Trauma in Older Adults: An Overview of Injury Patterns and Management
Trauma in Older Adults: An Overview of Injury Patterns and Management
Authors:
Ademola Adewale, MD, FAAEM, Assistant Program Director and Assistant Clinical Professor of Emergency Medicine, Florida Hospital EM Residency, Orlando, FL.
Megan Leonard, MD, Resident, Florida Hospital EM Residency, Orlando, FL.
Peer Reviewer:
Steven M. Winograd, MD, St. Barnabus Hospital, Core Faculty, Emergency Medicine Residency Program, Albert Einstein Medical School, Bronx, New York.
Introduction
As the baby boomers become older adults, we will see a rapid rise not only in the older population, but also an increase in older patients. While older adults accounted for 13% of the population in the year 2000, by 2030 they will be at least 20% of the population, or almost 71 million.1-3 Older adults account for only 15% of trauma victims; however, the risk of death after trauma is significantly increased in patients older than 65 years of age, and for those over the age of 80 it is approximately four-fold that of younger patients.4
The effect of age as a predictor of mortality in older adult trauma can be difficult to assess from published literature. There is no uniformity in the definition of geriatrics in these papers. In this paper, the definition of older adult will be those over the age of 65. However, in the literature, the definition extends from 55 years to 80 years of age, making it difficult to collate the available data. In addition, many of the studies of trauma in older adults were published decades ago. In a study in 1990, age was an independent predictor of mortality.5
The Physiology of Aging
When compared to younger patients, older adults have a higher likelihood of having underlying medical conditions that may affect their ability to respond to injury or that may be the inciting cause of the initial injury. Decreased vision and hearing may increase the risk of car accidents, while compromised coordination and balance increase the risk of falls. Impaired sensation, proprioception, and dementia can lead to decreased reaction times in older individuals. Prescribed medications and supplements can alter mentation causing sedation. Drugs utilized for anticoagulation increase the risk of bleeding from falls or a minor motor vehicle collision.
Cardiovascular System
The structural and physiologic changes that occur with aging include a stiffening of the heart, an increase in left ventricular wall thickness, a decrease in the number of myocardial cells, and an increase in collagen levels. These changes cause a decrease in stroke volume and cardiac output.6,7 Fibrosis of the conducting system of the heart decreases the ability to increase the heart rate. Cardiac reserve decreases by 1% every year after the age of 30.8,9 Older adults are likely to respond to hypovolemia with increased systemic vascular resistance and are less responsive to increased catecholamine stimulation from shock, limiting their ability to respond to hypovolemia.
The cardiovascular system may require more time to mount a tachycardic response to sudden stress. Hence, the initial vital signs could be misleading. Medications such as beta-blockers, calcium channel blockers, and digoxin may inhibit a tachycardic response, while after-load reducers and diuretics limit preload. Coronary artery disease can increase the risk of myocardial infarction secondary to hypotension.1
The vascular system ages in a similar manner to the heart, causing decreased compliance and increased fragility, which makes older patients more susceptible to dissection or aneurysm formation.6
Pulmonary System
The pulmonary system also undergoes many changes with aging. Arthritic changes in the rib cage articulations or osteoporosis of the thoracic spine can impair the compliance of the respiratory system. This reduction in resilience can restrict ventilation, resulting in an increase in the work of breathing.10
With aging, vital lung capacity and forced vital capacity decrease, while dead space ventilation, functional residual capacity, and residual volume increase.10,11 As a result, arterial partial pressure of oxygen (PaO2) may fall. There is a significant decrease in the protective mechanism of the respiratory system. The mucociliary apparatus activities and those of the mucosal phagocytes become less effective. Consequently, older adults are predisposed to respiratory infections especially in the presence of pulmonary trauma. Taken together, older adults are more likely to need ventilation assistance, such as CPAP or BiPAP, or intubation in the presence of pulmonary trauma, such as multiple rib fractures or pulmonary contusion. These changes also make ventilator weaning more difficult.12
Musculoskeletal System
Loss of muscle mass and concomitant reduction in muscle strength leads to increased frailty and the risk of fractures. With aging, muscle is replaced by fat and fibrous tissue and, as a consequence, by age 75, only 15% of the total body mass is muscle, compared to 30% in younger, healthy adults.13,14 Bone density decreases at the rate of 0.5% per year after bone mass peaks between ages 30 and 35 years.15
Osteoarthritis, osteoporosis, and osteopenia predispose older adults to fractures from seemingly minor trauma. A simple fall alone can cause spinal compression fractures, wrist, pelvic, hip, and skull fractures. In 2005 in the United States, there were more than 2 million fractures from osteoporosis, at an estimated cost of $17 billion.16 Fractures often require surgical correction, exposing patients to postoperative complications, such as deep venous thrombosis from prolonged immobilization, and infections.
Central Nervous System
Aging leads to decreased muscle strength, reduced deep tendon reflexes, decreased sensation of touch, pain, and vibration, and reduced nerve conduction velocity, which consequently results in slowed coordinated movements and decreased response time to stimuli.17 As a result of these changes, older adults can have an overall slowing of motor skills, and difficulty with balance, gait, coordination, reaction times, and agility.18
Mechanisms of Trauma
Motor vehicle accidents, falls, and burns make up more than 80% of accidental trauma in older adults. Approximately 40% of people older than 65 years report at least one fall per year, which increases to 50% in those older than 80 years. In long-term care facilities, the risk of falls increases to more than 50-60% per year.19-21 Falls occur equally between men and women, but more injuries occur in women. Risk factors include past history of falls, anemia, lower extremity weakness, female gender, balance problems, cognitive impairment, psychotropic drug use, arthritis, stroke, orthostatic hypotension or vasomotor insufficiency, and dizziness.22-28 The greater the height of the fall, the more likely the older adult patient will have a major injury, but significant injury may occur even from the height of standing. The mortality rate for elderly patients who fall is 12%, and 50% may die within a year of the fall.29
Motor vehicle accidents are the second most prevalent cause of trauma in older adults, accounting for 20-60% of trauma cases in the elderly.30,31 Even though statistics have shown that older drivers tend to drive at slower speeds, make shorter trips, and avoid driving at night or in bad weather, the consequences of motor vehicle collisions in this group are more severe than in younger patients.32 Most crashes are located at intersections while undertaking a left-hand turn in the daytime. A single-vehicle crash should raise suspicions for a medical cause, such as hypoglycemia, stroke, seizure, or myocardial infarction. Older drivers are more likely to be hospitalized or killed when compared to younger drivers, even if they were wearing a seatbelt. Slower reaction time, decreased auditory and visual acuity, and cognitive impairment put this population at higher risk for accidents.
