National Quality Improvement Efforts: What Will it Take to Make Them Succeed?
National Quality Improvement Efforts: What Will it Take to Make Them Succeed?
Authors: Edward L. Charnock, MD, Medical Director, Health Care Quality Improvement Program, Ohio KePRO; Margaret M. Toth, MD, Associate Medical Director, Health Care Quality Improvement Program, Ohio KePRO.
Editor’s Note—An 88-year-old man has been ill for 3 days with cough, fever, and confusion. His wife reports that he has been repeating himself and occasionally fails to recognize her. He arrives in the emergency department (ED) via EMS squad.
On admission the patient’s pulse is 94, respirations 26, temperature 36.2°C, and blood pressure 150/70. Physical examination reveals bi-basilar crackles. Chest x-ray shows infiltrates in the right middle and left lower lung fields. White blood cell count is 22,000. Blood cultures are obtained and the patient is admitted.
This patient’s chances for a full recovery are best if he receives his first dose of IV antibiotics in:
a. less than 8 hours.
b. 12 to 24 hours.
c. 24 to 48 hours.
A 68-year-old man is awoken with bilateral arm pain, chest pain, and diaphoresis. He arrives in the ED and reports the pain was relieved by oxygen and nitroglycerin administered by the EMS squad. An electrocardiogram is consistent with acute inferior wall myocardial infarction. Following standing protocol, the EMS squad also administered aspirin.
The early administration of aspirin in this patient reduced his 1-year mortality by:
a. 4%.
b. 23%.
c. 85%.
With more than 45 years of combined experience as physicians and health quality professionals, we can confidently predict that nearly every physician reading the preceding questions answered them correctly. As a group, healthcare practitioners in this nation bring to their professions and practice an extraordinary breadth of medical knowledge. This knowledge, coupled with genuine commitment to patient care, has led to monumental medical advances during the last half century. We have seen dramatic reductions in death from childhood cancers, advances in the treatment of acute stroke, and made great strides in conquering infections.
Despite these advances, patients with pneumonia admitted to acute care hospitals wait longer than 8 hours for their first dose of antibiotics every day. These patients will not benefit from the 15% lower risk of 30-day mortality reported when antibiotics are administered within 8 hours of hospital arrival.1
Moreover, 1 in 10 patients admitted to acute care hospitals with acute myocardial infarction and no contraindication to aspirin do not receive this medication during the first 24 hours of hospitalization, thereby depriving them of a 23% reduction in short-term mortality.2
Unfortunately, these discrepancies in care are not exceptional. Instead, they reflect a healthcare system in which, on average, it takes 17 years for new knowledge generated by randomized controlled trials to be incorporated into practice, and even then application is highly uneven.3
Clearly, this is not the result of a healthcare system populated with "bad" practitioners lacking fundamental medical knowledge or a lack of commitment to providing high quality patient care, but rather due to deficiencies in our healthcare system. For patients to benefit from the knowledge of practitioners and the advances in medicine, the healthcare delivery system must function efficiently and consistently. The discrepancies we are seeing in healthcare delivery suggest that our systems are in need of continuing improvement.
It appears these changes are beginning to take hold in the practice of medicine. As we enter what is to be the "decade of quality" in medicine, healthcare practitioners are defining the direction of change through the development and growth of evidence-based practice. No longer willing to accept the status quo, practitioners are now looking for and explicitly, judiciously, and conscientiously using the current best evidence when making decisions regarding the care of their individual patients. These practitioners recognize that they provide their patients the best quality of care when they integrate clinical experience with the best available scientific evidence.4
Much of this evidence comes from studies specifically designed to measure outcomes of clinical care. While these studies are common today, they were decidedly uncommon in the past. Medical education is also changing the way practitioners think. Many undergraduate and postgraduate programs now include evidence-based medicine and quality improvement training in their curricula. Much of this has led to the growth of practice guidelines and critical pathways, once criticized as "cookbook" medicine, but now recognized as valuable tools for clinicians as they navigate through the increasingly complex world of 21st century healthcare.
This article will describe how the Centers for Medicare and Medicaid Services (CMS) (formerly the Health Care Financing Administration [HCFA]), through its contracted Peer Review Organizations (PROs), is working to improve the mechanics of healthcare delivery by assisting healthcare organizations as well as individual practitioners apply these quality of care advances.
Prompted by the need for a national approach to improved healthcare delivery, CMS initiated the Health Care Quality Improvement Program (HCQIP) in 1992. This program is administered by CMS and carried out by the PROs and recognizes the importance of applying a systematic, evidence-based approach to improving healthcare quality. Nationally, the HCQIP program focuses on 6 clinical priority areas. These areas of priority are acute myocardial infarction, heart failure, stroke and atrial fibrillation, pneumonia and immunizations (influenza and pneumococcal), breast cancer prevention, and diabetes care. These priorities were selected because they significantly contribute to the overall morbidity and mortality of Medicare beneficiaries and have well established, scientifically sound standards for care.
The HCQIP national projects follow the scientific model, which, of course, is well known to physicians as it forms the basis for our own education and practice. For each project, a series of "quality indicators" have been developed. These indicators are scientifically sound and based on evidence and guidelines published by professional organizations such as the American Thoracic Society and American College of Cardiology. A baseline measurement of performance for these quality indicators establishes the care patterns within each state. The PRO then works collaboratively with healthcare practitioners and providers (hospitals, clinics, healthcare systems) to foster improvement. The work of the PRO focuses on systems improvements as it recognizes that deficiencies in care patterns are generally the result of system issues—not individual competency issues. The PROs encourage and facilitate the application of proven techniques, such as rapid cycle testing, to quality improvement efforts. Evidence-based tools and interventions are developed and shared with healthcare professionals and organizations. The success of the PROs work is evaluated through re-measurement of quality indicators.
In October 2000, Jencks and colleagues published the first national overview of the quality of care delivered to Medicare beneficiaries.5 The quality indicators established for the HCQIP program were used as the measures of quality for this study. Highlighted in this work were several opportunities for improvement in the areas of national priority. The subsequent sections of this article will focus on each of these areas of priority. Emphasis will be placed on the systems issues surrounding the care deficiencies. Examples of successful interventions will be discussed.
