The IUD: Is it on the comeback trail?
The IUD: Is it on the comeback trail?
The 2000 introduction of the Mirena levonorgestrel intrauterine system (IUS) from Berlex Laboratories of Montville, NJ, is bringing fresh interest in intrauterine devices (IUDs), according to providers participating in the 2001 Contraceptive Technology Update Contraception Survey.
IUD popularity jumps
Intrauterine contraceptive use has slightly increased with the introduction of Mirena, states Jeffrey Maurus, MD, medical director of the Rock Island (IL) County Health Department. Many women are interested in the device’s noncontraceptive benefits, he says.
Clinicians at Planned Parenthood of Santa Barbara, Ventura, and San Luis Obispo Counties in Santa Barbara, CA, insert at least three IUDs a week, estimates Deb Lowry, CNM, quality management coordinator.
"Numbers may be increasing," observes Lowry. "It is most popular among our Hispanic clients."
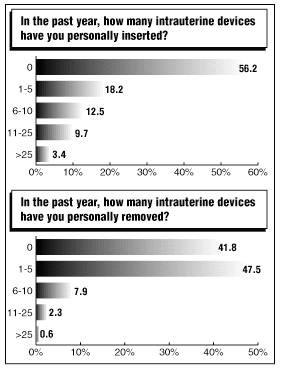
To track use of intrauterine contraceptive devices, the 2001 CTU survey included questions on device insertions and removals. While 56.2% of respondents said they had inserted no devices in the past year, a total of 30.7% indicated they had inserted one to 10 devices, and 13.1% said they had performed more than 10 insertions. About 42% said they had removed no devices during the year, with 55.4% removing one to 10 devices. About 3% had removed more than 10 devices in the past year. (See chart on insertions and removals, below.)
 |
More options for women
The Mirena IUS releases a steady 20 mcg dose of the progestin levonorgestrel and has been approved for five years of use in the United States. The overall failure rate during use of the IUS is 0.14 per 100 woman-years, based on more than 12,000 woman-years of use.1 This rate is comparable to annual failure rates for female sterilization.2 (CTU reported on the device approval in its February 2001 issue, p. 13, and further clinical information is included in the special Contraceptive Technology Report inserted in the May 2001 issue.)
Berlex Laboratories is marketing the device under a license from The Population Council, a New York City-based research organization that initially developed the IUS. The Mirena joins two other intrauterine contraceptives: the copper T380A IUD, which is marketed in the United States as the ParaGard Intrauterine Copper Contraceptive by Ortho-McNeil Pharmaceutical of Raritan, NJ, and the Progestasert Intrauterine Progesterone Contraceptive System, marketed by Alza Pharmaceuticals of Palo Alto, CA.
The levonorgestrel contained in the Mirena IUS aids in endometrial suppression and decreased blood flow. While the device presently carries only a contraceptive indication in the United States, other suggested uses include:
• providing an alternative to hysterectomy in women with heavy uterine bleeding;
• treating heavy idiopathic and adenomyosis-related bleeding and offering an alternative to endometrial resection for dysfunctional bleeding;
• delivering a progestin component in hormone replacement therapy (HRT) to protect the endometrium, offering the advantage of not causing monthly bleeding — the principal reason for discontinuation of HRT.3
Check training schedule
Family planning organizations such as the Washington, DC-based Association of Reproduc-tive Health Professionals (ARHP) have been active this year in offering training sessions on use of the Mirena device.
According to Wayne Shields, ARHP president and CEO, more than 4,000 physicians, nurse practitioners, physician assistants, and nurse midwives have participated in ARHP’s continuing medical education program, New Developments in Contraception: Counseling and Insertion Training Featuring the Levonorgestrel Intrauterine System, at 120 sites during the spring of 2001. Further sessions have been scheduled for ARHP’s annual meeting Sept. 12-15 in Washington, DC, as well as at the upcoming Oct. 10-13 seminar sponsored by the Washington, DC-based National Association of Nurse Practitioners in Women’s Health. (See CTU, August 2001, p. 95, for more information on these conferences.)
The curriculum was developed in partnership with the Ithaca (NY) Center for Postgraduate Medical Education, says Shields. Individual sessions scheduled for Fall 2001 and beyond will be held in various locations around the country; Shields suggests that providers check course availability by calling ARHP at (202) 466-3825 or sending e-mail to [email protected].
"We have been pleased about the extremely positive reaction ARHP has received to this program; health care providers are eager to learn about new contraceptive developments and the IUD in particular," Shields says. "We feel that the time is right for the U.S. to catch up with the rest of the world in its use of IUDs — a very safe and effective choice for many women."
Explain benefits, risks
An important motivator for increased provider training will be consumer demand, says Philip Darney, MD, MSc, professor at the University of California, San Francisco, and chief of the department of OB/GYN at San Francisco General Hospital Medical Center.
"If more women knew about the safety and efficacy of [intrauterine contraceptives], they would ask their providers for them, and the providers would ask for information and training," Darney observes. "We can start by offering IUDs to all our patients seeking contraception and explaining the great benefits and minimal risks."
References
1. Andersson K, Odlind V, Rybo G. Levonorgestrel-releasing and copper-releasing (Nova T) IUDs during five years of use: A randomized comparative trial. Contraception 1994; 49:56-72.
2. Peterson HB, Xia Z, Hughes JM, et al. The risk of pregnancy after tubal sterilization: Findings from the U.S. collaborative review of sterilization. Am J Obstet Gynecol 1996; 174:1,161-1,168.
3. Grimes DA, Jones KP, eds. A Clinician’s Guide to Levonorgestrel Intrauterine Contraception. Washington, DC: Association of Reproductive Health Professionals; 2001.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