Overall, the fatality rate among older adults involved in motor vehicle collisions approaches 21%.30
The third most common cause of injury in older adults is a pedestrian struck by a motor vehicle. Older adults account for about 22% of pedestrian fatalities, but the fatality rate is double that of younger adults. The predisposing factors to this injury mechanism include decreased peripheral vision, hearing, cognitive, memory, and judgment skills.
Older adults account for 13-20% of burn admissions. Predisposing physiologic changes include thinning of the skin, decreased subcutaneous tissue, and diminution of the immune system. More than 90% of burns occur in the home. Flame burns make up 50% of these injuries and occur most commonly during cooking. The overall mortality rate is about 30%.33,34
While older Americans comprise approximately 13% of the population, they account for 18% of all suicide deaths.35 The risk factors for suicide in this population could be easily overlooked. A paper published by Garand L et al35 summarized suicide risk factors under four broad headings: demographic characteristics (older age, male gender, Caucasian race, and unmarried conjugal status); mental health (major depression, primary psychotic illnesses, personality disorders, and alcohol or substance abuse); physical health (chronic debilitating disease, frailty, and global decreased health status causing functional impairment); and social isolation.
Older male patients are more likely to make successful suicide attempts.36 Older adults are less likely to inform family or friends that they are contemplating suicide, and they tend to have better planning and strategy to ensure successful completion.
Elder neglect and abuse is also a cause of trauma. It is thought that nearly 85% of elder abuse cases are not reported.37 Financial pressures, family stress, and decreased emphasis on traditional family roles play significant roles in this type of abuse. Delay in seeking medical attention, an inconsistent history of the event, or unexplained injuries are warning signs for elder abuse. When possible, interview the patient separately from the caregivers to obtain the patient's own account of the event.
Head Injuries
Head injuries are a major cause of death from falls in older adults. Epidural hematomas are rare due to the tight adherence of the dura to the skull; cerebral contusions and subdural hematomas are more likely to occur. Contusions occur in up to 30% of head-injured patients. Cerebral atrophy allows the brain to move more freely within the skull and the fragile bridging veins are stretched. Head trauma can rupture of these veins, resulting in a subdural hematoma, which occurs in up to 70% of older adult patients with mild to severe head trauma.38
Figure 1: Subdural Hematoma
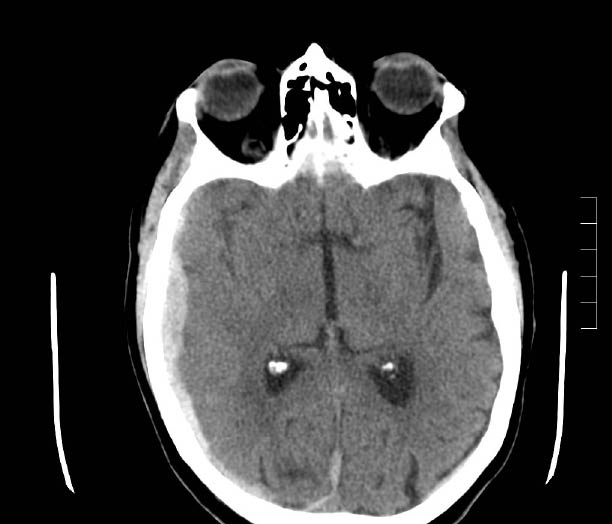
CT-san of a subdural hematoma on a 79-year-old female taking Coumadin for atrial fibrillation who fell and struck her head on a counter.
Acute subdural hematoma (SDH) is seen as a crescent-shaped hyperdense mass on CT scan (see Figure 1), but it becomes less dense with time. Chronic hematomas may become hypodense two weeks after injury. This injury is unlikely to produce an early elevation in intracranial pressures; however, worsening mental status changes portend an ominous outcome. Physicians should maintain a low threshold for obtaining head CT scan in this population because a seemingly minor fall with contusion to the nasal bridge or forehead may be a harbinger of an underlying subdural hematoma or intracranial injury. Patients with signs of neurologic dysfunction should receive a neurosurgical consultation for possible clot evacuation.
Mortality from head injury in older adults is about four times that of the younger population, and risk factors such as the use of anticoagulants undeniably play a role.39 A study by Rozelle CJ et al looked at 157 patients age 65 years and older. Strong predictors of in-hospital mortality included a Glasgow coma scale less than 7, age greater that 80 years, acute duration of hematoma, and the need for craniotomy.40 Rakier A et al evaluated 263 older with head injury. They reported a mortality rate of 33% for subdural hematoma and 28% for cerebral contusion. All patients with epidural hematoma had a poor outcome.41
From the above referenced studies, it is evident that there is an increase in mortality from subdural hematoma. Even with minor head trauma, an older patient may require home health nursing or placement in a skilled facility until full function is recovered.42
Spinal Injuries
Falls are the most common mechanism of spinal injury. Cervical spine injury accounts for almost 70% of fractures that result from falls, and the overall mortality from this injury is 14% in older adults. This is three times higher than for the younger patient population.43 Type 2 odontoid fractures are the most prevalent spinal injury in older adults. Fractures are not necessary for a cord injury to be present. Hyperextension injuries may result in cord contusions and development of central cord syndrome, which often manifests as greater upper extremity weakness with sensory loss than lower extremity findings.
