An Update on Sjogren's Syndrome
An Update on Sjogren's Syndrome
Introduction
Sjogren's syndrome is an autoimmune condition that leads to chronic inflammation with salivary and lacrimal gland dysfunction. The diagnosis of Sjogren's often is delayed by several years because the initial presenting symptoms can be non-specific. However, some manifestations of Sjogren's may be life threatening, including brain damage and cancer. It is very important for the primary care physician to recognize the early signs and symptoms and to initiate the appropriate workup and treatment in coordination with consulting specialists to prevent further morbidity and mortality.
Epidemiology
Sjogren's syndrome is divided into two subclasses, primary and secondary Sjogren's. Primary Sjogren's refers to an autoimmune condition of chronic inflammation with salivary and lacrimal gland dysfunction without another underlying autoimmune condition.1 Secondary Sjogren's is associated with autoimmune conditions, most commonly rheumatoid arthritis and systemic lupus erythematosus (SLE).1,2 It is estimated that 25% of patients with rheumatoid arthritis and SLE have secondary Sjogren's.1 The symptoms of Sjogren's and a secondary underlying autoimmune condition may overlap, which can make the diagnosis of secondary Sjogren's challenging. The prevalence of Sjogren's is estimated between 0.5% and 0.6% and it affects approximately 4 million people in the United States. The gender distribution is predominantly female, with a female to male ratio of 9:1. The mean age of onset is between 45 and 55 years of age. There is an equal distribution in the prevalence of primary and secondary Sjogren's.1,2
Pathology
The etiology of Sjogren's is unclear; however, there have been some reports of an association of this disease with specific HLA-DR and HLA-DQ alleles, but only in patients who are SS-A and SS-B antibody positive.2 A biopsy of the minor salivary and lacrimal glands reveals periductal focal lymphocytic infiltrates (See Figures 1 and 2). The severity of inflammation is determined by a scoring system called the "focus score." The pathologist will count the number of inflammatory infiltrates of at least 50 cells in 4 mm squared of gland surface unit. A focus score > 1 per 4 mm squared is significant.3
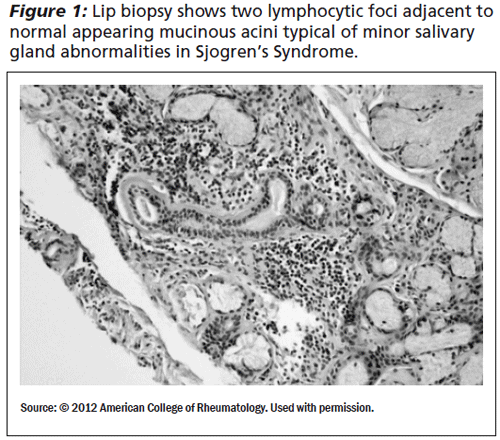
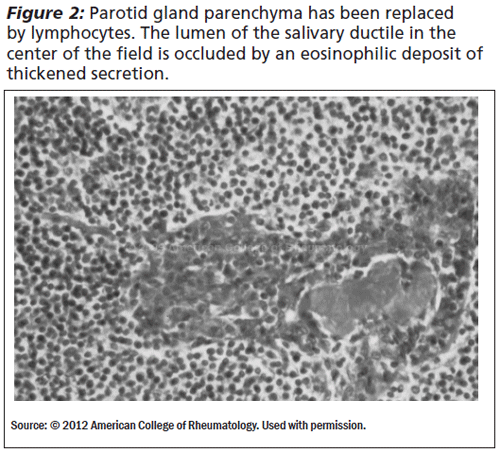
Immunohistology reveals that 75% of the infiltrating cells are T lymphocytes, mainly CD45RO memory helper T cells, and 10% are B cells that are usually found within clusters of T lymphocytes.4 Cell activating factor (BAFF) promotes maturation and survival of B cells. Elevated levels of BAFF have been found in the serum of Sjogren's patients and correlate with the levels of circulating autoantibodies.1 Some researchers propose