The Breadth of Evidence Favoring a Whole Foods, Plant-based Diet
The Breadth of Evidence Favoring a Whole Foods, Plant-based Diet
Authors:
Thomas M. Campbell II, MD, Resident Physician, Department of Family Medicine, Strong Memorial Hospital, University of Rochester, NY
T. Collin Campbell, PhD, Professor Emeritus of Nutritional Biochemistry, Division of Nutritional Science, Cornell University, Ithaca, NY
Peer Reviewer:
Harvey S. Hahn, MD, FACC, Director, Cardiovascular Fellowship Training Program and Director, Cardiac Noninvasive Laboratory, Kettering Medical Center; Associate Professor of Clinical Medicine, Wright State University/Boonshoft School of Medicine and Loma Linda University; Adjunct Professor of Medicine, University of Cincinnati, OH
Part I: Metabolic Diseases and Diseases of Aging
Authors' Note
Nutrition is a controversial topic, perhaps because with only minimal effort it is possible to find seemingly credible people advocating for totally opposite messages. In the realm of public media, it is even worse. Quick weight loss schemes dominate magazine covers and radio ads. People advocating for their own brand of nutrition and health might exaggerate credentials and expertise and the public rarely cares. What's hot is hot, and that's about all that matters. A few years ago the trend was to skimp on everything but the meat and fat as part of a high-protein diet. Now it is becoming more popular for people to eat everything BUT meat and fat as part of a more vegetarian diet trend. How long this will last is anyone's guess. The fickle whim of public interest soon may turn to a hormone-based diet and weight loss plan or perhaps back to the low-carbohydrate days of eating burgers without buns with a side of sour cream, cheese, and eggs.
Despite public confusion, reviewing the evidence relating nutrition to health and disease yields more clarity than most people realize. A whole foods, plant-based diet has the broadest range of support in the scientific literature. That breadth of evidence is highlighted in this article, which is divided into two parts. Part I focuses on metabolic diseases and conditions of aging. Part II will cover malignancies and inflammation dysregulation syndromes.
Introduction
Nutrition has become one of the hottest topics in health and wellness. Doctors, especially primary care doctors, often are thrust in positions of educating patients about nutrition and health. Beyond simple education of patients, primary care practitioners are responsible for treating diseases caused by lifestyle without sufficient training in how lifestyle causes these diseases. Most doctors do not receive significant training in nutrition. Yet every primary care doctor knows that the 30-year-old patient in the office with back pain, high blood pressure, hyperlipidemia, and a body mass index (BMI) of 38 mg/kg2 got there at least in part because of what he or she chose to eat every day.
Physicians know that food and lifestyle is critical, but don't really know what is true regarding the evidence linking food and disease. Even avid followers of peer-reveiwed, published nutritional research can become confused easily. One day eggs are linked to heart disease, and the next day they are excellent sources of vitamins and minerals. One day alcohol is good for heart disease, but the next day it is bad for breast cancer. One day nutrition is known to be an important factor for preventing a certain cancer, and the next day there is no relation.
There are inherent difficulties to studying nutrition and its effect on health, which creates confusion. Nutrition is a holistic undertaking that cannot be easily controlled in populations. Food is comprised of thousands of chemicals. People eat imprecise mixtures of foods at every meal. People do not sit down to eat 100 g of wheat and 200 g of beef. Instead, a meal consists perhaps of pasta with sauces and toppings and a meat-based casserole with a few vegetables, or a burrito with 12 or more different ingredients. Measuring a person's exposure to food components is very difficult. In addition, the effect of food on health usually is delayed over the course of decades. Finally, many other factors exercise, substance abuse, genes, and possibly environmental chemicals and sun exposure affect health and disease outcomes. There is no possibility of having randomized controlled trials that randomize one group to eat one way for decades and another group to eat a substantially different way for decades with all other things being equal, thereby leaving a nice clean interpretation of the outcomes. Nutrition simply can't be studied that way.
So despite these best efforts, physicians still wonder what is true. Most of the existing data and research are observational in nature. Two major components the depth and breadth of the evidence supporting a particular conclusion determine the truth of any scientific argument.
Based on extensive reviews of the literature, a whole food, plant-based diet is likely to be the optimal diet, and the most consistent with optimal function and with optimal prevention, treatment, and management of many chronic diseases. Health care professionals often underestimate the power of dietary choices; diet could well be the most powerful weapon in an approach to promote health, prevent disease, and even treat those people with advanced chronic disease. "The China Study" is based largely on the work, experiences, and findings from a lifetime of nutrition research and policymaking of the senior author, and makes the case that a whole foods, plant-based diet is the optimal diet.