The Canadian C-spine rule states that age greater than 65 years is a criterion for mandatory radiography in patients with an appropriate trauma mechanism or who have neck pain after trauma. Although the type of radiography is not specified, underlying osteoarthritis and degenerative changes can make the plain films of the cervical spine difficult to interpret, with the potential to miss an occult fracture. Consequently, a cervical CT scan may be warranted when injuries are suspected.44-47
The NEXUS study noted older adults have a relative risk of 2.09 (95% CI 1.77-2.59) for cervical spine injury, which was the highest relative risk of all demographic groups in their study.48 Touger et al studied Nexus criteria in 2943 older adults. In their population, cervical spine injury was twice as common, and odontoid fracture (see Figure 2) accounted for about 20%. Even older adults without midline tenderness may have a significant cervical fracture.49
Figure 2: Odontoid Fracture
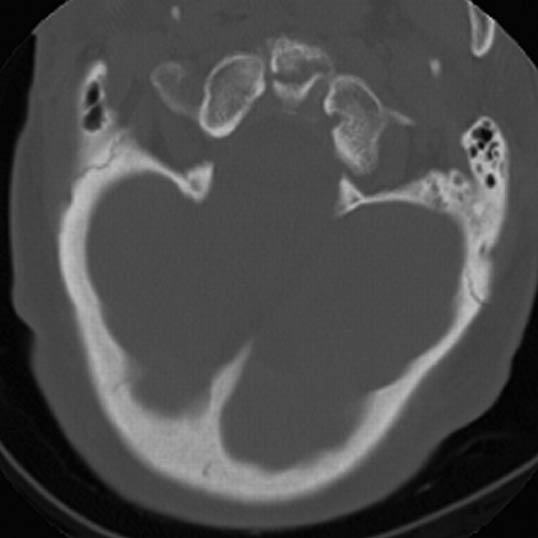
Odontoid fracture seen in a 67-year-old male who fell from standing.
Osteoporosis, osteoarthritis, and osteopenia are risk factors for thoracic and lumbar vertebrae fractures. (See Figure 3.) Presently in the United States, the lifetime risk for osteoporotic vertebrae fracture is 40% in white women and 13% in white men.50 The incidence of osteoporotic fractures increases with age. With age-related modeling, bones are weaker and stiffer, with decreased mobility and flexibility. The forces generated on impact from falls or motor vehicle-related trauma can lead to vertical compression or wedge-shaped fractures. (See Figure 4.)
Figure 3: Multiple Thoracic Spine Fractures
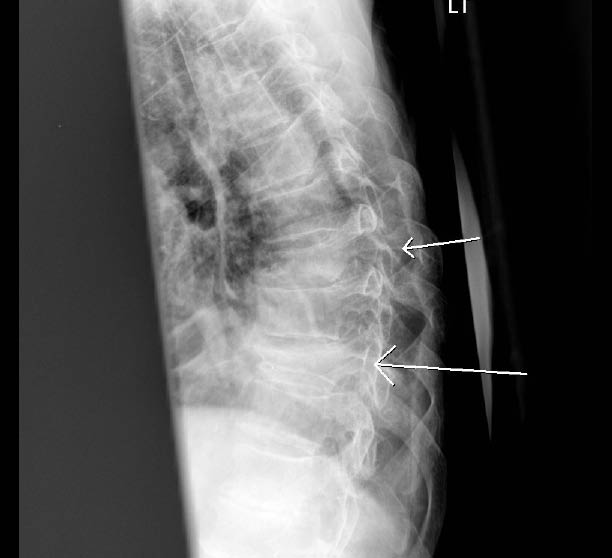
76-year-old female with multiple thoracic spine fractures after MVC
Figure 4: L1 Compression Fracture
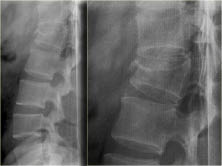
Image of an L1 compression fracture from MVC
Older adults with spinal fractures present with back pain or worsening of chronic back pain. The physical examination should include palpating for midline spinal tenderness or step off, as well as an appropriate neurologic examination. Since the quality of life is diminished and loss of function is increased in patients with vertebral fractures, it is important to obtain imaging when an older adult presents to the ED with significant acute back pain after a fall or motor vehicle accident.
Depending on the type of fracture and severity, pharmacologic therapy, rehabilitation, a thoracolumbar support brace, nerve blocks, and surgical intervention such as vertebroplasty or kyphoplasty may be indicated. Spinal cord injuries with these fractures are rare, but pain may be significant enough to necessitate admission. If leg weakness is present or bowel and bladder function are compromised, surgical intervention may be indicated for spinal canal decompression.
Chest Injuries
Chest trauma accounts for almost 10-15% of all trauma and is the cause of death in 25% of all fatalities due to trauma.51 Approximately 70% of traumatic chest injuries are blunt injuries.51 The most common chest injuries in this population are rib fractures (23.5%), flail chest (9.5%), and sternum fracture (5.9%).51 The majority of these injuries occur as a result of motor vehicle collisions. The presence of osteoporosis and degenerative joint disease makes the chest wall more rigid and fragile in older adults than in younger patients. Minor motor vehicle collisions may cause rib or sternal fractures with subsequent pulmonary contusions or hemothorax or pneumothorax. (See Figure 5.) Older adults have a higher rate of chest injuries from a motor vehicle accident than do younger adults (23.4% vs 18.1%).52
Figure 5: Multiple Rib Fractures and Hemothorax
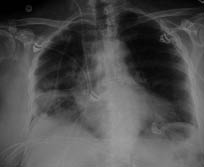
Image of a 73 year old female who fell, struck her right torso on the edge of a cabinet. She sustained multiple rib fractures with hemothorax requiring a chest tube and intensive care admission
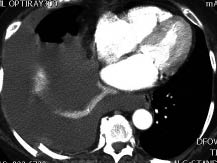
Rib fractures are the most common chest injury in older adults, and carry significant morbidity. Ribs tend to fracture at the site of impact or at the posterior angle where the rib structure is the weakest. Ribs four through nine are the most commonly fractured. Fractures involving first and second ribs should raise the suspicion of a potential great vessel injury, while fractures of ribs nine through 11 are associated with splenic or liver injury.53 Morbidity and mortality increase with the number of rib fractures. For each additional rib fracture, mortality increases by 19%.54
Poor pulmonary reserves in this population predispose them to infections and early decompensation. Hence, older adults with multiple rib fractures should receive early, aggressive pain management with regional nerve blockade, epidural analgesia, or intravenous analgesia.
