Medically Self-Sabotaging Behavior and its Relationship with Borderline Personality
Medically Self-Sabotaging Behavior and its Relationship with Borderline Personality
Authors:
Randy A. Sansone, MD, Professor, Departments of Psychiatry and Internal Medicine, Wright State University School of Medicine, Dayton, OH
Lori A. Sansone, MD, Medical Director, Family Health Clinic, Wright-Patterson Air Force Base Hospital, WPAFB, OH
Peer Reviewer:
Edward A. Selby, PhD, Assistant Professor, Department of Psychology, Rutgers, The State University of New Jersey, New Brunswick
The views and opinions expressed in this article are those of the authors and do not reflect the official policy or position of the U.S. Air Force, Department of Defense, or U.S. Government.
Medically self-sabotaging behavior encompasses a number of diverse phenomena that include factitious disorder, making medical situations worse on purpose, and preventing wounds from healing. Factitious disorder was the first clinically identified syndrome and is most rare. Existing studies indicate associations between factitious disorder and borderline personality disorder (BPD), as well as other psychiatric disorders. In addition to factitious disorder, population surveys indicate a number of other forms of medically self-sabotaging behavior, both in medical and psychiatric populations. Two of these behaviors making medical situations worse on purpose and preventing wounds from healing have undergone empirical investigation. Both are far more common than factitious disorder, exhibit higher rates in populations with greater psychiatric loading, and demonstrate associations with BPD. The association between medically self-sabotaging behavior and BPD is likely explained through the clinical feature of self-harm behavior. Self-harm behavior is an inherent feature of BPD, and medically self-sabotaging behavior may represent a "medicalized" version of self-harm behavior. If these behaviors are self-injury equivalents, they probably function to elicit caring responses from others, control negative emotions, and/or reinforce a dysfunctional identity. There is no known or recommended treatment approach to individuals who engage in medical self-sabotage. However, being alert to the existence of these behaviors and managing such patients conservatively seems to be prudent.
Introduction
Existing data indicate that a significant minority of patients actively sabotage, or intentionally impair, their medical care. Given their covert nature, these behaviors tend to be undetected and under-recognized, and are probably more widespread than indicated by existing prevalence rates. This article will review various aspects of medical self-sabotage, including a working definition of the term, a notorious psychiatric syndrome associated with medical self-sabotage (i.e., factitious disorder), two other studied behaviors (making medical situations worse on purpose, preventing wounds from healing), and empirical data on the relationship between medical self-sabotage and borderline personality disorder (BPD). We then review the syndrome of BPD. Importantly, this clinical area is relatively uncharted territory, and our sampling of existing data is likely to precipitate more questions than provide answers.
As a caveat, this article is not intended to be an in-depth review of existing data, but an overview of general prevalence and associated relationships between medically self-sabotaging behaviors and BPD. Given the surreptitious and deceptive nature of these behaviors, thorough empirical examination will always be realistically compromised.
Medical Self-Sabotage: A Working Definition
The term "medical self-sabotage" can be defined as: (1) the intentional or purposeful generation of surreptitious symptoms; (2) the intentional exaggeration of existing symptoms; and/or (3) the deceitful impedance or sabotage of medical care all with the conscious intent to impair health and/or engage health care professionals. Unlike malingering, in which there is an identifiable financial or legal goal, the benefits of medical self-sabotage appear to be singularly psychological in nature.
Factitious Disorder. Medical self-sabotage is by no means a new clinical phenomenon, but nearly all early references to such behaviors consist of case reports. Most of these case reports are relegated under the clinical heading of factitious disorder, an extreme and dramatic form of medical self-sabotage that was formerly designated as Munchausen's syndrome.
The First Identified Cases of Medical Self-Sabotage. Munchausen's syndrome was first coined by Dr. Richard Asher in 1951.1 This peculiar moniker is derived from Baron von Munchausen, who was born in 1720 near Hanover, Germany. He was described as a brilliant, theatrical, and imaginative storyteller.1 Like the Baron, patients with this psychiatric disorder characteristically present to clinicians with elaborate and incredible symptoms or injuries without any bona fide medical explanation. Therefore, Asher made a pragmatic association between the two. Factitious disorder has been empirically recognized as a form of medical self-sabotage for the past 60 years.
The DSM Description of Factitious Disorder. According to the Diagnostic and Statistical Manual of Mental Disorders, 4th Edition, Text Revision (DSM-IV-TR),2 there are three criteria for factitious disorder: (1) intentionally feigned physical (or psychological) signs or symptoms are present; (2) symptoms are generated to assume the sick role; and (3) there is an absence of external incentives, such as financial gain or avoiding legal responsibility. In comparison with the broader repertoire of behaviors encountered in medical self-sabotage, the behaviors associated with factitious disorder tend to be very dramatic and at times spectacular. Although factitious symptoms are characteristically striking and intense, they paradoxically lack the expected associated clinical features. For example, a patient might appear to exhibit severe hematuria without any global deterioration or abnormal laboratory studies.