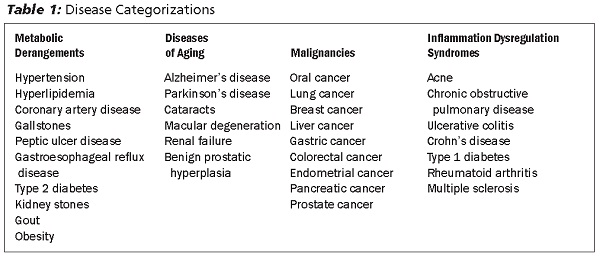
There are several ways to organize the different disease outcomes that diet may affect. One way is to consider disease outcomes as they cluster together. For the purposes of summarizing a wide range of possible dietary effects, this article will consider disease outcomes as part of four different categories, as shown in Table 1. This article will cover the metabolic derangements and diseases of aging and the article next month will cover malignancies and inflammation dysregulation syndromes.
Metabolic Derangements
It is perhaps most fitting to start with the effect of plant-based diets on vascular health. Hypertension, hyperlipidemia, obesity, diabetes, and coronary artery disease often cluster together. Metabolic syndrome, in fact, is defined by having three of the following: high blood pressure, high blood sugar, large waist circumference, low HDL, or high triglycerides. This constellation of ill health is common and is the group of ailments where there is the greatest depth of evidence that favors a whole foods, plant-based diet.
Hypertension
It has been observed repeatedly that vegetarians, and especially vegans, have a lower blood pressure than meat eaters. One study found that 15% of male meat eaters reported themselves as having a diagnosis of hypertension, whereas only 5.8% of their vegan counterparts said the same.1 For women, the story is similar: 12.1% of female meat eaters had hypertension but only 7.7% of female vegans. Much of the difference was due to the fact that the vegans were slimmer than meat eaters, but even after statistically eliminating the effect of body weight, vegans still had a significantly lower rate of high blood pressure. Another study of Seventh-Day Adventists in California found that vegans had a stunning 75% reduction in the prevalence of hypertension compared to nonvegetarians.2 Another study followed 500 patients participating in a 12-day diet program; after 12 days of eating a low-fat, plant-based diet, the patients' blood pressures dropped by 6%.3 Other researchers found that a more moderate vegetarian diet lowers systolic blood pressure by 5 mmHg in 6 weeks along with a modest drop in diastolic blood pressure. When subjects went back to their omnivorous diets, the blood pressure increased.4,5
Hyperlipidemia
Regarding blood cholesterol, plant-based diets are superior. One recent review of 27 randomized, controlled trials and observational studies in the American Journal of Cardiology found that people who eat plant-based diets have lower cholesterol levels.6 Trials putting patients on vegetarian or vegan diets repeatedly have shown that cholesterol levels go down.6 In one study, researchers studied three groups for a month: a control group who ate a very low-saturated fat vegetarian diet, a group who ate the control diet and took 20 mg of lovastatin daily, and a group that ate a low-dairy diet which cut out almost all animal foods and included more fiber and plant foods previously found to lower cholesterol.7 All groups ate a vegetarian diet, but the low-dairy diet was dramatically different in terms of protein content; it contained almost no animal protein, whereas the control diet had lots of protein from dairy sources. The result was that LDL cholesterol dropped 8.5% in subjects on the vegetarian, dairy-rich control diet alone, 33.3% on this control diet plus a statin, and 29.6% on the almost fully plant-based diet. The almost fully plant-based diet was nearly as effective as a dairy-rich vegetarian diet plus medication and was far better than the moderate vegetarian diet alone at lowering LDL cholesterol.7
Coronary Artery Disease
Historically, it has been well known that heart disease strikes populations of western countries far more commonly than traditional cultures.8,9 In fact, deaths from heart disease before the age of 65 were very rare in rural China around 1980.8 In addition, within populations of western countries, those groups that eat a more plant-based diet have a lower risk of cardiovascular mortality.2,10 Perhaps the effect is mediated by changes in hypertension, cholesterol levels, or even endothelial function. The dilatory arterial function was compared between vegetarians and nonvegetarians with both a mechanical and chemical challenge (a tourniquet test and administration of nitric oxide). The researchers found that the arteries dilated more in the vegetarians in response to both challenges.11
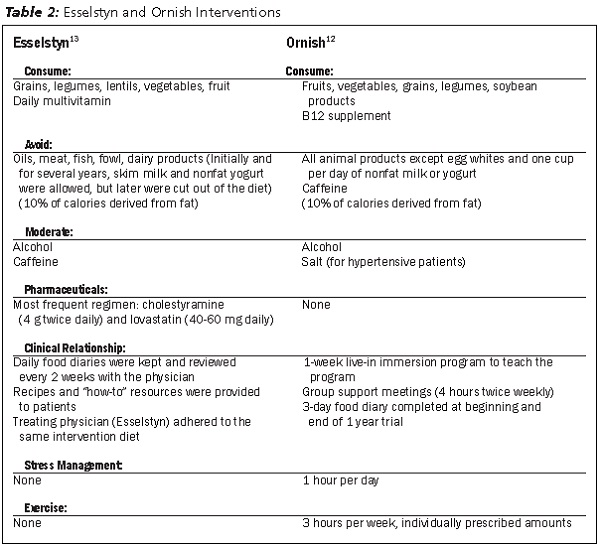
Most persuasively, it has now been shown that coronary heart disease can be reversed using a dietary approach. Two physicians, Dean Ornish and Caldwell Esselstyn, both have conducted trials of people with known heart disease and both have shown that interventions centered on low-fat, whole foods, plant-based diets can reverse blockages in coronary arteries and improve blood flow.12,13 Esselstyn included some cholesterol-lowering medicine in the intervention and Ornish included several other lifestyle components (See Table 2). Diets in both of these trials eliminated meat, added oils, and minimized dairy foods. No other diet-based trials, including those utilizing more moderate interventions, have ever reversed heart disease as these trials did.
