Target those most at risk of falls, but others too
Target those most at risk of falls, but others too
Fall prevention efforts usually target those thought most likely to fall, but does that leave the other patients at risk if no one is paying attention to their potential for falling? A special focus on high risk patients doesn't have to shortchange others, says Pamela E. Toto, PhD, OTR/L, BCG, FAOTA, an occupational therapist at the School of Health and Rehabilitation Sciences at the University of Pittsburgh in Pennsylvania.
Beginning Oct. 1, 2012, ambulatory surgery centers (ASCs) will be required to submit data on five quality measures to avoid a payment adjustment in 2014. They are patient fall; patient burn; wrong site, side, patient, procedure, or implant; hospital admission/transfer; and prophylactic IV antibiotic timing. The Centers for Medicare and Medicaid Services (CMS) has the statutory authority to apply a 2% penalty on ASC payments.
The highest risk patients should always get more attention to prevent falls, even when everyone else is still at risk to some degree, Toto says. (For information on those who are at most risk for falling, see "Study Identifies Patients at Risk for In-Hospital Falls," Same-Day Surgery Weekly Alert, Dec, 8, 2011. To sign up for this free weekly ezine, go to www.reliasmedia.com. In the left column, at the bottom, select "Free Alerts.")
"If you look at the literature, I could make the argument that the majority of people in the hospital are at risk for falls," Toto says. "I could go to a nursing home and tell you that 100% of the patients are at risk for falls. But you can make them into high, medium, and low risks relative to that particular population, and that can still be useful in directing your efforts."
The extra attention to high-risk patients is justified by the data that identifies risk factors, Toto says. That focused attention doesn't mean that other patients don't need the basic fall prevention efforts that can apply to anyone, such as keeping the room free of clutter and providing grab bars, she says. "We know, however, that certain patients at risk in certain ways or in certain conditions. If we know that a patient has urge incontinence, she is going to be in a hurry when she gets up, and that situation puts her at risk more than a patient without that condition," Toto says. "It's appropriate to provide more assistance and more education about that scenario even if you don't address that with everyone."
Healthcare providers are using increased knowledge about the risk factors for falls to prevent accidents in more practical and patient-friendly ways, Toto says. Rather than trying to keep patients in bed to avoid falls, the traditional approach, more hospitals are providing assistance to patients when they want to get up.
"It's not about limiting their ability to move, but rather providing them a safer way to move," Toto says.
Sources
• Pamela E. Toto, PhD, OTR/L, BCG, FAOTA, Department of Occupational Therapy, School of Health and Rehabilitation Sciences, University of Pittsburgh (PA). Telephone: (412) 383-6612. E-mail: [email protected].
Volunteer program cuts falls 46% Some of the best ways to prevent falls require personal, hands-on attention to individual patients, but hospitals don't have enough staff to provide as much of that tending as they would like. One hospital has found that volunteers are eager to do the job, and it has cut falls by a whopping 46% as a result. Overall compliance with fall-prevention protocol has improved significantly since the initiation of the program in April 2008, says Christine Waszynski, APRN, a geriatric nurse practitioner and clinical nurse specialist in the geriatrics program at Hartford (CT) Hospital. The volunteer program, which costs the hospital virtually nothing, started out with only two volunteers from a local job corps academy and has grown to 16 volunteers. Volunteers are particularly well suited to ensuring compliance with fall prevention protocols, Waszynski says. Many of the volunteers are teens who can be shy about interacting with patients in a way that requires them to strike up a conversation, but Hartford's Fall Prevention-Safety Monitor Volunteer Program provides them a specific set of factors to check with each patient. (For a video showing how the program works, go to http://vimeo.com/user7284985/videos and choose the video titled Safety Volunteer Program at Hartford Hospital. For