Opioid analgesia is often poorly tolerated. When available, epidural analgesia may provide better and safer pain control.55 Regional anesthesia can also improve ventilation and pulmonary toilet. A study comparing epidural analgesia to parenteral anesthesia in older adults demonstrated a mortality decrease (from 16% to 4%), and reduction in pneumonia (from 19% to 8%) and ARDS (from 14% to 6%).
Fractures of the sternum are generally the result of striking the steering wheel in a motor vehicle collision. These fractures are usually non-displaced, but may subluxate, causing injury to underlying heart, pulmonary parenchyma, and great vessels.56 A sternal fracture in older adults warrants further evaluation for potential concomitant intrathoracic injury or myocardial contusion.57 Figure 6 is of a 77-year-old male driver whose car was struck head-on at an intersection and who presented to the ED with a complaint of chest pain. The physical exam revealed bruising to the anterior chest with sternal tenderness. The patient was placed on a monitor, and the rhythm strip showed multifocal premature ventricular escape beats. His chest radiograph revealed a sternal fracture and his cardiac troponin was positive. The patient was admitted for suspected myocardial contusion from the depression from the sternal fracture.
Figure 6: Sternal Fracture and Myocardial Contusion
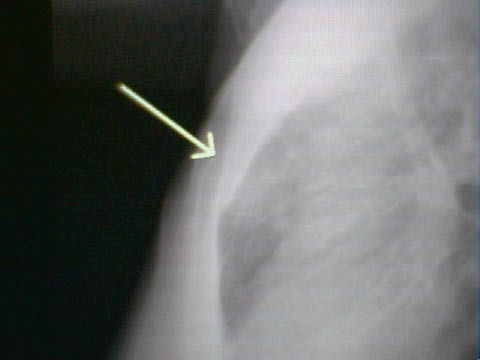
Radiograph of a 77-year-old male involved in a low speed MVC with sternal fracture and myocardial contusion
Rapid and sudden deceleration in motor vehicle collisions can cause tracheal, cardiac, and great vessel injury.58 Dyspnea, a hoarse voice, subcutaneous emphysema, or hemoptysis on initial presentation should prompt the consideration for injury to the trachea and bronchial system. A persistent air leak after chest tube placement is another important sign that a bronchial injury is present.
Figure 7: Aortic Dissection
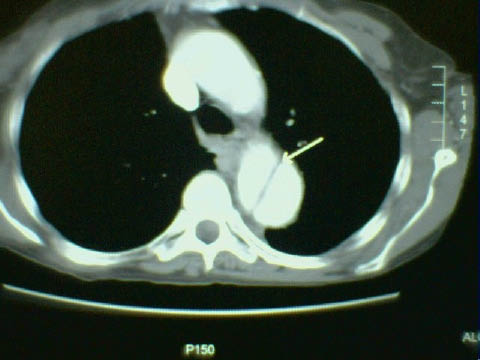
CT-scan of aortic dissection in a 81 year-old female involved in a low speed MVC rear ended at a stop sign
Traumatic aortic dissection is a rare but life-threatening injury associated with motor vehicle collisions, including motorcycles and falls from height. (See Figure 7.) The ascending aorta is relatively mobile, so during deceleration, it is still freely moving while the descending aorta is held in place. Rapid deceleration causes shearing forces on the aorta just distal to the left subclavian artery, where the ligamentum arteriosum and intercostal arteries tether the descending aorta. Alternatively, a burst of high intraluminal pressure within the aorta after a high-speed vehicle collision, the so-called "water hammer" effect, can lead to tears or the pinching of the aorta between the vertebral column and sternum.59-61 Older adults with atherosclerotic disease are at higher risk for these injuries. Tears usually involve the two inner layers of the aorta, the intima and muscularis, with the resultant leakage of blood pooling within the adventitia, forming a false lumen. Complete aortic rupture results in immediate death by exsanguination.62,63
The initial symptoms of an aortic tear include chest pain, back pain, and dyspnea. Patients may have persistent tachycardia and chest wall ecchymosis, or abrasions to the chest wall. Some patients may have a difference in blood pressures taken in the upper extremities compared to the lower extremities. 64 A harsh murmur may also be heard over the anterior chest or back at the site of the aortic disruption and has been reported in approximately 26% of cases.65 However 30% of patients may not have any external signs of injury.66
The management of aortic tears differs depending on the exact location of the tear. Ascending aortic tears generally are taken emergently to the operating room, while tears in the descending aorta can at times be managed medically with blood pressure and pain control.
Injury to the diaphragm is generally the result of blunt trauma. The left hemidiaphragm is injured in 60-90% of cases since the right is protected by the liver.67 The signs and symptoms depend on how much abdominal viscera herniates into the chest cavity. Symptoms may include cough, dyspnea, the sensation of peristalsis in the chest cavity, and non-specific chest or abdominal pain that radiates to the shoulder. Signs of diaphragm injury may manifest as a non-mobile left hemithorax, tympany to percussion in the chest, and decreased breath sounds. Because herniation of abdominal contents may mimic a pneumothorax, when possible obtain a chest X-ray prior to chest tube insertion after blunt trauma.
Esophageal injuries are quite rare, but can occur when blunt force occurs to the upper abdomen into the esophagus, causing perforation. The esophagus is most likely to perforate on the left distal side because this area lacks muscular fibers. Motor vehicle crashes are the most likely cause of this type of injury; the seatbelt compresses into the patient's abdomen during rapid deceleration. Patients present with subcutaneous emphysema in the supraclavicular fossa, dyspnea, dysphagia, pneumo-mediastinum, left-sided pleural effusion, and/or hematemesis.
Abdominal Injuries
Abdominal injuries after trauma are found in 30% of older trauma patients. Solid organs such as the spleen, liver, and kidneys are more commonly involved and associated with lower rib fractures. Patients with lower rib fractures have a 10.7% incidence of liver injury and 11.3% incidence of spleen injury.68
Figure 8: Motorcycle Injuries
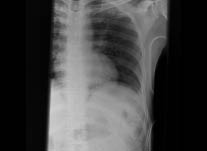
Images of a 68 year old male that fell off his motorcycle at a low speed
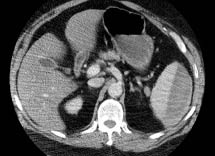
Figure 8 shows images of a 68-year-old male who presented to the emergency department after a fall from his motorcycle at a low speed. On presentation, he was tachycardic, with some splinting and noticeable bruising of his left lower ribs. The chest radiograph shows multiple lower rib fractures, and a CT-scan demonstrates a splenic hematoma.
