Interesting New Developments in Hypertension
Interesting New Developments in Hypertension
Abstracts & Commentary
Synopsis: These studies call for trials to see whether pharmacologic treatment of high-normal blood pressure will reduce cardiovascular events.
Sources: Vasan RS, et al. N Engl J Med. 2001;345: 1291-1297; Panza JA. N Engl J Med. 2001;345:1337-1340; Staessen JA, et al. Lancet. 2001;358:1305-1315.
The framingham heart study investigators have reported on the relationship between gradations of normal blood pressure (BP) and cardiovascular events during long-term follow-up of a large cohort of the original subjects as well as participants in the Framingham Offspring Study, followed for up to 12 years. Subjects were stratified on the basis of optimal, normal, or high-normal BP. The results indicate that high-normal BP imparts significant risk, particularly in older men and women. A total of 6859 subjects were included in this observational report. Examinations were carried out every 2 years. Baseline BP was recorded at one of the Framingham biannual examination cycles. Based on JNC VI and WHO-ISH criteria, optimal BP was defined as less than 120/80; a normal BP as 120-129/80-84; and high-normal as 130-139/85-89 mm HG. Hypertension was defined as a BP of > 140/90 mm HG or use of anti-hypertensive therapy. The primary outcome was time to occurrence of cardiovascular death, myocardial infarction, stroke, or congestive heart failure during the 11- to 12-year follow-up. A variety of statistical methods were used, including separate tracking of subjects who progressed to higher levels of BP during follow-up, and calculation of a theoretical number needed to treat for 5 years to prevent one major event. At baseline, one third of the cohort had normal BP, one quarter had high-normal BP, and the rest had optimal BP levels. The high-normals were older, had higher cholesterol levels, and greater BMI than those with optimal BP.
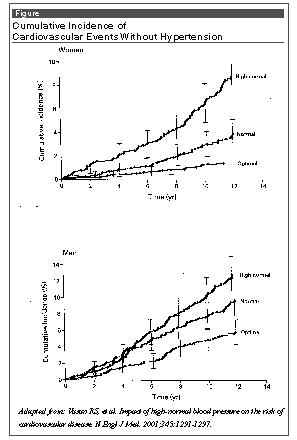
Results: The mean follow-up was 11 years; 397 cardiovascular events were documented, of which approximately half were myocardial infarction. There was an increasing risk of cardiovascular events in the middle and highest categories of BP (see Figure). Furthermore, in subjects < 65 years of age with high-normal BP, the 10-year cumulative incidence of cardiovascular events was only 4% in women and 8% in men. In contrast, in those individuals between 65 and 90 years, the event rates were 18% in women and 25% in men (a 3- to 4-fold increase), confirming that advanced age plus high-normal BP is a particularly lethal combination. Compared to optimal BP, the high-normal cohort had an adjusted hazard ratio of 2.5 in women and 1.6 in men. The normal BP cohort had an adjusted hazard ratio of 1.5 for women and 1.3 for men. In individuals whose BP increased over follow-up, there was a greater risk of cardiovascular disease. Vasan et al estimated that the number needed to treat to prevent 1 cardiovascular event in older subjects ranges from 24-71 in men and 34-102 in women, substantially higher than in younger subjects. NHANES III and other data indicate that the prevalence of high-normal BP is comparable to that of mild hypertension in the United States. Thus, the findings indicate a continuous and increased cardiovascular risk across 3 nonhypertensive BP cohorts, more so in men than women. The 10-year absolute event rate in older subjects was > 20% in men and close to 20% in women, thus meeting criteria for moderate to high risk for primary prevention interventions. Vasan and colleagues call for clinical trials to see whether pharmacologic treatment of high-normal BP will reduce cardiovascular events. They emphasize that risk in the high-normal cohort may not be solely related to the BP levels, as other studies have shown increased carotid IMT and LV diastolic abnormalities in such individuals.Comment by Jonathan Abrams, MD
In an accompanying editorial, Panza discusses the evidence for endothelial dysfunction in hypertensive patients, related to decreased nitric oxide availability and increased endothelin-1 levels. It is not known whether such abnormalities are present in individuals with high-normal BP, but based on the literature, it is likely that this is the case. Further, it is possible that many of the high-normal BP subjects have or are more likely to develop the insulin-resistance syndrome over time. The increase in other CAD risk factors, particularly higher cholesterol and BMI in the high-normal subjects, further confounds the issue. The issue of therapy for such individuals is speculative, but the Framingham observations are of real importance because of the clear and consistent gradient of increased cardiovascular end points as BP goes from the lowest to the highest levels, yet all within the normal range. This gradation of risk is similar to that with total LDL cholesterol levels, as well as glycemic control in diabetics. In all these conditions, less is more.
