Special Feature: Popliteal (Baker’s) Cyst
Popliteal (Baker’s) Cyst
By Richard A. Harrigan, MD, FAAEM
The differential diagnosis of the painful, swollen calf is one that frequently is encountered in the emergency department (ED). The clinician must consider deep venous thrombosis (DVT), cellulitis, calf muscle (i.e., soleus, gastrocnemius, plantaris) tear or rupture, ruptured superficial venous varicosity, hematoma, compartment syndrome, fasciitis, and dissecting or ruptured popliteal cyst (PC).1 It is the latter diagnosis that is less well-defined in our texts and literature—Emergency Medicine: Concepts and Clinical Practice devotes a single paragraph to this entity.2 The following review will discuss the anatomic and pathophysiologic basis, along with the clinical presentation of the PC—in both its intact and ruptured forms. Diagnostic features, including imaging options, as well as associated complications and treatment of this entity also will be described.
Anatomy and Pathophysiology
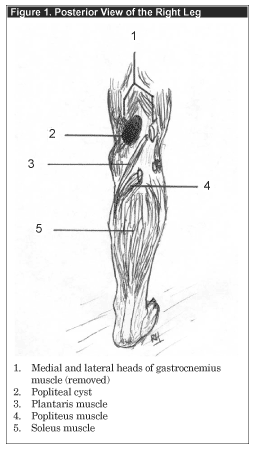
In 1877, Baker elaborated upon what had been described earlier that century by Adams—synovial cysts of the knee. Thereafter, the eponymous Baker’s cyst has been the term attributed to these cystic structures arising in the popliteal space.1-7 Enlargement of the gastrocnemius-semimembranosus bursa, one of six bursa found in the popliteal fossa, is widely accepted as the origin of the majority of these popliteal cysts. (See Figure 1.) As with most bursa, it may communicate with the joint, and thus as joint fluid is elaborated, it will flow into the bursa. A "one-way, valve-like" effect has been observed when studying joint injection of dye; knee flexion opens this valve and allows joint fluid to flow into the bursa; during extension of the knee, this valve is closed by contraction of the gastrocnemius and semimembranosus muscles. Whereas this unidirectional effect on fluid flow from knee joint to gastrocnemius-semimembranosus bursa is the cause of many PCs, other bursa have been implicated less frequently. Moreover, noncommunicating cysts also have been described—these being attributed to primary expansion of the bursa itself. Lastly, in some cases, a PC is actually a simple herniation of the posterior synovium of the knee.3-5,7 (See Table 1.)
 |
 |
PCs feature a bimodal peak age distribution: 4-7 years, and 35-70 years. The younger spike typically is not associated with joint disease and trauma, whereas the older variant—the more common—often has been associated with effusion-generating disease: osteoarthritis, rheumatoid arthritis, and knee trauma, especially medial meniscus tear (posterior horn) and chondral lesions.5-7 Thus, the PC seen in pediatric patients is generally a primary process without associated joint pathology, whereas the adult variety is usually a secondary process where the cyst communicates freely with the joint in the one-way manner outlined above. Joint effusions, from whatever cause, seem to be operative in the formation of the adult or secondary type, in which increasing volume of effusion leads to distention of the PC.4-7 Cyst incidence in adults increases with age, and it appears that, anatomically, the communication between the joint space and the bursa similarly increases with age.5
Clinical Presentation
The clinical appearance of PCs depends upon whether they are intact, dissecting, or ruptured. An intact PC may be asymptomatic, as has been demonstrated by arthrography and magnetic resonance (MR) imaging series; the former technique may overestimate the frequency, however, because the procedure itself distends the joint and may create a small PC.5 When symptomatic, intact PCs are typically mildly so, with patients noting discomfort behind the knee, stiffness, fullness, or swelling—all characteristically worsened by activity.3,5,7 PC symptomatology may be masked by that of the diseased joint.5 Physical examination may reveal posterior knee tenderness and a palpable popliteal mass, usually found on the medial side.7 This mass should be rounded, smooth, fluctuant, and will transilluminate. It is more evident and firm with the knee in full extension; on flexion, it becomes softer and less prominent, a finding referred to as Foucher’s sign.3,5,7 The majority of the mass should be distal to the flexion crease of the knee; pulsatility suggests popliteal artery aneurysm, as does bruit—although a distended cyst may have a pulsatile quality. Most are unilateral.3 Excessive warmth, pain, and tenderness suggest infection of the cyst, which is rare. Case series reflect Staphylococcus aureus to be the most common pathogen in cases of infected cyst, although a variety of organisms, including tubercular, have been implicated.8 Lateral popliteal fossa location with a similar clinical picture is consistent with popliteus bursal enlargement. A PC may still exist without palpable evidence; thus physical examination has both limited sensitivity and specificity.5
If the PC is dissecting, it may present with escalating signs and symptoms localized to the calf as well as the posterior aspect of the knee. If the cyst ruptures, painful swelling and warmth of the calf will ensue, thus mimicking DVT and muscle tear. Some authors do not differentiate between dissection and rupture.9 PC rupture has been labeled the "pseudothrombophlebitis syndrome," highlighting the difficulty in distinguishing this entity from DVT based purely on history and physical examination.1,7,9 Historically, ruptured PC-induced calf symptoms are preceded by symptoms related to the cyst itself; yet it should be remembered that PCs may be asymptomatic, or minimally so. Homan’s sign, infamous due to its insensitivity and lack of specificity for DVT, will likely be positive in dissecting or ruptured cysts. A crescent-shaped purplish discoloration distal to the malleoli in the presence of a swollen, tender calf favors the diagnosis of ruptured PC over DVT. Rarely, cyst rupture may track up the thigh, or rupture of the lateral popliteus cyst may extend down the anterolateral aspect of the lower leg.5 (See Table 2.)