In comparison with other types of medical self-sabotage, the element of intentional deception is heightened among individuals with factitious disorder. Specifically, these individuals vigorously engage with health care systems and seek hospitalizations with the intent to deceive. In addition, there is often a provocative emotional overtone among patients with factitious disorder, as many of these individuals seem to be deeply gratified by the challenge that their symptoms pose to health care providers. This does not exclude the psychological function of eliciting caring responses from health care professionals and/or fostering a dependent role.
The Prevalence of Factitious Disorder. According to the DSM-IV-TR,2 the prevalence of factitious disorder is understandably difficult to ascertain due to the element of deception. The DSM-IV-TR indicates that factitious disorder is encountered in about 1% of hospitalized patients who undergo psychiatric consultation. According to physician estimates, the prevalence of factitious disorder in various medical settings is between 1.3%3 and 1.5%.4 However, the prevalence of unexplained medical symptoms among patients may be as high as 11%.4 In a German study of children and adolescents, rates of factitious disorder were between 0.03% and 0.7%, depending on the specific clinical setting.5
The Clinical Context of Factitious Disorder. Despite its clandestine nature, researchers have described a number of clinical characteristics in factitious disorder. For example, in a retrospective study of 93 patients, Krahn and colleagues found that approximately two-thirds were women, the mean age-of-onset was 25 years, and women rather than men were far more likely to have histories of health care training or health care jobs.6 In addition, Krahn and colleagues found that the diagnosis of factitious disorder was established most often by laboratory studies that were inconsistent with presenting symptoms. Not surprisingly, in this sample of patients, only a minority (17%) admitted to their deceptive behavior.
There may be different subsets of patients with factitious disorder. For example, Goldstein found two general contexts for symptom production in factitious disorder. She described symptom emergence in relationship to current life stressors vs symptom emergence due to chronic life patterns.7 These contexts may predict for different underlying psychopathologies, as well.
Table 1: Examples of Feigned or Manufactured Symptoms Reported as Factitious Disorder
- Aortic dissection8
- Cancer9
- Chronic pain10
- Deaf/blindness11
- Hemiplegia12
- Hemoptysis13
- HIV infection14
- Hypoglycemic coma (insulin induced)15
- Mydriasis (induced with a mydriatic)16
- Neurological syndromes, various17
- Osteomyelitis18
- Quadriplegia19
The Symptom Array in Factitious Disorder. The potential types of symptoms produced by individuals with factitious disorder are seemingly endless. Table 1 includes some illustrative examples of symptoms from various case reports in the literature.8-19 For many symptoms, particularly cancer and pain, there are multiple case reports, but only one representative reference is listed.
From a clinical perspective, one of the more challenging factitious symptoms to unmask is pain, which has no objective confirmation. Therefore, we suspect that factitious pain is largely under-reported in the literature.
Psychological Themes in Factitious Disorder. As noted before, this unique subset of patients is distinguished from others who engage in medical self-sabotage by their melodramatic symptoms, intense psychological engagement with health care professionals, and characteristic hospitalizations. From a simplistic perspective, the predominant psychological theme among individuals with factitious disorder seems to be deceiving health care professionals in an effort to experience personal gratification. In contrast, patients with less dramatic types of medical self-sabotage seem to exhibit a broader range of psychological themes.
The Relationship between Factitious Disorder and BPD. Numerous case reports have indicated associations between factitious disorder and BPD.20-28 In the majority of these reports, the diagnosis of BPD was well-established before the clinical presentation of factitious symptoms. In addition, a number of authors have linked psychogenic seizures to BPD.29-31 Finally, Sutherland and Rodin retrospectively examined 10 cases of factitious disorder and found that 30% of individuals suffered from BPD.32 (Despite the fact that these patients were retrospectively assessed for BPD, suggesting missed diagnoses, the cohort still evidenced a substantial rate of this personality dysfunction.) Through a review of the literature, Sutherland and Rodin also confirmed associations between factitious disorder and BPD, among other psychiatric disorders.32
Other Forms of Medically Self-Sabotaging Behavior
In addition to factitious disorders, surveys of clinical samples indicate a potentially broad array of other self-sabotaging behaviors engaged in by patients.