a viral mechanism that either includes chronic inflammation or provides an antigen that triggers autoimmunity.1 Suggested viruses include Epstein-Barr virus (EBV), coxsackie, hepatitis C virus (HCV), human T-lymphotropic virus Type I, and human immunodeficiency virus (HIV). EBV DNA has been identified in the major and minor salivary gland tissue of Sjogren's patients and coxsackie RNA has been found in the minor salivary glands of primary but not secondary Sjogren's patients.1
Clinical Presentation
Patients with Sjogren's syndrome can present with a variety of clinical manifestations due to the inflammatory nature of the disease, but the two most common complaints are dry eyes and dry mouth. A prospective cohort of 400 patients found that 98% had xerostomia and 93% had xerophthalmia.5 Keratoconjunctivitis sicca results from decreased tear production and changes in the tear film, which leads to repeated dehydration of the ocular surface epithelium and keratinization.1 Characteristic symptoms include a foreign body sensation in the eye, pain, burning, inability to tear, and photophobia. The use of a tear substitute more than three times per day, even in the absence of xerophthalmia, fulfills the dry eye component of the diagnostic criteria. Patients with xerophthalmia have a higher risk of Staphylococcus aureus eye infections; immunosuppressant medications are commonly used in the management of Sjogren's, so early detection and treatment of ocular infections is important.1
Chronic inflammation of the salivary glands leads to decreased saliva production and changes in the oral flora of the mouth. Patients complain of dry mouth, have difficulty chewing or swallowing dry food, and often take frequent sips of water due to the xerostomia.1,2 The patient also may complain of a change in taste and a burning sensation in the mouth. Clinically, the examining physician should look for an absence of salivary pooling at the mouth floor, fissuring and redness of the tongue, and cavities in unusual places (See Figures 3 and 4). Patients with Sjogren's develop cavities at the neck of the teeth next to the gingiva, cusp tips of posterior teeth, or incisal edges of anterior teeth.6
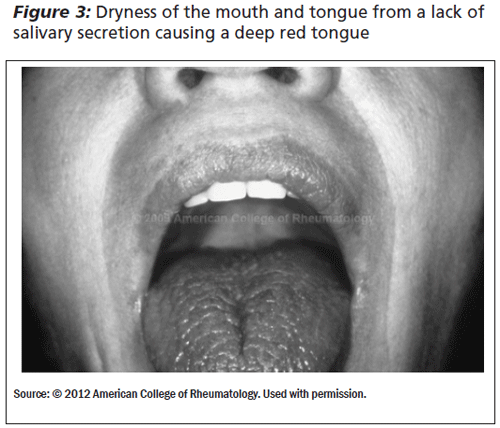
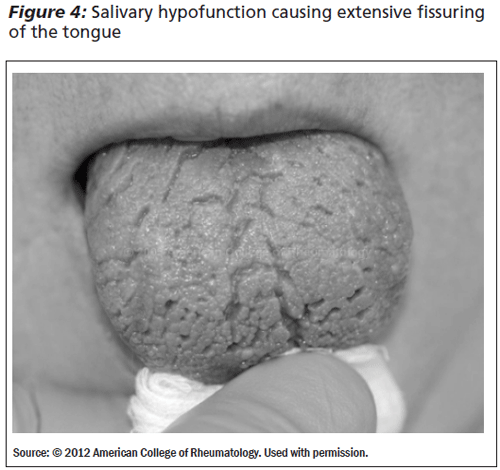
Because of the dryness, these patients may develop hoarseness, recurrent bronchitis, and pneumonia. Exocrine gland dysfunction also may produce a loss of pancreatic function and hypochlorhydria.7 Dermal and vaginal dryness also occur.
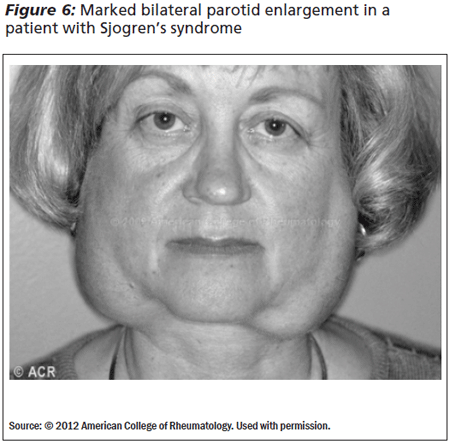
Salivary gland enlargement occurs in 30-50% of patients with Sjogren's, and the glands are firm, diffuse, and non-tender (See Figure 5). At least 20-30% of patients have bilateral enlargements of the parotid or submandibular glands (See Figure 6).