Healthcare practitioners play a pivotal role in bringing about systems improvements in the operations of their daily practices as well as the operations of the hospitals in which they work. They are encouraged to use the information provided in this article as a catalyst for making changes within their own care environment.
National Priorities
Acute Myocardial Infarction
The care and treatment of patients suffering acute myocardial infarction (AMI) is an obvious choice for a clinical priority. Each year, nearly 400,000 Medicare beneficiaries are hospitalized with AMI. One third of patients die during the acute phase of their AMI—many of those who survive suffer with residual disability. In fact, 85% of all AMI deaths occur in those age 65 and older. CMS payments to hospitals for the direct care of patients hospitalized with AMI exceeded $3.6 billion in 1996.6
The AMI projects currently administered by the PROs in all 50 states and 3 territories evolved from the Cooperative Cardiovascular Project (CCP) originally developed in 1992 by Qualidigm, Connecticut’s PRO, and later expanded as pilot studies in other states. Using evidence-based practice guidelines directed toward the timely treatment of patients with AMI, this initiative resulted in a 9.3% increase in aspirin use. Beta-blocker prescriptions at discharge rose from 47% to 67% over the 3-year study period. Most significantly, these process improvements were associated with a 10% reduction in 30-day and 1-year mortality rates.7
Building on the success of this project, the objective of the PROs national AMI project is to decrease the 1-year mortality rate for Medicare beneficiaries admitted to the hospital with AMI. Following careful review of existing scientific literature and the published guidelines of the American College of Cardiology and the American Heart Association (AHA),8 7 quality indicators were developed to measure improvement in AMI-related care processes. Statewide performance for each indicator is measured at regular intervals by CMS.5 Patient charts are comprehensively reviewed for inclusion/exclusion criteria and performance on quality indicators is measured for those patients who have no contraindications to the treatment being measured (see Table 1).
| Table 1. National Rates: Quality Indicators for the AMI Project | |||
| Quality Indicator | Potential Impact | National Median (%) | Range (%) |
| Aspirin administration within 24 hours of admission |
Early use of aspirin associated with 23% reduction in short-term mortality, ISIS-2 |
83.9 | 66.7-97.2 |
| Beta-blocker administration within 24 hours of admission |
Early use of beta-blockers reduced short-term mortality by 4.3-4.9%.7 |
64.0 | 33.1-79.0 |
| Timely initiation of reperfusion therapy |
Earlier access to reperfusion therapy increases efficacy of treatment and improves survival rates.43 |
40.0 | 21.0-66.0 |
| Aspirin prescribed at discharge | Long-term use of aspirin after AMI reduces vascular mortality by 13%, nonfatal AMI by 31%, and stroke by 42%. |
84.8 | 59.5-97.3 |
| Beta-blocker prescribed at discharge |
Long-term use of beta-blockers after AMI reduced mortality by 23%.44 |
72.0 | 46.7-93.1 |
| ACE inhibitor prescribed at discharge for patients with low left ventricular ejection fraction |
Long-term use of ACE inhibitors after AMI in patients with impaired ventricular contractility reduced mortality by 20-27%.45 |
70.4 | 55.6-90.0 |
| Smoking cessation counseling | Patients who continue to smoke after an AMI have a mortality rate 1.33 to 2.55 times higher than that of patients who quit.46 |
41.7 | 19.4-69.6 |
| Source: Data collected via chart abstraction form from hospital medical records (April 1998-May 1999). | |||
Like most deficiencies in healthcare delivery, the shortcomings measured in the performance of quality indicators for the national AMI project are more likely to be the result of systems breakdowns than individual failures. For example, the early administration of thrombolytics requires the coordinated efforts of physicians, pharmacists, nurses, technicians, and support and clerical workers, not to mention the patient and family. Breakdowns in communication or processes involving any of the multitude of steps that stand between the physician’s initial order and the administration of this potentially life-saving medication can result in delays that rob patients of treatment benefits.
To address these systems issues, the PROs have developed a variety of tools to assist healthcare organizations as they work to improve AMI care. Many PROs have developed tools such as pocket cards that serve as memory aids. The information supplied on these cards range from medication dosing to lists of treatment indications and contraindications. In addition, many PROs produce comprehensive resource manuals that they share with healthcare facilities. These manuals include relevant clinical guidelines and reference articles, clinical pathways, sample standing orders, patient education materials, and examples of successful interventions solicited from hospitals. These materials are provided free of charge to healthcare professionals and hospitals upon request.
Increasingly, the PROs are providing healthcare organizations with training in process improvement techniques aimed at addressing the complex array of systems issues reflected in the measures of these indicators. The potential gains associated with the use of these techniques were convincingly demonstrated by groups such as James A. Espinosa, MD, and colleagues at Overlook Hospital in Summit, NJ. Through the application of innovative systems-based interventions, this group successfully reduced time to thrombolytic administration from 60 to 16 minutes over a 2-year period beginning 1994, earning them recognition from CMS for "Best Practice for Time to Thrombolyics in AMI."9
Although many systems approaches are advocated, there appears to be no "magic bullet." Other factors may be more important in characterizing improvement efforts, eg, shared goals for improvement, administrative support, strong physician leadership, and use of data feedback.53
A great opportunity to harness and apply comprehensive systems-centered improvement strategies is demonstrated by the successful partnership between the American Heart Association, PROs, medical societies, health departments, hospital associations, managed care organizations, and others interested in improving the delivery of quality cardiovascular care to patients with heart disease and to promote and support the AHA’s Get With The Guidelines initiative.
