Homocysteine, Vitamins, and Cerebral Veins
Abstract & Commentary
Synopsis: In this population, deficient nutritional status may contribute to its relatively high incidence of CVT.
Sources: Cantu C, et al. Hyperhomocysteinemia, Low Folate and Vit B12 Concentrations, and Methylene Tetrahydrofolate Reductase Mutation in Cerebral Venous Thrombosis. Stroke. 2004;35:1790-1794.; Hankey GJ, et al. Vitamin Therapy to Prevent Stroke. The Jury is Still Out. Stroke. 2004;35: 1995-1998.
Hyperhomocysteinemia or elevation of plasma total homocysteine (Hyper-tHcy) is an independent risk factor for cardiovascular disease and stroke.1 A recent meta-analysis of data from 12 prospective studies found that a 25% elevation in tHcy was associated with a 10% higher risk of cardiovascular disease, and a 20% greater risk of stroke.2 Nevertheless, the recent Vitamins in Stroke Prevention (VISP) TRIAL3 did not find a significant treatment effect of lowering tHcy by therapy with folic acid, vitamin B12, vitamin B6, and riboflavin on recurrent stroke, coronary event, or death. Hyper-tHcy also has been implicated as a risk factor for AD4 and cerebral vein thrombosis (CVT)5.
Although CVT is an uncommon diagnosis in American and European stroke registries, CVT comprised 8% of more than 2000 cerebrovascular disease cases in a Mexico City Hospital stroke registry.6 Cantu and colleagues sought to explain this discrepancy by studying 45 Mexican patients with CVT and 90 control subjects. (see table) They measured plasma levels of tHcy, folate, and vitamin B12, and performed genotyping of the methylene tetrahydrofolate reductase (MTHFR) gene.
Table
CVT Patients Compared With Controls
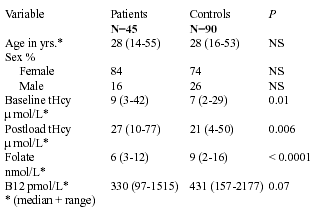
The most common predisposing factor for CVT was puerperium in 51%. Other predisposing factors included: anticardiolipin antibodies in 11 patients, protein S or protein C deficiency in 6, prothrombin gene mutation in 4, Factor V Leidin mutation in 2, use of oral contraceptives in 2, pregnancy in 1, and SLE in 1. Twenty-five patients (55%) were anemic.
Most patients presented clinically with headaches (96%), focal neurological deficits (69%), seizures (62%), impaired consciousness (44%), and intracranial hypertension (40%).
The most commonly affected venous sinuses were the superior sagittal (82%) and lateral sinuses (47%). Venous infarction was present on neuroimaging studies in 76%, and was hemorrhagic in 49%.
Prognosis was good: most patients made a total recovery (60%), or had only minor neurological deficits (36%).
The adjusted Odds Ratio (OR) for CVT associated with high (> 90th percentile) fasting levels of tHcy was 4.6. The adjusted OR for low plasma folate values or low B12 levels (< 10th percentile) and the presence of CVT was 3.5 and 5.1, respectively. There was a higher frequency of MTHFR mutation in patients with CVT (22% vs 10%), but it was not statistically significant. Patients with MTHFR mutation and low folate levels presented the highest tHcy levels. Cantu et al concluded that in this population, deficient nutritional status may contribute to its relatively high incidence of CVT.
Commentary
Cantu et al confirmed the previously noted5 association between Hyper-tHcy and CVT. Their results add to a large body of epidemiological and laboratory evidence that indicates that increased plasma concentrations of tHcy are thrombogenic. Additionally, they found that a low folate and vitamin B12 state was independently associated with an increased risk of CVT in a nutritionally deficient population. This latter result is consonant with the Health Professional Follow UP Study7 findings, namely that stroke risk was lower in healthy men whose folate intake was in the highest quintile, compared with those in the lowest quintile. In contrast, the VISP Trial3 found no significant difference in the 2-year cumulative incidence of recurrent cerebral infarction between patients allocated to high-dose multivitamins and those taking low-dose multivitamins. As pointed out by Hankey and colleagues in an editorial, VISP enrolled patients primarily from North America, and did not have the statistical power to exclude a modest, but clinically important, therapeutic effect of folic acid-based multivitamin therapy. Physicians in the United States, Canada, and Europe are justified in concluding that insufficient evidence exists to recommend routine screening and treatment of Hyper-tHcy with folate and other vitamins to prevent thrombotic vascular disease. In selected high risk individuals or populations for whom the potential benefits are great, however, clinicians should recommend folic-acid-based, multivitamin therapy in high doses. — John J. Caronna
Dr. Caronna, Vice-Chairman, Department of Neurology, Cornell University Medical Center; Professor of Clinical Neurology, New York Hospital, is Associate Editor of Neurology Alert.
References
1. Eikelboom JW, et al. Ann Int Med. 1999; 131:363-375.
2. Homocysteine Studies Collaboration. JAMA. 2002;288: 2015-2022.
3. Toole JF, et al. JAMA. 2004;291:565-575.
4. Seshadri S, et al. N Eng J Med. 2002;346:476-483.
5. Martinelli I, et al. Blood. 2003;102:1363-1366.
6. Baringarrementeria F, et al. Neurology. 1999;52:A442.
7. He K, et al. Stroke. 2004;35:169-174.
In this population, deficient nutritional status may contribute to its relatively high incidence of cerebral vein thrombosis.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
