A new standard of care in the ICU? 'Universal decolonization' cuts BSIs 44%
A new standard of care in the ICU? 'Universal decolonization' cuts BSIs 44%
'[The CDC] is likely to take this very seriously in guidance for prevention of hospital infections in ICU patients.'
By Gary Evans, Executive Editor
 In findings that may set a new standard of care in intensive care units, researchers demonstrated in a large-scale trial that a combination of daily chlorhexidine baths and a five-day regimen of nasal mupirocin reduced bloodstream infections (BSIs) for all pathogens by a staggering 44%.
In findings that may set a new standard of care in intensive care units, researchers demonstrated in a large-scale trial that a combination of daily chlorhexidine baths and a five-day regimen of nasal mupirocin reduced bloodstream infections (BSIs) for all pathogens by a staggering 44%.
The unpublished study has major implications for patient safety, as BSIs are among the most deadly and costly of health care associated infections (HAIs).
"I do think that this is a landmark study," says one of the lead investigators, Edward Septimus, MD, medical director of infection control and epidemiology for the Hospital Corporation of America.
Indeed, the study protocol is already being implemented across all ICUs in the Nashville-based 165-hospital HCA system.
"We expect to implement [this protocol] across all of our ICUs starting now and over our whole system by sometime early next year," Septimus tells Hospital Infection Control & Prevention. "Everywhere we have ICUs we will be implementing [this]."
There is the expected and appropriate concern about spurring resistance — particularly to mupirocin — but the caveats were overshadowed at least initially by the dramatic findings. (See related story, p. 124.) Though it began primarily as an intervention against methicillin-resistant Staphylococcus aureus (MRSA), the trial proved effective against a wide array of pathogens — yielding benefits that appeared to exceed the researchers' expectations.
 "We are talking about bloodstream infections — this is a big deal," lead investigator Susan Huang, MD, MPH, FIDSA, medical director of epidemiology and infection prevention at University of California Irvine Healthcare, tells HIC. "[The findings] suggest that the reduction is across the board — gram positive bacteria, gram negative bacteria, and candida.
"We are talking about bloodstream infections — this is a big deal," lead investigator Susan Huang, MD, MPH, FIDSA, medical director of epidemiology and infection prevention at University of California Irvine Healthcare, tells HIC. "[The findings] suggest that the reduction is across the board — gram positive bacteria, gram negative bacteria, and candida.
Unveiled Oct. 19, 2012 in San Diego at the IDWeek Conference, the randomized trial flexed plenty of statistical power. It included some 74,000 patients in 74 ICUs at 43 hospitals in 16 states.
"We think it is large enough that it is unlikely to be replicated," Huang says. [With a lot of research] people will still say — no matter what you found — 'We need a large-scale trial.' We really believe that this is the large-scale trial."
Three arms in randomized study design
Researchers conducted a three-arm cluster-randomized trial of MRSA prevention strategies.1 Study design included a one-year baseline period (Jan-Dec 2009; 48,390 ICU admissions) and an 18-month intervention period (Apr 2010 - Sept 2011; 74,256 ICU admissions). All ICUs in a given hospital were assigned to one of the following arms of the study:
1. MRSA screening and isolation: Nasal MRSA screening followed by contact isolation if positive.
2. Targeted decolonization: MRSA screening followed, if positive, by isolation and decolonization with chlorhexidine baths and nasal mupirocin for five days
3. Universal decolonization: Stop MRSA screening and go to use of mupirocin for five days with daily chlorhexidine baths for the duration of ICU stay.
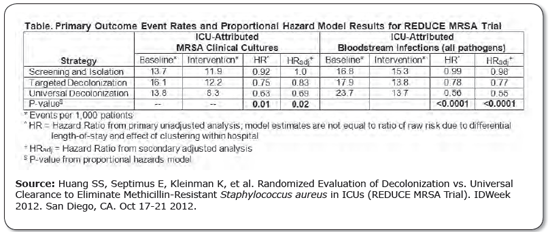
There were significant differences between the study arms for both clinical isolates of MRSA and bloodstream infections caused by all pathogens. In each case, universal decolonization produced a significantly greater reduction than screening and isolation. Targeted decolonization was not significantly different from screening and isolation alone. Adjusted analyses yielded similar results. (See table, below.)
"We found that giving all ICU patients a daily bath with antiseptic soap to remove bacteria from the skin, and applying antibiotic ointment to the nose of all patients was the most effective strategy," Huang says. "This reduced ICU bloodstream infections from all pathogens by nearly half."
While the research group has not released the full study protocol and is still analyzing the findings, it appears the daily baths and nasal decolonization not only lower the risk of cross-transmission but make it less likely the patients will infect themselves with their own bacterial flora.