Type 2 Diabetes
There is a great depth of evidence linking type 2 diabetes with diet, just as there is with cardiovascular disease. International populations that consume more fat and meat historically have been noted to have far higher rates of diabetes.14,15 This has been documented for more than 75 years.16 More recently, within a single population of Californian Seventh Day Adventists, a religious practice that encourages vegetarianism, vegetarians who consumed dairy foods were noted to have a 60% reduction in the prevalence of diabetes compared to nonvegetarians. Those who took it further, and were fully vegan, had an almost 80% lower prevalence of diabetes.2
But it doesn't stop with prevention. People who already have diabetes can treat and even reverse their disease using diet and lifestyle. A recent study found that even small increases in vegetable, fruit, and legume intake were associated with a lower risk of mortality, and particularly cardiovascular disease, among diabetics.17 More than 30 years ago, research was published where 20 thin diabetic men were monitored in the hospital and fed a high-carbohydrate, low-fat, high-fiber diet.18 All were on insulin at the start of the study. Of men with lower insulin dosages (up to 20 units per day), all but one were able to totally discontinue insulin after 16 days on the diet. The patient still on insulin decreased from 15 units to 2 units a day, and had to leave the hospital early, the day before his insulin was going to be stopped. Seven men required more daily insulin at baseline (an average of 30 units), and they were able to decrease their insulin to 12 units after just 16 days. Some of the men continued the diet and were able to totally discontinue their insulin as an outpatient. Three other men with more advanced disease and higher insulin requirements were able to lower their insulin requirements, but not by much, over the course of the trial.18 In addition, the average drop in blood cholesterol after just 16 days was 59 mg/dL, from 206 mg/dL to 147 mg/dL.18 Similar results have been achieved at another live-in program19,20
Obesity
Often people state that weight is a simple matter of calories in, calories out. But in fact there is evidence that where the calories come from matters. In a study of almost 400,000 people, researchers found that those people who ate more meat ended up gaining more weight.21 All things being equal, eating an extra 250 g of meat (half a steak) per day was associated with a weight gain of about 4.5 pounds over 5 years.21 This study controlled for the amount of total calories eaten, physical activity, and smoking among all participants. The authors write, "Our results suggest that a decrease in meat consumption may improve weight management."21 This observation comes on the heels of numerous observational studies that have found that vegetarians and vegans tend to be lower weight.2,10,22-26
Other results confirm that when people switch diets, they can lose weight. In one study of 64 overweight patients, participants embarked on an all-they-can-eat, low-fat, vegan dietary program over 3 months and lost an average of almost 13 pounds without extra exercise routines.27 A group eating a diet with only moderate changes lost about 7.5 pounds over the same time period.27
Gallstones
Gallstones are a harbinger of serious problems in the body. People who have gallstone disease die earlier, not necessarily from their gallbladder disease, but from the terrible health that usually goes hand in hand with gallbladder disease. They have a 50% higher rate of cardiovascular mortality, 30% higher rate of cancer mortality, 2.5 times the diabetes mortality, and higher mortality rates of chronic liver disease.28
Diet is convincingly associated with gallbladder health.29 Many animal models have shown that diets with more cholesterol increase the formation of gallstones and at least one human study has shown that the more cholesterol a person eats, the more cholesterol is in the bile, increasing the risk for gallstones.30 Cholesterol is only found in animal-based foods. Similarly, we know that obesity is linked with a higher risk of gallstones31 and some studies (but not all) have shown that eating more fat, particularly animal fat (including saturated fat), increases the risk of gallstones.32 Perhaps even more consistently, sugar consumption is implicated as a potential risk factor.29,32 In the Nurses' Health Study, researchers found that higher vegetable protein intake was linked to a decrease in the risk of having had the gallbladder removed, and higher total and animal protein was associated with higher risk, though the total and animal protein correlations may have been due to the effect of confounding variables, like weight and physical activity, as the correlation lost significance when adjusted for additional factors.33 In hamster experiments, 57% of the hamsters on diets with 20% casein (the main protein in cow's milk) had gallstones and only 14% of hamsters on diets with 20% soy protein had gallstones.34 More in-depth investigation35 of varying mixtures of casein and soy protein found that the more soy protein present in the feed, the fewer animals had gallstones. The benefits continued to accrue all the way down to diets containing no casein at all.
