Case Management Insider

A further look into case management roles, functions, models, and case loads
By Toni Cesta, PhD, RN, FAAN
Senior Vice President
Lutheran Medical Center
Brooklyn, NY
In the last two issues of Case Management Insider, we reviewed the roles and functions most often associated with the work of case managers in the acute care setting. In this issue we will discuss the ways in which these roles and functions can be combined to create the most effective and efficient model for any hospital or healthcare setting. We also will discuss the state-of-the-art staffing ratios needed to support the various models.
The history of case management models
The prospective payment system for Medicare patients initiated the need for hospital staff to begin to think differently about how they organize and deliver care. Because hospitals would now be paid one fee for the entire stay, managing length of stay and cost containment became new necessities for hospitals. Gone were the indemnity reimbursement methods under which hospitals had operated. Under the old payment schemes, hospitals were paid equally for services rendered, usually with little questions asked. With the advent of prospective payment and diagnosis related groups (DRGs), the federal government had essentially put hospitals on a budget, paying them a flat fee for the hospital stay, also known as a case rate payment. It was believed that this type of payment scheme was to provide incentives to hospitals to become more efficient, thereby lowering costs and length of stay.
The logic behind prospective payment systems that drives the need for hospitals to become more efficient is that the hospital is able to deliver the care, and spend less than the fixed reimbursement amount, then they get to keep the surplus. Conversely, if the hospital spends more than the fixed reimbursement amount, then they have to absorb that additional cost. The goal is to ultimately balance out all costs, knowing that some patients will cost more than the reimbursed amount, and some less.
Following Medicare's reimbursement changes, many states adopted similar case rate methodologies for their Medicaid programs. Within a few years, as healthcare costs continued to rise, managed care organizations began to offer healthcare benefit packages to employers at lower premium costs than had been offered under the indemnity programs. Although managed care had been around for decades, it wasn't until the later 1980s that it began to become increasingly popular. Its popularity correlated directly with the rising costs of healthcare throughout the United States. With increasing percentages of managed care penetration, a continued focus on length of stay management and cost containment remained critical to the financial viability of hospitals.
It became clear that modifications to the existing delivery methods that preceded prospective payment were essential. With this began a significant shift in how hospitals viewed case management, and many hospitals began to develop some version of a case management model at that time. There were no national standards for case management roles, functions, models, or staffing ratios yet. Each hospital attempted to take their existing structures and modify them in some way.
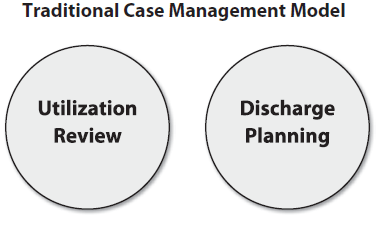
Most hospitals started with the traditional case management models which were a combination of utilization review and discharge planning. Utilization review, performed by nurses, was separate from discharge planning, performed by social workers. The two roles did not intersect and had little to do with each other. In fact, prior to the introduction of prospective payment and managed care, there was little need for an integrated approach to these functions. Once the reimbursement structures changed, the delivery models also had to change.
Partially integrating models and roles
By Toni Cesta, PhD, RN, FAAN
Senior Vice President
Lutheran Medical Center
Brooklyn, NY
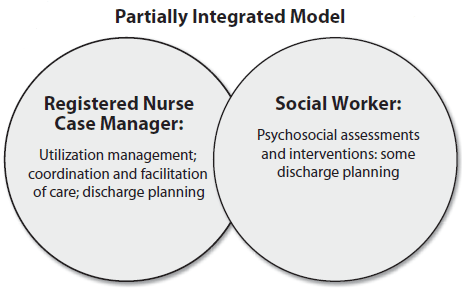
At this point, some hospitals began to attempt to interface the roles of utilization review and discharge planning. These models began to integrate the previously disconnected roles of utilization management and coordination and facilitation of care with discharge planning. These roles began to intersect with discharge planning, which was managed by social work in the early models.
As discharge planning began to become more complex, and as patients' psychosocial issues needed to be addressed, a shift began to take place in the management of the discharge planning processes. Some hospitals began to consider moving some of the discharge planning functions to the nurse case manager, so that the social worker could spend more time dealing with the patient's psychosocial issues. At the same time, this would allow the nurse to manage more clinically complex discharge planning activities, such as home care placement, sub-acute and home infusion therapy. The need to relate patients' clinical issues to their level of care and their discharge plan, drove this change forward. In addition, the continuum of care was becoming more robust, with ever increasing options available beyond the walls of the hospital. Care began to shift to the out-patient environment with an explosion in home care agencies, infusion companies, as well as the use of sub-acute and ambulatory surgery. By the mid-1990s hospitals began to move toward more fully integrated models. Today, we see a variety of models that have been adapted to the specific needs of organizations. However, there are some fundamentals to any model that should be used. Adaptations can be made to these fundamental core roles.
The state-of-the-art in CM models
By Toni Cesta, PhD, RN, FAAN
Senior Vice President
Lutheran Medical Center
Brooklyn, NY
Today, we see two basic versions of case management models: the integrated (dyad) model and the collaborative (triad) model. With each of these foundational models hospitals can add the additional roles that they require to meet their specific needs.
• The integrated dyad model.
