Case Management Insider: The Role of Case Management in an Era of Healthcare Reform Part 1

The Role of Case Management in an Era of Healthcare Reform Part 1
Value of healthcare being redefined
By Toni Cesta, PhD, RN, FAAN
Senior Vice President
Lutheran Medical Center
Brooklyn, NY
Healthcare reform has been discussed for many years, at the federal, state and local levels. While its parameters have been unclear until recently, they are now coming into focus. There is no doubt that the changes imposed by the Affordable Care Act and its value-based purchasing agenda will negatively impact reimbursement across the continuum of care. The Centers for Medicare & Medicaid services are moving away from being a passive payer to an active purchaser of value-based care products and services.
The value of healthcare is being redefined. Quality is defined as a composite of patient outcomes, safety and patient experiences. Payment is the cost to all purchasers of care. Value is then defined as:
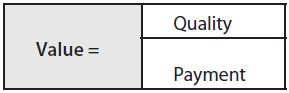
This transition from quantity to quality is a paradigm shift for healthcare providers. Initially hospitals submitted charges to insurers and were paid for services rendered, with few questions asked. In the mid-1980s, a shift occurred to the inpatient prospective payment system (IPPS). IPPS created a shift from payments based on charges to a system using diagnosis-related groups (DRGs) to determine a case rate payment. The IPPS system was used in an attempt to control healthcare expenditures by capping the amount a hospital would be reimbursed for certain types of patients classified into DRGs. Despite the development of this system, healthcare costs continued to climb. Managed care organizations began to grow as health care insurance purchasers sought to find lower-cost coverage for their employees. This shift toward managed care created a process to manage costs for the commercial patient population, but still left the Medicare and Medicaid patients in the old DRG system where costs were still climbing. Even with the introduction of MS-DRGs, costs did not decline.
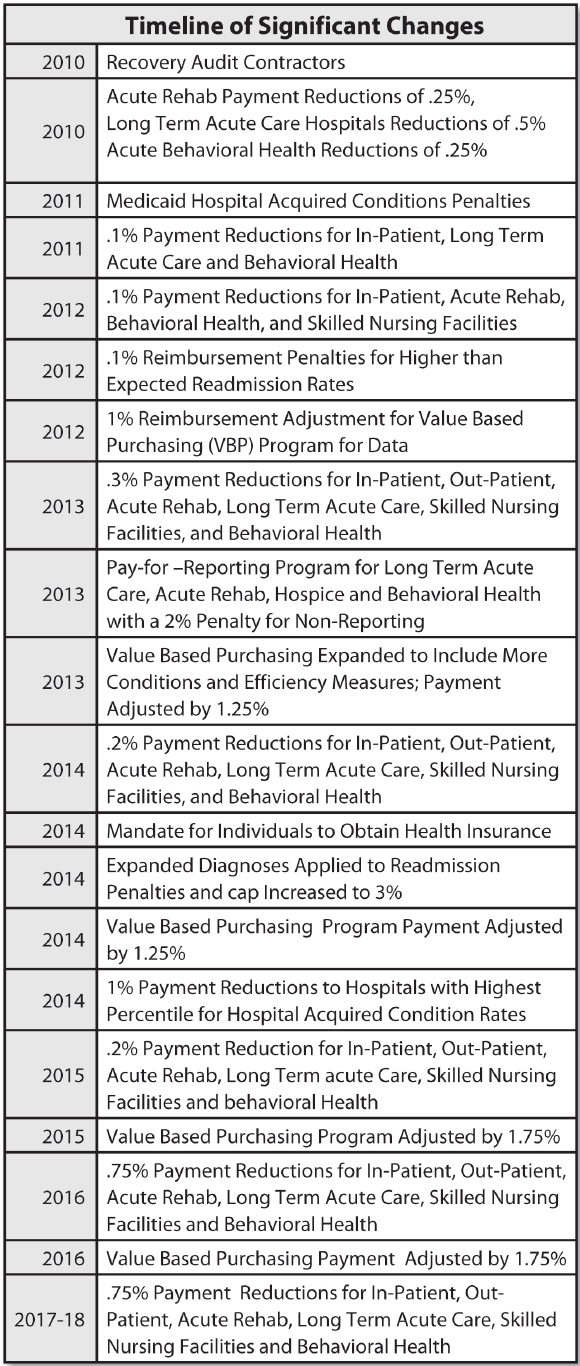
The movement toward reforming the payment system in healthcare has taken on many forms. Some things are for sure now. See page 104 for an outline of the most significant changes that are affecting our business with their timeline.
HealthCare Reform's Impact on the Business of Hospital Management
Some of the changes associated with healthcare reform are, and will continue, to have a profound impact on the business of hospitals. How they manage financially will be, in many ways, affected by how they manage clinically as measured by their quality outcome indicators. Among the most pressing issues that will have an impact are:
- National Coverage Determinations
- Local Coverage Determinations
- Readmissions
- Core Measures
- Hospital Acquired Conditions
- Reductions in Payment
- Meaningful Use
- HCAHPS Scores
National Coverage Determinations
The National Coverage Determinations are a nationwide determination as to whether Medicare will pay for an item or service. Examples include carotid stents, bariatric surgery, and certain pacemakers. Case management departments would stay current on these lists and use them to determine appropriateness for admission.
The newest lists can be found at: https://www.cms.gov/medicare-coverage-database/indexes/nca-open-and-closed-index.aspx?bc=BAAAAAAAAAAA&#Closed.