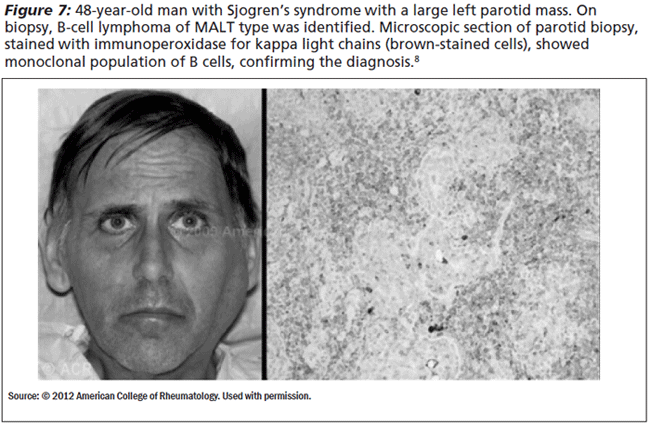
Patients with primary Sjogren's have 40 times the risk of developing lymphoma when compared to the general population.5 Tumors are usually lymphoepithelial lesions due to a benign reactive process; however, they can transform into mucosa-associated lymphoid tissue (MALT) lymphoma (See Figure 7). Patients with B symptoms such as fever, weight loss greater than 10% of body weight in 6 months, and night sweats are at a higher risk for developing lymphoma and should be monitored closely.8 The 5-year survival of appropriately treated MALT lymphoma is 85-95% and the 10-year survival is > 75%.8 Systemic manifestations of Sjogren's include arthralgias, myalgias, fever, and easy fatigability. Arthritis that appears and acts like rheumatoid arthritis and that has erosions occurs in about half of patients with Sjogren's. It can develop into Jaccoud's arthritis like that in SLE and rheumatic fever.7
Patients with Sjogren's syndrome may develop other extraglandular manifestations, such as Raynaud's syndrome, autoimmune thyroiditis, distal renal tubular acidosis (RTA), autoimmune hepatitis, primary biliary cirrhosis, pulmonary disease (chronic diffuse interstitial infiltrates, restrictive pattern demonstrated on pulmonary function tests [PFTs], pulmonary alveolitis, and later fibrosis), genitourinary symptoms (vaginal dryness, increased frequency of endometriosis, menorrhagia, metrorhagia), cutaneous vasculitis (usually small vessel lesions with a leukocytoclastic vasculitis and occasionally cerebral vasculitis), and peripheral nerve dysfunction.
Laboratory Tests
There are no definitive lab tests for Sjogren's; however, laboratory tests can be suggestive of Sjogren's. Patients may have elevated inflammatory markers including erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP), positive SS-A/SS-B antibodies, positive antinuclear antibody (ANA), and hypocomplementemia orcryoglobulinemia. A multicenter report of 400 patients with primary Sjogren's reported finding the following positive tests:2
- anti-Ro(ssA) 40%
- anti-La(ssB) 26%
- antinuclear antibody 74%
- rheumatoid factor (RF) 38%
- anemia 20%
- leukopenia 16%
- thrombocytopenia 13%
- hypocomplementemia 24%.
It is important to yearly monitor a rheumatoid factor, serum IGM, cryoglobulin level, and C4 levels in patients with Sjogren's syndrome, because decreased levels of one or all may herald the occurrence of a lymphoma. A number of diseases are associated with Sjogren's Syndrome including some other autoimmune diseases (See Table 1).

Diagnosis
The diagnosis of Sjogren's syndrome often is delayed because the initial presenting symptoms can be nonspecific. A survey of 3000 patients with Sjogren's reported that the average time between a patient's first symptoms and diagnosis was 6.5 years.2 More than 10 classification criteria have been developed, but the most widely used is the European Community Preliminary Criteria, which also is the least restrictive and diagnoses five times as many people as the most restrictive criteria.1 Several revisions to the European Community Preliminary Criteria have been made. The most current is the American-European Consensus (See Table 2).