Women who eat more fruits and vegetables have been found to have a lower risk of having had their gallbladder removed.36 Increasing fiber is linked to lower risk of gallstones,29 and vegetarians have been found to have half the rate of gallstones compared to meat-eating counterparts.37
Ulcers/Gastritis
In one large recent study, duodenal ulcers were 33% less likely in people who ate more fruits and vegetables, 45% less likely in those eating the most fiber, and 60% less likely in those consuming the most vitamin A.38 Many other studies have confirmed that high-fiber, unprocessed plant foods protect against ulcers.39 Sugar or other refined carbohydrates are especially problematic.39 It is also worth noting that alcohol generally is not good for the gastrointestinal (GI) tract. Alcohol can cause increased reflux symptoms and gastritis, and has been linked to increased risk of several different types of cancers, especially in the upper GI tract.40
Gastro-esophageal Reflux Disease (GERD)
One of the most significant reasons for the rise of the reflux is its association with obesity, which is becoming more and more common. Being overweight increases the odds of having reflux by more than 50% and being obese more than doubles the risk.41 Weight loss, whether achieved through dieting or through surgery, has been shown to improve reflux symptoms.42 Of the specific dietary components, dietary fat seems to be a problem, being linked to increased risk of GERD, whereas fiber intake seems to be protective.43
Kidney Stones
Worldwide, the prevalence of kidney stones range from 2-20%, with the incidence higher in more developed countries.44 Kidney stones are more prevalent in those people who are obese, diabetic, and hypertensive.45 Those with kidney stones are more likely to have heart disease.45
Just as vegetarians seem to fare better with regards to obesity, hypertension, heart disease, and diabetes, they also fare better with kidney stones. Vegetarians get kidney stones at only 40-60% of the rates of non-vegetarians.46 It has been known for several decades that higher animal protein intake is well correlated with getting stones.47,48 For those who have recurrent stones, the risk of having another episode can be altered dramatically by dietary choices. A recent dietary trial assigned men with recurrent kidney stones to a low-calcium diet or a diet that was low in animal protein and salt and found that those men on the low animal protein, low-salt diet had only 50% the rate of recurrent stone formation over the next 5 years.49 Staying well hydrated also appears to be very important. In one study of patients with kidney stones, the group instructed to drink enough water to increase their urine volume to at least 2 liters per day had less than 50% of the stone recurrences than the no-increased-water control group had over 5 years.50
Gout
Hippocrates called gout the "arthritis of the rich."51 Those at higher risk of the disease include those who are overweight, have high blood pressure, high blood cholesterol, kidney stones, and kidney disease.52 Dietary factors known to be associated with increased risk include alcohol, especially beer and liquor, meat, refined sugars, and seafood.52 Foods or parts of foods that have been found to be associated with a lower risk of gout include fiber, fruit, folate, and vitamin C (all plant-based foods).52 Interestingly, in the context of a rich Western diet, dairy intake is also linked to a lower risk of gout, possibly lessening the bad effects of the other animal-based foods in the diet.52,53
Diseases of Aging
Alzheimer's Disease
The Swedish Twin Study compared patients with Alzheimer's disease or dementia and those people without these diseases and correlated presence of disease with fruit and vegetable intake as measured in a survey done 30 years earlier, before any brain disease was evident.54 After controlling for other factors, the study found that risk of dementia decreased by 27% and risk of Alzheimer's decreased by 40% in those people who had either medium or great fruit and vegetable intake compared to those with no or small intake of fruits and vegetables.
A recent prospective cohort study enrolling almost 2000 residents of New York City is even more impressive.55 Both physical activity and a dietary pattern comprised of above-average consumption of fruits, vegetables, legumes, cereals, and fish, and below-average consumption of meat and dairy products, saturated fat intake, and a small amount of alcohol were correlated with avoiding Alzheimer's disease. In fact, those adults who best adhered to this dietary pattern, along with the most exercise, had an astonishing 67% reduction in risk of getting Alzheimer's disease. The findings persisted even after controlling for multiple other risk factors.55
The same research group found that subjects consuming a more plant-enriched diet had a 28% reduction in risk of having mild cognitive impairment.56
Parkinson's Disease
Data from the Health Professionals Follow-Up Study and the Nurses' Health Study show a non-significant 22% reduction in Parkinson's disease risk with higher consumption of a "prudent" dietary pattern characterized by more unrefined fruits, vegetables, and whole grains.57
Cataracts
One study of women aged 50-79 years found that those subjects who had the highest levels of the antioxidants lutein and zeaxanthin in their diet or blood had a 32% lower risk of getting cataracts.58 These antioxidants are abundant in leafy green vegetables and to a lesser extent in other vegetables like broccoli, peas, and beans. This finding confirmed an earlier research study which found that people who consumed the most lutein were only half as likely to get cataracts.59
Similarly, another study of 1808 women found that consuming diets that adhere to the 1995 U.S. dietary guidelines resulted in 37% lower odds for cataracts, even when they controlled for BMI, smoking, age, and iris color, all of which are known to be factors in determining cataract risk.60 Those women eating the "healthy" dietary pattern in this study ate a diet consisting of more fruits and vegetables, less cholesterol and saturated fat, and only moderate fat levels in general. They consumed a wide variety of foods, including oils, meat, and dairy foods. Both oil intake and meat intake, however, were found to correlate with higher risk of cataracts.