Older patients have a five-fold increase in mortality from abdominal trauma when compared to the younger population.69 Physical examination is often unreliable; unexplained hypotension may be the only initial finding.1 CT scans often demonstrate surprising injuries in seemingly stable older adults. Embarking on aggressive management can minimize preventable morbidity and even mortality.
Musculoskeletal Injuries
The musculoskeletal system is the most commonly injured organ system during older adult trauma. Trabecular bone thins and weakens with age, making fractures more likely in the elderly, even with simple falls from the height of standing. Pathologic conditions such as Paget disease, osteomalacia, metabolic derangements, malignancy, marrow dysplasia, and infection also predispose these patients to fractures.70
Figure 9: Ulnar Styloid Fracture
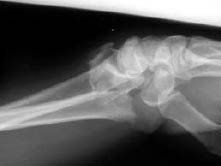
Image of a 74-year-old with fall on an outstretched arm with distal radius and ulnar styloid fracture
Overall, falls on outstretched hand (FOOSH) is the most common mechanism of injury of the upper extremity. Distal radius fractures are the most common fractures in the older adults, making up 50% of all fractures of the upper extremity (see Figure 9), followed by proximal humerus at 30%, with elbow dislocations and radial head fractures making up a combined 15%.71,72 Since more than 50% of people older than 70 years of age already have degenerative rotator cuff tears, this underlying condition can be worsened after falls and should be suspected if the patient is unable to move the shoulder despite negative bony abnormalities on radiographic studies.
Distal radius fractures can often be managed in the emergency department with reduction and immobilization, and orthopedic follow-up for casting or surgical repair. At present, there is no level-1 clinical evidence suggesting a superior modality for treatment of distal radius fracture.
Surgical management is often indicated in the presence of: post-reduction radial shortening of greater than 3 mm, dorsal tilt greater than 10 degrees, or intra-articular displacement or step off greater than 2 mm.73
Figure 10: FOOSH Injury
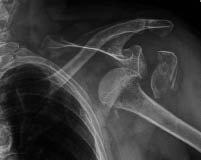
Left shoulder radiograph of a 68 year old female that fell on an outstretched arm. Image shows a fracture dislocation of the tuberosity and proximal humerus neck.
Fractures of the humerus are most often caused by direct trauma to the arm or shoulder, or via axial loading from FOOSH. (See Figure 10.) Proximal humerus fracture is more common in the older adult population and it is the third most common fracture after hip and distal radius fractures in this popuation.74 Fractures to the proximal humerus rarely involve nerve injury; however, there is the potential for rotator cuff involvement in older adults.
Radiographic evaluation for possible proximal humerus fracture should include an anterior-posterior view of the scapula and glenohumeral joint, an axillary view, and a lateral scapula Y view. When the fracture cannot easily be defined on X-ray imaging, a CT scan is a valuable adjunct.
The initial ED management includes an evaluation of neurovascular status, pain control, sling and swathe, with orthopedic consultation. Although proximal humerus fractures are not life-threatening, they may severely limit the activities of daily living for an older adult. Patients may require home health or extensive rehabilitation services. Surgery may be the option for some more active elderly patients, but in general, patients are treated with immobilization followed by physical therapy.
Fractures to the pelvis carry a high morbidity and mortality. Lateral compression fractures are more common and have the propensity for causing significant blood loss.74 Though rare, open fractures carry the worst prognosis. Unstable pelvic fractures due to motor vehicle collisions carry a high mortality rate of up to 80%.75,76 Falls on a level surface may cause pubic rami fractures that are stable; however, pain control and gait training often require these patients to be hospitalized. Whenever there is a pelvic fracture, there must be increased suspicion for concomitant intra-abdominal injury and the potential for blood loss, especially in a hypotensive older adult patient. A study done by Levy et al reported that the mortality rate increases by 50% when a pelvic fracture is accompanied by hypotension, and the mortality rate approaches 90% if the fracture is open.77
Nondisplaced pelvic fractures may be difficult to see on plain films. CT or MRI of the pelvis should be considered when older patients have difficulty ambulating after trauma.
Hip fractures are the most common lower extremity fracture (see Figure 11) sustained in the elderly population. The incidence increases with age, rising from 22.5 and 23.9 per 100,000 population at age 50, to 630.2 and 1289.3 per 100,000 population by age 80 for men and women, respectively.78 Patients with a hip fracture have an early mortality rate of 5% that increases to 13-30% in the year following the fracture due to recurrent falls and complications.76
Figure 11: Intertrochanteric Fracture
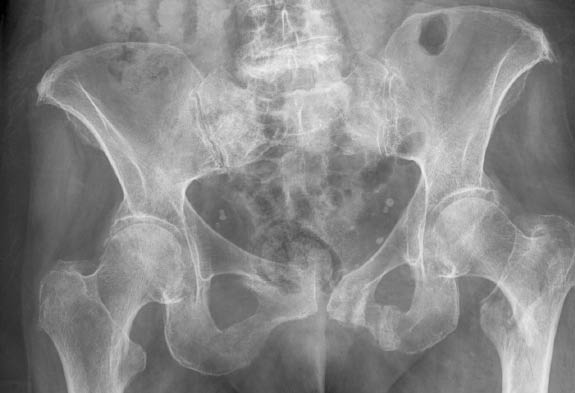
Radiograph showing left intertrochanteric fracture.
Patients with a fracture hip may have severe pain, or at times relatively little pain. They may also complain of knee pain, although on exam they will have pain with manipulation of the hip. The physical exam may reveal a shortened and externally rotated limb. X-rays are usually diagnostic, but CT or MRI may be needed to define subtle fractures.79
Pain management may be an issue in some patients. Opioids are not well-tolerated in older adults. Recently, ultrasound-guided regional anesthesia has been applied in the emergency department with near total analgesia. Surgery is required in nearly all cases of hip fracture, followed by rehabilitation.