Get With The Guidelines is a rapid-cycle, continuous quality improvement initiative for hospitalized patients who have had a coronary event. The program estimates it will be able to save more than 40,000 people annually if the American Heart Association guidelines are implemented at least 80% of the time. The program focuses on building consensus among a hospital team, identifying a "champion" to drive the program, and implementing discharge protocols that include medications and lifestyle modifications. Pilot test results from this program will be posted on the AHA website in August 2001 (http://www.americanheart.org/getwiththeguidelines/pilot.html)(See Table 2.)
| Table 2. PRO Contact Information* | |||
| State | Peer Review Organization | Web Site | Phone |
| Alabama | Alabama Quality Assurance Foundation | www.aqaf.com | (205) 970-1600 |
| Alaska | PRO-West Alaska Branch Office | www.pro-west.org | (907) 562-2252 |
| Arizona | Health Services Advisory Group | www.hsag.com | (602) 264-6382 |
| Arkansas | Arkansas Foundation for Medical Care, Inc. | www.afmc.org | (501) 649-8501 |
| California | California Medical Review, Inc. (CMRI) | www.cmri-ca.org | (415) 677-2000 |
| Colorado | Colorado Foundation for Medical Care | www.cfmc.com | (303) 695-3300 |
| Connecticut | Qualidigm | www.qualidigm.org | (860) 632-2008 |
| Delaware | Quality Insights of Delaware (QID) | www.qualityinsights.org | (302) 475-8100 |
| DC | Delmarva Foundation for Medical Care, Inc. | www.dfmc.org | (202) 293-9650 |
| Florida | Florida Medical Quality Assurance Inc. | www.fmqai.com | (813) 354-9111 |
| Georgia | Georgia Medical Care Foundation (GMCF) | www.gmcf.org | (404) 982-0411 |
| Hawaii | Mountain-Pacific Quality Health Foundation | www.mt.net/~mtwy | (808) 545-2550 |
| Idaho | PRO-West | www.pro-west.org | (208) 343-4617 |
| Illinois | Illinois Foundation for Quality Healthcare | www.ifqhc.org | (630) 571-5540 |
| Indiana | Health Care Excel, Inc | www.hce.org | (812) 234-1499 |
| Iowa | Iowa Foundation for Medical Care (IFMC) | www.ifmc.org | (515) 223-2900 |
| Kansas | Kansas Foundation for Medical Care, Inc. (KFMC) | www.kfmc.org | (785) 273-2552 |
| Kentucky | Health Care Excel, Inc | www.hce.org | (502) 339-7442 |
| Louisiana | Louisiana Health Care Review, Inc. | www.lhcr.org | (225) 926-6353 |
| Maryland | Delmarva Foundation for Medical Care, Inc. | www.dfmc.org | (410) 822-0697 |
| Massachusetts | MassPRO | www.masspro.org | (781) 890-0011 |
| Maine | North East Health Quality Foundation | www.medicarequality.org | (603) 749-1641 |
| Michigan | Michigan Peer Review Organization | www.mpro.org | (734) 459-0900 |
| Minnesota | Stratis Health | www.stratishealth.org | (612) 854-3306 |
| Mississippi | I.Q.H. - Information and Quality Healthcare | www.iqh.org | (601) 957-1575 |
| Missouri | Missouri Patient Care Review Foundation | www.mpcrf.org | (573) 893-7900 |
| Montana | Mountain-Pacific Quality Health Foundation | www.mt.net/~mtwy | (406) 443-4020 |
| Nebraska | The Sunderbrunch Corporation | www.ifmc.org | (515) 223-2900 |
| Nevada | Health Insight | www.healthinsight.org | (702) 385-9933 |
| New Hampshire | North East Health Quality Foundation | www.medicarequality.org | (603) 749-1641 |
| New Jersey | Peer Review Organization of New Jersey, Inc. | www.pronj.org | (732) 238-5570 |
| New Mexico | New Mexico Medical Review Association (NMMRA) | www.nmmra.org | (505) 998-9898 |
| New York | IPRO | www.ipro.org | (516) 326-7767 |
| North Carolina | Medical Review of North Carolina, Inc. (MRNC) | www.mrnc.org | (919) 851-2955 |
| North Dakota | North Dakota Health Care Review, Inc. | www.ndhcri.org | (701) 852-4231 |
| Ohio | Ohio KePRO, Inc. | www.ohiokeproinc.com | (216) 447-9604 |
| Oklahoma | Oklahoma Foundation for Medical Quality, Inc. (OFMQ) | www.ofmq.com | (405) 840-2891 |
| Oregon | Oregon Medical Professional Review Organization | www.ompro.org | (503) 279-0100 |
| Pennsylvania | Keystone Peer Review Organization, Inc. | www.kepro.org | (717) 564-8288 |
| Puerto Rico | Quality Improvement Professional Research Organization | netdial.caribe.net/~qipro | (787) 641-1240 |
| Rhode Island | Rhode Island Quality Partners | Under construction | (401) 528-3200 |
| South Carolina | Carolina Medical Review | www.mrnc.org | (803) 731-8225 |
| South Dakota | South Dakota Foundation for Medical Care, Inc. | www.sdfmc.org | (605) 336-3505 |
| Tennessee | Mid-South Foundation for Medical Care, Inc. | www.tnproqio.com | (901) 682-0381 |
| Texas | Texas Medical Foundation | www.tmf.org | (512) 329-6610 |
| Utah | Health Insight | www.healthinsight.org | (801) 892-0155 |
| Vermont | North East Health Quality Foundation | www.medicarequality.org | (603) 749-1641 |
| Virgin Islands | Virgin Islands Medical Institute PRO, Inc | www.vimipro.org | (340) 712-2400 |
| Virginia | Virginia Health Quality Center | www.vhqc.org | (804) 289-5320 |
| Wyoming | Mountain-Pacific Quality Health Foundation | www.mt.net/~mtwy | (406) 443-4020 |
| West Virginia | West Virginia Medical Institute, Inc. | www.wvmi.org | (304) 346-9864 |
| Washington | PRO-West | www.pro-west.org | (206) 364-9700 |
| Wisconsin | MetaStar, Inc. | www.metastar.com | (608) 274-1940 |
| *Certain PROs cover more than one state. Additional information may be obtained at www.ahqa.org. See institutional member list. | |||
Heart Failure
The reasons for including heart failure in the HCQIP quality improvement efforts are clear. It is one of the most common chronic diseases in the elderly with 550,000 new cases diagnosed each year. As the population ages and overall treatment of heart failure improves, the prevalence and toll of heart failure continues to mount. Today, heart failure accounts for more hospital admissions than any other diagnosis in the Medicare population. Twenty to 30% of patients with heart failure will die within 1 year and one half within 5 years. Patients who survive often have significant functional limitations and require intensive multidisciplinary care. It is estimated that heart failure expenditures in the United States exceed $40 billion a year.10
The goal of the National Heart Failure Project administered by the PROs is to decrease the mortality and morbidity associated with heart failure in Medicare beneficiaries. In order to achieve this goal, the project has directed its focus toward increasing the use of appropriate diagnostic tests to evaluate left ventricular systolic dysfunction (LVSD) and increasing the use of angiotensin-converting enzyme inhibitors (ACEIs) in patients with ejection fractions less than 40%. These areas of focus are derived from practice recommendations published by the Heart Failure Society of America,11 a joint committee of the American College of Cardiology/American Heart Association (ACC/AHA),12 and the Institute for Clinical Systems Improvement (ICSI).13
The National Heart Failure Project findings published by Jencks et al5 suggest that large numbers of patients with heart failure are not receiving treatments with proven morbidity and mortality benefit (see Table 3). In some states, less than one half of the eligible heart failure patients received ACEIs by the time of hospital discharge.