more on the results of the program and tips for replicating it, see the stories, below.) The program was developed to monitor and increase staff compliance with fall-prevention protocol measures, reduce patient falls, and increase involvement of patient and family in creating and maintaining a safe environment, Waszynski says. Volunteers are recruited and trained specifically for the program after completing the standard mandatory volunteer orientation. "We teach them to look for measures that should be in place for patients who are at risk for falls, and they correct any oversights they might find," Waszynski says. "They also remind patients and families about the risk of falling and their role in fall prevention." The volunteers visit all patients who have been designated as a fall risk, which can include up to 80% of patients on some units. On each visit, the volunteer introduces himself or herself to the patient and family, and the volunteer explains that the purpose of the visit is to help reduce falls and keep the patient safe. Using the hospital's fall safety screening tool, the volunteer confirms that the patient is at risk and then checks to see that all aspects of the fall prevention protocol are being followed. [A copy of that screening tool is included. For assistance, contact customer service at [email protected] or (800) 688-2421.] That includes verifying that the patient is wearing the hospital's green fall risk bracelet, there is a green triangle on the door, and the bed or chair alarm is activated. The volunteer also scans the room for fall hazards and improves safety however necessary, such as moving the phone to within the patient's reach, removing clutter, and making sure the patient knows how to call for assistance. Each bedside check is recorded by the volunteer. At the end of the volunteer's shift, the results are reviewed with the unit's nurse manager or charge nurse. The findings also are sent to the fall-prevention team coordinator, who compiles the results for each unit monthly and presents them as a graph depicting compliance over time. "We've used this program to help us change culture. When we started this program, the culture was 'patients fall, and there's nothing we can do about it,'" Waszynski says. "Our compliance with fall prevention was 50% at best. By talking about this all the time and using our volunteers, now our compliance is about 90%." Source
|
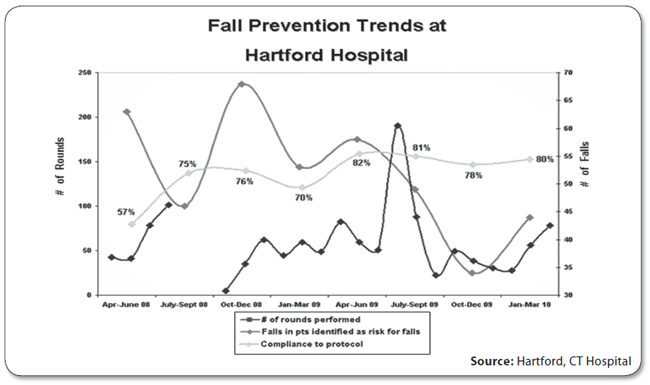
More rounding means better fall compliance Two years of the Fall Prevention — Safety Monitor Volunteer Program at Hartford (CT) Hospital has yielded significant results, says Christine Waszynski, APRN, a geriatric nurse practitioner and clinical nurse specialist in the geriatrics program. (See the charts, below.) In addition to reducing falls 46%, analysis of the bed check results shows these findings:
|

Clinical champion is a must for falls program Who wouldn't want to replicate a falls prevention program that cuts falls 46%? If you want the same results, here are some tips from Christine Waszynski, APRN, a geriatric nurse practitioner and clinical nurse specialist in the geriatrics program who works with the Fall Prevention-Safety Monitor Volunteer Program at Hartford (CT) Hospital: • You must have a clinical champion. The program can't be run solely out of volunteer services. A clinical professional from the fall prevention team needs to work closely with the volunteer coordinator to train the volunteers, monitor their work, and make good use of the data they collect. • Give the volunteers concrete, specific instructions. Don't educate them about fall prevention and then tell them to visit patients to look for fall hazards. Provide a checklist with precise items to inspect, correct, and talk to the patient about. The volunteers will be much more comfortable with their roles and more effective. • Involve the nursing department. Part of the program involves providing feedback to the nursing staff and holding staff accountable for deficiencies found by the volunteers. To ensure that the volunteer program is seen as an aid to the nursing staff rather than anything punitive, the nursing department needs to be on board from the start. |
Fall prevention efforts usually target those thought most likely to fall, but does that leave the other patients at risk if no one is paying attention to their potential for falling?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