Figure 12: Fracture Dislocation of the Ankle
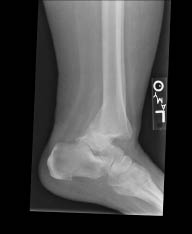
Image of fracture dislocation of the ankle
Ankle fracture (see Figure 12) is a common lower-extremity fractures in the older adult, occurring in about 4.2 per 1000 Medicare enrollees.80 The highest rate was seen in white women at 5.8, and lowest in nonwhite male at 1.5 per 1000 Medicare enrollees. Most ankle fractures in older adults are caused by falls on uneven pavement or down the stairs, with subsequent twisting of the ankle. Patients with signs of potential neurovascular compromise, such as paresis, pulselessness, and cold extremities, should have an urgent fracture reduction and subsequent immobilization.
Soft-Tissue Injury
With aging comes about a 20% loss in dermal thickness and a significant decrease in connective tissue integrity. This laxity in integrity decreases the tamponading effect of subcutaneous bleeding, which may lead to a significant amount of blood loss that can be easily overlooked. The loss of resiliency in the skin leads to tearing-type injuries. (See Figure 13.)
Figure 13: Simple Skin Tear
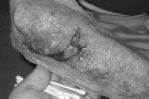
Management of these injuries could be a challenge, since they are often difficult to repair with sutures and may be prone to infection. The popularity of skin adhesives has made these injuries more amendable to repair, with good results.
Management of Elderly Trauma
The resuscitation of older adult trauma patients begins with the prehospital personnel. The initial triaging of these patients to trauma vs. non-trauma centers, depending of the perceived injury pattern, may contribute significantly to the morbidity or potential mortality of the victims. Several studies81,82 have shown that the very elderly are disproportionately triaged and cared for at non-trauma centers, and this is associated with increased mortality. A more recent study by Chang et al discovered that the risk of under-triage was higher (49% vs. 17.8%, p < 0.001) among those 65 years old or older.83
The older trauma patient should reassessed shortly after arrival by EMS, understanding the higher risk in this population. Blood pressure and heart rate responses to stress may be blunted because of hypertension, coronary artery disease, and the use of beta-blocker medication.
As with all injured patients, assessment begins with airway, breathing, circulation, and the remainder of the primary survey. Patients with hemodynamic instability require aggressive resuscitation. It can be challenging to aggressively fluid resuscitate patients with a history of congestive heart failure or renal failure, as well as those with hemodynamic instability. A pulmonary artery catheter can guide resuscitation of older adult trauma victims using the cardiac index of 4 L/min per square meter or oxygen consumption of 170 mL/min per square meter as an endpoint. Noninvasive Bioreactance monitoring has been used to provide similar hemodynamic information.
The base deficit assessed from a blood gas can be used to estimate the extent of shock and adequacy of resuscitation. In one study of patients 55 years and older, a base deficit of -6 to -9 carried a mortality of almost 60%, while a severe deficit of greater than -10 carried a mortality of almost 80%.84
Serum lactate has been shown to identify hypoperfusion early in older adult trauma patients, and its clearance directly correlates with mortality. Schulman et al85 found that a lactic acid level 22 mg/dL (> 2.4 mmol/L) for longer than 12 hours was associated with an increased mortality.
Older adults on oral anticoagulation who sustain blunt trauma and traumatic brain injury are particularly challenging. The mortality rate of trauma patients who receive anticoagulation therapy is up to four to five times that of normal subjects.55 Close observation and correction of coagulation status may be indicated depending on the injury sustained and the need for emergent surgical intervention. Reversal agents, such as vitamin K, fresh frozen plasma, cryoprecipitate, and, recently, recombinant coagulation factors and prothrombin complex concentrate, can be utilized.
Conclusion
Based on the projection for the aging population by the year 2030, there will likely be more older adults and, consequently, an increase in older trauma patients. Older adults are living a longer, active lifestyle, and the approach to care should optimize the outcome that allows for continuation of an active lifestyle. Although these patients can be challenging, almost 85% of survivors will eventually function independently at home. Understanding the physiology of aging, utilizing hemodynamic monitoring adjuncts (invasive or noninvasive) while incorporating necessary laboratory blood analysis and aggressive resuscitation to the endpoint will improve outcomes if started early both in trauma and non-trauma centers.
References
1. Geriatric trauma. In: Marx JA, Hockberger RS, Walls RM, et al, eds. Emergency Medicine: Concepts and Clinical Practice, 7th ed. Philadelphia: Mosby/Elsevier; 2010:281-85.
2. Trauma in the elderly. In: Wolfson AB, Harwood-Nuss AL, eds. Clinical Practice of Emergency Medicine, 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins, 2005: 1124-1128.
3. Larsen P. A review of cardiovascular changes in the older adult. Gerontology December 2008/January 2009:3.
4. Tornetta P, Mostafavi H, Riina J, et al. Morbidity and mortality in elderly trauma patients. J Trauma 1999;46:702.
5. Morris JAJ, MacKenzie EJ, Damiano AM, et al. Mortality in trauma patients: The interaction between host factors and severity. J Trauma 1990;30:1476-1482.
6. Davies M. Pathology of the Aging Heart. In: Brochlehurst SC, Talus RC, Dillit HM, eds Textbook of Geriatric Medicine and Gerontology. Edinburgh: Churchill Livingstone;1992: 181-185.
7. Johns Hopkins Medical Institutions. "Aging Heart Changes Shape, Shrinks And Loses Pumping Function Too." ScienceDaily 11/8/2007. Available at: http://www.sciencedaily.com/releases/2007/11/071104190622.htm. Accessed 10/10/2011.
8. Lakatta E. Determinants of cardiovascular performance: Modification due to aging. Chronic Dis 1983;36:15-30.
9. Schwartz JB, Zipes DP. Cardiovascular disease in the elderly. In: Libby P, Bonow RO, Mann DL, et al, eds. Heart Disease: A Textbook of Cardiovascular Medicine, 8th ed. Philadelphia, Pa; Saunders Elsevier; 2007.
10. Gulshan S, Goodwin J. Effects of aging on the respiratory system physiology and immunology. Clin Interv Aging 2006;1(3):253-260.