Table 2: The Prevalence of Self-reported Medically Self-Sabotaging Behaviors in a Convenience Sample of Family Medicine Outpatients (n = 411) and a Convenience Sample of Psychiatric Inpatients (n = 120)
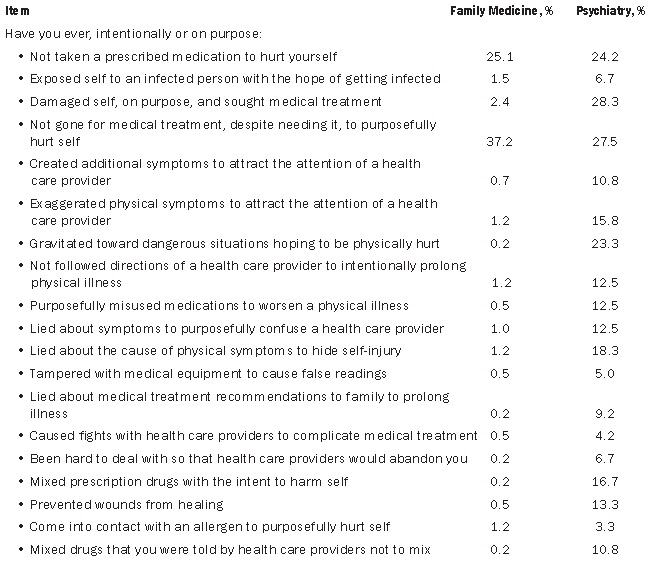
A Survey of Family Medicine Outpatients. We explored the prevalence of medical self-sabotage using a survey methodology among 411 outpatients seeking services at a family medicine clinic.33 For this study, we developed the 19-item Medical Self-Sabotage Survey that began with the query, "Have you ever, intentionally or on purpose,..." (see Table 2). In this sample of primary care patients, we found that 7% acknowledged at least one medically self-sabotaging behavior. Each of the 19 behaviors was reported by at least one participant. Among those who acknowledged histories of medical self-sabotage, the most commonly reported behaviors were "not gone for medical treatment, despite knowing that you need it, to purposefully hurt yourself" (37.2%) and "not taken a prescribed medication to hurt yourself" (25.1%). Note that in this survey, non-compliance with medication was limited to intentionally hurting oneself not due to the cost of the medication or forgetfulness. The results from this study are shown in Table 2. Findings indicate that a substantial minority of primary care patients report the intentional sabotage of their own medical care.
A Survey of Psychiatric Inpatients. In a second survey study, using the same 19-item Medical Self-Sabotage Survey, we examined the prevalence of medical self-sabotage among 120 psychiatric inpatients in an urban general hospital.34 In this sample, 63.3% of participants reported having engaged in at least one medically self-sabotaging behavior and, as in the previous study, each behavior in the survey was reported by at least one participant. In this sample, the two most frequently reported behaviors were "damaged self, on purpose, and sought medical treatment" (28.3%) and "not gone for medical treatment, despite needing it, to purposefully hurt self" (27.5%). The results of this study are also shown in Table 2. Findings indicate that a majority of psychiatric inpatients report the intentional sabotage of their own medical care.
In comparison with participants in the family medicine sample, participants in the psychiatric sample reported comparable or higher percentages of each medically self-sabotaging behavior with the exception of one item "not gone for medical treatment, despite needing it, to purposefully hurt self." This latter item was reported more frequently by participants in the family medicine sample.
One potential limitation in both of these studies is the self-report nature of the data, and related influences include possible misinterpretation, repression, suppression, and/or denial by participants regarding the individual queries (e.g., "I never really did that"). Despite these potential limitations, findings indicate that a meaningful percentage of patients in various clinical settings admit to actively sabotaging their own medical care in a broad number of ways. From these data, we can conclude that, compared with primary care patients, rates of such behavior appear to be generally higher among psychiatric patients. This conclusion strongly suggests an association between medically self-sabotaging behavior and psychopathology.
We now examine two specific medically self-sabotaging behaviors making medical situations worse on purpose and preventing wounds from healing. We elected these two specific behaviors because of the availability of empirical literature, not because these behaviors are necessarily the most common among patients.
Making Medical Situations Worse on Purpose
Prevalence. A potentially less dramatic form of medical self-sabotage is purposefully making medical situations worse (e.g., intentionally being non-compliant with medication to cause the worsening of a medical condition). We examined the prevalence of intentionally making "medical situations worse on purpose" in a study in which we compiled several of our own databases to develop a large sample of internal medicine outpatients (the combination of six databases resulted in a total of 332 participants) and a large sample of psychiatric inpatients (the combination of four databases resulted in a total of 441 participants).35 In each study, the query for making medical situations worse was identical and contained within a self-report survey. According to our findings, the prevalence of making medical situations worse on purpose in the internal medicine and psychiatric samples was 16.7% and 32.0%, respectively.
In a subsequent study of 367 consecutive internal medicine outpatients, we re-examined the prevalence of making medical situations worse on purpose.36 Using a self-report survey methodology and an identical inquiry for this behavior as reported in the previous study of compiled databases, we found that 6.8% of participants admitted to this behavior.
