Oral contraceptives are top choice when it comes to birth control
Oral contraceptives are top choice when it comes to birth control
Noncontraceptive benefits help drive the power of the Pill
Take a look at your patient roster for the past month. How many women left the office using oral contraceptives (OCs)? It’s a good bet that more than half of them did, according to responses to Contra-ceptive Technology Update’s 2001 Contraception Survey. The annual poll’s results show almost 53% of providers say more than half of their patients are using OCs, a number that rose slightly from 48.3% in 2000.
Birth control pills continue to be a popular choice among American women, according to survey respondents. About 29% say that 26%-50% of their patients receive pills each month, with about 13% reporting that 11%-25% receive them. Almost 6% say that 10% or less of their monthly patient population use the Pill.
At Arlington (VA) County Department of Human Services, the percentage of OC users has remained about the same in the past year, with more than 50% of women leaving the clinic each month with pill prescriptions, says Linda Hedlund, MD, medical supervisor. She also notes that Depo-Provera (depot medroxyprogesterone acetate, Pharmacia Corp., Peapack, NJ) remains a popular choice among the facility’s patient population.
Numbers of OC users seem to remain steady at Planned Parenthood of Santa Barbara, Ventura, and San Luis Obispo (CA) counties, observes Deb Lowry, CNM, a clinician and quality management coordinator.
Acceptance of the Pill is growing as more women now trust its safety and effectiveness. According to results of a 2000 survey conducted for the Washington, DC-based American College of Obstetricians and Gynecologists (ACOG), less than half (41%) of women said they believed there were "substantial health risks" associated with pill use.1 This figure reflects a drop from the 54% of women reporting such views in 1993, and a sharp decline from the 76% figure recorded in 1985.
Tri-Cyclen still tops
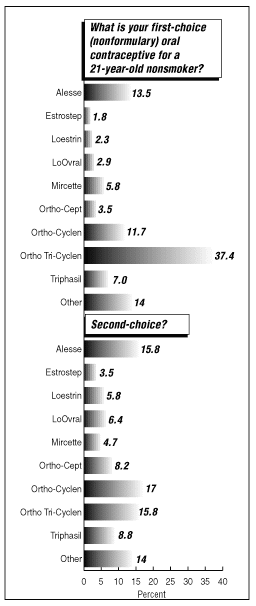
Ortho Tri-Cyclen, a 35 mcg ethinyl estradiol phasic pill marketed by Ortho-McNeil Pharmaceuticals of Raritan, NJ, continues to be the leading choice as the top nonformulary and formulary selections for a 21-year-old nonsmoking woman. (See charts on first- and second-choice nonformulary OC for a 21-year-old nonsmoker, below.) About 37% of respondents in the 2001 survey say Tri-Cyclen is their top nonformulary choice, and when bound by program formularies, almost 40% of 2001 responses list the OC as the No. 1 choice. The pill recorded a slight gain over its 32.9% share in the 2000 nonformulary category, and moved up from 2000’s 36.9% figure in the formulary category.
 |
What drives the OC’s continued popularity?
"Tri-Cyclen is our No. 1 OC because of the price we get for it and because of patient demand fueled by advertising," says Lowry.
Patients ask for Ortho Tri-Cyclen by name, due to the company’s product advertising, says Ann Jacob, CNM, clinic director of the University of Texas Medical Branch’s New Caney Clinic.
The pill currently is the only OC to carry a specific indication for the treatment of moderate acne vulgaris. However, two other companies have filed with the Food and Drug Administration for a similar indication: Wyeth-Ayerst Laboratories of Philadelphia for its monophasic 20 mcg pill, Alesse, and Pfizer of New York City for its multiphasic estrogen OC, Estrostep.
Ortho-Cyclen, a 35 mcg monophasic pill from Ortho-McNeil, was named for the second year as the top second-choice formulary OC for young nonsmoking women. Survey respondents also ranked it as the leading second-choice pill when not under formulary constraints.