11. Tockamn M. Aging of the respiratory system. In: Principles of Geriatric Medicine and Gerontology. New York, McGraw-Hill; 1994:555.
12. Schriber A. Aging changes in the lungs. National Library of Medicine National Institutes of Health. Verimed Healthcare Network, 29 Nov. 2010. Web. 10 Oct. 2011.
13. Levelser RF, Delbono O. Aging of the muscles and joints. In: Hazzard WR, Blass JP, Halter JB, et al, eds. Principles of Geriatric Medicine and Gerontology. New York: McGraw-Hill; 2003: 905-918.
14. Levelser RF, Shakoor N. Aging or osteoarthritis: Which is the problem? Rheumatic Dis Clin North Am 2003;29:653-673.
15. US Department of Health and Human Services (2004). Bone health and osteoporosis: A report of the Surgeon General. Retrieved February 13, 2007, from http://www.Surgeongeneral.govllibrarylbonehealth.
16. Facts and Statistics about Osteoporosis and it's Impact. International Osteoporosis Foundation. Available at http://www.iofbonehealth.org/facts-and-statistics.html. 10 Oct 2011.
17. Matsumura BA, Ambrose AF. Balance in the elderly. Clinics in Geriatric Medicine 2006;22:395-412.
18. Pakkar A, Cummings JL. Mental status and neurologic examination in the elderly. In: HazzardWR, Blass JP, Halter JB, et al, eds. Principles of Geriatric Medicine and Gerontology. New York: McGraw-Hill; 2003: 111-119.
19. Thapa P, Brockman K, Gideon P, et al. Injurious fall in nonambulatory nursing home residents: A comparative study of circumstances, incidence, and risk factors. J Am Geriatric Society 1996;44:273.
20. Nevitt M, Cummings S, Hudes E. Risk factors for injurious falls: A prospective study. Journal of Gerontology 1991;46:164.
21. Tinetti M. Preventing falls in elderly persons living in the community. N Engl J Med 1988;319:1701.
22. Graafmans W, Ooms M, Hofstee H, et al. Falls in the elderly: A prospective study of risk factors and risk profiles. Am J Epidemiology 1996;143:1129.
23. Campbell A, Borrie M, Spears G. Risk factors for falls in a community-based prospective study of people 70 years and older. Journal of Gerontology 1989;44:112.
24. Nevitt M, Cummings S, Kidd S, et al. Risk factors for recurrent nonsyncopal falls. A prospective study. JAMA 1989;261:2663.
25. O'Loughlin J, Robitaille Y, Boivin J, et al. Incidence of and risk factors for falls and injurious falls among the community-dwelling elderly. Am J Epidemiol 1993; 137:342.
26. Bueno-Cavanillas A, et al. Risk factors in falls among the elderly according to extrinsic and intrinsic precipitating causes. Eur J Epidemiol 2000;16:849.
27. Penninx B, et al. Late-life anemia is associated with increased risk of recurrent falls. J Am Geriatr Soc 2005:53:2106.
28. Ganz D, Bao Y, Shekella P, et al. Will my patient fall? JAMA 2007;297:77.
29. Helling TS, et al. Low falls: An underappreciated mechanism of injury. J Trauma 1999;46:453.
30. Cook LJ, et al. Motor vehicle crash characteristics and medical outcomes among older drivers in Utah, 1992–1995. Ann Emerg Med 2000;35:585.
31. Bergen G, Chen LH, Warner M, et al Injury in the United States: 2007 Chartbook. Hyattsville, Md, National Center for Health Statistics, 2008.
32. Preusser D, et al. Fatal crash risk for older drivers at intersections. Accident Analysis and Prevention 1998;30:151-159.
33. Ryan C, et al. Objective estimates of the probability of death from burn injuries. N Engl J Med 1998;38:362.
34. Lumenta D, Hautier A, et al. Mortality and morbidity among elderly people with burns Evaluation of data on admission. Burns 2008;34:965.
35. Garand,L, Mitchell AM, Dietrick A, et al. Suicide in older adults:nursing assessment of suicide risk. Issues Ment Health Nurs 2006;27:355-370.
36. Conwell Y, Duberstein P, et al. Risk factors for suicide in later life. Society of Biologic Psychiatry 2002;52:193-204.
37. Levine J. Elderly neglect and abuse: A primer for primary care physicians. Geriatrics 2003;58:37-44.
38. Wolfson A, et al. Head injuries. In: Harwood-Nuss Clinical Practice of Emergency Medicine, 4th Ed. Lipincott Williams &Wilkins, 2005.
39. Susman M, DiRusso SM, Sullivan T, et al. Traumatic brain injury in the elderly: Increased mortality and worse functional outcome at discharge despite lower injury severity. J Trauma 2002;53:219.
40. Rozelle CJ, Wofford JL,Branch CL. Predictors of mortality in older patient with subdural hematoma. J Am Geriatr Soc 1995;43:240-244.
41. Rakier A, Guilburd JN, Soustiel JF, et al. Head injury in the elderly. Brain Inj 1995;9:187-193.
42. Mosenthal AC, Livingston DH, Lavery RF, et al. The effect of age on functional outcome in mild traumatic brain injury: 6-month report of a prospective multicenter trial. J Trauma 2004;56:1042.
43. Sokolowski M, et al. Acute mortality and complications of cervical spine injuries in the elderly at a single tertiary care center. Journal of Spinal Disorders 2007;20:352.
44. Mower WR, et al. Odontoid fractures following blunt trauma. Emergency Radiology 2000;7:3.
45. Mann E, et al. Improving the imaging diagnosis of cervical spine injury in the very elderly: Implications of the epidemiology of injury. Emergency Radiology 2000;7:36.
46. Daffner R, et al. Imaging for evaluation of suspected cervical spine trauma: A 2-year analysis. Injury 2006;37:652.
47. Chapman J, Bransford R. Geriatric spine fractures: An emerging healthcare crisis. J Trauma 2007;62:61.
48. Beattie LK, Jack Choi. Acute spinal injuries: Assessment and management. EBMedicine.net 2006;8.
49. Barry TB, Mcnamara RM. Clinical decision rules and cervical spine injury in the elderly patient: A word of caution. J Emerg Med 2005;29:433-436.
