Poor communication: Root of most patient safety ills
Poor communication: Root of most patient safety ills
Change culture, improve patient satisfaction
A 54-year-old man presented to the ED with chest pain, and the emergency physician performed an initial evaluation, including an electrocardiogram and cardiac markers, but they didn’t reveal a diagnosis.
As the doctor continued to work on his differential diagnosis, the patient was having problems maintaining his blood pressure, so the physician considered the possibility of a thoracic aortic dissection. As a result, he took the chart and, according to him, notated in the order section that he wanted a computed tomography (CT) scan of the chest with infusion, and gave it to the clerk.
The order was not put in. The clerk said she never saw the order and didn’t believe it was communicated to her.
Two hours later, the patient was still in the ED and had not gone for a CT scan. The physician, upon realizing this, ran to the nurse and clerk to get the scan performed. The patient went down for a CT scan, and he died in the room. In court, the emergency physician pointed a finger at the clerk and vice versa. The jury believed the clerk.
The verdict was more than $2 million, according to Daniel J. Sullivan, MD, JD, FACEP, president of the Sullivan Group, a consulting company in Oak Brook, IL.
As this example clearly illustrates, poor communication in the ED can have dire consequences. In fact, poor communication between health care professionals is the root cause of nearly seven of 10 sentinel events, according to the Joint Commission on Accreditation of Healthcare Organizations — and nowhere is communication more critical than in the ED. According to the Joint Commission, there were a total of nearly 500 sentinel events in 2003 and more than 400 in 2002. (See chart, below.)
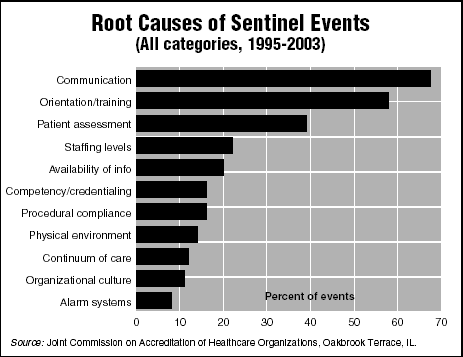
"The ED is a high-stress, high-risk environment where there is not a lot of room for mistakes," says Marc Taub, MD, FACEP, chairman and medical director of the ED at South Coast Medical Center in Laguna Beach, CA, and director of team training for California Emergency Physicians, an emergency physician partnership that includes more than 600 emergency physician partners in California.
Taub points to the pilot, co-pilot, crew model. "No one can possibly know everything that’s going on, so if there’s not good communication between staff and nurse and physician, there will be things [the physician] will not know about," he says. The physician’s decision-making ability and patient safety will be diminished, Taub adds.
Attitude is an important component of communication, adds Diana S. Contino, RN, MBA, CEN, CCRN, a consultant with MedAmerica, an Oakland, CA-based medical practice support company for emergency services, and owner of Emergency Management Systems, a Laguna Niguel, CA-based consulting firm that specializes in staffing issues.
"A nurse will be reluctant to approach a physician who unapproachable, and vice versa," Contino says. "It makes them less likely to solicit information from one another."
Whether you communicate openly should not be an option in the ED, says Taub. "You must open lines of communication and constantly work to improve," he advises. "Even when people have information they may not think is that important, it should be brought to the decision makers." For example, a registration clerk might hear a patient mentioning a suicidal plan. "That information should be brought immediately to the physician or nurse caring for the patient," Taub says. "Don’t assume they already know."
On the flip side, he says, decision makers should share what they’re thinking and planning and ask for input from others. "By communicating to others, it allows them be more proactive and helps you achieve your goals," he says.
Taub recommends that after seeing a patient, physicians share their impression and treatment plan directly with the patient’s nurse. For example, a physician could say, "I saw Mr. Jones in bed 8 and don’t think he’s having cardiac chest pain, but given his age and risk factors, I’m going to order a cardiac work-up. Any other thoughts or concerns?"
In addition, he says, it must be recognized that although physicians and charge nurses are the designated leaders, at any time anyone may become a situational leader. "For example, if multiple critical patients are in the ED simultaneously, a nurse or technician may need to step up to the plate and assume temporary leadership for a patient while waiting for the physician," Taub notes.