Local Coverage Determinations
The CMS definition of local coverage determinations is "for purposes of this section, the term 'local coverage determination' means a determination by a fiscal intermediary or a carrier under part a or part b, as applicable, respecting whether or not a particular item or service is covered on an intermediary- or carrier-wide basis under such parts, in accordance with section 1862(a)(1)(A)"
Case management departments can use the following website to find their local coverage determinations for their area: https://www.cms-gov/DeterminationProcess/04_LCDs.asp.
Readmissions
By now most healthcare organizations have implemented initiatives to reduce their Medicare readmissions within 30 days. However, you may be less familiar with the way in which CMS will be calculating your payment changes. (See figure, below, for an example of the calculations used.)
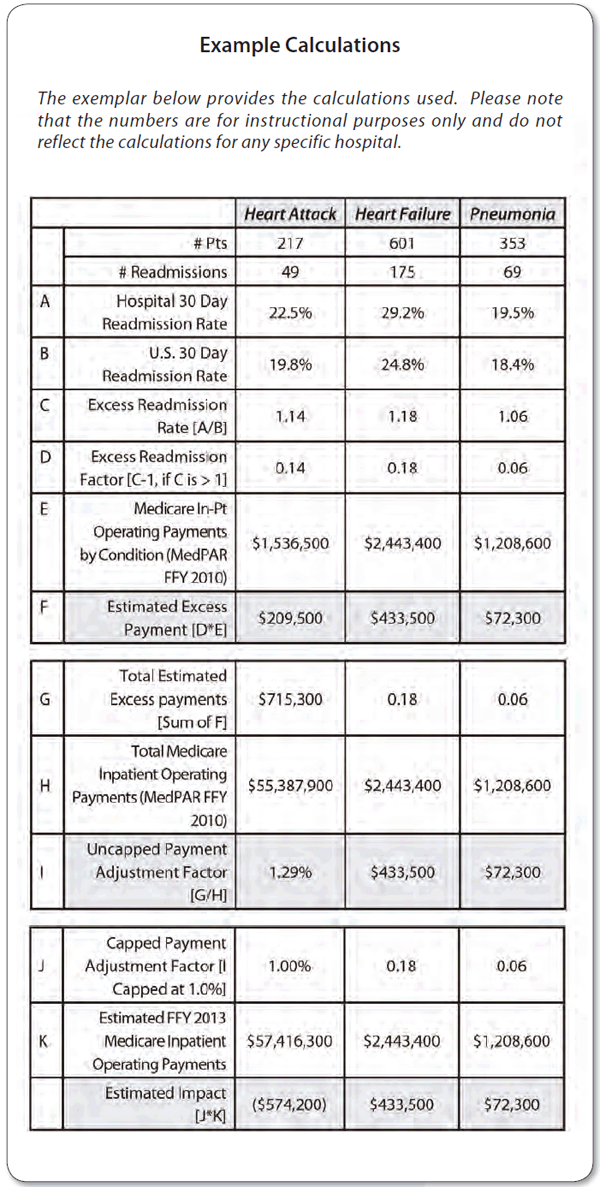
If you follow the table on page 105, you can see how your ranking is calculated. By following lines A C you can see how your hospital's rate is compared to the national rate, which gives you your hospital's "readmission rate."
On line D, if it is greater than 1.0, then your readmission factor is above the expected and an "estimated excess payment" is calculated (lines E- F).
Total estimated excess payments (line G) are the totals of the excess payments in line F.
The uncapped payment adjustment factor is G/H.
For this time period this is capped at 1%, so if your payment factor exceeds 1% it will be capped at 1% (lines I and J).
1% is then multiplied times the FFY 2012 Medicare in-patient operating payments for the hospital to give the final penalty amount (J * K).
You can check your ranking at the following website: www.hopitalcompare.gov
CMS considers readmissions as an "outcome" measure, so you should direct your search to the outcomes section of the website.
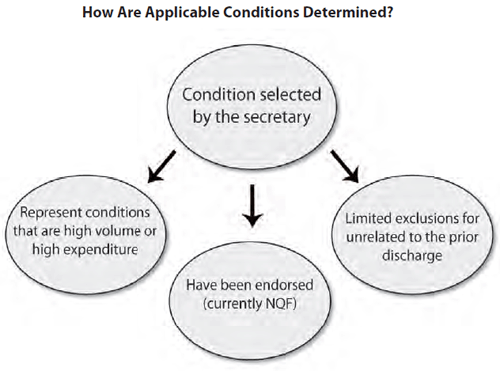
Readmission Applicable Conditions
For Federal Fiscal Year (FFY) 2012 the three diagnoses used in the calculations are:
- 30 Day Risk-Standardized Health Failure (HF)
- 30 Day Risk Standardized Heart Attack (AMI)
- 30 Day Risk-Standardized Pneumonia (PN)
A hospital must have at least 25 discharges for each of the three measures to be included in this measure.
Excluded from Readmission Data
- Discharged Against Medical Advise (AMA)
- In-Hospital Deaths
- Not enrolled in Medicare for 30 Days Post-Discharge
- Transfers to Other Acute Care Facilities
- Same Day Discharges (AMI Only)
Readmission Risk-Adjustment
Adjustments are made by CMS for case-mix differences based on the clinical status of the patient. Examples of these differences include:
- Demographic variables
- Co-Morbid diseases
- Indicators of patient frailty
Exclusions from risk-adjustment include:
- Admission source / discharge disposition
- Socioeconomic status (SES)

Readmission Future Expansion
Next month we will continue our discussion of healthcare reform issues impacting case management!
Healthcare reform has been discussed for many years, at the federal, state and local levels. While its parameters have been unclear until recently, they are now coming into focus.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
