Low-Carbohydrate Diets and Weight Loss
Obesity
Low-Carbohydrate Diets and Weight Loss
By Dónal P. O'Mathùna, PhD, and Catrina Feeney. Dr. O'Mathùna is a Senior Lecturer; Ethics, Decision-Making & Evidence; School of Nursing; Dublin City University; Ireland. Ms. Feeney is a Student Dietitian, The Ohio State University, Columbus, Ohio. Dr. O'Mathùna and Ms. Feeney report no financial relationships relevant to this field of study.
The incidence of obesity continues to rise. According to the World Health Organization, 1.5 billion people are overweight, with 300 million obese.1 About two-thirds of the U.S. population is overweight, with one-third being obese.2 The number of overweight children in the world more than doubled between 2005 and 2010.3 Obesity is a major risk factor for chronic illnesses, particularly type 2 diabetes, cardiovascular diseases, and some cancers.
In response, various weight-loss strategies have been proposed, popularized, and researched. Low-carbohydrate diets (LCD), while varying in their details, advocate reducing carbohydrate intake while increasing protein calories. The Atkins diet is the most popular of these, with similar principles underlying the Carbohydrate Addict's and Sugar Busters diets.4 Controversy exists over their effectiveness and safety, especially for long-term weight loss.3 With so many people shunning carbohydrates and loading up on protein, evidence from recent studies will be reviewed here so that practitioners can advise patients seeking to lose weight.
Background
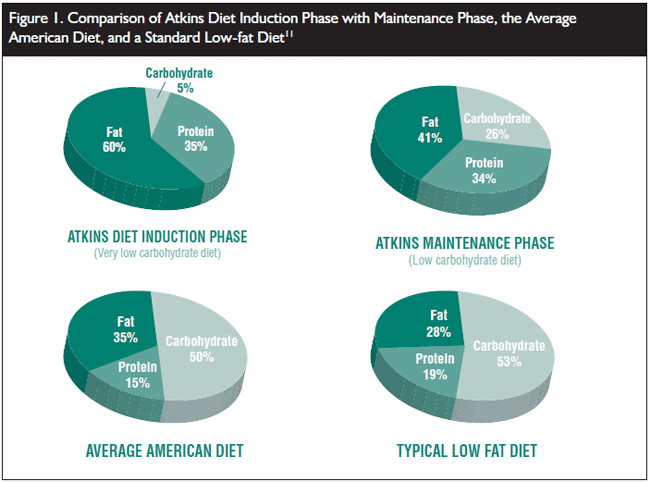
Evaluating LCD is challenging because many different approaches are recommended. Even in reports of clinical trials, it can be difficult to identify participant consumption. Most commonly, the diets are described based on the percent of each macronutrient. Figure 1 shows common diets presented this way. Such representations fail to identify the total number of calories consumed. In some cases, these diets have no restrictions on protein or fat.
Another approach to classifying LCD uses the absolute amount of carbohydrates. According to one scheme, very low carbohydrate diets restrict carbohydrate intake to < 20 g/d, and LCD to < 60 g/d,5 although other quantities are used.6 The average American diet now includes a higher proportion of carbohydrates than in previous generations. The average U.S. male consumes 300 g/d carbohydrates, compared to a recommended daily allowance of 130 g/d.7
Conventional dieting advice has recommended reducing calories and the proportion of fat, especially saturated fat. The Atkins diet was one of the first popular diets to recommend reducing carbohydrates while eating unrestricted amounts of high-protein, high-fat foods like meat, eggs, fish, cheese, olives, and nuts. After an initial 2-week induction period, small amounts of complex carbohydrates are allowed (primarily vegetables and fruits), but breads, pastas, and starchy foods are off limits. The goal is carbohydrate intake below 20 g/d.4 Part of Atkins' argument was that even while Americans were decreasing dietary fat from 40% to 32%, obesity became highly problematic.8 However, while the percentage of fat consumed has decreased since 1975, per capita fat consumption increased by 10 pounds per year, and consumption of simple carbohydrates (like sugar, syrup, and processed flour and rice) increased by 20 pounds per year.9 Clearly, the obesity problem is more complex than some promoters of various diets suggest, with the types of food available and exercise levels also being crucial factors.
Mechanism of Action
A number of metabolic processes are believed to contribute to LCD weight loss. Severely restricting carbohydrates causes glycogen stores to deplete. Each gram of glycogen is stored along with 3 g of associated water, which contributes to weight loss.3 Fewer serum carbohydrates leads to a lower insulin/glycogen ratio, which triggers fatty acid oxidation and ketone body production. The resulting ketosis (not to be confused with ketoacidosis) leads to ketone bodies being metabolized to provide energy for essential organs such as the brain, kidneys, and heart.3 Ketosis has been hypothesized to suppress appetite and promote thermogenic energy expenditure. Fatty acid oxidation may lead to weight loss as fat is metabolized. High-protein diets also may help people feel full quicker and for longer, thus reducing overeating and snacking. However, elevated serum fatty acid levels may also increase cardiovascular disease risk, insulin resistance, and liver steatosis.
