ECG Review
ECG Review
Would You Clear for Surgery?
By Ken Grauer, MD, Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
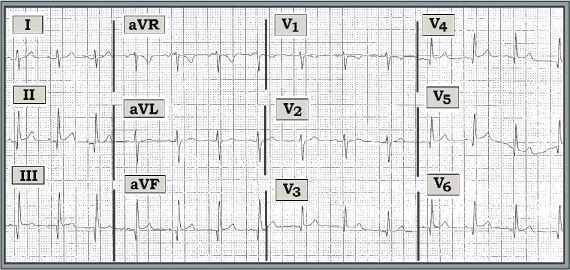
Scenario: The ECG shown above was obtained as part of a routine “pre-op evaluation” for a markedly overweight young adult scheduled for bariatric surgery. The patient was asymptomatic and had no history of cardiac disease. In view of the findings on this “pre-op” ECG, would you “clear” this patient for surgery?
Interpretation: The ECG in the figure shows sinus rhythm at ~ 85/minute. Intervals are normal. The axis is vertical (approximately +90 degrees). There is no chamber enlargement. Remarkable findings reside in assessment of QRST changes. Specifically, Q waves are present in no less than seven leads (II, III, aVF; V3, V4, V5, and V6). Although not overly wide, these Q waves are uncharacteristically deep in the inferior leads for a young adult with no history of cardiac disease. In addition, ST-segment elevation is seen in each of the leads that manifest Q waves. Clearly, this is not a normal tracing.
This case brings up a number of important issues: 1) Is this young, asymptomatic adult who manifests large Q waves and ST-segment elevation on pre-op ECG having an acute infarction? Given the patient’s age, asymptomatic status, and negative cardiac history, this is highly doubtful. Even if the patient were older and having symptoms, features against acute ST-elevation-myocardial-infarction (STEMI) are diffuseness of the changes, lack of reciprocal ST depression, and upward concavity (“smiley”-configuration) ST segment morphology with relative QT shortening that is much more suggestive of early repolarization.
The second issue brought up by this tracing involves the size and number of Q waves seen. Many factors in addition to infarction may produce Q waves on ECG. These include normal variants (due to septal depolarization), non-ischemic cardiomyopathy, and prominent septal forces either as a variant pattern or in its extreme as hypertrophic cardiomyopathy (HCM). Recognition of potential ECG manifestations of this latter entity is important because undetected HCM is the most common cause of sudden death during sports activity in previously healthy young athletes.
The final issue relates to preoperative clearance of this patient. As emphasized above, acute infarction is highly unlikely. On the other hand, this preoperative tracing is not normal. Determining the likely cause of the abnormalities seen is essential for optimal management. Pre-operative echocardiography should provide this information. Echocardiogram will rule out HCM and other forms of cardiomyopathy by providing accurate measurement of septal and posterior wall thickness as well as an estimation of left ventricular function. Given this patient’s large body habitus, the finding of eccentric hypertrophy (and possibly even right ventricular hypertrophy) would not be surprising. This should not preclude the bariatric surgery that is clearly in the best interest of this patient.
The ECG shown was obtained as part of a routine "pre-op evaluation" for a markedly overweight young adult scheduled for bariatric surgerySubscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