 |
Diagnostic Imaging Options
Although arthrography has traditionally been the gold-standard imaging procedure for popliteal cysts, newer non-invasive options have supplanted it. A variety of imaging studies can be used to detect intact PCs: arthrography, ultrasound, MR imaging, and computed tomography (CT) scan are those with the best literature support.1,5,7,10,11 Ultrasound has emerged as a favored test, for reasons of accuracy, ease, and utility in differentiating not only an intact PC from other popliteal pathology, but also ruptured PC from DVT.
Ultrasonic appearance of a PC is a round or ovoid avascular, nonechogenic mass with a well-defined border located medially in the popliteal fossa. It may have some hypoechoic material and septations in it due to hemorrhage and necrosis; bright echoes suggest proliferation of the synovial lining. Cysts bigger than 1-2 cm in diameter are distinguishable from the midline hypoechoic popliteal artery. False negative studies may result from total rupture and deflation of the cyst, filling of the cyst with echogenic debris, and diameter too small for detection. Ultrasound is especially good at distinguishing popliteal artery aneurysm (the most common site of peripheral aneurysms) from PC, as well as defining the dimensions of solid structures (e.g., tumors).7,11
Duplex sonographic imaging is important in the diagnosis of ruptured PC, in that it has become the ED test of choice for the main competing diagnostic entity: DVT. Applying the "worst first" doctrine, DVT should first be excluded, and then PC can be sought while doing the same test. If the cyst is decompressed totally, it may be difficult to find, but calf extension of the cyst features indistinct cyst borders together with the proper history (sudden onset calf pain) and no evidence of DVT. The clinician must be cautious, however, in that DVT and PC may coexist.1,5,7,9,10 Imaging techniques may be complementary and can be combined in difficult cases.5
Treatment
Treatment of a symptomatic, unruptured PC generally is conservative; in secondary PC, treatment should be directed toward decreasing the effusion associated with the underlying knee disorder. Intra-articular steroid injection after arthrocentesis has been recommended, along with ice, elevation, and anti-inflammatory medications. Less frequently, the cyst itself is aspirated and injected. Operative intervention is reserved for more severely symptomatic cases. In either case, orthopedic referral is appropriate. Treatment of ruptured PC is directed at symptom relief.5-7
References
1. Drescher MJ, Smally AJ. Thrombophlebitis and pseudo-thrombophlebitis. Am J Emerg Med 1997;15:683-685.
2. Antosia RE, Lyn E. Knee and lower leg. In: Rosen P, et al (eds). Emergency Medicine: Concepts and Clinical Practice. (4th ed.) St. Louis: Mosby-Yearbook;1998:786-821.
3. Meyerding HW, VanDemark RE. Posterior hernia of the knee. JAMA 1943;122:858-861.
4. Petros DP, et al. Posterior compartment syndrome following ruptured Baker’s cyst. Ann Rheum Dis 1990;49:944-945.
5. Handy JR. Popliteal cysts in adults: A review. Semin Arthritis Rheum 2001;31:108-118.
6. Rupp S, et al. Popliteal cysts in adults: Prevalence, associated intraarticular lesions, and results after arthroscopic treatment. Am J Sports Med 2002;30:112-115.
7. Langsfeld M, et al. Baker’s cyst mimicking the symptoms of deep vein thrombosis: Diagnosis with venous duplex scanning. J Vasc Surg 1997;25:658-662.
8. Drees C, et al. Baker’s cyst infection: Case report and review. Clin Infect Dis 1999;29:276-278.
9. Simpson FG, et al. Prospective study of thrombophlebitis and "pseudothrombophlebitis." Lancet 1980;331-333.
10. Gordon GV, Edell S. Ultrasonic evaluation of popliteal cysts. Arch Intern Med 1980;140:1453-1455.
11. Langer JE, et al. Imaging of the knee. Radiol Clin North Am 1990;28:975-990.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