Relationship with Borderline Personality Disorder. In our analysis of compiled databases, we not only examined the prevalence of making medical situations worse, but also relationships with BPD.35 In the internal medicine samples (n = 332), 78 (23.5%) respondents exceeded the cutoff score for BPD. Compared to respondents who did not exceed the cut-off score (n = 254), the BPD group was significantly more likely to have endorsed having made medical situations worse [16.7% vs 2.4%, t(1,330) = 3.30, P < 0.01]. In the psychiatric samples (n = 441), 325 (73.7%) respondents exceeded the cutoff score for BPD. Compared to psychiatric respondents who did not exceed the cutoff score (n = 116), the BPD subsample was significantly more likely to have endorsed having made medical situations worse [32.0% vs 21.6%, t(1,439) = 2.25, P < 0.05].
Preventing Wounds from Healing
Prevalence. We also have examined the intentional preventing of wounds from healing in a number of studies with different types of clinical populations.37-43 These seven studies comprise 1511 patients and are presented in Table 3. The query for preventing wounds from healing was self-report and identical in each study. Prevalence rates vary from 0.8-13.3%. These rates appear to fall into three categories: (1) low rates, observed in a medical sub-specialty population; (2) in-between rates, observed in the primary care populations; and (3) relatively high rates, observed in the substance-abuse/psychiatric populations. According to our findings, it appears that as the psychiatric loading in a given population increases, so does the prevalence of preventing wounds from healing. This finding is in keeping with our comparison of family medicine samples33 and psychiatric samples34 using the Medical Self-Sabotage Survey rates for 18 of 19 behaviors were higher in the psychiatric sample.
Table 3: The Prevalence of Intentionally Preventing Wounds from Healing in Various Clinical Samples

Relationship with Borderline Personality Disorder. We have examined the relationship between preventing wounds from healing and BPD in several clinical samples. In a consecutive sample of internal medicine outpatients,38 we found that those who admitted to preventing wounds from healing had significantly higher scores on two self-report measures for BPD. In addition, admitters were significantly more likely to exceed the cutoff scores for BPD on both measures. In a study of consecutive obstetrics/gynecology outpatients, we found a correlation between preventing wounds from healing and BPD of r = 0.30.40 In a second study of our compiled databases,44 we also found in both primary care and psychiatric samples that those participants who exceeded cutoff scores on the measure of BPD were significantly more likely to endorse preventing wounds from healing compared with those who did not exceed cutoff scores.
Summary. Medically self-sabotaging behavior constitutes a wide range of various behaviors. The most dramatic behaviors tend to fall under the diagnosis of factitious disorder, which constitutes a small subset of individuals. However, the majority of these behaviors appear to be "softer" in character and include intentionally making medical situations worse as well as preventing wounds from healing. According to available findings, there are associations between factitious disorder and BPD, although the specificity of this relationship is difficult to ascertain given the deceptive and uncooperative nature of individuals afflicted with factitious symptoms (i.e., it is difficult to undertake a psychiatric assessment). In addition, all studies examining relationships between making medical situations worse and preventing wounds from healing have confirmed statistical relationships with BPD.
What is Borderline Personality Disorder?
Although a number of psychopathologies may be linked with medically self-sabotaging behavior, especially various depressive disorders, BPD is particularly appealing as a psychiatric possibility because of its association with intentional self-harm behavior a characteristic feature of this type of personality dysfunction.2 We now provide a brief overview of this challenging psychiatric disorder.
A Description of BPD According to the DSM-IV-TR. BPD is classified in the DSM-IV-TR2 as a personality disorder (i.e., an Axis II disorder) as opposed to a major psychiatric disorder (i.e., an Axis I disorder). Among the 11 personality disorders currently identified in the DSM-IV-TR, BPD resides within the Cluster B grouping. As opposed to the Cluster A grouping (characterized by odd and eccentric personality characteristics) and the Cluster C grouping (characterized by fearful and anxious personality characteristics), the Cluster B grouping is characterized by dramatic, emotional, and erratic features and includes borderline, narcissistic, antisocial, and histrionic personality disorders.
Table 4: Resources for Borderline Personality Disorder
- Sansone RA, Sansone LA. Borderline Personality in the Medical Setting: Unmasking and Managing the Difficult Patient. New York: Nova Science Publishers; 2007.
- Kreisman JJ, Strauss H. I Hate YouDon't Leave Me. New York: Avon Books, 1989.
- Sansone RA, Sansone LA. Borderline personality: A primary care context. Innov Clin Neurosci 2004;1:19-27.
- Sansone RA, Sansone LA. Borderline personality and somatic symptoms. Dir Psychiatry 2007;27:17-23.
- Sansone RA, Sansone LA. Borderline personality: Somatic presentations in the medical setting. Prim Care Reports 2007;13:37-48.
- Sansone RA, Sansone LA. Borderline personality: Are proliferative symptoms characteristic? Innov Clin Neurosci 2008;5:18-21.
- Sansone RA, et al. Early family environment, borderline personality symptomatology, and somatic preoccupation among internal medicine outpatients. Compr Psychiatry 2009;50:221-225.
