ECG Review: Right Answer/Wrong Reason
By Ken Grauer, MD
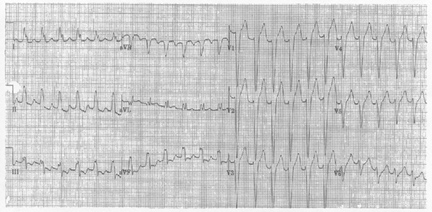
Figure. 12-lead ECG recorded from a 61-year-old woman
with a history of hypertension and chest pain.
The 12-lead ECG shown in the Figure was obtained in the emergency department (ED) from a 61-year-old woman with a history of significant hypertension. She was alert, oriented, and not in acute distress at the time this tracing was recorded, although she was markedly hypertensive and experiencing some chest pain. No prior ECG was available. The patient was treated in the ED with several doses of Adenosine and eventually converted to sinus rhythm. Your thoughts on the rhythm and the management?
Interpretation: The fact that Adenosine was selected and repeated as treatment suggests that the ED physician thought the rhythm was likely to be supraventricular. Since the patient converted to normal sinus rhythm following this treatment, it would be difficult to argue with success. That said, assessment of this ECG and the clinical situation should strongly favor ventricular tachycardia (VT) as the diagnosis with a statistical likelihood of between 80-90%. In similar situations, a different approach might therefore be preferable.
The rhythm in the Figure is a regular wide complex tachycardia (WCT) at a rate of about 150 beats/minute. A small upright deflection is seen in lead II midway between QRS complexes, however there is no way to know if this upright deflection represents a P wave or a T wave (or fusion of the two). Although this WCT rhythm could represent a supraventricular tachycardia with either preexisting bundle branch block or aberrant conduction, one should keep in mind that the statistical likelihood that a regular WCT without definite atrial activity will turn out to be VT exceeds 80%. In view of this patient's age (older adult), history of severe hypertension (underlying heart disease likely), presenting complaint (chest pain), and unusual QRS morphology for left bundle branch block (rS complexes across the precordium), the odds that this rhythm represents VT approach 90-95%. In such cases, specific antiarrhythmic therapy aimed at treating VT (such as IV Amiodarone) or electrical cardioversion may be preferable to a multiple dose trial of Adenosine.
Dr. Grauer, Professor, Assistant Director, Family Practice Residency Program, University of Florida, is Associate Editor of Internal Medicine Alert.
The ECG shown in the Figure was obtained in the emergency department (ED) from a 61-year-old woman with a history of significant hypertension. She was alert, oriented, and not in acute distress at the time this tracing was recorded, although she was markedly hypertensive and experiencing some chest pain. No prior ECG was available. The patient was treated in the ED with several doses of Adenosine and eventually converted to sinus rhythm. Your thoughts on the rhythm and the management?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