Better communication is built upon what Contino calls key tenets:
• Create systems that foster double-checks for verbal orders and clarification of written orders if they are illegible or don’t match the patient or their clinical presentation.
• Track and trend errors. Encourage reporting of errors and omissions in the ED. For example, if you have a large number of people giving the wrong drug accidentally, and you track and trend those errors, you can communicate specific information to staff and set up a different method of archiving or listing that medicine.
• Promote optimal communication through a multitude of channels. This communication can include written or verbal communication, postings, e-mail, one-on-one conversation, feedback to staff, educational events, telephone conversations, and meetings. "You have to set up a culture that fosters open and respectful communication between the clinicians, the lab, the pharmacy, radiology, and so on," says Contino.
• Hold people responsible for their interpersonal actions. "We all know people who get angry and then apologize, but never control their anger," Contino observes.
Communication in the form of personal coaching and/or mentoring can help, she says. This communication can be provided by professional coaches/mentors and hospital staff members who are exceptional leaders, she suggests.
• To promote patient safety, remove blame and look for solutions. Pursue more thoughtful reflection on situations rather than individuals. If a patient is discharged with the wrong prescription, don’t attack the discharging nurse, Contino suggests. Instead, evaluate the process to see how it happened and work with staff to set up processes to minimize the chance for this occurring in the future, she advises.
• Give staff the tools to improve. This includes a feedback loop, says Contino.
"You need to catch them being good; acknowledge and reward the things they do," she advises.
Rewards can include thank-you letters, gift certificates, or meal tickets good for free food in the hospital cafeteria.
Principles such as insisting on open communication’ sound fine in theory, but how do you translate that theory into reality?
Taub’s hospital and five others affiliated with California Emergency Physicians implemented a program called MedTeams, a teamwork training course from Dynamics Research Corp. in Andover, MA. The course teaches teamwork principles, including communication, based on a model used in high-risk industries. (For more information, see resources, below.) The program is based on error reduction, teamwork, specific behaviors, and cultural change.
The course begins by recognizing human fallibility, Taub says. In this new paradigm, everyone is encouraged to feel confident and empowered to bring information forward. In this culture, "It is no longer good to have a hierarchy if patient safety is involved," he explains.
Taub points to two specific behaviors he says have been instrumental in improving performance:
• Interdisciplinary rounds or briefings. Scheduled after each shift, these include physicians, nurses, registration, and anyone else who worked on the shift.
"The physician leads a quick briefing on all available information on each patient, as well as logistics, such as are we on diversion, bed issues, and so on," Taub explains. "It’s like a pre-flight briefing." And, he notes, no pilot would ever take off without a pre-flight briefing.
• Conflict management. "You want to get away from notes like Doctor so and so was aware . . .’" Taub explains. "If you have a concern, go to the physician and voice the concern. We give staff a specific script to voice concerns, and as in aviation, if the concern is not answered, we have a double-challenge rule; you can go back a second time."
Sources and Resources
For information on improving communication, contact:
- Diana S. Contino, RN, MBA, CEN, CCRN, Owner, Emergency Management Systems, 51 Hancock St., Laguna Niguel, CA 92677, Phone: (510) 835-7405. E-mail: [email protected].
- Daniel J. Sullivan, MD, JD, FACEP, The Sullivan Group, 2000 Spring Road, Suite 200, Oak Brook, IL 60523. Phone: (630) 990-9700. Web: www.thesullivangroup.com.
- Marc Taub, MD, FACEP, Chairman and Medical Director, ED, South Coast Medical Center, Laguna Beach, CA. Phone: (949) 489-3891. E-mail: [email protected].
For more information on two-way radios, contact:
- Ken DeMott, RN, MS, CEN, Nurse Manager, Emergency Departments, Wilson Memorial Regional Medical Center, 3355 Harrison St., Johnson City, NY 13790. Phone: (607) 763-6616. E-mail: [email protected].
A three-day "Train the Trainer" program costs $3,500 per instructor trained. For information on the teamwork training course, contact:
- Judy Barrett, Dynamics Research Corp., 60 Frontage Road, Andover, MA 01810. Phone: (866) 372-8326 or (978) 475-9090. Web: www.drc.com.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