- Sansone RA, Sansone LA. Borderline personality and somatic symptomatology. In: Jackson MH, Westbrook LF (eds.). Borderline Personality Disorder: New Research. Hauppauge, NY: Nova Science Publishers;2009:147-157.
- Sansone RA, Lam C, Wiederman MW. Responses to the medical review of systems: Borderline versus nonborderline patients in an internal medicine setting. Prim Care Companion 2011;13: e1-5.
- The Borderline Personality Disorder Resource Center: An informational resource on borderline personality disorder for both patients and clinicians, located at the New York-Presbyterian Hospital-Westchester Division. For more information, visit: http://bpdresourcecenter.org/whatIs.html.
- BPD Central: An informational resource for both patients and clinicians. For more information, visit: www.bpdcentral.com/index.php.
In the DSM-IV-TR,2 BPD is defined by nine clinical features: (1) frantic efforts to avoid abandonment; (2) a history of unstable and intense relationships with others; (3) identity disturbance; (4) impulsivity in at least two functional areas such as spending, sex, substance use, eating, or driving; (5) recurrent suicidal threats or behaviors as well as self-mutilation; (6) affective instability with marked reactivity of mood; (7) chronic feelings of emptiness; (8) inappropriate and intense anger or difficulty controlling anger; and (9) transient stress-induced paranoid ideation or severe dissociative symptoms. Given that only five of the preceding nine features are required for diagnosis, there are potentially many symptomatic permutations across affected individuals.
The Clinical Texture of BPD. From a clinical perspective, while patients with BPD present in a myriad number of ways, this disorder is consistently characterized by a distinct psychopathological texture. This texture consists of three key features: (1) a seemingly intact social façade (i.e., most individuals can appear quite normal during brief social encounters, such as during office appointments); (2) longstanding self-regulatory disturbances; and (3) chronic self-destructive behavior. Note that this psychopathological composite results in an unusual clinical paradox a seemingly normal exterior coupled with a chaotic interior.
As emphasized previously, every individual with BPD has at least one type of self-regulatory disturbance. A self-regulatory disturbance is the inability to regulate a core self-function. For example, if the core self-regulatory disturbance entails eating behavior, the individual may develop an eating disorder such as anorexia nervosa, bulimia nervosa, binge eating disorder, or obesity. If the core self-regulatory disturbance relates to substance intake, the individual may develop alcohol or drug abuse/dependence, and/or prescription misuse/abuse. If the core self-regulatory disturbance entails the regulation of pain, the individual may develop a chronic pain syndrome.
In addition to one or more self-regulatory issues, individuals with BPD exhibit repetitive self-destructive behavior. These behaviors are usually prolific and may be self-directed (e.g., hitting, cutting, burning oneself; suicide attempts) and/or provoked or elicited from the interpersonal environment (e.g., partner violence, bar fights).
On a side note, prolific symptoms seem to be a characteristic finding among individuals with BPD, either multiple psychiatric or multiple medical symptoms. When multiple psychiatric symptoms are present, the individual will likely have multiple psychiatric diagnoses. When multiple somatic symptoms are present, the individual likely will have multiple medical diagnoses. In either clinical scenario, multiple diagnoses tend to foster multiple points-of-service, numerous medications, and various allergies. The patient's medical history also may be peppered with multiple treatment providers, laboratory studies, treatment failures, and hospitalizations. The general impression in these cases is an over-utilization of health care resources.
The Prevalence of BPD. According to the DSM-IV-TR,2 the prevalence of BPD in the community is around 2%. However, in a recent and well-executed community study, Grant and colleagues reported a prevalence rate of 6%.45 To provide some perspective, the overall prevalence of personality disorders in the general population is around 10%.46
In addition to prevalence rates in the community, the prevalence of BPD has been investigated in a number of clinical settings. In an urban internal medicine outpatient practice, Gross and colleagues found a prevalence rate of 6.4%.47 In resident-provider primary care clinics, which have higher loadings of indigent and lower-functioning patients, we have encountered rates of BPD between 15% and 25%.41
In psychiatric settings, BPD is one of the most frequently encountered Axis II disorders.48 In keeping with this impression, according to the DSM-IV-TR,2 the prevalence of BPD in outpatient and inpatient psychiatric populations is 10% and 20%, respectively. However, in a diagnostically conservative university-based clinic, we found that 22% of outpatients were diagnosed with borderline personality traits or disorder.49 In addition, in an urban inpatient sample, we found a prevalence rate of 50%.50
Gender Patterns in BPD. Although female gender is traditionally associated with BPD,2 Grant and colleagues found equal rates of BPD among the genders.45 We believe that the genders have slightly different clinical presentations with females having histrionic features, eating disorder and trauma diagnoses, and self-directed self-harm behavior, and males having antisocial features, alcohol and substance abuse diagnoses, and more externalized self-harm behavior (e.g., bar fights).51
Age-of-Onset in BPD. According to the DSM-IV-TR,2 BPD symptoms typically emerge during adolescence or early adulthood. This onset period is consistent across cultures.