| Table 3. National Rates: Quality Indicators for the National Heart Failure Project | |||
| Quality Indicator | Potential Impact | National Median (%) | Range (%) |
| Ejection fraction assessed | Evaluation and documentation of ejection fraction is critical for directing appropriate use of ACEI inhibitors |
64.3 | 33.7-78.6 |
| ACEI @ discharge | ACEI prescription in the elderly may lower mortality by 25-33%, while improving functional capacity and quality of life.47 |
69.4 | 46.8-90.9 |
| Fee-for-service patients only (June 1999-August 2000). | |||
Reflected in these numbers are deficiencies in outpatient as well as inpatient care. CMS’s focus on inpatient care in the PRO projects reflects a recognition that given the clear long-term benefits of ACEIs, one of the goals of hospitalization should be to initiate and titrate ACEIs toward target doses that have been identified in large-scale clinical trials and clinical practice guidelines.14 To aid physicians with this task, many PROs have provided pocket cards that reference starting and target doses of ACEIs as well as indications and contraindications to treatment. A card published by the Ohio PRO (Ohio KePRO) is an example (see Figure 1). Acceptance and use of this card by Ohio providers has resulted in its widespread distribution and use by hospitals and physician groups.
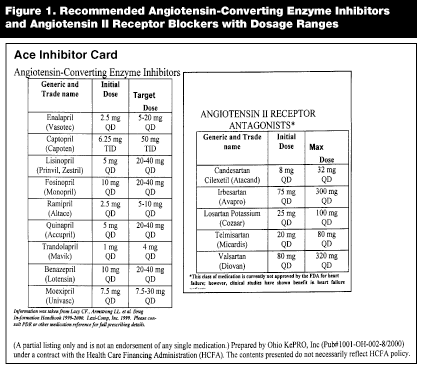 |
In addition, the PROs have developed a variety of initiatives focused on assisting hospitals with the successful implementation of clinical practice guidelines and pathways. Effective implementation of well-designed practice guidelines is one key to improving care in this group of patients. By their very design, practice guidelines take into account the extraordinarily complex processes and vast knowledge that physicians are required to incorporate into the care of each patient. The sheer volume of information, coupled with the demands of practice makes unaided compliance with treatment recommendations an unattainable goal. Thus, effectively implemented guidelines and pathways, which foster cooperative efforts across disciplines, ease the burden for physicians while enhancing the overall quality of care for patients.15,16
As treatment options and best practices for heart failure evolve, the PROs will continue to measure and work with providers to bring these advances to every day practice. An example of these advances is the growing role of beta-blockers in the treatment of heart failure.17-20
Future directions will surely include encouraging healthcare delivery innovations that are better adapted to meet the needs of the chronically ill. The roadmap for these innovations was published recently by the Institute of Medicine in its March 2001 report, Crossing the Quality Chasm: A New Health System for the 21st Century.21
Stroke and Atrial Fibrillation
The prevention and treatment of stroke is the primary focus of the PROs National Atrial Fibrillation and Stroke Projects. When considered on its own, stroke is the third leading cause of death, behind heart disease and cancer. Every 53 seconds, someone in the United States suffers a stroke and every 3.3 minutes, someone dies as a result.22 Overall, Americans of either gender have a 1 in 20 chance of having a stroke before the age of 70. Twenty-nine percent will die within the first year. In 1995, $3.7 billion was paid for the treatment of Medicare beneficiaries with stroke, according to CMS data.22
Among the many causes of stroke, embolic events resulting from under treatment of atrial fibrillation patients with stroke prophylaxis is regrettably common. Antithrombotics (eg, warfarin) are indicated in a large percentage of patients. CMS’s national study confirmed significant under use of this important agent (see Table 4). The implications of this under treatment will continue to mount as our population ages.23 Atrial fibrillation currently affects 4% of the population older than 60 and 10% of the population older than 80.24 Research supported by the Agency for Health Care Policy and Research, found that the expanded use of warfarin in patients with atrial fibrillation could lead to 40,000 fewer strokes each year.25 Addressing the gap in optimal care delivery is a primary objective of the PROs Atrial Fibrillation Project.
