematomas in children. Pediatr Neurosurg 1996;25:116-122.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