Macular Degeneration
One case-control study published in 1994 found that certain nutrient intakes were protective against macular degeneration.61 Those who consumed the most carotenoids, especially lutein and zeaxanthin, were found to have a 43% lower risk of getting age-related macular degeneration. Found in no animal foods (except in tiny amounts where the animal concentrate the carotenoids they eat in their diet), the hundreds of different carotenoids provide the bright colors of many different vegetables. Researchers also found that those patients who ate the highest quantities of foods that are rich in carotenoids, including broccoli, cabbage, carrots, leafy greens, sweet potatoes, and squash, had lower rates of macular degeneration.
Renal Failure
Renal blood flow and glomerular filtration rate (GFR) declines with age, but diet may play an important role. For 175 years it has been known that protein intake has a special effect on kidney function.62 High protein intake causes increased blood flow through the glomerulus. With unrestricted calorie intake of high-protein foods, increased blood flow has been found to cause glomerular hypertrophy and sclerosis.63
In the early 1980s, a paper was published that showed extra filtration was associated with damage to the kidney units,64 an idea referred to as the "hyperfiltration hypothesis." Researchers who originated the hyperfiltration hypothesis found that a low-protein diet seemed to significantly blunt the damage to the kidneys by lowering the amount of filtration through each glomerulus.64
Most of the professional societies worldwide suggest that people with chronic kidney disease consume no more than the minimum amount recommended of daily protein levels and certainly far less than the average western diet.65 The recommendations are 0.6-0.8 g/kg/day of protein rather than 1.3-1.4 g/kg/day typical of the Western diet.65 Other benefits of adopting a lower-protein diet for kidney health include improving insulin resistance, hypertension, bone and mineral disorders, and cholesterol profile, all of which are important for patients with impaired kidney function.66 In addition, there has been evidence that less protein spills out of the urine, a change that happens within days.66
Not only the amount of protein, but also the type may make a difference. There is now evidence to suggest that plant proteins are less toxic to kidneys than animal proteins.67-69
Benign Prostatic Hypertrophy
Benign prostatic hypertrophy is present in up to 90% of men in their 70s.70 Men with diabetes and obesity have a higher risk of disease, and eating meat and fat are associated with increased risk.71,72 Eating vegetables is associated with a decreased risk.71-73 Furthermore, although prostate size is not assessed routinely in a precise way, prostate-specific antigen (PSA) is a good marker for the actual size of the prostate itself.74 Dean Ornish and colleagues performed a 1-year, randomized, controlled dietary trial of men with prostate cancer and found that a whole foods, plant-based diet lowered PSA by 4% compared to a 6% PSA increase in the control group following regular dietary advice.75
Conclusion
In medical communities, diet is sometimes mentioned as an option to improve health or prevent or treat disease, but it usually is discussed only in the context of metabolic derangements. It is easy to see why this is the case. For all the breadth of effects across various disease groups, there is no greater depth of evidence supporting the importance of diet than that for dietary effects on metabolic diseases. There are human observational and intervention trials and supporting animal model mechanistic research for a number of different common metabolic problems. Published results now show that hypertension, hyperlipidemia, coronary artery disease, obesity, diabetes, and recurrent kidney stones all have been treated effectively with diet and lifestyle interventions. In fact, the most profound angiographically documented reversal of heart disease published has come from a primarily dietary intervention.13 Furthermore, the intervention that has been linked to such broad benefits is consistently the same type of dietary intervention: more fruits, vegetables, and whole grains, and less meat, dairy, added fat, and processed foods. No other dietary pattern can boast such robust support in published literature, despite the variety of claims and dietary patterns trumpeted in the public media.
The fact that the same type of diet or dietary components have been linked to lower incidence of the conditions assigned to "disease of aging" adds to the weight of the evidence. The depth of evidence present for diseases of aging is not nearly as robust as that for metabolic derangements. For example, though cataracts and macular degeneration are inversely associated with dietary intake of certain antioxidants in observational trials, the evidence thus far is fairly limited. There is even less depth of evidence for Parkinson's disease. Alzheimer's disease now has a deeper base of data, as does kidney disease, but even these do not have the depth of evidence equal to that present in diet-metabolic disease literature.