Clinical Studies
Many studies have been conducted on LCD for weight loss, although most are not randomized controlled trials (RCT). The most recent systematic review was published in August 2012.1 Seventeen RCTs were identified that lasted at least 3 months. Studies involving subjects with diabetes, cancer, epilepsy, or other diseases were excluded as the reviewers focused on healthy people seeking weight loss. The included studies had a variety of control diets in the comparison groups, and some controlled the total calorie intake and some did not. To avoid complications from these variations, a meta-analysis was conducted using only before and after data from the LCD groups. Significant weight loss compared to baseline was identified at various intervals. At 6 months, mean weight loss was 6.82 kg (95% confidence interval [CI], -7.03 to -6.61); for 6-11 months, -8.09 kg (95% CI, -8.38 to -7.79); for 12-23 months, -6.33 kg (95% CI, -6.87 to -5.79); and at 24 months, -4.65 kg (95% CI, -5.37 to -3.93). However, the reviewers noted that the long-term effectiveness remains unclear as only two studies had follow-up assessments at 24 months. Cardiovascular risk factors also were found to change positively, including significant reductions in blood pressure, plasma triglycerides, blood glucose and plasma insulin, and increased high-density lipoprotein cholesterol (HDL-C).
Earlier systematic reviews compared the effectiveness of LCD with other diets, particularly low-fat diets (LFD). One published in 2009 identified 13 such RCTs lasting at least 6 months.5 After 6 months, weight loss with LCD was significantly greater than with LFD (-4.02 kg; P < 0.00001). At 12 months, the difference had fallen to -1.05 kg (P < 0.05). The dropout rate across all these studies was 36%, with significantly greater attrition from the LFD (P = 0.001). One study lasted 36 months, at which point the two groups did not differ significantly. Between 6 and 36 months, the low-fat group did not change weight, while those on LCD regained weight to a non-significant degree. Total cholesterol was significantly higher with LCD after 6 months (0.19 mmol/L; P < 0.0001), but not after 12 months (0.10 mmol/L; P = 0.31). Low-density lipoprotein cholesterol (LDL-C) was significantly higher with LCD after 6 months (0.14 mmol/L; P < 0.00001) and even higher after 12 months (0.37 mmol/L; P < 0.00001). HDL-C was significantly higher with LCD after 6 months (0.04 mmol/L; P = 0.03) and higher after 12 months (0.06 mmol/L; P < 0.05).
An earlier systematic review identified five trials involving subjects with a body mass index of at least 25.10 This meta-analysis found significantly more weight loss with LCD than LFD at 6 months (-3.3 kg; 95% CI, -5.3 to -1.4) but not at 12 months (-1.0 kg; 95% CI, -3.5 to +1.5). Similar results to the more recent systematic review were noted for serum lipid levels: LCD led to more favorable changes in triglyceride and HDL-C levels, with less favorable changes in total cholesterol and LDL-C levels. The lipid outcomes were similar after 6 and 12 months.
Adverse Effects
Short-term adverse effects are relatively common with LCD, though these are usually transient and not serious. In a study funded by the Atkins Center, among those using the Atkins diet for 6 months, 70% were constipated, 65% had halitosis, 54% had headaches, and 10% had hair loss.12 Reduced fruit, vegetable, and whole-grain consumption may explain these effects.
Much of the controversy about LCD arises from concerns about long-term adverse effects. These center around their high fat content and potentially low plant and fiber content. Additional dietary protein often comes from animal sources that are high in saturated fat and cholesterol. For example, in one study, people consuming the Atkins diet increased their cholesterol intake from 215 mg to 461 mg and then to 285 mg (at baseline, 3 months, and 6 months, respectively).13 These levels were significantly higher than those on the conventional diet: 273 mg, 169 mg, and 182 mg, respectively (P ≤ 0.05).
The impact of elevated cholesterol intake is seen in the serum lipid changes identified in RCTs and systematic reviews discussed above. Although beneficial changes are found in total triglyceride and HDL-C levels, changes that increase cardiovascular risk are found for total cholesterol and LDL-C levels. The overall change and direction of risk with these effects is debated.6 The U.S. Nurses' Health Study found no association between LCD and coronary heart disease risk.14 In contrast, three small European studies showed some association, leading to an extensive cohort study of more than 43,000 Swedish women monitored for 15 years.15 This found that for every 10% decrease in carbohydrate intake or increase in protein intake, the risk of cardiovascular disease increased by 5%, which was statistically significant.
A cross-sectional study of 247 patients with elevated cardiovascular risks examined the impact of LCD on arterial wall function.16 A scoring tool quantified the macronutrient percentages with the lowest quartile scores corresponding to 45% carbohydrate, 20% protein, and 32% fat. The highest quartile scores were diets containing 29% carbohydrate, 24% protein, and 40% fat. Those with the highest scores (lowest carbohydrate) had significantly higher arterial vascular reactivity as measured by peripheral arterial tonometry (P = 0.037). This association was strongest in patients with type 2 diabetes or metabolic syndrome, and was independent of common confounding factors. Such negative effects on endothelial function have been demonstrated in a few other studies. A cohort study of more than 40,000 men followed for 20 years found that LCD was associated with increased risk of type 2 diabetes (P < 0.01).17
Conclusion
Controlled studies of LCD support its greater effectiveness than LFD over 6 months and, possibly, over 12 months. Very few studies last longer than 12 months, but the evidence suggests that long-term weight loss is difficult to sustain. During LCD, changes in the lipid profile are conflicting (but mostly beneficial for triglycerides and fasting insulin), making clear conclusions difficult. However, cohort studies have revealed associations between cardiovascular disease risks and long-term LCD that must be taken seriously.