Low-dose OCs move up
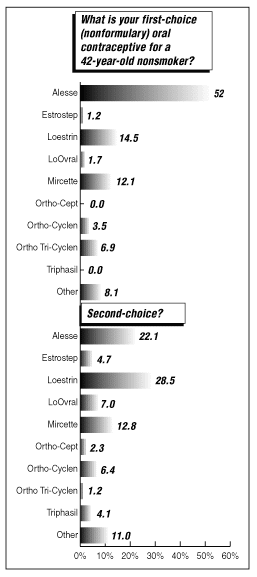
Alesse continues to gain favor as the preferred OC for older, nonsmoking women, according to survey results. More than 50% of responses listed the pill as their leading choice. Loestrin, another Pfizer OC, regained the top spot as the second-choice pill, reversing its position with Alesse from 2000’s poll results. (See charts on first- and second-choice nonformulary OC for a 42-year-old nonsmoker, below.)
 |
Women in perimenopause indeed may be using low-dose OCs for more than contraception. More than one-third of women participating in the 2000 ACOG poll said they were either taking, or knew someone who was taking, the Pill to reduce symptoms of perimenopause, such as hot flashes or irregular periods.
"As endogenous estrogen secretion is thought to decline gradually into maturity, I like the idea of being able to provide a lower exogenous hormone dose," states Patricia Carrick, FNP-C, a family nurse practitioner at Beaverhead Family Planning Clinic in Dillon, MT. "I have seen women who tolerated the 20 mcg dose right into menopause and then made the transition to hormone replacement therapy pretty seamlessly."
Don’t expect the trend to stop for the lowest-estrogen pill, says Robert Hatcher, MD, MPH, professor of gynecology and obstetrics at Emory University School of Medicine in Atlanta and chairman of the CTU editorial advisory board. A 15 mcg pill already is being marketed in Europe, and companies in the United States also are considering such OCs, he notes.
"The concerns raised today in some circles about 20 mcg pills are the same concerns one heard 25 years ago when we switched from 80 and 100 mcg pills to 50 mcg pills, and then 35 mcg pills," notes Hatcher.
Which pill for nausea?
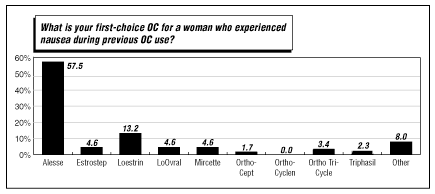
For women who have experienced bothersome nausea on previous OCs, but can’t remember the brand name of the pill used, more than half of the respondents to the 2001 CTU survey say they would prescribe Alesse. (See chart on first- and second-choice OCs for women who have experienced nausea during previous OC use, below.)
 |
 |
Mircette from Organon of West Orange, NJ, a pill with a unique dosing schedule (21 days of 150 mcg desogestrel/20 mcg ethinyl estradiol, two days of placebo pill, followed by five days of 10 mcg ethinyl estradiol) was named the leading second-choice pill for women with nausea problems. The pill rose from a third-place position in the 2000 survey in the second-choice category.
Look at the Pill’s benefits
In addition to its fertility-related benefits, the Pill offers advantages such as:
• less iron deficiency anemia, due to lighter menstrual bleeding;
• more regular cycles;
• less dysmenorrhea;
• less severe premenstrual symptoms;
• protection from two cancers of the reproductive organs: endometrial cancer and epithelial ovarian cancer.2
According to the 2001 CTU Contraception Survey, more providers say they are recommending pills to women specifically to reduce their risk of cancer of the ovary. Almost 34% of survey respondents indicated they prescribed pills based on patient history of ovarian cancer risk, up from 2000’s 31% figure.
Ruth Shaber, MD, women’s health leader at Kaiser Permanente Northern California in Oakland, proactively lets women know of the decrease in ovarian cancer risk for those with more than one relative with ovarian cancer.
"I also routinely educate women without a family history of the health benefits of OCs, especially if they have been influenced by the common myths that long-term OC use is dangerous and they are considering stopping their pills," states Shaber.
References
1. American College of Obstetricians and Gynecologists. The Pill at 40: Women say it’s safer, has extra benefits, but not covered by insurance. Press release. Washington, DC; May 2, 2000.
2. Blackburn RD, Cunkelman JA, Zlidar VM. Oral contraceptives — an update. Population Reports Spring 2000; Series A (No. 9):11.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