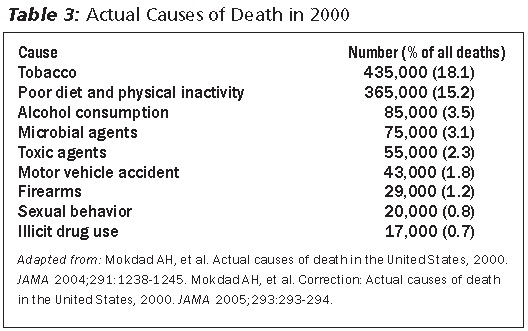
Nonetheless, there is enough research to begin to piece together some interesting trends. Given this, the emerging trend of unrefined, plant-based foods being linked to benefits across such a range of disease processes and organ systems suggests obvious conclusions. In part II of this series, the trend continues, but additional discussion is required to disentangle the nutrition and cancer literature. Though there is more research needed to refine our conclusions, this should not stop us from translating this research into clinical practice. A recent conservative analysis76,77 shows that poor diet and physical inactivity (as manifested by being overweight) is responsible for 15% of all deaths and is the second leading cause of death resulting from modifiable risk factors (See Table 3). Conservatively, almost one out of every six patients walking into a primary care clinic will die of what they choose to eat or not eat and whether they exercise or not.
References
1. Appleby PN, et al. Hypertension and blood pressure among meat eaters, fish eaters, vegetarians, and vegans in EPIC-Oxford. Public Health Nutr 2002;5:645-654.
2. Fraser GE. Vegetarian diets: What do we know of their effects on common chronic diseases? Am J Clin Nutr 2009;89:1607S-1612S.
3. McDougall J, et al. Rapid reduction of serum cholesterol and blood pressure by a twelve-day, very low fat, strictly vegetarian diet. J Am Coll Nutr 1995;14:491-496.
4. Margetts BM, et al. Vegetarian diet in mild hypertension: A randomised controlled trial. Br Med J (Clin Res Ed) 1986;293:1468-1471.
5. Rouse IL, et al. Blood-pressure-lowering effect of a vegetarian diet: Controlled trial in normotensive subjects. Lancet 1983;1:5-10.
6. Ferdowsian HR, Barnard ND. Effects of plant-based diets on plasma lipids. Am J Cardiol 2009;104:947-956.
7. Jenkins DJ, et al. Direct comparison of a dietary portfolio of cholesterol-lowering foods with a statin in hypercholesterolemic participants. Am J Clin Nutr 2005;81:380-387.
8. Campbell TC, et al. Diet, lifestyle, and the etiology of coronary artery disease: The Cornell China study. Am J Cardiol 1998;82:18T-21T.
9. Scrimgeour EM, et al. Levels of serum cholesterol, triglyceride, HDL-cholesterol, apoproteins A-I and B, and plasma glucose, and prevalence of diastolic hypertension and cigarette smoking in Papua New Guinea highlanders. Pathology 1989;21:46-50.
10. Key TJ, et al. Mortality in vegetarians and nonvegetarians: Detailed findings from a collaborative analysis of 5 prospective studies. Am J Clin Nutr 1999;70:516S-524S.
11. Lin CL, et al. Vascular dilatory functions of ovo-lactovegetarians compared with omnivores. Atherosclerosis 2001;158:247-251.
12. Ornish D, et al. Can lifestyle changes reverse coronary heart disease? The Lifestyle Heart Trial.[see comment]. Lancet 1990;336:129-133.
13. Esselstyn CB Jr, et al. A strategy to arrest and reverse coronary artery disease: A 5-year longitudinal study of a single physician's practice. J Fam Pract 1995;41:560-568.
14. West KM, Kalbfleisch JM. Influence of nutritional factors on prevalence of diabetes. Diabetes 1971;20:99-108.
15. West KM, Kalbfleisch JM. Glucose tolerance, nutrition, and diabetes in Uruguay, Venezuela, Malaya, and East Pakistan. Diabetes 1966;15:9-18.
16. Himsworth H. Diet and the incidence of diabetes mellitus. Clin Sci 1935;2:117-148.
17. Nothlings U, et al. Intake of vegetables, legumes, and fruit, and risk for all-cause, cardiovascular, and cancer mortality in a European diabetic population. J Nutr 2008;138:775-781.
18. Anderson JW, Ward K. High-carbohydrate, high-fiber diets for insulin-treated men with diabetes mellitus. Am J Clin Nutr 1979;32:2312-2321.
19. Barnard RJ, et al. Response of non-insulin-dependent diabetic patients to an intensive program of diet and exercise. Diabetes Care 1982;5:370-374.