| Table 4. National Rates: National Stroke and Atrial Fibrillation Project Quality Indicators | |||
| Quality Indicator | Potential Impact | National Median (%) | Range (%) |
| Warfarin at discharge (atrial fibrillation) |
68% reduction in relative risk of stroke with virtually no increase risk of intracranial bleeding.24 |
55.7 | 28.8-65.3 |
| Avoidance of sublingual nifedipine (stroke) |
Aggressive antihypertensive therapy can further reduce cerebral perfusion. |
94.9 | 86.2-100 |
| Antithrombotic treatment @ discharge (stroke) |
Proper use of these agents can result in a 2-fold risk reduction in preventing a second stroke.24,48 |
82.5 | 72.0-90.1 |
| Fee-for-service patients only (claims data). | |||
A myriad of factors contribute to the under treatment of atrial fibrillation. Patients are often reluctant to take warfarin for fear of bleeding complications, while the medication’s narrow therapeutic index and the complexity of its administration and monitoring often discourage physicians from enthusiastically recommending this medication.24 Comprehensive manuals such as The AFP Guide To Preventing Strokes and Lowering Health Risks in Patients with Atrial Fibrillation, published in collaboration with the National Coalition for Stroke Prevention and Awareness, provide clinicians with a rational model for delivering this treatment.24 The guide shows that by combining the contemporary management strategies of empowerment, computerization, technology-driven improvements, and outsourcing, processes of care can be made easier, better, and cheaper. Much of the PRO work is focused on bringing valuable resources such as the AFP guide to the attention of physicians.
In 1996, the Food and Drug Administration (FDA) accepted the recommendations of the American Stroke Association and approved tissue plasminogen activator (tPA) for the treatment of stroke in selected patients.26 This advance, and the subsequent inclusion of additional thrombolytic agents, has changed forever the manner in which stroke patients will be evaluated and selectively treated. Considering stroke as a "brain attack" and recognizing that "time is brain" has prompted public education regarding symptom recognition and importance of seeking immediate medical care. CMS and the PROs have collaborated with public organizations and local, state, and national medical societies to promote these public education activities. Equally as important, PROs are collaborating and sponsoring healthcare professional education programs to increase the use of diagnostic studies and the appropriate use of therapeutic modalities for thrombolysis and preservation and resuscitation of brain tissue.
While most of the PRO quality improvement objectives aim to enhance the application of medical advances, the Stroke Project has focused some of its efforts on eliminating a debunked treatment. The use of sublingual nifedipine in the setting of acute stroke, once a standard treatment, has been clearly shown to be harmful. Blood pressure is often reflexively increased early in the course of a stroke. Acute reduction of blood pressure with agents such as sublingual nifedipine may precipitate further cerebral ischemia and tissue damage. Despite warnings published in the 1994 AHA guidelines, sublingual nifedipine remains in use.27
Nonetheless, great strides are being made in eliminating this dangerous treatment. Many hospitals have achieved total compliance with this recommendation by removing sublingual nifedipine from EDs. This intervention, which replaces our customary practice of relying on education and training with a definitive action (using the removal of nifedipine from the ED as a constraint) elegantly demonstrates the effect of applying principles developed by other high-reliability organizations to medical practice. As a group, high-reliability industries such as aviation provide complex services (airplane transportation) with minimal error (major crashes). They achieve this success largely by becoming "fault tolerant." This means that they recognize the propensity for humans to deviate from norms and make mistakes. But, instead of insisting that humans fundamentally alter their nature, they design changes into their systems that make it more difficult for humans to commit errors. This approach is becoming an increasingly important aspect of redesigning healthcare.28
Pneumonia and Immunization
Community acquired pneumonia (CAP) is the most common infectious cause of death and the sixth leading cause of death overall in the United States. Unlike many other common diseases, the overall age-adjusted death rate associated with CAP has increased by 22% in the last 20 years.29 Nearly 90% of deaths due to pneumonia occur in those older than age 65.30
Approximately 600,000 Medicare patients are hospitalized for pneumonia each year representing 4.2 million days of inpatient care. Pneumonia is also the principal reason for more than 500,000 ED visits by Medicare patients each year.31
Decreasing the morbidity and mortality associated with CAP in Medicare beneficiaries is the primary objective of the National Pneumonia Project. This is best accomplished by increasing the number of patients who receive immunizations against influenza and pneumococcal pneumonia. In addition, survival benefits have been demonstrated with the timely administration of the appropriate antibiotics and diagnostic cultures.
The 7 quality indicators developed by CMS for the National Pneumonia Project (see Table 5) reflect these objectives and are based on guidelines published by the Infectious Disease Society of America32 and the American Thoracic Society.33
| Table 5. National Rates: Quality Indicators for Community Acquired Pneumonia/Immunization | |||
| Quality Indicator | Potential Impact | National Median (%) | Range (%) |
| Inpatient* | |||
| First antibiotic received within 8 hours |
15% decrease in 30-day mortality when antibiotics were administered within 8 hours of hospital arrival.1 |
85.4 | 38.4-92.8 |
| Antibiotic consistent with guidelines |
Following recommendations of published guidelines has been shown to decrease mortality, morbidity, and length of stay.32 |
78.6 | 54.9-87.1 |
| Blood cultures before antibiotics |
An association between blood cultures within 24 hours and a lower 30-day mortality.1 |
82.3 | 65.2-93.4 |
| Screened for influenza vaccinev | Immunizations administered during in-patient stay have no higher complication rate and immunogenicity has been established.49 |
14.3 | 5.9-39.2 |
| Screened for pneumonia vaccine |
11.2 | 3.5-26.1 | |
| Outpatient** | |||
| Influenza immunization | Influenza and pneumonia vaccines effectively lower the rates of these diseases, and, therefore, morbidity and mortality in Medicare beneficiaries.50,52 |
65.9 | 41.5-71.4 |
| Pneumonia immunization | 45.8 | 32.2-59.4 | |
| * Data collected by chart abstraction for fee-for-service inpatients (April 1998-March 1999). | |||
| ** Behavioral Risk Factor Surveillance Survey (BRFSS)-1999. | |||
In order to effectively treat CAP, many system changes must occur. Innovations, such as empowering ED physicians and other healthcare professionals to begin empiric therapy using standing orders, can lead to reductions in antibiotic administration times. Projects such as the "Right Med, Right Time" initiative, administered by MetaStar, the Wisconsin PRO, provide hospitals and practitioners with expert coaching and guidance in the development and use of tools and interventions aimed at improving the coordination of treatment. This program includes clinical pathways, standing orders, and protocols aimed at decreasing care variations that can result in less than optimal outcomes for patients.
