Special Feature: Should the Definition of ARDS be Changed?
Special Feature
Should the Definition of ARDS be Changed?
By Jun Takezawa, MD
Although a tremendous amount of resource has been allocated to develop a novel treatment for the acute respiratory distress syndrome (ARDS), all the clinical trials to date—such as those using anticytokine therapies, NO inhalation, surfactant, and prone positioning—have failed, except for the low tidal volume strategy trial organized by the ARDS network of the National Institutes of Health (NIH).1 Several factors are speculated to be responsible for these disappointing results, and most of them are addressed to the definition or diagnostic criteria of ARDS. In this article, background of this argument and its rationale are reviewed and the future direction of clinical trials on ARDS is addressed.
Background: Why Change of ARDS Definition is Recommended
One of the biggest arguments in the definition of ARDS is related to diagnostic criteria. Regarding the interpretation of chest x-ray film, massive atelectasis in the dependent regions of both lungs and the bilateral presence of small amounts of pleural effusion are easily misdiagnosed as bilateral infiltrates. Considerable interobserver variation in chest radiograph interpretation has been documented.2,3 Interobserver variation of chest radiograph interpretation for ARDS by intensivists was also evaluated by Canadian hospitals, and it was found that agreement of the interpretation between intensivist and radiologist was 60-80%. Meade and colleagues recommended the provision of chest x-ray reading consensus training before starting a clinical trial;4 otherwise, the findings of the study may be misled, and/or a very large sample size is required to reach the final conclusion.
The second argument is related to severity of lung injury. According to the definition of ARDS by the American-European Consensus Conference on ARDS,5 the deterioration of pulmonary gas exchange is assessed by the P/F ratio (arterial PO2 divided by inspired oxygen fraction), independently of the level of positive end-expiratory pressure (PEEP). However, it is well known that the PEEP level can easily affect the P/F ratio, and this can become the source of bias for patient entry in the clinical trial. Additionally, whether the magnitude of deterioration in pulmonary gas exchange at the initial stage of ARDS affects outcome is still unknown. On the other hand, although the peak airway pressure (PIP) level is well known to affect the outcome of ARDS patients, lung compliance—that is, the reflection of PIP during volume-targeted ventilation—was not taken into account in determining the severity of lung injury. As a result, severity of lung injury in terms of both pulmonary gas exchange and lung mechanics is not included as a risk factor in the outcome of ARDS.
The third argument is related to diverse etiologies and a variety of clinical manifestations of ARDS. Although several etiologic factors such as the effects of neutrophils and cytokines have been nominated as candidates, the precise mechanism for developing ARDS is still unclear. Thus, it is likely that treatment modalities may attempt to target diseases of different etiologies, which are encompassed in disease categories termed as a syndrome. This would not only require a large sample size but also inherit a risk of unknown confounders being unequally distributed in both arms of the randomized clinical trials (RCTs).
Bilateral infiltrates developed during bacterial and interstitial pneumonia can fulfill the diagnostic criteria of ARDS. However, treatment should be focused on the original disease rather than ARDS itself to improve outcome. Therefore, unequal distribution of these types of pneumonia in the treatment and control arms interferes with the quality of any RCT. Evaluation of a risk factor and its outcome also supports this context where mortality of ARDS associated with sepsis is much higher than that associated with trauma, extracorporeal circulation, and massive transfusion.
The fourth argument is similar to that being referred to during the clinical trial for sepsis such that the initiation of intervention as a trial was too late to affect the outcome of septic patients. This concern encouraged the development of the new concept of the systemic inflammatory response syndrome (SIRS). However, this expansion of inclusion criteria requires a large number of enrolled patients, and the improvement of mortality becomes extremely small even though it reaches a significant difference (thus making the interpretation of its clinical merit difficult).
The fifth argument is that ARDS can be regarded as a complication, such as with nosocomial infections. Therefore, patient outcome is affected by both severity of illness (usually assessed by the APACHE scoring system) and severity of complication (ARDS) itself. However, the overlapped effect of this complication on outcome has not been well stratified.6 Table 1 shows a comparison of outcomes between ARDS and overall patients who were admitted to ICUs and required mechanical ventilation in 31 Japanese ICUs. Both predicted and actual mortality of ARDS patients were higher than that of patients who required mechanical ventilatory support. However, the standardized mortality rate (SMR) of ARDS patients was much higher than that of overall ventilated patients (1.25 vs 0.76). In other words, the APACHE score could not accurately predict mortality of ARDS patients.
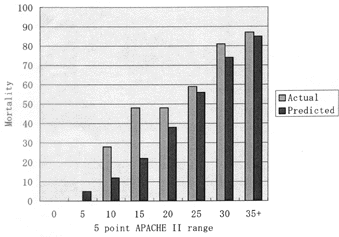
Comparison of actual and predicted mortality of the ARDS patients (289 patients) in Japanese ICUs indicates that the actual mortality of the ARDS patients was higher than predicted mortality in the full range of APACHE score (see Figure). Especially in the 5-10 and 10-15 ranges of APACHE score, actual mortality was more than twice of that predicted, indicating again that the APACHE scoring system did not stratify the ARDS patients.
Outcome Comparison Between ARDS and All Ventilated Patients in ICUs
ARDS Ventilated Cases No. of Patients 289 5738 Predicted Mortality (%) 49.5 27.5 Actual Mortality (%) 61.9 20.9 SMR 1.25 0.76 ICU Mortality (%) 48.4 13.3 LOS in ICU (days) 12.9 5.9 LOS in Hospital (days) 67.4 55.7 Ventilation Day (days) 10.9 3.1 LOS: Length of stayThe Future Direction of Clinical Trials for ARDS
In order to organize a clinical trial either from the standpoint of a professional society, government, or pharmaceutical company, the effect of ARDS on the overall health care system such as volume, mortality, cost, and burden should be assessed. Each country has a different priority for ARDS as a health care challenge. Unfortunately, most countries, including Japan, have no such database, making it difficult to determine the priority of ARDS as an issue of health care policy.
In addition to the inaccuracy of diagnosis, the biggest problem associated with clinical trials of ARDS is that severity of lung injury is not taken into account as a risk factor for the outcome. If severity of lung injury does not affect the outcome of ARDS, ARDS should not be a target of treatment. It should be the first step to make a (inter) national database for disease registration for the stratification of severity of ARDS in terms of outcome. A new prognosis predicting scoring (PPS) system may be required with the combination of both APACHE score and severity of lung injury, because APACHE system alone does not stratify ARDS patients. This PPS system may be made based on primary diseases. If this attempt is to be made, international collaboration is required because a large number of patients should be registered to establish a primary disease-based PPS system of ARDS for epidemiological evaluation.
1. The Acute Respiratroy Distress Syndrome Network. N Engl J Med. 2000;342:1301-1308.
2. Tudor GR, et al. Clin Radiol. 1997;52:235-238.
3. Acad Radiol. 1969;41:10-14.
4. Meade MO. Am J Respir Crit Care Med. 2000;161: 85-90.
5. Bernard GR. Am J Respir Crit Care Med. 1994; 149:818-824.
6. Knaus WA, et al. Am J Respir Crit Care Med. 1994; 150:311-317.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