20. Barnard RJ, et al. Long-term use of a high-complex-carbohydrate, high-fiber, low-fat diet and exercise in the treatment of NIDDM patients. Diabetes Care 1983;6:268-273.
21. Vergnaud AC, et al. Meat consumption and prospective weight change in participants of the EPIC-PANACEA study. Am J Clin Nutr 2010;92:398-407.
22. Ellis FR, Montegriffo VM. Veganism, clinical findings and investigations. Am J Clin Nutr 1970;23:249-255.
23. Bergan JG, Brown PT. Nutritional status of "new" vegetarians. J Am Diet Assoc 1980;76:151-155.
24. Appleby PN, et al. Low body mass index in non-meat eaters: The possible roles of animal fat, dietary fibre and alcohol. Int J Obes Relat Metab Disord 1998;22:454-460.
25. Dwyer JT. Health aspects of vegetarian diets. Am J Clin Nutr 1988;48:712-738.
26. Newby PK, et al. Risk of overweight and obesity among semivegetarian, lactovegetarian, and vegan women. Am J Clin Nutr 2005;81:1267-1274.
27. Barnard ND, et al. The effects of a low-fat, plant-based dietary intervention on body weight, metabolism, and insulin sensitivity. Am J Med 2005;118:991-997.
28. Ruhl CE, Everhart JE. Gallstone disease is associated with increased mortality in the United States. Gastroenterology 2011;140:508-516.
29. Gaby AR. Nutritional approaches to prevention and treatment of gallstones. Altern Med Rev 2009;14:258-267.
30. Lee DW, et al. Effect of dietary cholesterol on biliary lipids in patients with gallstones and normal subjects. Am J Clin Nutr 1985;42:414-420.
31. Banim PJ, et al. The aetiology of symptomatic gallstones quantification of the effects of obesity, alcohol and serum lipids on risk. Epidemiological and biomarker data from a UK prospective cohort study (EPIC-Norfolk). Eur J Gastroenterol Hepatol 2011;23:733-740.
32. Cuevas A, et al. Diet as a risk factor for cholesterol gallstone disease. J Am Coll Nutr 2004;23:187-196.
33. Tsai CJ, et al. Dietary protein and the risk of cholecystectomy in a cohort of US women: The Nurses' Health Study. Am J Epidemiol 2004;160:11-18.
34. Kritchevsky D, Klurfeld DM. Influence of vegetable protein on gallstone formation in hamsters. Am J Clin Nutr 1979;32:2174-2176.
35. Kritchevsky D, Klurfeld DM. Gallstone formation in hamsters: Effect of varying animal and vegetable protein levels. Am J Clin Nutr 1983;37:802-804.
36. Tsai CJ, et al. Fruit and vegetable consumption and risk of cholecystectomy in women. Am J Med 2006;119:760-767.
37. Pixley F, et al. Effect of vegetarianism on development of gall stones in women. BMJ 1985;291:11-12.
38. Aldoori WH, et al. Prospective study of diet and the risk of duodenal ulcer in men. Am J Epidemiol 1997;145:42-50.
39. Misciagna G, et al. Diet and duodenal ulcer. Dig Liv Dis 2000;32:468-472.
40. Bujanda L. The effects of alcohol consumption upon the gastrointestinal tract. Am J Gastroenterol 2000;95:3374-3382.
41. Corley DA, Kubo A. Body mass index and gastroesophageal reflux disease: A systematic review and meta-analysis. Am J Gastroenterol 2006;101:2619-2628.
42. De Groot NL, et al. Systematic review: The effects of conservative and surgical treatment for obesity on gastro-oesophageal reflux disease. Aliment Pharmacol Ther 2009;30:1091-1102.
43. El-Serag HB, et al. Dietary intake and the risk of gastro-oesophageal reflux disease: A cross sectional study in volunteers. Gut 2005;54:11-17.
44. Johri N, et al. An update and practical guide to renal stone management. Nephron Clin Prac 2010;116:c159-c171.
45. Sakhaee K. Nephrolithiasis as a systemic disorder. Curr Opin Nephrol Hypertens 2008;17:304-309.
46. Robertson WG, et al. Prevalence of urinary stone disease in vegetarians. Eur Urol 1982;8:334-339.
47. Robertson WG. Diet and calcium stones. Min Electrolyte Metab 1987;13:228-234.
48. Robertson WG, et al. Dietary changes and the incidence of urinary calculi in the U.K. between 1958 and 1976. J Chron Dis 1979;32:469-476.
49. Borghi L, et al. Comparison of two diets for the prevention of recurrent stones in idiopathic hypercalciuria.[see comment]. N Engl J Med 2002;346:77-84.
50. Borghi L, et al. Urinary volume, water and recurrences in idiopathic calcium nephrolithiasis: a 5-year randomized prospective study. J Urol 1996;155:839-843.