As electronic media become increasingly accessible to physicians and hospitals, decisions regarding appropriate antibiotic selection and administration can be supported using information from the Internet. Standards, such as those published by the Infectious Disease Society of America (www.idsa.org), and dosing and antibiotic selection information from the Johns Hopkins Antibiotic Guide (www.hopkins-abxguide.org) can be easily downloaded to hand-held devices. Ohio KePRO has developed a quick reference card (see Figure 2) for use by hospital staffs. These are provided free of charge to hospitals and practitioners within each state (see Table 2).
 |
More than one half of the cases of pneumococcal pneumonia occur in persons in whom vaccination is indicated; yet nationwide vaccination rates, ranging from 32% to 60%, remain far below the 90% target set by the Healthy People 2010 initiative.30 Disappointing measurements of performance on inpatient pneumococcal and influenza vaccination screening and outpatient vaccination rates demonstrate an important opportunity for improvement.5
Guides, such as Immunization 2000, Flu and Pneumonia Vaccination for the Acute Care Hospital, produced by Ohio KePRO provide hospitals with comprehensive resources for establishing, maintaining, and monitoring a hospital-wide vaccination plan.34-36 The guide includes standing orders, patient education materials, provider information sheets that address common myths surrounding vaccination, sample consent and order forms, roster billing information, patient reminders, chart stickers, and a month-by-month planning timeline. Similar guides have been developed for use in home health/dialysis centers and the physician office setting. Physician offices and health departments have used this guide as a resource for organizing vaccination days. In addition, PROs are often involved in efforts to expand their proactive approach to pneumonia prevention through their involvement with coalitions that sponsor community-based initiatives to increase vaccination rates.
Breast Cancer Prevention
Breast cancer ranks second among cancer deaths in women. An estimated 182,800 new cases of invasive breast cancer are expected to occur among women in the United States each year, and 40,800 women will die from the disease.37 Breast cancer and associated comorbidities and mortalities become more prevalent with increasing age, and more than one half of breast cancers occur in women 65 years and older. The risk of developing breast cancer by age 30 is approximately 1 in 2500; this risk increases to 1 in 14 for women by age 70.38
Periodic screening mammography saves lives by detecting breast cancer early, when it is most treatable. It appears that judicious use of mammography can prevent approximately one fourth of breast cancer deaths. Yet, this important screening test is underused.39 The National Breast Cancer Project focuses on regular breast cancer screening with mammography. The objectives are to increase the mammography use rate among female Medicare beneficiaries and as a result reduce the incidence of late-stage breast cancer in this population.
The quality indicator measured by CMS for the PROs National Breast Cancer Prevention project is the percentage of non-HMO female beneficiaries aged 52-69 who have had a screening or diagnostic mammogram during a 2-year period. The recommendation of the American College of Surgeons and the American Cancer Society is that mammography be performed annually after age 45 or 50. The reason for the PRO’s biennial measurement was to determine whether a woman was being tested at all and to overcome the measurement problem if a mammogram was performed at 1 year plus 1 day.
Data for this indicator are collected using Medicare claims data. These data (see Table 6) reveal a lower than expected rate of mammography use. According to the 1992 National Health Interview Survey, the following factors were associated with reduced mammography use: lack of physician recommendation, a common misconception that without symptoms there is no need to get screened, lack of awareness about mammography, cost and/or lack of health insurance, lack of access to mammography facilities, fear of cancer detection, and cultural beliefs and values not consistent with preventive medical care.39
| Table 6. National Rates: Quality Indicators for National Breast Cancer Project | |||
| Quality Indicator | Potential Impact | National Median (%) | Range (%) |
| Mammogram within a 2-year period |
Randomized controlled trials in the United States and Europe indicate clearly that use of regular screening mammography can reduce breast cancer mortality by 20-40% for women aged 50 years and older. Based on a meta-analysis of 13 studies reported from 1966 to 1993, it appears that judicious use of mammography can prevent approximately one-fourth of breast cancer deaths.37 |
Aged 50-67: 55.9 Aged 68 +: 42.7 All: 44.6 |
47.4-65.6 34.8-51.3 37.2-53.3 |
| >* Fee-for-service patients only (claims data) for period Jan. 1, 1997-Dec. 31, 1998. | |||
Many of the interventions developed by the PROs to increase breast cancer prevention are guided by recommendations developed by Evidence-based Practice Centers (EPCs), which were commissioned by the Agency for Health Care Policy and Research (AHCPR)—now the Agency for Health Research and Quality (www.ahrq.gov). The role of these centers is to conduct systematic reviews of the literature and report on the effect of healthcare interventions.
In the case of breast cancer prevention, these centers have not uncovered a "magic bullet," for increasing mammography use, but they did find that organizational rather than individual change was one of the most consistently effective means of improving cancer screening. While no one organizational change was superior to others, examples of successful interventions involved the use of a "prevention team" that included nurse standing orders for mammography and use of a health educator to contact patients via telephone. Patient and provider reminders were also effective at increasing use of cancer screening. Patient reminders that were personalized were superior to those that were generic. Provider reminders, particularly those making use of computerized information technology, appeared to be useful and cost-effective. On average, the simultaneous use of multiple intervention strategies enhanced effectiveness.40
In addition, many PROs, including Ohio KePRO, have published newsletters directed at beneficiaries. These newsletters provide beneficiaries with information regarding Medicare’s coverage of screening mammograms as well as accurate information regarding mammography. In addition to providing beneficiaries with information, this forum is used to encourage beneficiaries to take an active role in their healthcare. Many PROs are also helping spread the "word" through partnerships with breast cancer coalitions within their respective states.
