Healthcare Infection Prevention-The sky’s no limit if workers need PEP
Healthcare Infection Prevention-The sky’s no limit if workers need PEP
Having served 14 years as a flight nurse in "a previous life," it’s not all that surprising that Karen Miller, RN, should look at an incoming medical helicopter and see an infection control opportunity. The infection control professional works at Borgess Medical Center, in Kalamazoo, MI. The center is affiliated with West Michigan Air Care, an air medical transport service that may bring patients in from accidents or transfer them from other hospitals.
Having worked before on such a unit and now learning infection control as an ICP, Miller realized that air medical and transport crew members are at risk for occupational exposure to blood and body fluids. For example, they are often involved in extricating injured patients in conditions of wreckage and broken glass, she says. "There is a lot of potential for exposure to blood or body fluids. They start IVs, work with test tubes, airway intubation, all types of procedures. It’s just like an ER [emergency room]."
Crew members report any exposure upon return to a hospital, at which time assessment of infection risk, including source-patient testing is done. If indicated (i.e., a deep needlestick to an HIV-positive patient) HIV post-exposure prophylaxis (PEP) is administered. But in patient transport, operational and unforeseen factors may result in the transports lasting several hours.
With the sooner-the-better mentality for administering PEP for true exposures, Miller wondered if she could devise a protocol that would allow crew members to self-administer one dose of the drugs during very long or delayed flights. "We had a couple of exposures that happened out in the field," she says. "There could have been better knowledge that there was something that could be done with post-exposure prophylaxis. We felt if it was relatively safe to administer one dose it might help them."
As a result, Miller and colleagues developed a protocol for self-administration of HIV PEP. (See protocol, p. 4.) To do so, they developed objective field criteria for assessing the risk of HIV infection and provided thorough education, training, and counseling prior to beginning the program. The protocol is essentially an algorithm that asks the crew member to determine the nature of the exposure, assess the risk for infection, and determine whether PEP is necessary. For example, the most severe exposure to a known HIV-positive source would call for the worker to take a three-drug dose of zidovudine, lamivudine, and nelfinavir. Of course, the crew member’s condition would be completely assessed upon return, and a decision would be made whether PEP will be continued.
|
West Michigan Air Care Corporate Operations Manual Clinical Protocol: HIV Post-Exposure Prophlaxis |
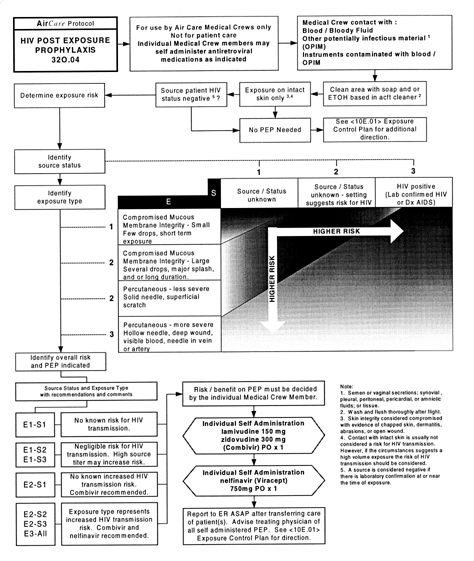 |
The protocol was implemented late last year and antiretroviral agents were made available to the Air Care medical crew on the helicopter. However - not surprisingly from Miller’s perspective - no crew member has taken the pills. "We don’t anticipate that they will use it much," she says. "With the education we did up front and the specific protocol we developed, I actually think it will prevent them from [using PEP] unnecessarily."
The education, for example, clarified that blood exposures (even if the blood is HIV-positive) to intact skin do not warrant PEP.
"It was helpful because they thought everything was an exposure," Miller says. "If you get blood on intact skin, you just wash it off."
Indeed, a surprising secondary gain has been heightened communication and improved infection control education for the medical flight crew. "We’ve made recommendations for personal protective gear and needle safety devices that they use," she says.
(Editor’s note: The protocol used by West Michigan Air Care was developed prior to recent issuance of new PEP guidelines by the Centers for Disease Control and Prevention. While the exposure descriptions and drug selections appear to be in keeping with the new CDC recommendations, ICPs may want to consult their infection control committees or the CDC before adopting a similar approach. Miller says she will review the new guidelines and revise the protocol if needed. We will publish an updated version, if one is deemed necessary, in a future issue of Hospital Infection Control.)