51. Nuki G, Simkin PA. A concise history of gout and hyperuricemia and their treatment. Arthritis Res Ther 2006;8(Suppl 1):S1.
52. Singh JA, et al. Risk factors for gout and prevention: A systematic review of the literature. Curr Opin Rheumatol 2011;23:192-202.
53. Choi HK, et al. Purine-rich foods, dairy and protein intake, and the risk of gout in men. N Engl J Med 2004;350:1093-1103.
54. Hughes TF, et al. Midlife fruit and vegetable consumption and risk of dementia in later life in Swedish twins. Am J Geriatr Psychiatry 2010;18:413-420.
55. Scarmeas N, et al. Physical activity, diet, and risk of Alzheimer disease. JAMA 2009;302:627-637.
56. Scarmeas N, et al. Mediterranean diet and mild cognitive impairment. Arch Neurol 2009;66:216-225.
57. Gao X, et al. Prospective study of dietary pattern and risk of Parkinson disease. Am J Clin Nutr 2007;86:1486-1494.
58. Moeller SM, et al. Associations between age-related nuclear cataract and lutein and zeaxanthin in the diet and serum in the Carotenoids in the Age-Related Eye Disease Study, an Ancillary Study of the Women's Health Initiative. Arch Ophthalmol 2008;126:354-364.
59. Lyle BJ, et al. Antioxidant intake and risk of incident age-related nuclear cataracts in the Beaver Dam Eye Study. Am J Epidemiol 1999;149:801-809.
60. Mares JA, et al. Healthy diets and the subsequent prevalence of nuclear cataract in women. Arch Ophthalmol 2010;128:738-749.
61. Seddon JM, et al. Dietary carotenoids, vitamins A, C, and E, and advanced age-related macular degeneration. Eye Disease Case-Control Study Group. JAMA 1994;272:1413-1420.
62. Anderson JW, et al. Effects of soy protein on renal function and proteinuria in patients with type 2 diabetes. Am J Clin Nutr 1998;68:1347S-1353S.
63. Brenner BM, et al. Dietary protein intake and the progressive nature of kidney disease: The role of hemodynamically mediated glomerular injury in the pathogenesis of progressive glomerular sclerosis in aging, renal ablation, and intrinsic renal disease. N Engl J Med 1982;307:652-659.
64. Hostetter TH, et al. Hyperfiltration in remnant nephrons: A potentially adverse response to renal ablation. J Am Soc Nephrol 2001;12:1315-1325.
65. Fouque D, et al. Nutrition and chronic kidney disease. Kidney Int 2011;80:348-357.
66. Fouque D, Aparicio M. Eleven reasons to control the protein intake of patients with chronic kidney disease. Nat Clin Pract Nephrol 2007;3:383-392.
67. Bernstein AM, et al. Are high-protein, vegetable-based diets safe for kidney function? A review of the literature. J Am Diet Assoc 2007;107:644-650.
68. de Mello VD, et al. Withdrawal of red meat from the usual diet reduces albuminuria and improves serum fatty acid profile in type 2 diabetes patients with macroalbuminuria. Am J Clin Nutr 2006;83:1032-1038.
69. Knight EL, et al. The impact of protein intake on renal function decline in women with normal renal function or mild renal insufficiency. Ann Intern Med 2003;138:460-467.
70. Edwards JL. Diagnosis and management of benign prostatic hyperplasia. Am Fam Phys 2008;77:1403-1410.
71. Kristal AR, et al. Dietary patterns, supplement use, and the risk of symptomatic benign prostatic hyperplasia: Results from the prostate cancer prevention trial. Am J Epidemiol 2008;167:925-934.
72. Parsons JK. Lifestyle factors, benign prostatic hyperplasia, and lower urinary tract symptoms. Curr Opin Urol 2011;21:1-4.
73. Rohrmann S, et al. Fruit and vegetable consumption, intake of micronutrients, and benign prostatic hyperplasia in US men. Am J Clin Nutr 2007;85:523-529.
74. Roehrborn CG, et al. Serum prostate-specific antigen as a predictor of prostate volume in men with benign prostatic hyperplasia. Urol 1999;53:581-589.
75. Ornish D, et al. Intensive lifestyle changes may affect the progression of prostate cancer. J Urol 2005;174:1065-1069; discussion 9-70.
76. Mokdad AH, et al. Actual causes of death in the United States, 2000. JAMA 2004;291:1238-1245.
77. Mokdad AH, et al. Correction: actual causes of death in the United States, 2000. JAMA 2005;293:293-294.
Nutrition is a controversial topic, perhaps because with only minimal effort it is possible to find seemingly credible people advocating for totally opposite messages. In the realm of public media, it is even worse. Despite public confusion, reviewing the evidence relating nutrition to health and disease yields more clarity than most people realize.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