"It is known that if you don't have MRSA on your body then you are less likely to get infected by it," Huang says. "We also know that if we decolonize people they are less likely to transmit. That has been shown in other smaller studies, and it looks like that is the case here."
In addition, while the mupirocin was only administered for five days to decolonize the nose, the chlorhexidine baths were given daily for the entire patient stay — "for two days or two months," she notes.
"We know from other studies that chlorhexidine has a very broad spectrum for bacterial and fungal coverage," she says. "Even though we stopped screening people [for MRSA], the numbers still came down. So it's not like we were missing people and not detecting folks. We were able to get the MRSA off the body and show that the total amount of cultures that were positive for MRSA were lower in the decolonization arm. We suspect that is because we were able to reduce the bioburden. That translates to protection for the patients themselves and also prevents transmission to others."
Overall, universal decolonization with chlorhexidine and mupirocin in adult ICUs yielded a 37% reduction in risk of an MRSA clinical isolate and a 44% reduction in risk of bloodstream infections due to all pathogens. Bloodstream infections due to all causes in the universal decolonization group decreased from 6.1 infections per 1,000 patient days to 3.6 infections.
"The results are fairly conclusive that the daily bathing and using the ointment in the nose significantly reduced bloodstream infections in a very high-risk population," Septimus says. "We call this a horizontal [study] – that is, we did an intervention that was effective against not just MRSA, but against multiple organisms. When you target an organism that's one thing, but when you target a high-risk population and you can reduce infection risks across multiple pathogens I think that has a great deal of validity. Our study group feels that this certainly should be strongly considered as a standard of care for intensive care unit patients."
The approach eliminates that need for active surveillance for MRSA upon admission to an adult ICU "under normal circumstances," he says. "Anytime you get into an outbreak situation you may alter that, but in the normal circumstance day in and day out, Arm 3 confirms that active surveillance is probably not necessary."
In dropping MRSA screening in favor of the universal decolonization approach, it follows that there will be less patients under contact isolation precautions in the ICU.
"That may have some benefits on a number of fronts. One, it will reduce the costs associated with having patients in isolation," Septimus says. "Secondly, some [isolated] patients feel abandoned. They don't have their vital signs [checked as] frequently, so there are some unintended consequences of putting people in isolation. All of these factors make the intervention in arm three very attractive in a high-risk population like the ICU."
Findings in 'bread and butter' hospitals
Another promising aspect of the trial is that it was conducted primarily in community hospitals rather than large academic centers, meaning the results should translate broadly to U.S. hospitals.
"Most of these trials are done in academic centers and a lot of the other hospitals can't relate," Huang says. "We just never know if the outcomes will be the same in the community-based settings, but these were really bread-and-butter hospitals across America, which makes it really promising."
Similarly, the trial was performed using the typical infrastructure for quality improvement interventions at community hospitals. No study investigators were onsite at the various ICUs, suggesting the approach could be adopted locally without new staff and special expertise.
"That is one of our favorite things about this — how practical it was and how it really used infrastructure that already exists in every hospital," Huang says. "Every hospital normally does their own quality improvement. They all have campaigns, whether it's for hand washing or something else. We believe that these same teams that normally do this for every hospital can readily adopt this in the same way."
The results speak to the much-debated question of whether it's best to target patients who have high-risk pathogens or to target patients in high-risk settings. "We're really pleased to find that a more universal approach is better," she says. "It benefits more patients and it prevents infections from all pathogens — not just MRSA. This may also call in to question the legislation that requires targeted pathogen screening in ICUs in many states."
Indeed, various states have adopted screening requirements for MRSA and other HAIs, but they are unlikely to revisit them in the absence of a formal endorsement of the findings by the Centers for Disease Control and Prevention. That is something that will likely have to go through review by the CDC's Healthcare Infection Control Practices Advisory Committee (HICPAC), and the study has yet to be published in a peer-reviewed journal. Both the CDC and the Agency for Healthcare Research and Quality (AHRQ) were involved in funding the study, but the researchers issued a disclaimer stating that the findings and opinions were theirs alone. Septimus emphasizes that hospitals should continue to follow their state screening laws, but expressed hope that such mandates will be reconsidered in light of the findings.
"[The CDC] is likely to take this study very seriously in upcoming guidance for prevention of hospital infections in ICU patients," Huang says.
Reference
- Huang SS, Septimus E, Kleinman K, et al. Randomized Evaluation of Decolonization vs. Universal Clearance to Eliminate Methicillin-Resistant Staphylococcus aureus in ICUs (REDUCE MRSA Trial). IDWeek 2012. San Diego, CA. Oct 17-21 2012.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
