Discharge Planning Advisor: Discharge process enables faster placement
Discharge Planning Advisor: Discharge process enables faster placement
Report quality greatly enhanced, CM director says
Case managers at New York Hospital of Queens in Flushing are using a new software tool to determine the availability of post-acute services, then request and schedule those services over the Internet, says Caroline Keane, RN, MSN, ANP, CCM, director of case management and social work.
Since implementing eDischarge, a product of Curaspan Inc., in Needham, MA, in mid-January, her staff have dramatically reduced time spent on the telephone, enhanced the quality of report writing, and are able to make more precise matches of patients with care facilities, she says.
CM drives discharge plan
"It’s real time," she explains. "We used to send out PRIs [patient review instruments] — maybe a 20-page package — to five facilities via fax. Even though it was programmed into the fax machine, it took a lot of effort, and then maybe it didn’t go out right. Now we put in one [PRI] and send it out to all five at once. The PRIs are much more legible."
The high-quality reports alone are a huge plus to her operation, Keane says. But Columbia Presbyterian, the network to which her hospital belongs, chose to implement eDischarge in large part because of the patient privacy protection it provides, she notes.
With the privacy regulations of the Health Insurance Portability and Accountability Act (HIPAA) becoming effective in April 2003, Keane adds, "we’re looking toward the future. This is an encrypted system, a secure system. We decide how much information the person on the other side receives, and at what time we give it."
As part of the eDischarge process, post-acute providers that take referrals from the hospital, including skilled nursing facilities (SNFs), home health services, and rehabilitation facilities, complete a profile outlining the services they offer. Each day, the provider updates the bed or service availability.
At her hospital, Keane explains, there is a merged case management/social work department, with 19 registered nurse case managers, seven social workers, and one placement coordinator, who acts as a liaison between the post-acute facilities and the social workers. The hospital has about 460 patients at any one time, she notes, and her department arranges between 200 and 220 nursing home placements per month.
The case manager drives the discharge plan, she says, determining whether the patient should be placed in a facility or cared for at home, doing the initial intervention with the patient’s family, and performing the ongoing chart review. Once the discharge plan is ready and there is a solid placement need, the case manager makes a referral to the social worker, Keane says.
"The case manager continues to review the case, and as the patient becomes closer to discharge-ready,’ issues the PRI, entering it electronically into the computer," she says.
Meanwhile, Keane adds, the social worker has developed a relationship with the family, helping them understand the process and negotiating where the patient will receive post-hospital care.
When the patient is ready for discharge and the PRI is completed, the case manager transfers the PRI to the social worker, who completes the departmental screen of the patient and transfers the case to the placement coordinator with a list of appropriate facilities, Keane says.
"The placement coordinator electronically sends out queries to facilities the patient and family have chosen and awaits the follow-up. When she gets that, she transfers the information appropriately. If there is a medical need or question, it goes to the case manager, but if there is a financial or psychosocial need, it goes to the social worker."
Once the patient is accepted by the facility, she notes, the PRI is updated, if necessary, and the social worker proceeds with the transfer. If the patient came from a nursing home and is returning there, the process is driven by the case manager from start to finish, and there might not be a social worker involved, Keane adds.
To protect patient confidentiality, identifying information on the patient is sent to the provider only after the final match is made, she notes. "We can give [the provider] just a look at the PRI and whatever clinical information is necessary. We’re not giving them next of kin until we’re ready to give them next of kin, and we’re not using fax lines that may not be secure."
The eDischarge system "eliminates the back and forth," Keane points out. "Otherwise, people are going back and forth, faxing within the building, going up and down [floors] all day. We’ve decreased the unnecessary steps."
A clerical employee, for example, used to spend five hours collecting data and typing and distributing a monthly report showing where patients have been placed, she says. "The system does it in a minute, and we run a great report at the end of the business day."
Her staff can look at data showing where a patient was placed, how many facilities were sent applications, and what facilities have taken what types of patients in the past, Keane adds.
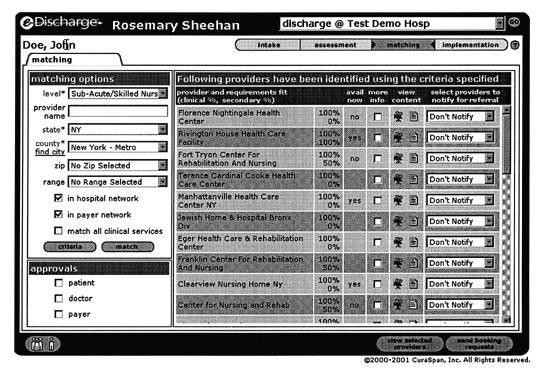
Using the criteria match, which is part of eDischarge, case managers sometimes are able to find an appropriate placement for patients they didn’t think a facility could accommodate, she points out.
"We’d look at the criteria match and say, Oh, we didn’t know they did dialysis,’ so it was a heads-up that a facility we didn’t think about would take a patient." Placing patients who need dialysis is particularly difficult because of limited resources in the area, Keane adds.
Placement of people with "extreme needs," such as a recent 540-pound patient, also is facilitated by the on-line system, she says. "We can query [regarding] specific patients who have specific needs to see if a facility we don’t use very often can provide that service.
"You know the facilities in your area that you use all the time," Keane adds, "but occasionally a facility is changing its scope of practice or opening a new unit. It’s right there on the computer." Meeting a special language or dietary need, for example, is particularly crucial with long-term placements, she notes.
Communication with payers is enhanced, Keane says, in that her staff can take a list of all the facilities within a certain plan and electronically transfer the PRI and other information in real time. "We don’t have to find a fax machine and fax to five different facilities. We can make one phone call to a managed care company and say, This patient has been medically approved by one of your preferred providers. Can I get an authorization number?’"
At present, Keane says, most of the post-acute facilities to which her hospital historically has made referrals are part of the eDischarge system.
"Some smaller facilities that service another community more than ours, or are borderline, have not joined, but it has not remotely been an issue," she adds. "If they didn’t get on board in the beginning, I think most of those we do business with will join."
Similar products her hospital tried several years ago "didn’t pan out," Keane says. "I don’t think they were clinically as good. With one, we tried making referrals without enough information — we couldn’t scan in enough to give the full package. Also, there was not a tremendous buy-in. [Participants] were not as computer savvy. There’s been a lot of change in our environment that made this the right time."
What Keane likes about eDischarge, she notes, is that it is "very comprehensive and very user-friendly, and it’s done at the front line. The case manager controls the discharge."
In addition, she says, the vendor provided a tremendous amount of support during implementation. "None of the other programs had the technical support this one has, or the time [the vendor] spent training and retraining."
What the vendor did make clear, Keane points out, is that the on-line discharge system by necessity must "change the way you do business. You have to set a limit [on telephone calls], squelch that knee-jerk impulse to use the phone."
And, she adds, "it takes getting used to seeing the PRI in the computer instead of in front of you — even though you can print it if you want to."
Although cases already are being turned around and decisions being made more quickly, Keane says she expects further improvements as staff get more comfortable with the system. "We’ve created our own security measures, but as time goes by we’ll drop some of the unnecessary [backup] steps and will get faster."
"Any time there’s a change," she adds, "there’s always a little holding on to the past, but the future is where you need to be."
[For more information, contact:
- Caroline Keane, New York Hospital of Queens, 5645 Main St., Flushing, NY 11355. Telephone: (718) 670-1300.
- Jackie Birmingham, Managing Director, Professional Services, Curaspan Inc., 368 Hillside Ave., Needham, MA 02494. Telephone: (781) 433-9800. E-mail: [email protected].]
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