The Etiology of BPD. Like many psychiatric disorders, BPD appears to be a multi-determined disorder52,53 with contributions from genetics, repetitive trauma in childhood, parental psychopathology, family dysfunction, and a possible triggering event. As for genetics, Distel and colleagues found that heritability accounted for 42% of the variance,54 but what appears to be inherited is non-specific.55 In our opinion, a principal risk factor for the development of BPD is repetitive trauma in early development (i.e., physical, sexual, and emotional abuses as well as the witnessing of violence) a relationship that has been confirmed in the majority of empirical studies.56 Parental psychopathology and family dysfunction also appear to contribute to the development of BPD. Corresponding parental themes may include neglect, lack of empathy, conflicting or invalidating interactions, negativity, over-control, and criticalness.57 Finally, BPD may be precipitated by a triggering event an acute psychosocial stressor that appears to abruptly unleash BPD symptomatology.58
Psychological vs Medical Symptoms in BPD: A Bifurcation Hypothesis. Although many primary care clinicians are familiar with BPD and its association with self-mutilation and suicide attempts, this disorder may also manifest through "medicalized" symptoms such as somatic preoccupation, multiple somatic complaints, and chronic pain.59 Although for many patients there is symptom overlap, it appears that the majority display symptoms that consolidate into either a psychological pattern (i.e., combinations of self-mutilation, suicidal behaviors, interpersonal difficulties, affective instability) or a "medicalized" pattern. This "bifurcation" of symptoms appears to develop early on. The "medicalized" pattern may be associated with a perceived unusual or complicated illness in childhood.60
The Potential Psychological Functions of Medically Self-Sabotaging Behavior. We are not aware of any empirical data on the psychological functions of medically self-sabotaging behavior. However, if these behaviors serve psychological functions similar to other types of self-harm behavior encountered in BPD, such as cutting and overdosing, these might include eliciting caring responses from others (e.g., health care professionals), controlling or regulating strong negative emotions, and/or maintaining a dysfunctional identity.
Medically Self-Sabotaging Behavior and BPD: An Explanation
Given a relationship between medically self-sabotaging behavior and BPD among some individuals, the most likely explanation is that the self-destructive behavior characteristically encountered in individuals with BPD may, in some cases, manifest in "medicalized" ways. In other words, rather than cutting or burning oneself, some individuals may elect to mimic medical syndromes or create/impair illness as an alternative form of self-destructive behavior. Likewise, while the explicit psychological rationales for "medicalized" behavior are empirically unknown, we suspect that the same motivations encountered in traditional self-harm behavior apply. Specifically, such behaviors may be undertaken to elicit caring responses from others, regulate negative emotions, and/or reinforce a "disabled" identity. Clearly, this is a fertile area for future research.
Treatment
At the present time, there is no known effective treatment for individuals who actively sabotage their medical care. The only available approach is for clinicians to be alert to the possibility of medical self-sabotage and, when present, to conservatively manage the patient. As a caveat, given that multiple physicians may be involved with the patient's care, attempting a conservative management plan may be challenging, particularly when contributing providers are unaware of borderline personality psychopathology. On a side note, the effectiveness of open confrontation with the patient remains unknown.
Some patients may be amenable to referral for psychiatric/psychological assessment and treatment. When considered, the clinician may couch this recommendation to the patient in terms of dealing with stress, sleep disturbance, anxiety, etc. If this type of intervention can be successfully undertaken, the patient may benefit from treatment with psychotropic medication (e.g., antidepressants), discussion of stressors, and the processing of "medicalized" self-harm behavior (i.e., motivation for the behaviors). However, in our experience, a substantial percentage of these individuals seem to remain anchored around their physical symptoms, attempting to sustain them through guile, and actively avoid psychiatric/psychological treatment.
Conclusion
Medically self-sabotaging behavior encompasses a broad range of various behaviors that may result in the generation of surreptitious symptoms, exaggeration of existing symptoms, and/or impedance or sabotage of medical care. Although factitious disorder is best known, it represents a very small subset of existing medically self-sabotaging behavior. Studies are limited, but two other forms of medical self-sabotage have been examined making medical situations worse and preventing wounds from healing. Both of these behaviors evidence considerably higher prevalence rates in clinical populations than factitious disorder. There appear to be a number of other medically self-sabotaging behaviors in existence, but these have yet to be empirically explored in any depth. All three of the medically self-sabotaging behaviors discussed in this article (i.e., factitious disorder, making medical situations worse, preventing wounds from healing) evidence relationships with BPD, although for factitious disorder, the evidence is least clear due to the difficulty in systematically studying this population. Why do these behaviors exhibit relationships with BPD? The psychological link is likely to be self-harm behavior. Specifically, medically self-sabotaging behavior may be functioning as a self-harm equivalent, and given that BPD is defined by chronic self-harm behavior, a link is plausible. However, why some patients with BPD elect to medically self-harm vs self-harm in more traditional ways (i.e., self-mutilation) remains unknown. In terms of intervention, at the present time, recognition is all that we can promote, with possible referral to a mental health professional. There is no known clinical intervention or treatment for medically self-sabotaging behavior. Clearly, the area of medical self-sabotage warrants extensive further investigation.