50. Lenchik L, Rogers LF, Delmas PD, et al. Diagnosis of osteoporotic vertebral fractures: Importance of recognition and description by radiologists. AJR 2004;183:949-958.
51. Yee WY, Cameron PA, Bailey MJ. Road traffic injury in the elderly. Emerg Med J 2006;23:42-46.
52. Surmal M, Turut H, Topcu S, et al. A comprehensive analysis of traumatic rib fractures: Morbidity, mortality, and management. Eur J Cardiothorac Surg 2003;24:133-138.
53. Wolfson A, et al. Blunt chest trauma. In: Harwood-Nuss Clinical Practice of Emergency Medicine, 4th ed. Lipincott Williams &Wilkins, 2005.
54. Bulger EM, Arneson MA, et al. Rib fractures in the elderly. J Trauma 2000;48:1040-1046.
55. Victoriono GP, Chong TJ, Pal JD. Trauma in the elderly patient. Arch Surg 2003;138:1094-1098.
56. Bulge E, Arenson M, Mock C, et al. Rib fractures in the elderly. J Trauma 2000;48:1040-1046.
57. Potaris K, Gakidis J, Mihos P, et al. Management of sternal fractures: 239 cases. Asian Cardiovascular Thoracic Annals 2002;10:145-149.
58. McGwin G Jr, Reiff D, Moran S, et al. Incidence and characteristics of motor vehicle collision-related blunt thoracic aortic injury according to age. J Trauma 2002;52:859-865.
59. Feckzo J, Lynch L, et al. An autopsy case review of 142 nonpenetrating (blunt) injuries of the aorta. J Trauma 1992;33:846.
60. Crass J, Cohen A, et al. A proposed new mechanism of traumatic aortic rupture: The osseous pinch. Radiology 1990;176:645-649.
61. Patel N, Stephen K, et al. Imaging of acute thoracic aortic injury due to blunt trauma: A review. Radiology 1998;209:335-348.
62. Benmenacham Y. Rupture of the thoracic aorta by broadside impacts in road traffic and other collisions: Further angiographic observations and preliminary autopsy findings. J Trauma 1993;35:363.
63. Cernainu A, Cilley J, et al. Determinants of outcome in lesions of the thoracic aorta in patients with multiorgan system trauma. Chest 1992;101:331.
64. Fox S, Waldhausen J. Acute hypertension: Its significance in traumatic aortic rupture. J Thoracic Cardiovascular Surgery 1979;77:672.
65. Symbas P, et al. Traumatic rupture of the aorta. Ann Surgery 1973;178:6.
66. Sturm J, et al. Significance of symptoms and signs in patients with traumatic aortic rupture. Ann Emerg Med 1984;13:876.
67. Mizushima Y, Hiraide A, et al. Changes in contused lung volume and oxygenation in patients with pulmonary parenchymal injury after blunt chest trauma. Am J Emerg Med 2000;18:385-389.
68. Shweiki E, Klena J, Wood GC et al. Assessing the true risk of abdominal solid organ injury in hospitalized rib fracture patients. J Trauma 2001;50:684-688.
69. Finelli FC, Johnson J, Champion HR. A case control study for major trauma in geriatric patients. J Trauma 1989;29: 541-548.
70. Baron JA, Barrett JA, Karagas MR. the epidemiology of peripheral fracture. Bone 1996;Mar 18 (3 Suppl):209S-213S.
71. De Laet CE, Pols HA. Fractures in the elderly: Epidemiology and demography. Baillieres Best Pract Res Clin Endocrinol Metab 2000;14:171.
72. Fernandez D, Jupietr J. Fractures of the Distal Radius: A Practical Approach to Management. New York: Springer-Vertag; 1996.
73. American Academy of Orthopedic Surgeons: The Treatment of Distal Radius Fractures: Guidelines and Evidence-based Report. AAOS v 1.0 12.05.09.
74. Henry SM, Pollak AN, Jones AL, et al. Pelvic fracture in geriatric patients: A distinct clinical entity. J Trauma 2002;53:15-20.
75. Alost T, Waldrop RD. Profile of geriatric pelvic fractures presenting to the emergency department. Am J Emerg Med 1997;15:576.
76. Stevens JA, Ryan G, Kresnow MS. Fatalities and injuries from falls among older adults United States, 1993–2003 and 2001–1005. MMWR Morb Mortal Wkly Rep 2006;55:1221.
77. Levy DB, Hanlon DP, et al. Geriatric trauma. Clin Geriartr Med 1993;9:201-274.
78. Beaupre LA, Jones CA, Sanders D, et al. Best practice for elderly hip fracture patients: A systemic review. J Gen Intern Med 2005;11:1019-1025.
79. Evans R. Trauma and falls. In: Sanders A, ed. Emergency Care of the Elder Person. St. Louis: Beverly Cracom Publishing; 1996: 153-170.
80. Koval KJ, Lurie J, Zhou W, et al. Ankle fracture in the elderly: What you get depends on where you live and who you see. J Orthop Trauma 2005;19:635-639.
81. Smith JSJ, Martin LF, Young WW, et al. Do trauma centers improve outcome over non-trauma centers? The evaluation of regional trauma care using discharge abstract data and patient management categories. J Trauma 1990;30: 1533-1538.
82. Meldon SW, Reilly M, Mancuso C, et al. Trauma in the very elderly: A community based study of outcomes at a trauma versus non-trauma centers. J Trauma 2002;52:79-84.
83. Chang DC, Bass RR, Cornwell EE, et al. Undertriage of elderly trauma patients to state-designated trauma centers. Arch Surg 2008;143:776-781; discussion 782.
84. Davis JW, Parks SN, Kaups KL, et al. Admission base deficit predicts transfusion requirements and risk of complications. J Trauma 1996;41:769-774.
85. Schulman AM, Claridge JA, Young JS. Young versus old: Factors affecting mortality after blunt traumatic injury. Am Surg 2002;68:942-947.
As the baby boomers become older adults, we will see a rapid rise not only in the older population, but also an increase in older patients. While older adults accounted for 13% of the population in the year 2000, by 2030 they will be at least 20% of the population, or almost 71 million.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
