ECG Review-ST Elevation in Lead aVL
ECG Review-ST Elevation in Lead aVL
 |
By Ken Grauer, MD
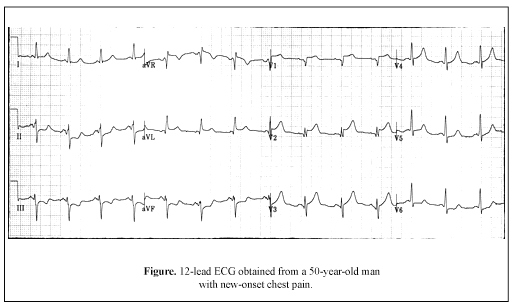
Clinical Scenario: The 12-lead ECG shown in the Figure was obtained from a 50-year-old man with new-onset chest pain. In view of a negative prior history of coronary disease, what might cardiac catheterization show?
Interpretation: The rhythm in this tracing is sinus, albeit with a shortened PR interval. The mean QRS axis is leftward (about -40°), consistent with a left anterior hemiblock pattern. There is no sign of chamber enlargement. Small q waves are seen in leads I and aVL, as in leads V2 and V3. A QS complex is seen in lead V1. Obvious ST segment elevation is seen in the anterior precordial leads, with reciprocal ST segment depression in most other leads on this tracing. As suggested in the title of this ECG Review, ST segment elevation is also seen in lead aVL. In the setting of new-onset chest pain, the overall ECG picture seen here is strongly suggestive of acute anteroseptal infarction.
ST segment elevation in lead aVL has been shown to provide insight into the anatomic site of acute coronary occlusion. In an interesting correlative study by Birnbaum et al, patients with ST segment elevation in lead aVL that occurred in association with ST segment elevation in several other anterior precordial leads (V1, V3, V4, and/or V5) most often were found at cardiac catheterization to have acute occlusion of the left anterior descending (LAD) coronary artery proximal to the first diagonal branch.1 This was precisely what was found at catheterization for the patient whose ECG is shown in the Figure. In contrast, patients with ST segment elevation in lead aVL and V2, but ST segment depression in other precordial leads most commonly had acute occlusion of only the diagonal branch of the LAD. Those in the study with ST segment elevation in lead aVL but ST segment depression in lead V2 were more likely to have a culprit lesion in the obtuse marginal branch of the circumflex artery.
Reference
1. Birnbaum Y, et al. Am Heart J. 1996;131:38-42.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
