Updating the 2000 Published Guidelines for Preventing Episodic Migraine: Is Anyone Listening?
Updating the 2000 Published Guidelines for Preventing Episodic Migraine: Is Anyone Listening?
Abstract & Commentary
By Jeff Unger, MD. Director, Metabolic Studies, Catalina Research Institute, Chino, CA. Dr. Unger reports no financial relationships relevant to this field of study.
Synopsis: This paper updates the American Headache Society and American Academy of Neurology guidelines for prevention of episodic migraine that were previously published in 2000.
Source: Loder E, et al. The 2012 AHS/AAN guidelines for prevention of episodic migraine: A summary and comparison with other recent clinical practice guidelines. Headache 2012; 52:930-945.
Headache specialist liz loder performed a medline search for publications dated January 2008 through April 2012 using the text words and medical subject heading "migraine" and "guidelines." The electronic database search was supplemented by a computerized website query that listed disease state guidelines. Two other authors rated the quality of evidence presented in the papers using the Appraisal of Guidelines for Research and Evaluation (AGREE) II criteria, which are used to assess the quality of clinical practice guidelines. AGREE's evidence-based premise is predicated on 23 questions distributed among six quality domains and two global quality rating scales.1 Two to four reviewers must assess each of the domains independently to determine the true quality of the level of evidence presented in a given paper. Before explaining what treatments for migraineurs are now recommended, we must first define the population for which these guidelines are intended. Episodic migraine pertains to patients who experience headache < 15 days each month and who are age 18 and older.2,3 (Patients having more frequent headaches are diagnosed with chronic, rather than episodic, migraine. These updated guidelines are irrelevant to chronic migraine patients). Similarly, onabotulinumtoxin A (BOTOX) is not mentioned in this paper because the FDA approved its use for the treatment of chronic migraine in October 2010. Pregnancy was excluded from this review.
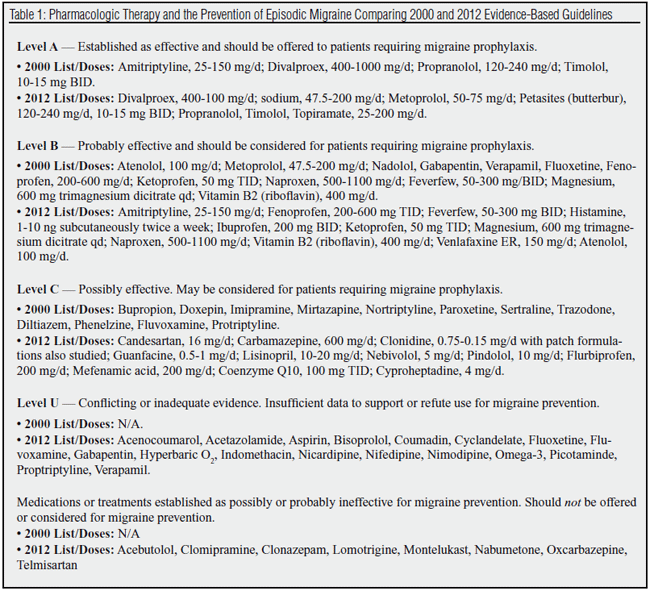
The authors defined four levels of evidence: Level A (drugs that are established as effective and should be prescribed to patients requiring migraine prevention); Level B (drugs that are probably effective and should be considered for patients requiring migraine prevention); Level C (drugs that could possibly be effective and may be considered for patients requiring migraine prevention); and Level U (drugs with conflicting or inadequate evidence of efficacy or with evidence indicating lack of efficacy).
Table 1 shows the medications that may be considered for migraine prevention, based on this extensive evidence-based literature search. Note that the position of several drugs has changed from 2000 to 2012, with some rising to higher levels of evidence and others dropping to lower rated evidence-based scores.
Commentary
The United States is home to 21 million migraineurs, and nearly 90% of these patients frequent the offices of primary care physicians, not headache specialists.4 My guess is that very few of my peers are aware of these published guidelines. Patients with migraine are often misdiagnosed as having acute sinusitis and are treated with courses of antibiotics and NSAIDS.3
Unless a patient has a coexisting mental illness, very few migraineurs look forward with open anticipation to their next disabling headache! Migraineurs are born with a genetically enhanced sensitive nervous system that may be activated by specific or mysterious triggers. I like to explain to my patients that I can give anyone a migraine. It's really easy. All I have to do to trigger a migraine is to hit someone over the head with a baseball bat. Within a few minutes they will have a severe, disabling headache associated with nausea, vomiting, and light and sound sensitivity. I doubt that they would be able to return to work over the course of the next 72 hours as they recover from the beating. Migraineurs do not require this type of blunt trauma to activate the trigeminal nerve and trigger an episodic migraine. Instead, a simple change in weather could cause their trigeminal nucleus caudalis to come to life, sending neurological impulses to the brainstem resulting in dizziness, nausea, and vomiting or to the cortex where for the next 72 hours they will experience a moderate-to-severe headache. By the way, if the second branch of the trigeminal nerve is activated, patients will experience facial pain and nasal congestion that will be interpreted as originating from the maxillary sinuses.5 Most migraineurs will be shocked when they learn that they are actually experiencing a true migraine as opposed to a sinus headache.
Migraineurs who attempt to work will likely be limited in their productivity. Likewise, what would an employer do if the office manager called in sick 7 days each month due to headache?
As primary care physicians, we owe our patients the ability not only to diagnose primary headache properly, but to provide the best possible prevention strategies. Behavioral interventions favorable to migraineurs include going to bed and waking up at the same time each day of the week, avoiding meal skips, stopping smoking, exercising for 30 minutes each day, and minimizing caffeine consumption. Using Loder's evidence-based list of preventives for episodic medications is also helpful. The initial goal is to reduce the headache frequency, intensity, and duration by 50% within 4 weeks of a patient's first visit with the use of behavior changes in combination with preventive and abortive migraine agents.
References
1. Brouwers MC, et al. AGREE II: Advancing guideline development, reporting and evaluation in health care. J Clin Epidemiol 2010;63:1308-1311.
2. Lipton RB, et al. Migraine prevalence, disease burden, and the need for preventive therapy. Neurology 2007; 68:343-349.
3. Holland S, et al. Evidence-based guideline update: NSAIDs and other complementary treatments for episodic migraine prevention in adults. Neurology 2012; 78:1346-1353.
4. Unger J, Schreiber CP (Eds). Disease-a-Month. Migraine. Vol. 52, No. 10. Philadelphia: Mosby Publications; 2006: 363-402.
5. Unger J, Guest Editor. Clinics in Family Medicine Migraine. Philadelphia: Elseiver Publications; 2005.
This paper updates the American Headache Society and American Academy of Neurology guidelines for prevention of episodic migraine that were previously published in 2000.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
