From a small seed to a garden of data
From a small seed to a garden of data
A little idea grows to fruition at Iowa hospital
When Diane Prieksat, RN, BSN, CIC, started her job as director of quality and medical staff services at Mercy Medical in Sioux City, IA, two years ago, she often struggled to gather data from various sources.
"We used to report based on who we were doing the data collection for," she says. The list included ORYX indicators, Healthy People 2000, the Institute for Quality Healthcare, and national registries for oncology, trauma, and myocardial infarctions. There were reports for various internal departments and for some 65 indicators requested by various medical staff. But nowhere was there a master list of what was being collected and for whom. "I thought it would make my life easier if I could find out all about a particular area without having to grab a whole bunch of reports."
Turning data into information
Starting with a list scribbled on her office white board, Prieksat developed an idea that came to be known as Service Line Indicator Reporting. Like many other industries, it involved looking at each line of business as a unit rather than looking at various aspects of all lines of business. For example, rather than looking at the average charges for a heterogeneous group of patients, the data would be developed based on diagnostic-related groups. In addition, the data wouldn’t be limited to one particular element — financial, quality, or satisfaction — but would include all data sets in one report.
The result is a data repository and management program that has been lauded by Prieksat’s hospital, the Trinity Health System, and even the Joint Commission on Accreditation of Healthcare Organizations (JCAHO). She eliminated what she called a "data rich, information poor" environment and created a system in which data is collected, mined, and actually used. And Prieksat can tell you exactly what information is being collected and how it is being used at any given time.
Prieksat’s first step was to determine what was being collected and why. One of Prieksat’s colleagues, director of clinical and physician services at Trinity Health, Paul Conlon, along with Prieksat and her staff, held a data summit in which every department was quizzed about what data it gathered and how it was used.
"We asked them what, how long it was being collected, why, how it is being used, who sees it, what the trends over time are, and whether they were using any benchmarks," she recalls. "This really got people thinking."
The summit revealed a lot of duplication, as well as data being continuously collected for some specific need that had expired long ago. That alone led to a reduction in work. Working with the staff in the quality services department, Prieksat developed a data repository that can tell her at any point in time what information is being gathered as well as performance improvement programs related to that data element.
Wherever possible, Prieksat and her team also eliminated the need for paper records. "We used to fill out records on paper and then send them up to be input electronically," she notes. "Whenever we can, we only have it input electronically now." The hospital also purchased an autoscan machine that allows for easy conversion of paper data to graphics.
Marrying the elements
When recruited to her position at Mercy, Prieksat was challenged by her CEO to focus improvement initiatives on meeting the hospital’s "mission critical" focus areas — quality and service, relationships, and financial performance. One of the weaknesses of previous data gathering initiatives was that they rarely included all three of those "mission critical" elements. "I wanted to see all three elements on one report: the quality and outcomes-related data, the relationship data, and the financial data. Working with her systems analyst, the vision became a reality. "Information relative to each service line is presented in a concise service report," Prieksat explains. "It includes graphs that allow for analysis of trends over time and benchmarking to best in class’ data."
In the first category is data including structural, process, outcomes, and clinical appropriateness indicators; benchmarks; variances, claims, and litigation; clinical pathways; and performance improvement initiatives.
For obstetrical cases, for instance, there would be data on admissions, how many of those were by which kinds of physicians, and the total number of physicians admitting. Data on mortality rates, average length of stay, and vaginal vs. cesarian section delivery rates would also be included in the reports, as would information on medical errors, falls, and other adverse events. How all the data compare to the hospital’s previous rates, as well as how they compare to benchmark data, is included.
Relationship data includes patient, employee, and physician satisfaction; service care standards; service recovery; community and systemwide assessment and initiatives; and staff and physician continuing education.
Financial data includes information on market share; estimated costs, charges, and reimbursement; analysis of charges by UB92 code; revenue; and payor mix.
Having these elements available together has led to some solid positive outcomes. For example, in obstetrics, having all of the charges analyzed by UB92 code enabled the facility to determine why vaginal births were costing more than C-sections. Nurses were often grabbing supplies a la carte, rather than grabbing packs. Once that was determined, practices changed and costs decreased.
Another benefit, says Prieksat, is that more people are involved and interested in data collection, management, and use. "When the reports are completed, they are shared with all the stakeholders, from front line staff to physicians and administration," she says. Even marketing is involved, since data is used as part of the strategic planning process. All of those stakeholders are involved in developing an action plan with a time line. "Even if our statistics look great, there’s always the need to continuously improve."
In the obstetrics department, getting the team together to discuss the report created a lot of interest. "They wanted to figure out why things were the way they were and what could be done to change it," says Prieksat.
"This has enhanced staff motivation and input and created a systematic method of measurement of all aspects of delivery of care," she says. "JCAHO loves it, and we are better able to understand how all three areas interrelate. We can identify variation in the clinical management of patients quickly, and develop action plans for eliminating that variation."
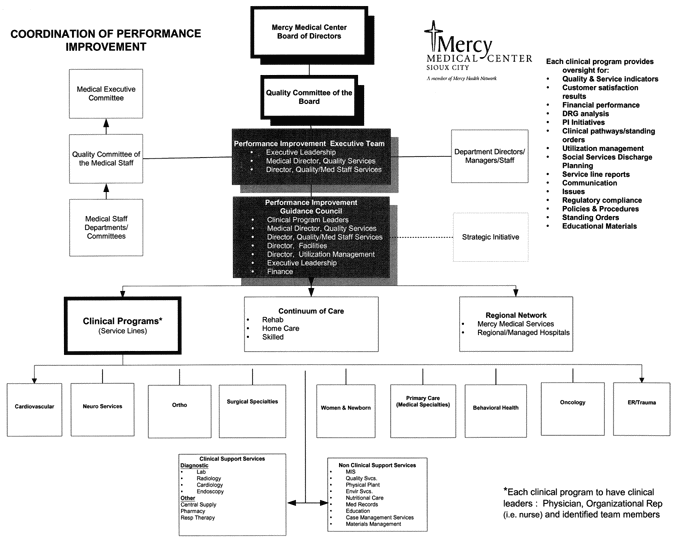
One of the strategic initiatives of Mercy Medical Center is to continuously enhance physician involvement and alignment, particularly in improvement initiatives. In collaboration with the hospital’s chief medical officer, Larry Sellers, MD, and medical director of quality services, Ross Bacon, MD, Prieksat recently redesigned the framework for evaluating and coordinating performance improvement at the facility. (To see Mercy’s redesigned framework, see inserted chart.)
Service line teams, led by a physician and nurse specializing in those areas and including a multidisciplinary team of appropriate hospital and medical staff, will be responsible for reviewing and analyzing all reports and progress related to quality and service, customer satisfaction, financial performance, DRG analysis, and utilization management.
In addition, she notes, these teams will identify variation in clinical management of patients and diagnoses, develop clinical pathways, identify opportunities for improvement, and assess educational needs for hospital and medical staff. The activities of each of the service line teams will be coordinated through the performance improvement guidance council, and represented by the service line physician and nurse leaders, as well as various hospital and administrative staff.
The service line approach that Prieksat implemented has received widespread support at the hospital. "It supports the concept that performance improvement should be data-driven, coordinated, and continuous," she says.
[For more information, contact:
• Diane Prieksat, RN, BSN, CIC, director of quality & medical staff services, Mercy Medical Center, 801 Fifth St., Sioux City, IA 51101. Telephone: (712) 279-2389.]
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