References
1. Fisher JA. Investigating the Barons: Narrative and nomenclature in Munchausen syndrome. Perspect Biol Med 2006;49:250-262.
2. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision. Washington, DC: American Psychiatric Association; 2000.
3. Fliege H, et al. Frequency of ICD-10 factitious disorder: Survey of senior hospital consultants and physicians in private practice. Psychosomatics 2007;48:60-64.
4. Swanson LM, et al. Physician-based estimates of medically unexplained symptoms: A comparison of four case definitions. Fam Pract 2010;27:487-493.
5. Ehrlich S, et al. Factitious disorder in children and adolescents: A retrospective study. Psychosomatics 2008;49:392-398.
6. Krahn LE,. Patients who strive to be ill: Factitious disorder with physical symptoms. Am J Psychiatry 2003;160:1163-1168.
7. Goldstein AB. Identification and classification of factitious disorders: An analysis of cases reported during a ten year period. Int J Psychiatry Med 1998;28:221-241.
8. Chambers E, et al. Factitious aortic dissection leading to thoracotomy in a 20-year-old man. Psychosomatics 2007;48:355-358.
9. Feldman MD, Escalona R. The longing for nurturance: A case of factitious cancer. Psychosomatics 1991;32:226-228.
10. Fishbain DA, et al. Munchausen syndrome presenting with chronic pain: Case report. Pain 1988;35:91-94.
11. Miner ID, Feldman MD. Factitious deafblindness: An imperceptible variant of factitious disorder. Gen Hosp Psychiatry 1998;20:48-51.
12. Biver F, et al. Factitious hemiplegia and Munchausen's syndrome. Acta Neurologica Belgica 1992;92:289-295.
13. Ozden A, Canat S. Factitious hemoptysis. J Am Acad Child Adolesc Psychiatry 1999;38:356-357.
14. Sno HN, et al. Psychogenic "HIV infection." Int J Psychiatry Med 1991;21:93-98.
15. Price WA, et al. Insulin-induced factitious hypoglycemic coma. Gen Hosp Psychiatry 1986;8:291-293.
16. Warrens AN, et al. Positive diagnosis of self-medication with homatropine eye drops. Br J Psychiatry 1990;156:124-125.
17. Bauer M, Boegner F. Neurological symptoms in factitious disorder. J Nerv Ment Dis 1996;184:281-288.
18. Azahin S, Kaya B. A case report of factitious disorder with osteomyelitis symptomatology and chronic pain. Klinik Psikiyatri Dergisi 2009;12:147-152.
19. Feldman MD, Duval NJ. Factitious quadriplegia: A rare new case and literature review. Psychosomatics 1997;38:76-80.
20. Johnson TM. Vomiting as a manifestation of borderline personality disorder in primary care. J Am Board Fam Pract 1993;6:385-394.
21. Hirayama Y, et al. Fatality caused by self-bloodletting in a patient with factitious anemia. Int J Hematol 2003;78:146-148.
22. Archer-Dubon C, et al. Two cases of psychogenic purpura. Rev Invest Clin 1998;50:145-148.
23. Bouden A, et al. Munchausen syndrome by proxy: A challenge for medicine. Presse Med 1996;6:567-569.
24. Popli AP, et al. Factitious disorders with psychological symptoms. J Clin Psychiatry 1992;53:315-318.
25. Castor B, et al. Infected wounds and repeated septicemia in a case of factitious illness. Scand J Infect Dis 1990;22:227-232.
26. Schulz BM, Strauch RJ. A case of factitious subfascial emphysema. Orthopedics 2008;31:495.
27. Chastaing M. Pathomimesis and Munchhausen syndrome. Rev Prat 2009;59:511-517.
28. Jacobi A, et al. Bullous cryothermic dermatitis artefacta induced by deodorant spray abuse. J Eur Acad Dermatol Venereol 2011;25:978-982.
29. Harris CL, et al. Partial seizure-like symptoms in borderline personality disorder. Epilepsy Behav 2002;3:433-438.
30. Reuber M, et al. Multidimensional assessment of personality in patients with psychogenic non-epileptic seizures. J Neurol Neurosurg Psychiatry 2004;75:743-748.
31. Binzer M, et al. Recent onset pseudoseizures clues to aetiology. Seizure 2004;75:743-748.
32. Sutherland AJ, Rodin GM. Factitious disorder in a general hospital setting: Clinical features and a review of the literature. Psychosomatics 1990;31:392-399.