Part of the difficulty in assessing LCD comes from their many variations. As carbohydrates are restricted, protein and fat portions are increased, but often in different ways. Animal sources will lead to increased consumption of saturated fat and cholesterol, but plant sources can be used instead. Protein can be obtained from lower-fat meats (such as chicken or turkey) and vegetable sources to minimize the proportion of saturated fat (see Harvard HEALTHbeat18 for some specific examples). Fruit and vegetable consumption is sometimes curtailed as a way of avoiding carbohydrates; this may lead to insufficient vitamins being consumed and the need for vitamin supplementation.3
Recommendation
Current evidence supports the use of LCD for weight loss up to about a year. Beyond this, they appear to be no more effective than conventional, low-fat, reduced-calorie diets, but LCDs are significantly more effective than those diets for insulin resistance and related conditions; hence, there may be a subset of patients for which this diet is important to consider. This may be due to the difficulty of sustained adherence to these diets. At the same time, constipation and headaches are common, and may lead to discouragement in their use. In addition, the long-term nutritional quality of LCDs, and their impact on cardiovascular risk factors, is a major concern.
Diet recommendations should be individualized and take account of total calorie consumption, exercise, and availability of personal support. Those already at higher risk for cardiovascular disease should be more cautious about LCDs. At the same time, the risk from these diets may be less than from obesity itself. For those who are generally healthy and seeking shorter-term weight loss, LCD may be an effective strategy at least in the short-term.
References
1. Santos FL, et al. Systematic review and meta-analysis of clinical trials of the effects of low carbohydrate diets on cardiovascular risk factors. Obes Rev 2012 [Epub ahead of print].
2. Bray GA. Diet and exercise for weight loss. JAMA 2012;307:2641-2642.
3. Frigolet ME, et al. Low-carbohydrate diets: A matter of love or hate. Ann Nutr Metab 2011;58:320-334.
4. Bravata DM, et al. Efficacy and safety of low-carbohydrate diets: A systematic review. JAMA 2003;289:1837-1850.
5. Hession M, et al. Systematic review of randomized controlled trials of low-carbohydrate vs. low-fat/low-calorie diets in the management of obesity and its comorbidities. Obes Rev 2009;10:36-50.
6. Hite AH, et al. Low-carbohydrate diet review: Shifting the paradigm. Nutr Clin Pract 2011;26:300-308.
7. Wright JD, Wang C-Y. Trends in intake of energy and macronutrients in adults from 1999–2000 through 2007–2008. Available at: www.cdc.gov/nchs/data/databriefs/db49.pdf. Accessed Oct. 10, 2012.
8. Stephenson J. Low-carb, low-fat diet gurus face off. JAMA 2003;289:1767-1768, 1773.
9. Ornish D. Was Dr. Atkins right? J Am Diet Assoc 2004;104:537-542.
10. Nordmann AJ, et al. Effects of low-carbohydrate vs low-fat diets on weight loss and cardiovascular risk factors. A meta-analysis of randomized controlled trials. Arch Intern Med 2006;166:285-293.
11. Last AR, Wilson SA. Low-carbohydrate diets. Am Fam Physician 2006;73:1942-1948.
12. Westman EC, et al. Effect of 6-month adherence to a very low carbohydrate diet program. Am J Med 2002;113:30-36.
13. Brehm BJ, et al. A randomized trial comparing a very low carbohydrate diet and a calorie-restricted low fat diet on body weight and cardiovascular risk factors in healthy women. J Clin Endocrinol Metab 2003;88:1617-1623.
14. Halton TL, et al. Low-carbohydrate-diet score and the risk of coronary heart disease in women. N Engl J Med 2006;355:1991-2002.
15. Lagiou P, et al. Low carbohydrate-high protein diet and incidence of cardiovascular diseases in Swedish women: Prospective cohort study. BMJ 2012;344:e4026.
16. Merino J, et al. Negative effect of a low-carbohydrate, high-protein, high-fat diet on small peripheral artery reactivity in patients with increased cardiovascular risk. Br J Nutr 2012 [Epub ahead of print].
17. de Koning L, et al. Low-carbohydrate diet scores and risk of type 2 diabetes in men. Am J Clin Nutr 2011;93:844-850.
18. Salamon S. Going low-carb? Pick the right proteins. Harvard HEALTHbeat. 28 February 2012. Available at: www.health.harvard.edu/healthbeat/archive. Accessed Oct. 10, 2012.
The incidence of obesity continues to rise. According to the World Health Organization, 1.5 billion people are overweight, with 300 million obese.1 About two-thirds of the U.S. population is overweight, with one-third being obese.2Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