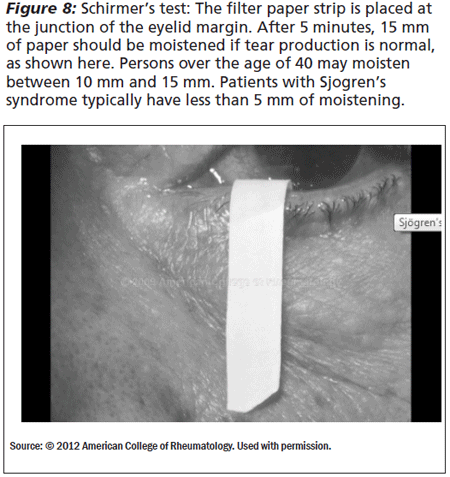
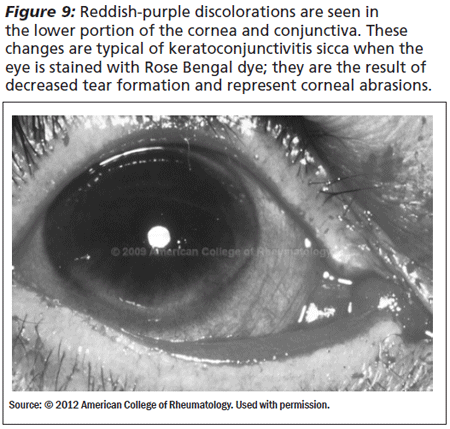
The three tests for keratoconjunctivitis sicca are Schirmer's test, Rose Bengal, and tear breakup time. The Schirmer's test involves placing a piece of filter paper in the lateral third of the lower eyelid. The patient then closes his eye and the amount of wetting on the paper is measured. More than 10 mm of moisture on the filter paper in 5 minutes is normal. Less than 5 mm is definitely abnormal (See Figure 8). The Rose Bengal measures damage to the conjunctival and corneal epithelial cells by staining damaged tissue with Rose Bengal solution.9,10,11 A slit lamp is needed to score the staining so this test is primarily performed by ophthalmologists (See Figure 9). The tear break-up time measures the stability of the tear film. Fluorescein drops are added to the eye and the tear clearance is measured. Patients with Sjogren's have disturbances in the tear film and they have rapid clearance of tears. A clearance time of > 10 seconds is normal, 5-10 seconds is marginal, and < 5 seconds is abnormal.10,11
There are four tests to quantify xerostomia, salivary gland scintigraphy, parotid sialography, whole sialometry, and the Saxon test. Salivary scintigraphy measures the function of the major salivary glands. A very low uptake is specific but not sensitive for Sjogren's.12 Parotid gland sialography is rarely performed in the United States and involves cannulating the major salivary gland ducts and adding a contrast material to aid in visualization. Studies report that salivary scintigraphy correlates better with parotid function.13 Whole sialometry measures the volume of unstimulated saliva production in 15 minutes. Greater than 1.5 ml of saliva is normal. The Saxon test also measures the amount of saliva produced but also measures the amount of stimulated saliva production. The patient is given a sponge to chew on for 2 minutes and the weight of the sponge prior and post chewing is measured. An increase in weight of at least 2.75 g is considered normal.14 It is important to note that these tests for xerostomia are primarily done for research purposes.
If clinical and serologic evidence is not sufficient to make the diagnosis, labial salivary gland biopsy can be performed. It is important for the surgeon to obtain the biopsy from the lower lip that is macroscopically normal and obtain at least four lobules of salivary tissue.1,2
The nonspecific nature of Sjogren's allows for many mimicking diseases. A differential diagnosis for dry eyes should include anticholingeric medications, chronic conjunctivitis, neurologic diseases that impair blinking such as Bell's palsy, and diseases that infiltrate the lacrimal glands such as sarcoidosis, amyloidosis, and lymphoma.1,2 The differential diagnosis for dry mouth should include anticholinergic medications, sialadenitis, viral infections such as HIV and HCV, and irradiation.1,2
If a patient has unilateral parotid swelling you should rule out infection, stones, and malignancy. The differential diagnosis of bilateral parotid swelling includes acute viral infections such as EBV, mumps, coxsackie, and chronic viral infections such as HCV, HIV, and tuberculosis. Other causes of bilateral parotid swelling include sarcoidosis, malnutrition, alcoholism, bulimia, acromegaly, and diabetes.1,2 (See Table 3.)

Treatment
The treatment for ocular symptoms depends on the severity of symptoms and is often comanaged with an ophthalmologist. For mild keratoconjunctivitis sicca, artificial tear drops during the day and preservative-free ointments at night are the treatments of choice. For advanced disease, patients may benefit from systemic cholinergics, such as pilocarpine 5 mg TID to QID or cevimeline 30 mg TID.1,2 It is advisable to start the patient on a low dose and slowly titrate up to minimize side effects. Cyclosporine 0.05% ophthalmic solution also can be beneficial, but it is important to evaluate for underlying eye infections before starting cyclosporine eye drops.2,15 Aside from treating dry mouth symptoms, early detection and treatment of oral caries by a dentist is critical because many patients with salivary hypofunction cannot wear dentures. Dentists will use various fluoride preparations, make dietary recommendations, and use antibiotics to control oral flora. There are commercially available tests that monitor the level of caries causing bacteria.6 Fluoride is used for remineralization of early cavity-causing lesions and also inhibits demineralization and may inhibit plaque bacteria.6 Several over-the-counter synthetic saliva preparations are available and sugar-free lozenges for salivary stimulations are effective techniques for managing xerostomia.1,2,6 Systemic cholinergics (pilocarpine and cevimeline) are also beneficial.1,2 About 33% of patients with Sjogren's suffer from chronic erythematous candidiasis. Clinically, there is an absence of filiform papillae and symmetric mucosal erythema. If the patient produces an adequate amount of saliva, which is observable as salivary pooling at the mouth floor, then fluconazole 100 mg daily for 2 to 4 weeks is the recommended regimen.2,15 If the patient does not produce an adequate amount of saliva, systemic antifungal agents will not reach the infected region so topical antifungals are the preferred treatment.1,2 All commercially available topical antifungal preparations contain sucrose, which is contraindicated in Sjogren's, so the patient will have to be referred to a specialty pharmacy for a sugar-free preparation.1,6
The treatment of extraglandular manifestations depends on the manifestation and severity. Arthralgias and arthritis can be treated with non-steroidal anti-inflammatory drugs, hydroxychloroquine, and methotrexate.1,2 Severe extraglandular manifestations, such as vasculitis, CNS disease, cardiopulmonary disease, and glomerulonephritis, may require glucocorticoids and strong systemic immunosuppressants, such as mycophenolate mofetil, cyclophosphamide, or rituximab.1,2 Treatment with immunosuppressant agents should be administered under the guidance of a rheumatologist, if possible, largely to judge the effect of the medication and the early presence of potentially serious side effects.