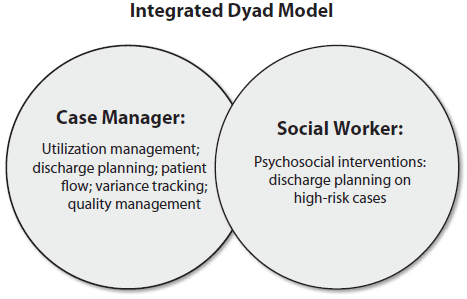
The integrated model represents a fully integrated model in which all core functions of case management are under the responsibility of the nurse case manager. It represents one of the state-of-the-art models in use today. In this model, all case management roles are performed by a single case manager. The model integrates all previously disconnected roles and functions. In the integrated model, the nurse case manager and social worker collaborate on the most complex cases.
Case managers working in this type of structure manage the patients in one of two ways. Either all the patients have a case manager assigned to them, or some do, based on pre-determined selection criteria. Today, the state-of-the-art model is to have all patients assessed and followed by a nurse case manager. Selecting only some patients for case management may result in patients falling through the cracks and ultimately not receiving the post-acute care services they may need.
However, in this model, not all patients will need to be followed by a social worker. The patients that will be followed will depend on the hospital's high-risk criteria that they select to help identify those patients who would benefit from social work services. These criteria should be prospectively determined and understood by the case management team, as well as the other disciplines such as physicians and nurses. If not well understood, this can result in unnecessary referrals being made to social work, and additional work placed on the social worker to screen these patients out.
In the dyad model, the case manager is responsible for some additional roles and functions. These include the addition of discharge planning and variance management.
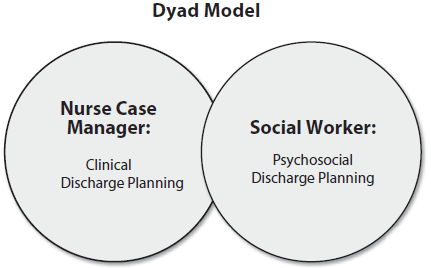
In the dyad model, the social worker may be responsible for some of the discharge planning functions, or may be solely responsible for psychosocial assessments and interventions, with discharge planning completely under the responsibilities of the nurse case manager. The decision to share the discharge planning functions is that of the hospital, and has to be carefully considered. Things to be considered would include the types of patients the hospital typically cares for. If the hospital deals with highly psychosocially complex patients, then some consideration should be given to how the work is allotted to each discipline.
The average hospital should expect to have 30–40% of their patients followed by a social worker as these are the average percentages of patients that will typically match high-risk referral criteria. The role of the social worker will be discussed in more detail in a future issue.
The integrated model is designed to allow for the division of discharge planning functions based on the issues that the patient presents with. Simply stated, the nurse case manager takes responsibility for the functions associated with discharge planning that are more clinical in nature, and the social worker takes responsibility for the function of discharge planning that are more psychosocial in nature.
• The collaborative (triad) model.
The collaborative or triad model adds a third key player to the core case management team. In this model, the clinical and business functions of case management are separate roles with three team partners actively working together. The case manager is not responsible for the business functions which are defined as:
Utilization management: Obtaining authorizations, managing observation status, and denial management.
• Clinical documentation improvement.
These roles are performed by the third member of the team, the Utilization Management/Diagnosis Related Group (UM/DRG) manager. The UM/DRG manager primarily works the business side of case management, including intense review of documentation. The UM/DRG manager is the liaison between the team members and the regulatory and payer entities.
The case manager is responsible for risk screening, assessment and planning, coordination of care, resource management, and outcomes management. By separating the business roles from the clinical roles of case management, the case manager can spend more time dealing with complex clinical issues instead of payer or reimbursement issues.
In this model, the social worker performs very similar roles and functions as in the integrated model. These include screening of patients, assessment and planning, brief therapeutic interventions, care planning, and crisis intervention. For high-risk cases, the social worker assists with discharge planning functions as needed.
The key difference between these case management models is the integration of utilization management into the case manager role versus a separate UM/DRG specialist role. Since both models are considered state-of-the-art, each hospital must determine which model will best help them achieve their expected outcomes.
Pros and cons of CM models
By Toni Cesta, PhD, RN, FAAN
Senior Vice President
Lutheran Medical Center
Brooklyn, NY
All models have advantages and disadvantages. The decision to select one model over another will depend on many factors that must be taken into consideration. To aid in the decision making process, below is a table outlining the advantages of each model.
| Advantages of Integrated v. Collaborative Model | |
|
Integrated Model |
Collaborative Model |
|
Everything under one umbrella. |
Consolidates business functions of case management into one role- builds expertise. |
|
Reduced duplication, fragmentation and redundancy. |
Case managers not consumed with routine payer functions. |
|
Data collected once for multiple purposes. |
Case managers have time to focus on more leveraged functions. |
|
Case manages in direct communication with third-party payers and vendors — they know the case. |
Expanded focus on documentation review and improvement. |
| Disadvantages of Integrated v. Collaborative Model | |
|
Integrated Model |
Collaborative Model |
|
Bundles highly time-dependent functions [discharge planning and utilization management]. Can be frustrating for staff to manage. |
Requires intensive communication between triad members. |
|
If not done well, can morph into a set of tasks rather than an integrated approach to the roles and functions. |
Creates some duplication. The utilization manager and case manager are reviewing the chart for similar or same information. |
|
Detail work of UM may appeal to some staff more than other aspects of case management. |
Works best if all disciplines report to the same administrator. |
|
Will not work if staffing is inadequate. Infrastructure will crumble. |
May be more costly and require more staff members. |
|
Will not work if staffing is inadequate. Infrastructure will crumble. |
|
In the last two issues of Case Management Insider, we reviewed the roles and functions most often associated with the work of case managers in the acute care setting.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