Diabetes
Adult onset diabetes mellitus affects 1 in 10 Americans older than the age of 65. In some states, 25% of all people diagnosed with diabetes are Medicare beneficiaries. Diabetes is the seventh leading cause of death (sixth leading cause of death by disease) in the United States. Diabetes contributed to 198,140 deaths in 1996.41
Diabetes is one of the most costly health problems in America. Healthcare and other costs directly related to diabetes treatment, as well as the costs of lost productivity, run $98 billion annually.41 Individuals with diabetes have 2-5 times higher per capita medical expenditures and per capita out-of-pocket expenditures than people without diabetes.
The complications of diabetes include heart disease, stroke, vision loss/blindness, amputations, and renal disease. It is recognized that HgA1c should be obtained at least quarterly in patients with uncontrolled (or poorly controlled) diabetes. Similarly, dilated eye examinations and lipid profiles should be performed annually based on American Diabetes Association guidelines. The goal of the National Diabetes Project is to reduce the rates of blindness, amputations, renal failure, and diabetes-associated cardiovascular disease. The short-term objectives of the project are to determine whether key examinations and laboratory tests are being obtained at all and to increase the rates at which they are obtained. Many opportunities for improvement are reflected in recent CMS data (see Table 7).
| Table 7. National Rates: Diabetes Project Quality Indicators | |||||
| Quality Indicator | Potential Impact | 1996-1999* Median (%) | National Median** (%) | Range (%) | |
| Annual HbA1c |
Control of mean blood glucose is essential to prevent complications |
59.0 | 70.6 | 41.2-85.3 | |
| Biennial eye exam |
Early detection and treatment of retinal disease prevents blindness. |
44.2 | 69.1 | 54.1-79.7 | |
| Biennial lipid profile |
Control of lipids will decrease rates of vascular and renal complications. |
68.4 | 56.8 | 38.8-72.7 | |
| FFS patients only (claims data). | |||||
| * Baseline values from 19 peer review organization projects performed during 1996 through 1999. | |||||
| ** Baseline data published by Jencks et al. | |||||
In our continuing efforts to enhance the clinicians’ ability to meet the healthcare needs of their patients, PROs develop and facilitate the use of interventions designed to improve care. Among these interventions are tools developed for office collection of performance data, patient reminders and beneficiary newsletters stressing the importance of diabetes screening, referral documents, foot exam posters, and other office aids.
Collaborative educational efforts are being implemented. Partnerships with the American Academy of Ophthalmology, the American College of Optometry, and the American College of Podiatric Medicine have been established. The goals of these collaborations are to increase primary care physicians’ awareness and use of strategies to reduce visual loss secondary to diabetic retinopathy and increase proficiency in performing screening foot examinations.
In an effort to foster patient-centered care, PROs such as Ohio KePRO have supported the development of tools such as the Diabetes Self-Help Handbook, which are designed to shift control of care to the patient.42
Summary
The article by Jencks et al is a challenge to all healthcare stakeholders to collaborate in a comprehensive quality improvement effort. This effort must be coordinated, focused, and inclusive at all levels. Physicians must be involved as proactive, well-informed opinion leaders, sponsors, and team members. We must be a resource to assist the stakeholder teams in overcoming barriers created by our peers and others and involve patients in their own care processes.
Recent articles have highlighted the total commitment that must be present at all levels.53,54 It is quite clear that at the hospital and healthcare system levels, there must be active participation by governing boards, management, and physician leadership. Our goal as PROs is to encourage and support healthcare professionals and providers in their efforts to meet this challenge.
References
1. Meehan TP, et al. Quality of care, process, and outcomes in elderly patients with pneumonia. JAMA. 1997;278:2080-2084.
2. Randomised trial of intravenous streptokinase, oral aspirin, both, or neither among 17,187 cases of suspected acute myocardial infarction: ISIS-2. ISIS (Second International Study of Infarct Survival) Collaborative Group. Lancet. 1988;2:349-360.
3. Balas EA, Boren SA. Managing clinical knowledge for health care improvement. Yearbook of Medical Informatics. Bethesda, Md: National Library of Medicine; 2000:65-70.
4. Sackett DL, et al. Evidence based medicine: What it is and what it isn’t. BMJ. 1996;312:71-72.
5. Jencks SF, et al. Quality of medical care delivered to Medicare beneficiaries: A profile at the state and national levels. JAMA. 2000;284:1670-1676.
6. Health Care Financing Review. Medicare and Medicaid Statistical Supplement, 1998. Baltimore, Md: Health Care Financing Administration; 1998.
7. Marciniak TA, et al. Improving the quality of care for Medicare patients with acute myocardial infarction: Results from the Cooperative Cardiovascular Project. JAMA. 1998;279: 1351-1357.
8. Ryan TJ, et al. Committee on management of acute myocardial infarction. 1999 update: ACC/AHA Guidelines for the management of patients with acute myocardial infarction. Circulation. 1999;100:1016-1030.
9. Espinosa JA, Kosnik L. Healthcare storytelling as practical magic: Lessons learned in our five-year journey. QuIC/IHI Breakthrough Series Collaborative: Improving Safety in High Hazard Areas. Palm Harbor, Fla. 2001.
10. O’Connell JB, Bristow MR. Economic impact of heart failure in the United States: Time for a different approach. J Heart Lung Transplant. 1994;13:S107-112.
11. Heart Failure Society of America (HFSA) Practice Guidelines: HFSA guidelines for management of patients with heart failure caused by left ventricular dysfunction-pharmacological approaches. J Card Fail. 1999;5:357-382.
12. Guidelines for the evaluation and management of heart failure. Report of the American College of Cardiology/American Heart Association Task Force of Practice Guidelines (Committee on Evaluation and Management of Heart Failure). Circulation. 1995;92:2764-2784.
13. Institute for Clinical Systems Improvement. 8009 34th Avenue South, Suite 1200, Bloomington, MN 55425. www.icsi.org.
14. Wachter RB, Goldman L, Hollander H, eds. Hospital Medicine. Baltimore, Md: Lippincott, Williams & Wilkins; 2000.
15. Grady KL, et al. Team management of patients with heart failure: A statement for healthcare professionals from The Cardiovascular Nursing Council of the American Heart Association. Circulation. 2000;102:2443-2456.