Conclusion
Sjogren's syndrome is an autoimmune condition that leads to chronic inflammation and dysfunction of the salivary and lacrimal glands. Sjogren's syndrome is a systemic condition and extraglandular manifestations are common. The nonspecific nature of the disease often results in delays in the diagnosis. The management is typically multidisciplinary and requires primary care physicians, rheumatologists, ophthalmologists, and dentists to work together closely.
References
1. Klippel J, et al. Sjogren's Syndrome. Primer on the Rheumatic Diseases. New York: Springer. 2008; 389-396.
2. Moutsopoulos H, et al. Sjogren's Syndrome. Harrison's Rheumatology. New York: McGraw-Hill. 2010; 124-128.
3. Daniels TE, Whitcher JP. Association of patterns of labial salivary gland inflammation with keratoconjunctivitis sicca. Analysis of 618 patients with suspected Sjogren's syndrome. Arthritis Rheum 1994;37:869-877.
4. Adamson TC 3rd, et al. Immunohistological analysis of lymphoid infiltrates in primary Sjogren's syndrome using monoclonal antibodies. J Immunol 1983;130:203-208.
5. Kruszka P, O'Brian R. Diagnosis and management of Sjogren syndrome. Am Fam Physician 2009;79:465-470. Available at: http://www.aafp.org/afp/2009/0315/p465.html. Accessed July 8, 2012.
6. Wu AJ. Optimizing dry mouth treatment for individuals with Sjogren's syndrome. Rheum Dis Clin North Am 2008;34:1001-1010.
7. Tzioufas AG, et al. Sjogren Syndrome. In: Eds. Hochberg MC, et al. Rheumatology. 5th Edition. Philadelphia, PA: Mosby/Elsevier. 2011;1339-1350.
8. Voulgarelis M, Moutsopoulos HM. Mucosa-associated lymphoid tissue lymphoma in Sjogren's syndrome: Risks, management, and prognosis. Rheum Dis Clin North Am 2008;34:921-933.
9. Afonso AA, et al. Correlation of tear fluoresceine clearance and Schirmer test scores with ocular irritation symptoms. Ophthalmology 1999; 106:803-810.
10. Van Bijsterveld. Diagnostic tests in the Sicca syndrome. Arch Ophthalmol 1969;82:10-14.
11. Kassan SS, Moutsopoulos H. Clinical manifestations and early diagnosis of Sjogren's syndrome. Arch Intern Med 2004;162:1275-1284.
12. Hermann GA, et al, Scintigraphic features of chronic sialadenitis and Sjogren's syndrome: A comparison. Nucl Med Commun 1999; 20:1123-1132.
13. Aung W, et al. Sjogren's syndrome: Comparison of assessments with quantitative salivary gland scintigraphy and contrast sialography. J Nucl Med 2000;41:257-262.
14. Kohler PF, Winter ME. A quantitative test for xerostomia. The Saxon test, an oral equivalent of the Schirmer test, Arthritis Rheum 1985;28:1128-1132.
15. Self SE. Autoantibody testing for autoimmune disease. Clin Chest Med 2010;31:415-422.
Sjogren's syndrome is an autoimmune condition that leads to chronic inflammation with salivary and lacrimal gland dysfunction. The diagnosis of Sjogren's often is delayed by several years because the initial presenting symptoms can be non-specific. However, some manifestations of Sjogren's may be life threatening, including brain damage and cancer. It is very important for the primary care physician to recognize the early signs and symptoms and to initiate the appropriate workup and treatment in coordination with consulting specialists to prevent further morbidity and mortality.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