33. Sansone RA, et al. Sabotaging one's own medical care. Arch Fam Med 1997;6:583-586.
34. Sansone RA, et al. The relationship between medically self-sabotaging behaviors and borderline personality disorder among psychiatric inpatients. Prim Care Companion J Clin Psychiatry 2008;10:448-452.
35. Sansone RA, Wiederman MW. Making medical situations worse: Patient disclosures in psychiatric versus medical settings. J Med 2009;2:169-171.
36. Sansone RA, et al. Medically self-sabotaging behavior and multiple symptoms on the review of systems. Prim Care Companion J Clin Psychiatry 2011;13:e1.
37. Sansone RA, et al. The prevalence of self-harm behaviors in a consecutive sample of cardiac stress test patients. Int J Psychiatry Med 2011;41:123-126.
38. Sansone RA, et al. Preventing wounds from healing: A relationship with borderline personality? Int J Psychiatry Med 2010;40:469-471.
39. Sansone RA, et al. The prevalence of self-harm behaviors among a sample of gastric surgery candidates. J Psychosom Res 2008;65:441-444.
40. Sansone RA, et al. Preventing wounds from healing and borderline personality symptomatology in an obstetrics/gynecology sample. Prim Care Companion J Clin Psychiatry (in press).
41. Sansone RA, et al. Medically self-harming behavior and its relationship to borderline personality symptoms and somatic preoccupation among internal medicine patients. J Nerv Ment Dis 2000;188:45-47.
42. Sansone RA, et al. Self-harm behaviors among buprenorphine-treated patients. Prim Care Companion J Clin Psychiatry 2010;12:e1.
43. Sansone RA, et al. The relationship between medically self-sabotaging behaviors and borderline personality disorder among psychiatric inpatients. Prim Care Companion J Clin Psychiatry 2008;10:448-452.
44. Sansone RA, Wiederman MW. Interference with wound healing: Borderline patients in psychiatric versus medical settings. Prim Care Companion J Clin Psychiatry 2009;11:271-272.
45. Grant BR, et al. Prevalence, correlates, disability, and comorbidity of DSM-IV borderline personality disorder: Results from the Wave 2 National Epidemiologic Survey on Alcohol and Related Conditions. J Clin Psychiatry 2008;69:533-545.
46. Ellison JM, Shader RI. Pharmacologic treatment of personality disorders: A dimensional approach. In: Shader RI (ed.). Manual of Psychiatric Therapeutics. Philadelphia: Lippincott, Williams, & Wilkins; 2003:169-183.
47. Gross R, et al. Borderline personality in primary care. Arch Int Med 2002;162:53-60.
48. Quigley BD. Diagnostic relapse in borderline personality: Risk and protective factors. Dissert Abstr Int 2005;65:3721B.
49. Sansone RA, et al. Borderline personality and psychotropic medication prescription in an outpatient psychiatry clinic. Compr Psychiatry 2003;44:454-458.
50. Sansone RA, et al. Diagnostic approaches to borderline personality and their relationship to self-harm behavior. Int J Psychiatry Clin Pract 2001;5:273-277.
51. Sansone RA, et al. Self-harm behaviors in borderline personality: An analysis by gender. J Nerv Ment Dis 2010;198:914-915.
52. Bandelow B, et al. Early traumatic life events, parental attitudes, family history, and birth risk factors in patients with borderline personality disorder and healthy controls. Psychiatry Res 2005;134:169-179.
53. Paris J. The development of impulsivity and suicidality in borderline personality disorder. Dev Psychopathol 2005;17:1091-1104.
54. Distel MA, et al. Heritability of borderline personality disorder features is similar across three countries. Psychol Med 2008;38:1219-1229.
55. Skodol AE, et al. The borderline diagnosis II: Biology, genetics, and clinical course. Biol Psychiatry 2002;51:951-963.
56. Sansone RA, Sansone LA. Borderline personality disorder: The enigma. Prim Care Rep 2000;6:219-226.
57. Sansone RA, Sansone LA. The families of borderline patients: The psychological environment revisited. Innov Clin Neurosci 2009;6:19-24.
58. Zanarini MC, Frankenburg FR. Pathways to the development of borderline personality disorder. J Pers Disord 1997;11:93-104.
59. Sansone RA, Sansone LA. Borderline Personality in the Medical Setting. Unmasking and Managing the Difficult Patient. New York: Nova Science Publishers, 2007.
60. Sansone RA, et al. Early family environment, borderline personality symptomatology, and somatic preoccupation among internal medicine outpatients. Compr Psychiatry 2009;50:221-225.
Medically self-sabotaging behavior encompasses a number of diverse phenomena that include factitious disorder, making medical situations worse on purpose, and preventing wounds from healing.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