16. Krumholz HM, et al. Evaluating quality of care for patients with heart failure. Circulation. 2000;101:E102-140.
17. Young JB. Carvedilol for heart failure: Renewed interest in beta-blockers. Cleve Clin J Med.1997;64:415-422.
18. Packer M, et al. Effect of carvedilol on survival in severe chronic heart failure. N Engl J Med. 2001;344:1651-1658.
19. The Beta-Blocker Evaluation of Survival Trail (BEST) Investigators. A trial of the beta-blocker bucinidolol in patients with advanced chronic heart failure. N Engl J Med. 2001;344: 1659-1667.
20. Braunwald E. Expanding indications for beta-blockers in heart failure. N Engl J Med. 2001;344:1711-1712.
21. Crossing the Quality Chasm: A New Health System for the 21st Century. Institute of Medicine, 2001. www.iom.edu.
22. American Heart Association. 2001 Heart and Stroke Statistical Update. American Heart Association: Dallas, Tex; 2000.
23. Go AS, et al. Prevalence of diagnosed atrial fibrillation in adults. JAMA. 2001;285:2370-2375.
24. Fintel DJ, Hoffman C. The AFP Guide to Preventing Strokes and Lowering Health Risks in Patients with Atrial Fibrillation. Lisle, Ill: Illinois Academy of Family Physicians; 2000.
25. Matchar DB, et al. Medical treatment for stroke prevention. Ann Intern Med. 1994;121(1):41-53.
26. Adams HP, et al. Guidelines for thrombolytic therapy of stroke: A supplement to guidelines for the management of patients with acute ischemic stroke. A statement for healthcare professionals from a special writing group of the stroke council, American Heart Association. Circulation. 1996;94:1167-1174.
27. Adams HP, et al. Guidelines for the management of patients with acute ischemic stroke: a statement for healthcare from a special writing group of the stroke council, American Heart Association. Stroke. 1994;25:1901-1914.
28. To Err Is Human: Building a Safer Health System. Kohn LT, Corrigan JM, and Donaldson MS, eds. Institute of Medicine; 2000. www.iom.edu.
29. Marston BJ, et al. Incidence of community-acquired pneumonia requiring hospitalization: Results of a population-based active surveillance study in Ohio. Arch Intern Med. 1997;157: 1709-1718.
30. Robinson KA, et al. Epidemiology of invasive Streptococcus pneumoniae infections in the United States, 1995-1998: Opportunities for prevention in the conjugate vaccine era. JAMA. 2001; 285:1729-1735.
31. Dicker RC, et al. Quality of care surveillance using administrative data. 1996. Quality Resume, No. 2. Baltimore, Md: Health Care Financing Administration; 1998.
32. Bartlett JG, et al. Practice guidelines for the management of community-acquired pneumonia. Infectious Disease Society of America. Clin Infect Dis. 2000;31:347-382.
33. Niederman MS, et al. Guidelines for the initial therapy of community-acquired pneumonia. Am Rev Resp Dis. 1993;148: 1418-1426.
34. Immunization 2000: Flu and Pneumonia. Physician Office/Clinic. Ohio KePRO. Seven Hills, Ohio; 2000.
35. Immunization 2000: Flu and Pneumonia. Acute Care Hospital. Ohio KePRO. Seven Hills, Ohio; 2000.
36. Immunization 2000: Flu and Pneumonia. Home Health/Dialysis Center. Ohio KePRO. Seven Hills, Ohio; 2000.
37. American Cancer Society. Current Facts and Figures 2001. Available: www.cancer.org/statistics/
38. Reis LAG, et al, eds. SEER Cancer Statistics Review, 1973-1991; Tables and Graphs. Bethesda, Md: National Cancer Institute; 1994. (NIH Publication#94-2789.)
39. Kerlikowske K, et al. Positive predictive value of screening mammography by age and family history of breast cancer. JAMA. 1993;270(20):2444-2450.
40. Evidence report and evidence-based recommendations: Interventions that increase the utilization of medicare-funded preventive services for persons age 65 and older. www.hcfa.gov/healthyaging/download/2a1.doc.
41. National Diabetes Data Group. Diabetes in America. 2nd ed. Harris M, ed. Bethesda, Md: National Institutes of Health; 1995.
42. Managing Your Diabetes: You Can Do It! Ohio KePRO. Seven Hills, Ohio; 2000.
43. Trent R, et al. Impact of resuscitation and thrombolysis on mortality rate in acute myocardial infarction. Int J Cardiol. 1995; 49:33-37.
44. Yusuf S, et al. Beta blockade during and after myocardial infarction: An overview of randomized trials. Prog Cardiovasc Dis. 1985;27:335-371.
45. Khalil ME, et al. A remarkable medical story: Benefits of angiotensin-converting enzyme inhibitors in cardiac patients. J Am Coll Cardol. 2001;37:1757-1764.
46. Burling TA, et al. Smoking following myocardial infarction: A critical review of the literature. Health Psychol. 1984;3:83-96.
47. Parmley WW. Evolution of angiotensin-converting enzyme inhibition in hypertension, heart failure, and vascular protection. Am J Med. 1998;105(1A):27S-31S.
49. Berry BB, et al. Influenza vaccination is safe and immunogenic when administered to hospitalized patients. Vaccine. 2001; 19:3493-3498.
50. Influenza and Pneumococcal Vaccination Levels Among Adults > 65 years-United States, 1997. MMWR Morb Mortal Wkly Rep. 1998;47:797-802.
52. Use of Standing Orders Programs to Increase Adult Vaccination Rates: Recommendations of the Advisory Committee on Immunization Practices (ACIP) MMWR Morb Mortal Wkly Rep. 2000; 49(RR01):15-26.
53. Bradley EH, et al. A qualitative study of increasing beta-blocker use after myocardial infarction: Why do some hospitals succeed? JAMA. 2001;285:2604-2611.
54. Weiner BJ, et al. Promoting clinical involvement in hospital quality improvement efforts: The effects of top management, board, and physician leadership. Health Serv Res. 1997;32:491-510.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