Another publication appearing in the Lancet examines the question as to whether sepecific pharmacologic therapy for hypertension has salutary effects beyond BP lowering. This is a new meta-analysis of antihypertensive drugs from Belgium. The data focus on systolic BP in middle-aged and older individuals. Two different analyses were carried out. One compared outcome results in trials that used "old" agents, such as diuretics and beta blockers, with new agents, including calcium channel blockers (CCB), ACE inhibitors, and alpha blockers. Eleven trials were included. The second component was to examine the relationship between treatment groups and the corrected baseline BP differences, ie, was the effectiveness in reducing events in part related to non-BP lowering actions of a given class of therapy. A total of 27 studies were included in this meta-analysis, which compared older drugs to each other and newer classes compared to other newer compounds. The trials included more than 33,000 subjects randomly assigned old drugs and 29,000 given new drugs.
Results: 1) New antihypertensive drugs (CCB, ACE inhibitors) were as effective as older ones (diuretics, beta blockers) for prevention of cardiovascular death, stroke, fatal, and nonfatal myocardial infarction; 2) patients randomized to diuretics or beta blockers had similar outcomes to those receiving initial treatment with a CCB or ACE inhibitor; 3) overall risk of stroke was decreased with CCB, but CCB increased the risk of myocardial infarction; 4) in an analysis of the degree of BP reduction to cardiovascular end points, there was a reduction in events directly related to gradations of BP. Thus, BP differences during follow-up accounted for all differences in outcomes between treatments. Staessen and colleagues conclude that "results of outcomes trials for anti-hypertensive drugs can be explained by BP differences between randomized groups;" 5) all antihypertensive drugs had similar long-term efficacy and safety; 6) this analysis could not confirm that non-antihypertensive actions of various agents are of importance in influencing cardiovascular end points as opposed to the actual degree of BP lowering; the lower the BP, the greater reduction in cardiovascular complications.
Staessen et al point out that this relationship has been shown previously in isolated systolic hypertension, with substantial reductions in stroke and myocardial infarction attributable to relatively modest differences in BP reduction between groups. Even after adjustment for baseline BP, the conclusions remained the same. The analysis suggests that for all outcomes combined, a 5 mm HG difference in systolic pressure was clinically important. Furthermore, "all possible benefits" of therapy were seen at systolic BP gradients or differences of about 15 mm HG. (However, this degree of BP difference was achieved in only 4% of patients in the entire analysis). Staessen et al discuss the HOPE trial and the hypothesis of these investigators and others that the benefits from ramipril were unrelated to BP lowering; there was a 3.3 mm HG difference in systolic pressure between ramipril in HOPE and placebo. They conclude that BP lowering itself could have accounted for most of the benefits in HOPE in those allocated to ramipril. In summary, the conclusions of this "quantitative overview" of many thousands of patients suggests that CCB and ACE inhibitors are equally effective as diuretics and beta blockers in decreasing multiple fatal and nonfatal cardiovascular outcomes, and offer comparable protection. CCB appear to reduce the risk of stroke more than other agents but impart a lesser protection for myocardial infarction. Similar conclusions have been made in 2 recently published meta-analyses of hypertensive therapy emphasizing CCBs.1,2 Staessen et al stress that this analysis emphasizes "the desirability of BP control," and that any suggestion that a given class of drugs may have clinically relevant actions over and above BP lowering remains an unproven hypothesis.
Comment by Jonathan Abrams, MD
This is another significant contribution to the mega hypertension meta-analysis industry. The conclusions are concordant with other analyses, although this publication represents the largest number of patients analyzed (27 trials). As Staessen et al point out, the various published BP trials are disparate and not homogenous in design, use of statistical analysis, and methodology in measuring end points. Also, this meta-analysis uses combined or summary data; individual patient data were not entered, as is the case in a more formal meta-analysis. This may result in somewhat less reliability and validity. As in other meta-analyses, researchers pick and choose among the studies selected for analysis. The controversy about safety of calcium channel blockers will linger. It does appear, based on several different meta-analyses of contemporary antihypertensive therapy, that CCBs have a greater effect on lowering stroke rates than other agents but are less protective regarding reduction in myocardial infarction. This does not necessarily mean that CCBs are hazardous but may indicate only that they are somewhat less potent than other agents, particularly beta blockers and ACE inhibitors, in reducing infarction rates. This analysis strongly supports that the optimal BP lowering target is as low as is feasible without producing limiting side effects. One might not have thought small differences in mean systolic BP levels between 2 study cohorts, such as 2-5 mm HG, would have a significant effect on cardiovascular event rate gradients, but this appears to be the case. Thus, the arguments of Peter Sleight and the HOPE investigators that the modest BP differences in that study between ramipril and placebo are not important must be reconsidered in light of this meta-analysis. High-risk populations, such as the elderly (see first review on page 91), diabetics, and those with established vascular disease, are particularly vulnerable to the effects of hypertension. Such individuals demand even more vigorous and aggressive efforts to lower BP. In conclusion, more is better with respect to BP lowering. All commonly used agents are effective, well tolerated, and have excellent safety profiles. There is no excuse for physicians not to effectively use these data in daily practice.
References
1. Lees, K, et al. Lancet. 2000;355:1949-1954.
2. Neoptolemos J, et al. Lancet. 2000;355:1955-1960.
![]()
A progressive gradation in risk of cardiac events over the high-normal to abnormal range has been shown for:
a. blood pressure.
b. LDL cholesterol.
c. blood glucose.
d. All of the above
::::
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
